Diuretics
Diuretics. A. Kidney functions. Kidneys have a number of essential functions:. 1. excretion. 2. regulate: fluid balance electrolyte composition acid-base balance . 3. secrete enzyme renin . 4. secrete erythropoietin (a hormone that stimulates RBC production).

Diuretics
E N D
Presentation Transcript
A. Kidney functions • Kidneys have a number of essential functions:
2. regulate: • fluid balance • electrolyte composition • acid-base balance
4. secrete erythropoietin (a hormone that stimulates RBCproduction)
5. produce calcitriol, the active form of vitamin D, which helps maintain bone homeostasis
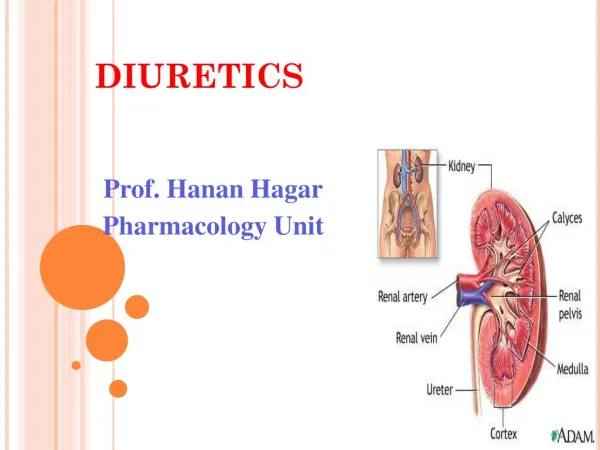
B. Kidney structure • Each kidney contains more than 2 million nephrons, the functional unit of the kidney.
Each nephron is composed of several parts: • glomerulus • proximal convoluted tubule (PCT) • loop of Henle • distal convoluted tubule (DCT) • collecting ducts
The glomerulus is the site where filtration of substances in the blood occurs.
Small molecules, electrolytes and water are filtered from the blood into the glomerular filtrate by passing through filtration slits and pores.
Molecules small enough to be filtered include: • amino acids • creatinine • certain drugs • electrolytes • glucose • urea, uric acid • certain vitamins
Substances in the blood greater than 8 nm are retained in the blood, and include: • blood cells • plasma proteins (i.e. albumin) • hormones
The rest of the nephron (PCT, loop of Henle and DCT) is involved with either: • reabsorbing many of these small molecules, electrolytes, and water and transporting them back into the blood
For every 180 liters (47 gallons) of water entering the filtrate each day, 178.5 liters are reabsorbed, leaving only 1.5 liters to be excreted in the urine.
or, secreting other waste products from the blood to the filtrate for removal in urine
The PCT is the site where water, electrolytes (Na1+, Cl1-, and HCO31- ), glucose and amino acids are reabsorbed.
After leaving the PCT, the filtrate travels through the loop of Henle. This is the site of tubular reabsorption of water, Na1+, K1+, Ca2+, Mg2+, Cl1-, and HCO31- .
Next, the filtrate passes through the DCT. This is the site of tubular reabsorption of most ions including Na1+, K1+, Ca2+, Mg2+, Cl1-, and HCO31-.
The convoluted part of the distal tubule is virtually impermeable to water and urea.
The late distal tubule has a varying permeability to water, depending on the concentration of ADH.
When ADH is elevated, water is reabsorbed. • In the absence of ADH, water is not reabsorbed.
Then the filtrate passes into tubes called collecting ducts where water may be reabsorbed, again dependent on ADH levels.
This is considered a desirable effect in the treatment of the following conditions:
hypertension (HT) • heart failure (HF) • kidney failure • pulmonary edema • liver failure or cirrhosis
The most common way in which diuretics act is by blocking sodiumreabsorption in the nephron, thus sending more of this ion into the urine.
Therefore, blocking the reabsorption of sodium will keep more water in the filtrate.
The more water retained in the filtrate, the greater the volume of urination, or diuresis.
1. Thiazide diuretics • Thiazide diuretics are some of the most widely used of the diuretic drugs.
The site of diuretic action for the thiazide diuretics is the early DCT.
Thiazides are the preferred diuretic in the treatment of HT, mild HF, and certain renal disease (nephrolithiasis, nephrogenic diabetes insipidus).
They cause a greater diuresis than the K1+ sparing diuretics, but a lesser diuresis than the organic acid diuretics.
This results in a mild increase in serum Ca2+ levels, which decreases bone resorption (release of Ca2+ from bone).
They would be recommended for patients at risk of osteoporosis.
The distal tubule is the main site in the nephron for the secretion of K1+ , normally in exchange for Na1+ .
Thiazide diuretics work by inhibiting sodium reabsorptionwhich increases its excretion, along with Cl1- and substantial amounts of water.
Thiazide diuretics include: • chlorothiazide (diuril): 500 mg – 2,000 mg/day for both HT, edema. • Duration: 6 – 12 hours
hydrochlorothiazide (HydroDIURIL, Hydropar, Ezide): • 25 - 50 mg/day for HT • 25 - 100 mg/day for edema • Duration: 6 – 12 hours
This drug is a derivative of chlorothiazide that is more popular than the parent drug.