Atherosclerosis
Atherosclerosis . By Joshua Bower Easter Revision 2014 J.Bower@warwick.ac.uk. Distinguish arteriosclerosis, atherosclerosis and arteriolosclerosis. ARTERIOSCLEROSIS – generic term meaning ‘hardening of the arteries’ which encompasses the other 2

Atherosclerosis
E N D
Presentation Transcript
Atherosclerosis By Joshua Bower Easter Revision 2014 J.Bower@warwick.ac.uk
Distinguish arteriosclerosis, atherosclerosis and arteriolosclerosis • ARTERIOSCLEROSIS – generic term meaning ‘hardening of the arteries’ which encompasses the other 2 • ATHEROSCLEROSIS – intimal lesions of arteries caused by atheromas • ARTERIOLOSCLEROSIS – arteriolar hardening seen in HTN and DM
Intima: • Endothelium • BM • Subendothelial connective tissue • Internal elastic lamina • Media: • SMCs • Connective Tissue • Externa/Adventitia • Connective tissue • External elastic lamina • Vasa vasorum
What are vasa vasorum? • Network of small blood vessels supplying walls of large blood vessels • Provide blood supply and nourishment to tunica adventitia and outer part of tunica media
What is an atheroma? • Chronic intimal lesion occurring in arteries • Causes lumen narrowing and weakening of vessel wall
Atheromas are characterised by accumulation of what FOUR things? [4] • Vascular SMCs (vascular smooth muscle cells) • ECM • Inflammatory cells • Lipids
List FOUR modifiable and non-modifiable risk factors for atherosclerosis • Hyperlipidaemia • HTN • Smoking • DM Modifiable Non-modifiable • Older • Male • FHx • Genetics (e.g. ?)
Give an example of a genetic abnormality which may contribute to atheroma development • Apolipoproteins • APLs package fats e.g. LDL • Some APLs act as ligand for receptors for uptake into cells • Abnormal APL or receptors means: • Reduced uptake • Reduced excretion • Thus increased serum LDL
What are the THREE key features of chronic inflammation? [3] • Ongoing inflammation • Ongoing tissue destruction • Ongoing tissue repair
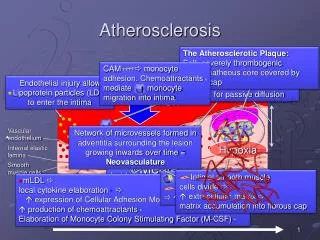
List the steps leading to atheroma development [6] • Chronic endothelial injury (e.g. HTN, smoking) • Endothelial dysfunction (becomes more permeable, cholesterol-rich LDLs enter and becomes oxidised • Monocytes enter, becomes macrophages and attempt to digest the cholesterol – become foam cells (visible as a fatty streak) • Foam cells release growth factors, stimulating SMC infiltration from the media, which then proliferate • Collagen and ECM becomes deposited, forming fibrofatty plaque • SMCs calcify as they degenerate in aged plaques, making them more vulnerable to rupture
Suggest THREE outcomes of atheroma [3] Occlusion Bleeding into atheroma Weakening of vessel wall Aneurysm Thrombus Plaque rupture Atheroma Chronic Narrowing of lumen Embolus Chronic reduction in blood flow Chronic ischaemia
List THREE features of vessels which may make them more vulnerable to atheroma development [3] • High pressure • Bifurcation (e.g. abdominal aorta) • Narrow lumen with high flow (e.g. cerebral vasculature)
An obese 67yo diabetic male presents to his GP with pain in his lower leg which becomes worse after he has been walking for a while. Diagnosis? • Peripheral vascular disease • Intermittent claudication • Pain at rest • Ischaemic limb • These are atherosclerotic blockages outside of the coronary tree – usually lower limb
The effects of the atheroma on distal tissue is dependent on what THREE things? [3-5] • Size of lumen • Stability of plaque • Degree of degeneration of underlying wall • Natural Hx of plaque • Type of blood supply
How can atheroma be treated? [3] • Reduce risk • Stenting by PCTA • Bypass grafting via CABG
Questions? By Joshua Bower Easter Revision 2014 J.Bower@warwick.ac.uk