Enterobacteriaceae
Enterobacteriaceae. Enterobacteriaceae. Classification – more than15 different genera Escherichia Shigella Edwardsiella Salmonella Citrobacter Klebsiella Enterobacter Hafnia Serratia. Enterobacteriaceae. Proteus Providencia Morganella Yersinia Erwinia Pectinobacterium.

Enterobacteriaceae
E N D
Presentation Transcript
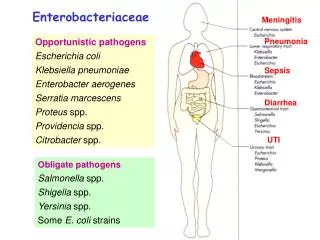
Enterobacteriaceae • Classification – more than15 different genera • Escherichia • Shigella • Edwardsiella • Salmonella • Citrobacter • Klebsiella • Enterobacter • Hafnia • Serratia
Enterobacteriaceae • Proteus • Providencia • Morganella • Yersinia • Erwinia • Pectinobacterium
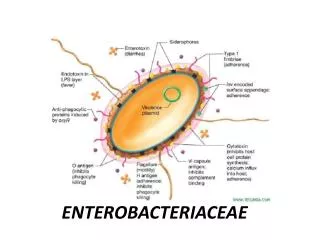
Enterobacteriaceae • Morphology and General Characteristics • Gram-negative, non-sporing, rod shaped bacteria • Oxidase – • Ferment glucose and may or may not produce gas in the process (aerogenic vs anaerogenic) • Reduce nitrate to nitrite (there are a few exceptions)
Enterobacteriaceae • Are facultative anaerobes • If motile, motility is by peritrichous flagella • Many are normal inhabitants of the intestinal tract of man and other animals • Some are enteric pathogens and others are urinary or respiratory tract pathogens • Differentiation is based on biochemical reactions and differences in antigenic structure
Enterobacteriaceae • Most grow well on a variety of lab media including a lot of selective and differential media originally developed for the the selective isolation of enteric pathogens. • Most of this media is selective by incorporation of dyes and bile salts that inhibit G+ organisms and may suppress the growth of nonpathogenic species of Enterobacteriaceae. • Many are differential on the basis of whether or not the organisms ferment lactose and/or produce H2S.
Enterobacteriaceae • On CBA they all produce similar colonies that are relatively large and dull gray. They may or may not be hemolytic. • The three most useful media for screening stool cultures for potential pathogens are TSI, LIA, and urea or phenylalanine agar. • The antigenic structure is used to differentiate organisms within a genus or species. • Three major classes of antigens are found:
Enterobacteriaceae • Somatic O antigens – these are the heat stable polysaccharide part of the LPS. • Variation from smooth to rough colonial forms is accompanied by progressive loss of smooth O Antigen. • Flagellar H antigens – are heat labile • Envelope or capsule K antigens – overlay the surface O antigen and may block agglutination by O specific antisera. • Boiling for 15 minutes will destroy the K antigen and unmask O antigens. • The K antigen is called the Vi (virulence) antigen in Salmonella typhi.
Enterobacteriaceae • Escherichia coli • Normal inhabitant of the G.I. tract. • Some strains cause various forms of gastroenteritis. • Is a major cause of urinary tract infection and neonatal meningitis and septicemia. • May have a capsule. • Biochemistry • Most are motile.
E. coli • May be hemolytic on CBA – more common in pathogenic strains • KEY tests for the normal strain: • TSI is A/A + gas • LIA K/K • Urea – • Indole + • Citrate – • Motility + • There is an inactive biotype that is anaerogenic, lactose –, and nonmotile.
E. coli • Antigenic structure - has O, H, and K antigens. K1 has a strong association with virulence, particularly meningitis in neonates. • Virulence factors • Toxins • Enterotoxins – produced by enterotoxigenic strains of E. coli (ETEC). Causes a movement of water and ions from the tissues to the bowel resulting in watery diarrhea. There are two types of enterotoxin: • LT – is heat labile and binds to specific Gm1 gangliosides on the epithelial cells of the small intestine where it ADP-ribosylates Gs which stimulates adenylate cyclase to increase production of cAMP. • Increased cAMP alters the activity of sodium and chloride transporters producing an ion imbalance that results in fluid transport into the bowel.
E. coli toxins • ST – is heat stable and binds to specific receptors to stimulate the production of cGMP with the same results as with LT.
