Comprehensive Guide to Childhood and Adolescent Immunizations
This guide provides essential information on immunization processes for childhood and adolescent health. It outlines the importance of both natural and artificial exposure to pathogens, the recommended vaccination schedule, and details on specific vaccines like Hepatitis B, DTaP, MMR, and HPV. Special focus is given to the timing of doses, protective strategies like cocooning against pertussis, and the significant role of vaccinations in preventing serious diseases such as meningitis and pneumonia. Staying informed is crucial for safeguarding public health.

Comprehensive Guide to Childhood and Adolescent Immunizations
E N D
Presentation Transcript
Immunizations Childhood and Adolescent Jan Bazner-Chandler CPNP, MSN, CNS, RN
What Immunization Is • Immunization is the process by which a subject is rendered immune or resistant to a specific disease • Natural exposure – contact with the agent • Artificial exposure – parts of the infectious agent or inactivated version is given for the purpose of becoming immune to the disease agent it causes.
Childhood Immunization • Childhood immunization schedule American Academy of Pediatrics • http://www.cispimmunize.org/ • Download children age 0 - 6 • Download children age 7 - 18 American Academy of Pediatrics: protect tomorrow initiative: http://www.aap.org/protecttomorrow/
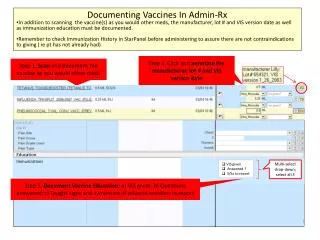
Hepatitis B (HepB) Vaccine • All infants should receive the first dose soon after birth or before hospital discharge. • Second dose should be given at least 4 weeks after the first • Third dose 16 weeks after the first dose and at least 8 weeks after the second dose • Infants born of HBsAg-postive mothers should receive first immunization within 12 hours of birth as well as HBIG.
Diphtheria, Tetanus, Acellular Pertussis • DTaP • Given at 2, 4 and 6 months • 4th dose between 15 and 18 months • Last DTaP at the 4-6 year pre-K check up • 1st Tdap at age 11-12 years or at least 5 years from last DTap • Tetanus every 10 years after that
Cocooning • New term for 2010 • Strategy to protect the newborn up to 6 month old from pertussis or “whooping cough” • Booster available for adults Tdap • The goal to immunize all adults who interact with infants to prevent pertussis
Polio • Injection form given at 2 months, 4 months after 6 months and at kindergarten check-up • Oral not given due to shedding virus in stool
Haemophilus Influenza Type b • Hib • Given at ages 2 and 4 months and 12 months • Any child entering child care or pre-kindergarten under age 5 years in California are required to have Hib. • Not a standard immunization for children born outside the USA
Why? • Haemophilus influenzae type B (Hib) disease is a serious disease caused by bacteria. It usually strikes children under 5 years of age. • Leading cause of bacterial meningitis in children under 5 years • Pneumonia • Epiglottitis – severe swelling of epiglottis – resulting in death for obstruction of breathing • Before Hib immunization 20,000 children per year had the infectious disease with 1000 deaths per year.
Measles, Mumps, Rubella • MMR • Two doses: • 1st 12 months or older • 2nd dose kindergarten visit • If no record of second dose it should be given at 11 to 12 year old visit • May develop a rash a week to ten days after immunization • Not immunized against wild strain – exposure would bring milder case
Mumps outbreak • 2010 in New York 1500 Orthodox Jews over had case of mumps during a 7 month period. • One un-immunized child at camp from England spread the disease. • Why a problem? • Complications • Hearing loss • Testicle swelling - infertility
Varicella • Chicken pox – recommended at 12 – 15 months and second dose at 4-6 years or kindergarten visit • Un-immunized children over 13 years would receive two doses at least 4 weeks apart
Varicella • Contraindication: allergy to immunization, pregnancy or possibility of pregnancy within 4 wks • Children on high dos immunosuppressive therapy or immunocompromised HIV / AIDS – vaccination can be given if CD4 T-lymphocyte percentages or 15% or greater. • Precautions: • if blood, plasma or immune globulin given within the past 11 months. • Antiviral drugs 24 hours before or 14 days after immunization
Chicken Pox Parties • Fact or fiction?
