Managing Heavy Menstrual Bleeding
Managing Heavy Menstrual Bleeding. By Dr. Rebecca Cox & Dr. Nabeela Hasan. Aims & Objectives. Defining heavy menstrual bleeding Why is it important Causes Case Scenarios Familiarise new NICE guidelines. What is heavy menstrual bleeding?.

Managing Heavy Menstrual Bleeding
E N D
Presentation Transcript
Managing Heavy Menstrual Bleeding By Dr. Rebecca Cox & Dr. Nabeela Hasan
Aims & Objectives • Defining heavy menstrual bleeding • Why is it important • Causes • Case Scenarios • Familiarise new NICE guidelines
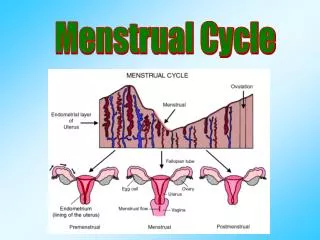
What is heavy menstrual bleeding? Heavy menstrual bleeding (HMB) can be defined as excessive menstrual blood loss which interferes with a woman’s physical, social, emotional and/or material quality of life. (NICE guidelines for Heavy Menstrual Bleeding : January 2007)
Why is it important ? • 1 in 20 women aged 30-49 years consults her GP with HMB • Once referred to gynaecologist, surgical intervention is highly likely • 1 in 5 women in the UK will have a hysterectomy before age 60 • In at least ½ of those who undergo hysterectomy, HMB is the main presenting problem • About ½ of all women who have a hysterectomy for HMB have a normal uterus removed • Only 58% of women receive medical therapy for HMB before referral to a specialist • NICE issued new guidelines for HMB in Jan 2007 (www.doctorsnet.uk- menorrhagia module 2004/5)
Benign: Fibroids DUB PID Endometriosis Polyps Malignant: Endometrial Ca Cervical Ca Ovarian Ca Systemic: thyroid disease coagulation disorders Causes For HMB & Erratic Bleeding
Case 1 • A 28 year old lady comes to see you as she is tired of having heavy periods. • She says she has always had heavy and painful periods for a long time but is finally at the end of her tether with them. • What do you do first?
History • Frequency of bleeding: - Has to change tampon and pad every 2-3 hrs - has flooded several times and is always worried about this. - Bleeds heavily for 4 days. • Menstrual cycle: regular 28 day cycle, bleeds for 6 days. • Pelvic pain only when menstruating • No IMB • No dyspareunia, No PCB • No discharge • Married for 8 yrs, no other partners. • Smear aged 25 - normal • PMH: Nil significant, smoker • FH: Nil signiicant.
Would you examine her? • Abdominal examination – YES • Pelvic exmination +/_ swabs – NO • O/E: Abdomen soft, no tenderness or masses.
NICE guidelines Re: abdominal examination • Abdominal examination is recommended for patients with: • Abdominal pain • Bloating • Constipation • Back pain • Urinary symptoms
Nice GuidelinesRe: pelvic examination • Pelvic examination: If history suggests HMB without structural or histological abnormality, pharmaceutical therapy can be started without pelvic examination or further investigations unless choice of therapy is the IUCD. • If history suggests HMB with structural or histological abnormality eg.IMB, post-coital bleeding, pelvic pain or pressure symptoms then pelvic examination and further investigations should be carried out.
What investigations would you request? • FBC – indicated in all women with heavy menstrual bleeding • Coagulation – only indicated if heavy bleeding since menarche, other symptoms or FH. • TFT’s and Ferritin not required unless clinically indicated. • What management options would you offer?
Nice Guidelines re: pharmaceutical options 1. Levonorgestrel-releasing intrauterine system. • IUCD which slowly releases progesterone and prevents proliferation of the endometrium. • Pelvic exam needed first • Acts as contraceptive • Side effects: Irregular bleeding, hormone related problems
2. Tranexamic Acid, NSAIDs or COCPs.. • Can be used while investigations are being carried out. • Stop tranexamic or NSAIDs after 3 cycles if no improvement. • NSAIDs preferred if dysmenorrhoea • Side effects- see hand out.
3. Oral progestogen (northisterone) or Injected progestogen. • Prevent proliferation of the endometrium. • 15mg daily for days 5-26 of the menstrual cycle or long acting injection. • Contraceptive • Side effects- irregular bleeding, hormonal symptoms, bone density loss
Case 2 • A 30 year old woman had the mirena coil put in one month ago for heavy menstrual bleeding. • Before this she was on the COC which did not control her periods. • Unfortunately she presents today because the coil was expelled a few days ago. • She said this was because her bleeding was so heavy. • She is now on her fourth day of her heavy period & suffering mild discomfort. She goes through 10 pads per day & has passed a few small clots. • She said she had to take 2 days off work because she had to change her pads so often, was fearful of accidents & had pain.
She wants something done about her periods. • She is adamant that she does not want another mirena inserted as she feels it won’t work. • What other treatments could you offer her?
Management options • Tranexamic acid • NSAIDs • COC • Oral progesterones • Injected/implanted progesterones. • Consider referral to a specialist.
