Digestive System: Overview
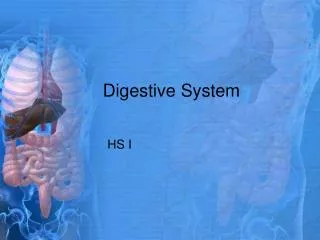
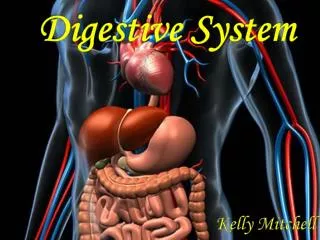
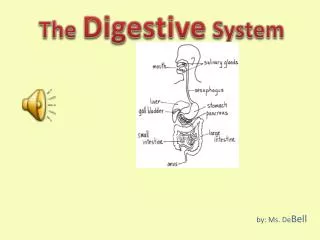
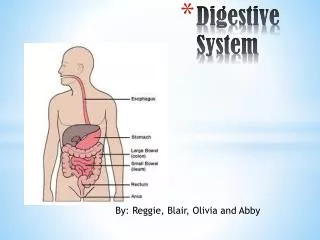
Digestive System: Overview. The alimentary canal or gastrointestinal (GI) tract digests and absorbs food Alimentary canal – mouth, pharynx, esophagus, stomach, small intestine, and large intestine Accessory digestive organs – teeth, tongue, gallbladder, salivary glands, liver, and pancreas.

Digestive System: Overview
E N D
Presentation Transcript
Digestive System: Overview • The alimentary canal or gastrointestinal (GI) tract digests and absorbs food • Alimentary canal – mouth, pharynx, esophagus, stomach, small intestine, and large intestine • Accessory digestive organs – teeth, tongue, gallbladder, salivary glands, liver, and pancreas
Digestive Process • The GI tract is a “disassembly” line • Nutrients become more available to the body in each step • There are six essential activities: • Ingestion, propulsion, and mechanical digestion • Chemical digestion, absorption, and defecation
Gastrointestinal Tract Activities • Ingestion – taking food into the digestive tract • Propulsion – swallowing and peristalsis • Peristalsis – waves of contraction and relaxation of muscles in the organ walls • Mechanical digestion • Physically prepares food for chemical digestion. Includes chewing, mixing of food w/ saliva by the tongue, churning food in the stomach, and segmentation of the intestine (mixing food w/digestive enzymes)
Peristalsis and Segmentation Figure 23.3
Gastrointestinal Tract Activities • Chemical digestion • Series of catabolic steps in which food molecules are broken down to amino acids, simple sugars, free fatty acids by enzymes (mouth & s. intestine) • Absorption – movement of nutrients from the GI tract to the blood or lymph (mainly s. intestine) • Defecation – elimination of indigestible solid wastes
GI Tract • External environment for the digestive process • Regulation of digestion involves: • Mechanical and chemical stimuli – stretch receptors, osmolarity, and presence of substrate in the lumen • Extrinsic control by CNS centers • Intrinsic control by local centers
Receptors of the GI Tract • Mechano- and chemoreceptors respond to: • Stretch, osmolarity, and pH • Presence of substrate, and end products of digestion • They initiate reflexes that: • Activate or inhibit digestive glands that secrete digestive enzymes into the lumen or hormones into the blood • Mix lumen contents and move them along by stimulating smooth muscles of the GI tract walls
Nervous Control of the GI Tract • Intrinsic controls (short reflexes) • Nerve plexuses near the GI tract initiate short reflexes • Short reflexes are mediated by local enteric plexuses (gut brain) • Extrinsic controls (long reflexes) • Long reflexes arising within or outside the GI tract • Involve CNS centers and extrinsic autonomic nerves
Nervous Control of the GI Tract Figure 23.4
Peritoneum and Peritoneal Cavity • Peritoneum – serous membrane of the abdominal cavity • Visceral – covers external surface of most digestive organs & is continuous w/ the parietal peritoneum • Parietal – lines the body wall • Peritoneal cavity • Lies between the visceral & parietal peritonea • Contains serous fluid • Allows the visceral & parietal peritonea to slide across one another
Peritoneum and Peritoneal Cavity Figure 23.5a
Peritoneum and Peritoneal Cavity • Mesentery – double layer of peritoneum that extends to the digestive organs from the body wall and provides: • Vascular, lymphatic and nerve supplies to the digestive viscera • Hold digestive organs in place and store fat • Retroperitoneal organs – organs outside the peritoneum • Adhere to the dorsal abdominal wall and lack mesentary • E.g. pancreas and parts of the l. intestine • Peritoneal organs (intraperitoneal) – organs surrounded by peritoneum & remain in the peritoneal cavity • E.g. stomach
