Chapter 3 Immunity
Chapter 3 Immunity. Outline The Acquired Immune Response Antigens Cellular Involvement in the Immune Response Major Divisions of the Immune Response Memory and Immunity Types of Immunity Immunopathology Oral Diseases with Immunologic Pathogenesis


Chapter 3 Immunity
E N D
Presentation Transcript
Chapter 3 Immunity
Outline The Acquired Immune Response Antigens Cellular Involvement in the Immune Response Major Divisions of the Immune Response Memory and Immunity Types of Immunity Immunopathology Oral Diseases with Immunologic Pathogenesis Autoimmune Diseases that Affect the Oral Cavity
The Acquired Immune Response (pg. 82) Defends the body against injury Has the capacity to remember and respond more quickly the second time a foreign material enters the body Works with the inflammatory response and a working repair process Involves white blood cells, especially lymphocytes and their products
Antigens (pg. 82) Foreign substances Mainly proteins, often microorganisms and their toxins Human cells that have been transformed May be tumor cells, or cells infected with viruses
Antigens (cont.) Human tissue Organ transplants, tissue grafts, incompatible blood types during a transfusion Autoimmune diseases Tissue from the person’s own body becomes an antigen
Cellular Involvement in the Immune Response B lymphocytes T lymphocytes Macrophages Cytokines
Cellular Involvement in the Immune Response (cont.) (pg. 83) Cells that are able to recognize and respond to antigen Derived from precursor cells in bone marrow (stem cells) 20% to 25% of the WBC (white blood cell) population Two main types B lymphocytes (B cells) T lymphocytes (T cells) Also there are natural killer cells (NK cells) Can destroy cells recognized as foreign without recognizing specific antigens
B Lymphocytes (pgs. 83-84) Mature and reside in lymphoid tissue Lymph nodes, tonsils, and other body tissue B lymphocytes travel to the site of injury when stimulated by antigen Two main types Plasma cells Produce specific antibodies B memory cell Retains the memory of previously encountered antigen and will clone itself in the presence of antigen
Plasma Cells Produce antibodies that are categorized into 5 classes of immunoglobulins, which are carried in blood serum All have the same basic “Y” structure, but have an area with variable (V) structure at the tips of the Y The stem of the Y is constant (C) for all 5 types, and links the antibody to other components of the immune response Immune complex Antigen combined with antibody
T Lymphocytes (pgs. 83, 85) Travel to the thymus and mature The thymus is large in an infant, shrinks as the child matures Several different types of T lymphocytes Memory cells T-helper cells Increase functioning of B lymphocytes T-suppressor cells Turn off functioning of B lymphocytes T-cytotoxic cells Attack virally infected cells or tumor cells
Macrophages (pg. 84) Active in phagocytosis of foreign material Produce cytokines called monokines Help both B and T lymphocytes After phagocytosis, they process and present antigen to lymphocytes This stimulates lymphocytes to travel from lymphoid tissue to the injury site Amplify the immune response but do not remember the antigen like lymphocytes
Cytokines (Cont.) (pgs. 84-85) (Table 3-2) Proteins made by cells that are able to affect the behavior of other cells Different cytokines have different functions.
Major Divisions of the Immune Response (pgs. 85-86) Humoral response B lymphocytes are the primary cells. Involves production of antibodies Cell-mediated response T lymphocytes are the primary cells. Lymphocytes may work alone or be assisted by macrophages. The cell-mediated portion regulates both major responses.
Memory and Immunity (pg. 86) The immune system has memory; the inflammatory system does not. Some lymphocytes retain memory of an antigen after an initial encounter. This means the immune response will be faster and stronger the next time an antigen enters the body. The retained memory is called immunity.
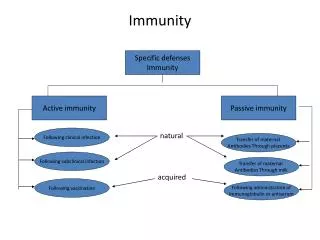
Types of Immunity Passive Immunity Active Immunity
Passive Immunity (pg. 86) Using antibodies created by another person to prevent infectious disease Natural When antibodies from the mother pass through the placenta to the developing fetus Acquired When antibodies are acquired through an injection Short lived but fast acting
Active Immunity (pg. 86) Antibodies created by the person themselves Natural Protection conferred following survival from an infectious disease Acquired Injection or ingestion of either altered pathogenic microorganisms or products of those microorganisms – immunization with a vaccine
Immunopathology (pg. 86) The study of immune reactions involved in disease The immune system can malfunction and cause tissue damage. Hypersensitivity Autoimmune diseases
Hypersensitivity (Cont.) (pgs. 87-88) (Table 3-3) An allergic reaction An exaggerated response Tissue destruction occurs as a result of the immune response. Four main types
Type I Hypersensitivity (pg. 87) Immediate (anaphylactic type) The reaction occurs within minutes after exposure to an antigen. Plasma cells produce IgE. IgE causes mast cells to release histamine, causing increased dilation and permeability of blood vessels and constricting smooth muscle in bronchioles of the lungs. The reaction may range from hay fever to asthma and life-threatening anaphylaxis.
