PURPOSE
Evaluation Of RTOG Guidelines For Monte Carlo Based Lung SBRT Planning. PURPOSE. Compare Monte Carlo (MC) based lung stereotactic body radiotherapy (SBRT) plans on BrainLab iPlan treatment planning system against Pencil Beam (PB) plans and evaluate results as per RTOG 0813 guidelines. METHODS.

PURPOSE
E N D
Presentation Transcript
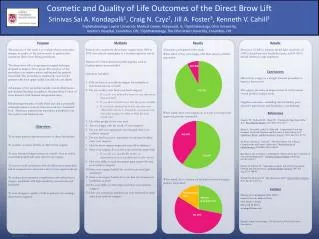
Evaluation Of RTOG Guidelines For Monte Carlo Based Lung SBRT Planning PURPOSE Compare Monte Carlo (MC) based lung stereotactic body radiotherapy (SBRT) plans on BrainLab iPlan treatment planning system against Pencil Beam (PB) plans and evaluate results as per RTOG 0813 guidelines. METHODS Twelve lung SBRT plans calculated with heterogeneity corrected PB algorithm on the Brainlab iPlan were normalized to deliver 50Gy PTV dose in 5 fractions using 8-12 non-coplanar, conformal 6MV fields. (PB) Treatment plans were then recalculated using MC algorithm without changing any beam parameters (MC Non-Optimized). Next, MUs in MC plans were optimized (MC Optimized) to satisfy PTV prescription dose at 50Gy. PTV dose parameters Dmin, Dmax, Dmean, D90, D2cm, R50% and conformality index (CI), were evaluated and compared per RTOG 0813 guidelines for PB, MC Non-Optimized and MC Optimized plans. RESULTS PB treatment plans satisfied all criteria for RTOG guidelines, without major deviations. When PB plans were recalculated using Non-Optimized MC, PTV dose was significantly less. PB PTV Dmin, D90 and Dmean exceeded MC Non-Optimized plans by 20±8%, 17±6% and 13±5% respectively (p <0.0001).(Figure 1 and 2) Joanne Zhung MD2, Edward Melian MD1, Iris Rusu MS1, Suneel Nagda MD3, Anil Sethi PhD1 1Department of Radiation Oncology, Loyola University Medical Center, Maywood, IL, 2Department of Radiation Oncology, Tufts Medical Center, Boston, MA, 3Penn Radiation Oncology, University of Pennsylvania, Philadelphia, PA PB RESULTS (cont’d) MU optimized MC plans resulted in target dose spillage leading to an increase in most dose parameters. Compared to PB, average values of Dmax, Dmean, and D90 were larger in optimized MC plans by 15±9%, 9±4%, 4±3% (p≤0.0009). Similarly, D2cm, R50% and CI were also higher in optimized MC plans resulting in major deviations in RTOG guidelines. Maximum increase (mean 35%, max 59%) was observed in R50% compared to PB plans. The greatest differences were seen in targets surrounded completely by lung tissue, see Figures 3. MC RUL T1aN0 NSCLC, 10.7cm3 PTV 9 non-coplanar 6MV beams Pencil Beam MC Non-optimized MC Optimized Volume (% of PTV) Figure 3. CT planning scans comparing isodose lines (IDL) for the 3 plans. ITV and PTV depicted. Note only 90% IDL (yellow) covers ITV for MC Non-optimized. Figure 2. DVH comparison of PB vs. MC (Non-Optimized) CONCLUSIONS Treatment plans generated with PB dose algorithm lead to significant target under-dosage, when recalculated using MC. When treatment plans were optimized using MC, RTOG protocol criteria could not be satisfied for most patients. Based on the above results, RTOG 0813 constraints should be revised in light of treatment plans performed using sophisticated dose calculation algorithms such as MC. If revised constraints do not provide clinical value, novel dose parameters may need to be investigated. Figure 1. Mean and Range for PTV Dmax, Dmean, Dminin three treatment plans. Table 1. RTOG 0813 major deviations, in red When MUs were optimized for PTV coverage in MC plans, RTOG guidelines could not be satisfied (Table 1). All patients had at least minor deviations in RTOG parameters, with major deviations in red, above. DOSE (%)