Peritoneum and Peritoneal Cavity Figure 23.5b
Blood Supply: Splanchnic Circulation • Involves those arteries that branch off the abdominal aorta to serve the digestive organs & the hepatic portal circulation • Hepatic, splenic and left gastric branches of the celiac trunk serving the spleen, liver and stomach • Hepatic portal circulation: • Collects nutrient-rich venous blood from the digestive viscera • Delivers this blood to the liver for metabolic processing and storage • Mesenteric arteries serving the s. & l. intestine
Histology of the Alimentary Canal • From esophagus to the anal canal the walls of the GI tract have the same four tunics (layers) • From the lumen outward they are the: • mucosa, submucosa, muscularis externa, and serosa • Each tunic has a predominant tissue type and a specific digestive function
Histology of the Alimentary Canal Figure 23.6
Mucosa (Mucous Membrane) • Moist epithelial layer that lines the lumen of the alimentary canal • Three major functions: • Secretion of mucus, enzymes & hormones • Absorption of end products of digestion into the blood • Protection against infectious disease • Consists of three sublayers: a lining epithelium, lamina propria, and muscularis mucosae
Mucosa: Epithelial Lining • Simple columnar epithelium and mucus-secreting goblet cells • Mucus secretions: • Protect digestive organs from digesting themselves • Ease food along the tract • Stomach and small intestine mucosa contain: • Enzyme-secreting cells • Hormone-secreting cells (making them endocrine and digestive organs)
Mucosa: Lamina Propria and Muscularis Mucosae • Lamina Propria • Loose areolar and reticular connective tissue • Nourishes the epithelium and absorbs nutrients • Contains lymph nodes (part of MALT) important in defense against bacteria • Muscularis mucosae – smooth muscle cells that produce local movements of mucosa
Mucosa: Other Sublayers • Submucosa – dense connective tissue containing elastic fibers, blood and lymphatic vessels, lymph nodes, and nerves • Muscularis externa • responsible for segmentation and peristalsis • Inner circular layer that may thicken to form sphincters • Outer longitudinal layer • Serosa – the protective visceral peritoneum • Replaced by the fibrous adventitia in the esophagus • Retroperitoneal organs have both an adventitia and serosa
Enteric Nervous System • Composed of two major intrinsic nerve plexuses: • Submucosal nerve plexus – regulates glands and smooth muscle in the mucosa • Myenteric nerve plexus – Located between the circular & longitudinal muscle layers. • Major nerve supply that controls GI tract mobility • Segmentation and peristalsis are largely automatic involving local reflex arcs
Enteric Nervous System • Linked to the CNS via long autonomic reflex arc • Parasympathetic inputs enhance secretory activity and motility • Sympathetic impulses inhibit digestive activities
Saliva: Source and Composition • Secreted from serous and mucous cells of salivary glands • 97-99.5% water, hyposmotic, slightly acidic solution containing • Electrolytes – Na+, K+, Cl–, PO42–, HCO3– • Digestive enzyme – salivary amylase • Proteins – mucin, lysozyme, defensins, and IgA • Metabolic wastes – urea and uric acid • Lingual lipase (enzyme) digests fat • Protection agaisnt microrganisms: e.g. IgA & lysozyme
Control of Salivation • Intrinsic salivary glands secrete saliva continuously to keep mouth moist • Extrinsic salivary glands: submandibular (submax.), sublingual & parotid are activated when food enters the mouth • Extrinsic salivary glands secrete serous, enzyme-rich saliva in response to: • Ingested food which stimulates chemoreceptors and mechanoreceptors • The thought of food • Controlled by parasympathetic nervous system • Sympathetic N.S. releases mucin rich saliva • Strong activation of the sympathetic N.S. inhibits saliva release (dry mouth)