Type II Hypersensitivity (pg. 87) Cytotoxic type Antibody combines with an antigen bound to the surface of tissue cells, usually a circulating RBC (red blood cell). Activated complement components, IgG and IgM antibodies in blood, participate in this type of hypersensitivity reaction. This destroys the tissue that has the antigens on the surface of its cells (e.g., Rh incompatibility).
Type III Hypersensitivity (pg. 87) Immune complex type (serum sickness) Immune complexes are formed between microorganisms and antibody in circulating blood. These complexes leave the blood and are deposited in body tissues, where they cause an acute inflammatory response. Tissue destruction occurs following phagocytosis by neutrophils.
Type IV Hypersensitivity (pg. 87) Cell-mediated type (delayed) T lymphocytes that previously have been introduced to an antigen cause damage to tissue cells or recruit other cells. Responsible for the rejection of tissue grafts and transplanted organs
Hypersensitivity to Drugs (pgs. 87-88) Drugs can act as antigens. Topical administration may cause a greater number of reactions than oral or parenteral routes. But the parenteral route may cause a more widespread and severe reaction.
Autoimmune Diseases (pg. 88) Immunologic tolerance The body learns to determine self from nonself. Autoimmune disorder The recognition mechanism breaks down; some body cells are not tolerated and are treated as foreign antigens.
Immunodeficiency (pg. 88) An immunopathologic condition A deficiency in number, function, or interrelationships of the involved WBC’s and their products May be congenital or acquired Infections and tumors may occur as a result of the deficiency.
Oral Diseases with Immunologic Pathogenesis Aphthous ulcers Urticaria and angioedema Contact mucositis and dermatitis Fixed drug eruptions Erythema multiforme Lichen planus Reactive arthritis (Reiter syndrome) Langerhans cell disease
Aphthous Ulcers (pgs. 88-91) Painful oral ulcers with an unclear cause Occur in about 20% of the population Trauma is the most common precipitating factor. May be caused by emotional stress or certain food May be associated with certain systemic diseases Thought to have an immunologic pathogenesis Occur in three forms: minor, major, and herpetiform
Minor Aphthous Ulcers (pg. 89) Discrete, round or oval ulcers Occur on movable mucosa Up to 1 cm in diameter with a erythematous halo surrounding a yellowish-white fibrin surface May have single or multiple lesions May have a prodrome of 1 to 2 days
Major Aphthous Ulcers (pgs. 89-90) Larger (>1 cm), deeper, and longer lasting than minor aphthous ulcers Very painful Occur in the posterior of the mouth more often than minor aphthous ulcers May require several weeks to heal May require a biopsy
Herpetiform Aphthous Ulcers (pgs. 89-90) Tiny (1 to 2 mm) Resemble herpes simplex ulcers Painful, generally occur in groups
Diagnosis of Minor Aphthous Ulcers (Cont.) (pgs. 89-91) (Table 3-4) Clinical appearance Location Herpetic lesions appear on mucosa fixed to bone, aphthous lesions appear on movable tissue Clinical history Aphthous ulcers do not produce systemic signs or symptoms as do herpetic lesions
Treatment of Minor Aphthous Ulcers (pg. 91) Treatment There are several OTC medications such as Orabase and Zilactin. Topical or systemic steroids may help. Topical anesthetic may help.
Urticaria (Hives) (pg. 91) Appears as multiple areas of well-demarcated swelling of skin May have itching (pruritis) Lesions caused by localized areas of vascular permeability in superficial connective tissue
Angioedema (pg. 91) Lesions caused by diffuse swelling due to increased permeability of deeper blood vessels The skin covering the swelling appears normal Usually do not have itching
Urticaria and Angioedema (pgs. 91-92) Often idiopathic cause May be due to infection, trauma, emotional stress, and certain systemic diseases May be due to ingested allergens
Contact Mucositis and Dermatitis (pg. 92) Lesions resulting from contact of an allergen with skin or mucosa Involves CMI (cell-mediated immunity) The mucosa initially becomes erythematous and edematous. Often there is burning and pruritus Later, the area becomes white and scaly. Treatment Topical and/or systemic corticosteroids
Fixed Drug Eruptions (pgs. 92-93) Lesions that appear in the same site each time a drug is introduced Generally appear suddenly after a latent period and subside when the drug is discontinued May be single or multiple slightly raised, reddish patches or clusters of macules on the skin, or sometimes the mucous membranes May have pain or pruritis
Fixed Drug Eruptions (cont.) A type of allergic reaction (Type III) Immune complexes are deposited along the endothelial walls of blood vessels. Inflammation causes vasculitis with damage to the vessel wall. This creates erythema and edema in superficial layers of skin or mucosa. Treatment The drug causing the reaction should be identified and discontinued.
Erythema Multiforme (pgs. 93-94) Cause is not clear; may be a hypersensitivity reaction Most commonly occurs in young adults, affects men more commonly than women Target lesion Characteristic skin lesion with concentric erythematous rings alternating with normal skin color