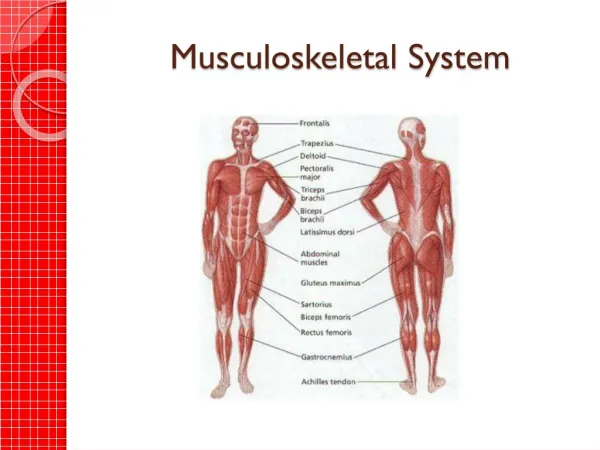
Musculoskeletal System
Musculoskeletal System. Inflammatory Disorders. Presentations Rheumatoid Arthritis Ankylosing spondylitis Osteomyelitis Bursitis. Degenerative Disorders. Osteoporosis Osteoarthritis DJD/Degenerative Joint Disease Total Joint Arthroplasty. Osteoporosis. Increased porosity in the bone

Musculoskeletal System
E N D
Presentation Transcript
Inflammatory Disorders • Presentations • Rheumatoid Arthritis • Ankylosing spondylitis • Osteomyelitis • Bursitis
Degenerative Disorders • Osteoporosis • Osteoarthritis DJD/Degenerative Joint Disease • Total Joint Arthroplasty
Osteoporosis • Increased porosity in the bone • Common disorder of bone metabolism • Decreased mineral and protein matrix • Bone brittle, fragile • Prone to fractures
Osteoporosis • 10 million people in United States have Osteoporosis • Another 34 million have low bone density, which puts them at risk for Osteoporosis • 80% of affected are women • 1.5 million fractures occur each year related to Osteoporosis
Osteoporosis • Silent disease • No symptoms of bone loss • May have 50% loss prior to diagnosis • Multiple fractures may cause decrease in height • Only diagnosed by BMD • Bone Mineral Density • Painless • Non-invasive • safe
Osteoporosis • Risk Factors • Small bones • Advanced age • Family history • Post-menopause with out estrogen replacement • Eating disorders • Low calcium diet • Inactive activity • Smoking • Increased alcohol consumption • Use of corticosteroids or anticonvulsant medications
Medical-Surgical Management • Pharmacological four medications – • Estrogen • Fosamax • Miacalcin • Testosterone • No cure • Prevention
Osteoporsis • Diet • Activity
Nursing Process • Assessment • Subjective Data
Degenerative Joint Disease/DJDOsteoarthritis • NOT inflammatory • Wear and tear disease • Slow, steady, progressive destruction of the joint • Etiology unknown • Most common form of arthritis
Osteoarthritis or DJD • Symptoms • Early morning stiffness • Pain after physical activity • Joint enlargement • Bouchard’s nodes • Heberden’s nodes • Hypertrophic spurs • Distal interphalanges • Hard, painless
Heberden’s Nodes Heberden’s nodes.
Osteoarthritis • Diagnostic tests • Radiographic studies • Arthroscopy • Synovial fluid examination • Bone scans
Osteoarthritis • Medical management/nursing interventions • Surgery
Total Joint Arthroplasty • Joint replacement • Replacement of both articular surfaces with in a joint capsule • Hip, knee, shoulder and fingers are most common sites • Replacement consist of metal and polyethylene
Total Joint Arthroplasty • Older method of cemented in prepared bone is not used as often • New technology uses porous coated cement-less artificial joint component. This allows bone to grow into the joint and less prosthesis failure noted.
Total Hip Replacement • Replacement of severely damaged hip with an artificial joint • Usually people over 60 years • Severe pain, irreversible damage to hip joints
Hip Replacement • Potential problems • Dislocation of prosthesis • Excessive wound drainage • Infection
Following Hip Replacement • Client’s hip and leg to be kept in position of adduction and extension • Knees are apart by abductor pillow or by using foam wedges • Entire leg to be supported when turning side to side • AVOID ACUTE FLEXION OF THE HIP
Following Hip Replacement • Fracture bed pan should be used • Raised toilet seat in bathroom • Vital signs, circulation, movement and sensation checks (CMS) to be done frequently • Inspect dressing frequently • Monitor drainage from portable suction device (JP Drainage) can be as high as 200 -500 cc. With in 48 hours should be less than 30 cc and suction devices can be removed.
Client Goals after Hip Replacement • Ambulate independently • Out of bed the night of the surgery or the next day • Gait training begins so that client can use crutches or cane • FLEXION OF KNEE TO BE AVOIDED • No more than 90 degrees • No stair climbing for three months
Total Knee Replacement • Severe pain and functional disability related to joint destruction • Following knee replacement clients may use CPM continuous passive motion machine which helps increase circulation to operative area and promotes flexibility with in he knee joint.
Knee Replacement • Following surgery…. • Knee to be imoblized • Firm compression dressing • Adjustable soft knee immobilizer • Transfer to chair ok, but NO WEIGHT BEARING is allowed on knee until ordered my MD
Total knee replacement • SCD – Sequential Compression Device may be used or • TED hose – Anti embolism stocking worn to minimize the development of thrombophlebitis • Rehabilitation starts second day • When patient is sitting knee should be elevated • Weight bearing should start with in 1- 2 days
Nursing Management • Cough and deep breathe • Use trapeze to raise hips off bed for bedpan use
NursingAssessment • Nursing Assessment should include… • Neurovascular assessment of affected extremity • Incision assessment • Vital signs • Lung sounds • Pedal pulses • Intake and output
Nursing Assessment • Irritablity • Restlessness • Orientation • Neurovascular assessment for pain, numbness, tingling and paresthesia
Objective Assessment • Incision assessment for • Approximation • Redness • Drainage • Skin color
Assessment • Other assessments • Tachypnea • Dyspnea • Hypoxia • Crackles and wheezes ( s/s of fat embolism) • Position of affected part
Care Plans • Divide in to groups and create care plans