She now decides that she does not want any further hormonal treatment as when she was on the pill, she noticed severe changes in her mood & breast tenderness. • After discussion of all the options, you both agree a trial of tranexamic acid. • You also organise a pelvic USS scan. • She tries tranexamic acid for 3 months.
3 months later she comes back and says that tranexamic acid has made very little difference to her periods. • Her USS was normal. • She has been discussing matters with her mother who had a hysterectomy in her 30s. • She says she would like to be referred for a hysterectomy.
What could you do next? • Discuss another less invasive technique such as ablation • Make a referral
NICE Guidelines • When a 1st pharmaceutical treatment proves ineffective, a 2nd can be considered rather than immediate referral to surgery. • However following 2 failed management options it is recommended that the patient is referred.
NICE guidelines re: imaging • Imaging is recommended in the form of USS if • pharmaceutical treatment fails • VE examination reveals a pelvic mass of unknown origin • the uterus is palpable abdominally
NICE guidelines: re endometrial ablation • Endometrial ablation should be considered in women: • where bleeding has a severe impact on QoL & they do not want to conceive in future • with HMB who have a normal uterus & with small uterine fibroids(<3cm in diameter) • preferentially to a hysterectomy alone when the uterus is no bigger than 10/40 & suffer from HMB alone • Women must be advised to avoid subsequent pregnancy & the need to use effective contraception, if required
Case 3 • A 41yr old lady comes to see you with a 12 month history of increasingly heavy and painful periods significantly affecting her quality of life. • No dysuria, frequency or incontinence • LMP 2 weeks ago, Menstrual cycle: 7/28 • She has 2 children • Her last smear was normal • PMH: Nil significant • FH: Grandmother had fibroids
What would you do next? • Abdominal and pelvic examination • Obtain swabs for infection • O/E: Abdominal exam: Suprapubic uterine mass. Pelvic examination reveals a bulky uterus. • You suspect she has uterine fibroids however cannot at this stage rule out anything more sinister.
Investigations • Pregnancy Test – Negative • Urine Dipstix - NAD • FBC • USS: first line investigation for detecting structural abnormalities • Hysteroscopy – only if USS inconclusive
Results.. • USS confirms large uterine fibroids, the largest being 3.6cm diameter.
Do you refer? • Yes: • “Women with fibroids that are palpable abdominally or who have intracavity fibroids and/or whose uterine length as measured at ultrasound or hysteroscopy is greater than 12 cm should be offered immediate referral to a specialist.”
What management should she be offered next? • Endometrial Ablation? No, - This can be offered to women with small fibroids <3cm diameter
Management options • Uterine Artery Embolisation - for women who want to preserve uterus and avoid surgery. May remain fertile. • Myomectomy - for women who want to preserve uterus. May remain fertile.
Hysterectomy - if other treatments fail, if the women no longer wishes to retain her uterus or fertility - if she has been fully informed - if she wishes to have amenorrhoea
Case 4 • A 58 year old lady has been menopausal for the past 5 years. • She comes to the surgery because she has had 2 days of period like bleeding. • She is concerned. • What would you do next?
Obtain further history • Degree of bleeding • Confirm start of menopause • Has it happened before • Weight loss • Pressure symptoms – esp. pelvic pain, urinary frequency/ incontinence, constipation, bloating • Other GU & GI symptoms • O&G hx esp.smears • FHx of Ca • PMH
The lady says that before this bleeding that she has no had a period for 5 years. • This is the first time that this bleeding has happened. • She has noticed some bloating for the past 2 days. No other symptoms • She is nulliparous. Last smear 1yr ago-NAD • No significant PMH or FHx.
You perform a pelvic and abdominal examination. • O/E: • abdomen soft & non-tender. No masses. Normal bowel sounds. • Pelvic exam shows an atrophic looking vaginal walls. Small cystocele. Normal cervix. No blood. • You feel a small 5cm postmenopausal uterus. No masses. • You take swabs for infection.
Would you refer this patient? • Yes • Why? • To rule out endometrial ca/atypical hyperplasia by endometrial sampling and hysteroscopy • Urgent/non-urgent referral? • Urgent • Would you do anything else? • Consider USS
NICE guidelines re: urgent referrals • PMB is endometrial Ca until proven otherwise • Urgent referral is made within one working day • Refer urgently patients with: • Not on HRT with PMB • ON HRT with persistent /unexplained PMB after cessation of HRT for 6 weeks • Taking tamoxifen with PMB • With clinical features suggestive of cervical Ca • Unexplained vulval lump • With vulval bleeding due to ulceration • Consider urgent referral for persistent IMB & negative pelvic exam
NICE guidelines re: pelvic examination • Full pelvic examination including speculum examination is recommended for the following symptoms: • Alterations in menstrual cycle • IMB • PCB • PMB • Vaginal discharge
Endometrial biopsy • Nice Guidelines for HMB recommend that biopsy is indicated for: • Persistent IMB • Women aged >45 • Following treatment failure BUT • When referring patients with a suspicion of endometrial cancer, it is highly likely that they will require an endometrial biopsy, usually via hysteroscopy in this trust.