Control of Salivation • Chemo- & mechanoreceptors send signals to the salivary nuclei in the brain stem (pons & medulla) • Chemoreceptors: activated strongly by acidic substances • Mechanoreceptors: “ “ any mechanical stimulus • Efferent impulses are sent via motor fibers in the facial & glossopharyngeal nerves • Strong sympathetic stimulation inhibits salivation and results in dry mouth
Pharynx • From the mouth, the oro- and laryngopharynx allow passage of: • Food and fluids to the esophagus • Air to the trachea • Lined with stratified squamous epithelium and mucus glands • Has two skeletal muscle layers • Inner longitudinal • Outer pharyngeal constrictors
Esophagus • Muscular tube going from the laryngopharynx to the stomach • Travels through the mediastinum and pierces the diaphragm • Joins the stomach at the cardiac orifice
Digestive Processes in the Mouth • Mouth & salivary glands are involved in the digestive process • Food is ingested • Mechanical digestion begins (chewing) • Propulsion is initiated by swallowing • Salivary amylase begins chemical breakdown of polysaccharides (starch & glycogen) • Lingual lipase secreted in the mouth acts in the acidic condition of the stomach • The pharynx and esophagus serve only as conduits to pass food from the mouth to the stomach
Mastication (Chewing) • Partly voluntary, partly reflexive • The pattern & rhythm of continued jaw movements are controlled mainly by stretch reflexes and in response to pressure inputs from receptors in the cheeks, gums, tongue
Deglutition (Swallowing) • Food is first compacted by the tongue • Deglutination involves the coordinated activity of the tongue, soft palate, pharynx, esophagus, and 22 separate muscle groups
Deglutition (Swallowing) • Deglutination involves 2 main phases: • 1) Buccal phase (mouth) • Voluntary • Bolus is forced into the oropharynx • Bolus stimulates mechanoreceptors in the pharynx generating reflex activity • 2) Pharyngeal-esophageal phase • Involuntary • Motor impulses from medulla & pons via the vagus nerve cause contraction of muscles of the pharynx & esophagus • All routes except into the digestive tract are sealed off • Peristalsis moves food through the pharynx to the esophagus • The gastroesophogeal sphincter relaxes as the peristaltic wave reaches the end of the esophagus allowing food to enter the stomach
Bolus of food Tongue Uvula Pharynx Bolus Epiglottis Epiglottis Glottis Esophagus Trachea Bolus (a) (b) Upper esophageal sphincter contracted Upper esophageal sphincter relaxed (c) Upper esophageal sphincter contracted Relaxed muscles Relaxed muscles Circular muscles contract, constricting passageway and pushing bolus down Gastroesophageal sphincter open Bolus of food Longitudinal muscles contract, shortening passageway ahead of bolus Stomach Gastroesophageal sphincter closed (e) (d) Figure 23.13
Stomach • Temporary storage area • Chemical breakdown of proteins begins and food is converted to chyme • Nerve supply – sympathetic and parasympathetic fibers of the autonomic nervous system • Blood supply – celiac trunk, and corresponding veins (part of the hepatic portal system)
Digestion in the Stomach • The stomach: • Holds ingested food • Degrades this food both physically and chemically • Delivers chyme to the small intestine • Enzymatically digests proteins with pepsin • Protein digestion is the only significant type of enzymatic digestion that occurs in the stomach • Secretes intrinsic factor required for absorption of vitamin B12
Digestion in the Stomach • Proteins are denatured by HCl produced by stomach glands to prepare proteins for enzymatic cleavage • Major enzymes in stomach: • Pepsinogen (inactive) is released by chief cells and is cleaved by HCl forming pepsin (active) in the stomach lumen (protective mechanism) • Rennin: cleaves casein & produced by infants • Lingual lipase (intrinsic salivary gland): triglyceride digestion • Intrinsic factor: required for intestinal absorption of vitamin B12 needed to produce mature RBCs