E. coli toxins • Both enterotoxins are composed of five beta subunits (for binding) and 1 alpha subunit (has the toxic enzymatic activity).
E. coli toxins • Shiga-type toxin – also called the verotoxin -produced by enterohemorrhagic strains of E. coli (EHEC) – is cytotoxic, enterotoxic, neurotoxic, and may cause diarrhea and ulceration of the G.I. tract. • There are two types shiga-like toxin 1 and shiga-like toxin 2. • Inhibit protein synthesis by cleaving a 28S rRNA that’s part of the 60S subunit
E. coli toxins • Enteroaggregative ST-like toxin – produced by enteroaggregative strains of E. coli (EAEC) – causes watery diarrhea. • Hemolysins – two different types may be found: cell bound and secreted. • They lyse RBCs and leukocytes and may help to inhibit phagocytosis when cell bound. • Endotoxin • Type III secretion system to deliver effector molecules directly into the host cells. • Involved in inducing uptake of EIEC into intestinal cells. • Involved in development of an attachment and effacing lesion in EPEC characterized by microvilli destruction and pedestal formation.
E. coli • Adhesions – are also called colonization factors and include both pili or fimbriae and non-fimbrial factors involved in attachment (e.g. intimin). • There are at least 21 different types of adhesions. • Antibodies to these may protect one from colonization. • Virulence factors that protect the bacteria from host defenses • Capsule • Iron capturing ability (enterochelin) • Outer membrane proteins - are involved in helping the organism to invade by helping in attachment (acting as adhesion) and in initiating endocytosis.
Types of adhesions (intimin)
E. coli • Clinical significance • Is the leading cause of urinary tract infections which can lead to acute cystitis (bladder infection) and pyelonephritis (kidney infection).
Urinary tract infections (UTI) • New evidence in women who suffer from recurrent UTIs suggests that this is due to the formation of pod-like E. coli biofilms inside bladder epithelial cells. • Bacteria living on the edges of the biofilms nay break off leading to a round of infection.
E. coli infections • Neonatal meningitis – is the leading cause of neonatal meningitis and septicemia with a high mortality rate. • Usually caused by strains with the K1 capsular antigen. • Gastroenteritis – there are several distinct types of E. coli that are involved in different types of gastroenteritis: • enterotoxigenic E. coli (ETEC), • enteroinvasive E. coli (EIEC), • enteropathogenic E. coli (EPEC) , • enteroaggregative E. coli (EAEC), and • enterohemorrhagic E. coli (EHEC).
E. coli gastroenteritis • ETEC – is a common cause of traveler’s diarrhea and diarrhea in children in developing countries. • The organism attaches to the intestinal mucosa via colonization factors and then liberates enterotoxin. • The disease is characterized by a watery diarrhea, nausea, abdominal cramps and low-grade fever for 1-5 days. • Transmission is via contaminated food or water. • EPEC – Bundle forming pili are involved in attachment to the intestinal mucosa. • The type III secretion system inserts the tir (translocated intimin receptor) into target cells, and intimate attachment of the non-fimbrial adhesion called intimin to tir occurs. • Host cell kinases activated to phosphorylate tir which then causes a reorganization of host cytoskeletal elements resulting in pedestal formation and development of an attaching and effacing lesion • The exact mode of pathogenesis is unclear, but it is probably due to the attachment and effacement. • Diarrhea with large amounts of mucous without blood or pus occurs along with vomiting, malaise and low grade fever. • This is a problem mainly in hospitalized infants and in day care centers.
BFP EPEC EPEC EPEC
EPEC Tir injected
E. coli gastroenteritis • EIEC – The organism attaches to the intestinal mucosa via pili and outer membrane proteins are involved in direct penetration, invasion of the intestinal cells, and destruction of the intestinal mucosa. • There is lateral movement of the organism from one cell to adjacent cells. • Symptoms include fever,severe abdominal cramps, malaise, and watery diarrhea followed by scanty stools containing blood, mucous, and pus. • EAEC – Mucous associated autoagglutinins cause aggregation of the bacteria at the cell surface and result in the formation of a mucousbiofilm. • The organisms attach via pili and liberate a cytotoxin distinct from, but similar to the ST and LT enterotoxins liberated by ETEC. • Symptoms include watery diarrhea, vomiting, dehydration and occasional abdominal pain.