Regulation of Gastric Secretion • Neural and hormonal mechanisms regulate the release of gastric juice • Nervous control is provided by long (vagus) and short (enteric) nerve reflexes • When the vagus nerves stimulate the stomach, secretory activity in all its glands increases • The hormone gastrin stimulates secretion of enzymes and HCl
Regulation of Gastric Secretion • Stimulatory and inhibitory events occur in three phases • Cephalic (reflex) phase: prior to food entry • Gastric phase: once food enters the stomach • Intestinal phase: as partially digested food enters the duodenum • The effector site in all 3 phases is the stomach
Phase 1: Cephalic Phase • Reflex phase that occurs before food enters stomach • Several minutes in duration • Excitatory events include: • Sight, smell, taste or thought of food • Stimulation of taste or smell receptors relays signals to the hypothalamus which stimulates the vagal nuclei of the medulla oblongata causing motor impulses to be transmitted via the vagus nerve to parasympathetic enteric ganglion which stimulate stomach glands • Inhibitory events include: • Loss of appetite or depression • Decrease in stimulation of the parasympathetic division
Phase 2: Gastric Phase • Once food reaches the stomach • Several hours in duration • Excitatory events include: • Stomach distension • Activation of stretch receptors (neural activation) • Activation of chemoreceptors by peptides, caffeine, and rising pH • All of these initiate both local reflexes and long vagal reflexes resulting in ACh release causing… • Release of gastrin to the blood and increase in HCl production in the stomach
Phase 2: Gastric Phase (cont.) • Inhibitory events include: • A pH lower than 2 • Emotional upset that overrides the parasympathetic division
Phase 3: Intestinal Phase • Excitatory phase – low pH; partially digested food enters the duodenum of the s. intestine stimulating intestinal mucosal cells to release hormones that mimic gastrin (intestinal gastrin) • Inhibitory phase – distension of duodenum, presence of fatty, acidic, or hypertonic chyme, and/or irritants in the duodenum initiates the enterogastric reflex: • 1) Initiates inhibition of local reflexes • 2) Inhibition of vagal nuclei in the medulla • 3) Activate sympathetic fibers constricting the pyloric sphincter preventing entry into the s. intestine Thus, gastric secretory activity stops protecting the s. intestine from excess acid
Release of Gastric Juice: Stimulatory Events Figure 23.16.1
Release of Gastric Juice: Inhibitory Events Figure 23.16.2
The Hormone Gastrin • Chemical stimuli provided by partially digested proteins, caffeine, and rising pH activate gastrin secreting cells (G cells) in the stomach stimulating them to produce more HCl • As pH falls, G cells are inhibited • G cells are also activated by neural reflexes (fear, anxiety, etc…) and the sympathetic N.S. overrides the parasympathetic N.S.
Regulation and Mechanism of HCl Secretion • HCl secretion is stimulated by ACh, histamine, and gastrin through second-messenger systems (e.g Ca++ for ACh & gastrin; cAMP for histamine) • Release of HCl: • Is low if only one ligand binds to parietal cells • Is high if all three ligands bind to parietal cells • Antihistamines block H2 receptors and decrease HCl release
Regulation and Mechanism of HCl Secretion Bicarbonate Alkaline Tide: blood draining from the stomach is more alkaline than the blood serving it Figure 23.17
Response of the Stomach to Filling • Stomach pressure remains constant until about 1L of food is ingested • Relative unchanging pressure results from reflex-mediated muscle relaxation