E. coli gastroenteritis • EHEC – The organism attaches via pili to the intestinal mucosa and liberates the shiga-like toxin. • The symptoms start with a watery diarrhea that progresses to bloody diarrhea without pus and crampy abdominal pain with no fever or a low-grade fever. • This may progress to hemolytic-uremic syndrome that is characterized by low platlet count, hemolytic anemia, and kidney failure. • This is most often caused by serotypes O157:H7. • This strain of E. coli can be differentiated from other strains of E. coli by the fact that it does not ferment sorbitol in 48 hours (other strains do). • A sorbitol-Mac (SMAC) plate (contains sorbitol instead of lactose) is used to selectively isolate this organism. • One must confirm that the isolate is E. coli O1547:H7 using serological testing and confirm production of the shiga-like toxin before reporting out results. • Serotypes of E. coli other than O157H7 have now been found to cause this disease
E.coli • Antimicrobic therapy- E. coli is usually susceptible to a variety of chemotherapeutic agents, though drug resistant strains are increasingly prevalent. • It is essential to do susceptibility testing. • Treatment of patients with EHEC infections is not recommended because it can increase the release of shiga-like toxins and actually trigger HUS
Shigella species • Shigella • Contains four species that differ antigenically and, to a lesser extent, biochemically. • S. dysenteriae (Group A) • S. flexneri (Group B) • S. boydii (Group C) • S. sonnei (Group D) • Biochemistry • TSI K/A with NO gas • LIA K/A • Urea – • Motility - • All ferment mannitol except S. dysenteriae • S. sonnei may show delayed lactose fermentation
Shigella species • Antigenic structure • Differentiation into groups (A, B, C, and D) is based on O antigen serotyping; K antigens may interfere with serotyping, but are heat labile. • O antigen is similar to E. coli, so it is important to ID as Shigellabefore doing serotyping. • Virulence factors • Shiga toxin – is produced by S. dysenteriae and in smaller amounts by S. flexneri and S. sonnei. • Acts to inhibit protein synthesis by inactivating the 60S ribosomal subunit by cleaving a glycosidic bond in the 28S rRNA constituents. • This plays a role in the ulceration of the intestinal mucosa.
Shigella species • Outer membrane and secreted proteins • These proteins are expressed at body temperature and upon contact with M cells in the intestinal mucosa they induce phagocytosis of the bacteria into vacuoles. • Shigella destroy the vacuoles to escape into the cytoplasm. • From there they spread laterally (Polymerization of actin filaments propels them through the cytoplasm.) to epithelial cells where they multiply but do not usually disseminate beyond the epithelium.
Shigella • Clinical significance • Causes shigellosis or bacillary dysentery. • Transmission is via the fecal-oral route. • The infective dose required to cause infection is very low (10-200 organisms). • There is an incubation of 1-7 days followed by fever, cramping, abdominal pain, and watery diarrhea (due to the toxin)for 1-3 days. • This may be followed by frequent, scant stools with blood, mucous, and pus (due to invasion of intestinal mucosa). • It is rare for the organism to disseminate. • The severity of the disease depends upon the species one is infected with. • S. dysenteria is the most pathogenic followed by S. flexneri, S. sonnei and S. boydii.
Shigella • Antimicrobial therapy • Sulfonamides are commonly used as are streptomycin, tetracycline, ampicillin, and chloramphenicol. • Resistant strains are becoming increasingly common, so sensitivity testing is required.
Salmonella • Salmonella • Classification has been changing in the last few years. • There is now 1 species: S. enteritica, and 7 subspecies: 1, 2 ,3a ,3b ,4 ,5, and 6. • Subgroup 1 causes most human infections • Clinically Salmonella isolates are often still reported out as serogroups or serotypes based on the Kauffman-White scheme of classification. • Based on O and H (flagella) antigens • The H antigens occur in two phases; 1 and 2 and only 1 phase is expressed at a given time. • Polyvalent antisera is used followed by group specific antisera (A, B, C1, C2, D, and E) • Salmonella typhi also has a Vi antigen which is a capsular antigen.
Salmonella • Biochemistry • TSI K/A + gas and H2S: S. typhi produces only a small amount of H2S and no gas , and S. paratyphi A produces no H2S • LIA K/K with H2S with S. paratyphi A giving K/A results • Urea – • Motility + • Citrate +/- • Indole - • Virulence factors • Endotoxin – may play a role in intracellular survival • Capsule (for S. typhi and some strains of S. paratyphi) • Adhesions – both fimbrial and non-fimbrial