Pneumococcal Vaccine • PCV - Prevnar • Recommended for all children 2 to 23 months and certain populations up to 59 months • 2, 4, 6 and 4th dose after 12 months of age • High risk populations • Asthma • Sickle cell anemia • Cystic fibrosis
Human Papillomavirus • HPV is the most common sexually transmitted virus • 40 types of HPV • Spread through sexual contact • Can cause cervical cancer • Can also cause genital warts
Human Papillomavirus • HPV series • Recommended for all girls 11-12 years • Can be given as young as 9 years • Get HPV before first sexual contact and by 26 years of age • 1st dose • 2nd dose 2 months after 1st dose • 3rd dose 6 months after dose one
HPV • Contraindications: • Allergy to yeast or reaction to first immunization • HPV will not help if already infected
Meningococcal meningitis • Meningococcal disease is a serious illness • Leading cause of bacterial meningitis in 2 – 28 year old in USA • Also called Neisseria meningtides • High risk populations • High school students • College age students • Military – boot camp • Travel to third-world countries
Meningococcal polysaccharide Vaccine • MPSV4 • Prevents 4 types of meningococcal diseases – 2 out of 3 of the most common strains seen in the US
Recommendations • MPSV4 recommended for all children at their routine preadolescent visit (11 – 12 years) • College freshmen living in dorms • U.S. military recruits • Traveling to Africa • Persons exposed to meningitis outbreak
Influenza (Flu) Vaccine • “Flu shot”: Inactivated vaccine containing the virus • Approved for infants older than 6 months • Nasal spray flu vaccine: live, weakened flu viruses • Approved for children over 5 years to 49 years.
When to get Flu Vaccination? • October or November yearly
Contraindications to Flu Vaccine • Children with severe allergy to chicken eggs. • Severe reaction to influenza vaccination in the past. • Less than 6 months of age. • Children who have developed Guillain-Barre syndrome after previous immunization. • Do not give if child has moderate to severe illness with fever until a later date.
Rotavirus • Rotavirus causes severe diarrhea • Rotarix (RV1) or RotaTeq (RV5) given at 2, 4 and 6 months • First dose may be given as early as 6 weeks • Give final dose no later than 8 months of age • Contraindications: allergy to previous immunization or allergy to latex (use RV5) • Precaution: moderate or severe illness, moderate to severe acute gastroenteritis or pre-existing gastrointestinal disease or history of Intussusception
Premature Infants • AAP currently recommends that all premature infants receive full dose immunizations at the same chronologic age as term infants even if hospitalized • Contraindications include: significant febrile seizure, active seizure disorders, encephalopathy (DTaP) • Infants with BPD (Bronchopulmonary dysplasia) or RAD (Reactive Airway Disease) should receive influenza immunizations • Infants with congenital heart and premature infants immunization against Respiratory Syncytial Virus or RSV.
Premature continued • Hepatitis B may be deferred until discharge unless mother is Hep B positive • Do NOT dilute dosages • Usually given when they reach at least 2 kg or 4.4 pounds
To Immunize or Not to Immunize • Children on antibiotics • Children with minor illness – otitis, cough, diarrhea, sore throat, low grade fever • Children with mild allergies • Breast feeding infants • Children with pregnant household contacts
True Contraindications • True allergic response • Rash or hives after previous vaccination • Allergy to eggs or egg products should not be given influenza vaccination
Reactions to Immunizations • Fever greater than 103, shock or collapse, or inconsolable crying for greater than 3 hours. (DTaP) • Low grade fever, fussiness, and soreness at injection site are not reasons to prevent further vaccinations • Mild rash or fever may occur 10 days to 2 weeks after MMR or Varicella
Interventions • Tylenol every 4 hours for fussiness or low grade fever • Warm bath • NO ASPIRIN • NO Motrin for infants under 6 months of age • AAP recommends Tylenol for all ages due to confusion in dosing.
Adolescents • Hepatitis A (recommended only) • Pneumococcal if they have any chronic disease: heart, sickle cell disease, cystic fibrosis, diabetes, or organ transplant or receiving chemotherapy • Hepatitis B • MMR: second booster • D Tap • Varicella if no reliable history or negative titers • Meningococcemia for all college freshman and all military • Influenza yearly
Hepatitis A • Recommended for children and adolescents living in selected states or regions and for certain high risk groups • This would include California, Texas, and Arizona • 2 doses 6 months apart
L.A. Unified Recommendations • Complete health and immunization record • All new students must have written results of a PPD test for tuberculosis within 12 months • If PPD is positive a chest x-ray is recommended • Treatment is recommended unless the child has some immune suppressed condition.
PPD Waiver • I hear by request exemption of the child from the tuberculosis assessment requirement for school / childcare entry because this is contrary to my beliefs. I understand that should there be cause to believe that my child is infected with active TB or should there be a tuberculosis outbreak, my child may be temporarily excluded from school.
Pre-school and Child Care • Pre-kindergarteners must be immunized against Haemophilus influenza type B or Hib. • This is not a standard immunization for children born outside the United States • Hib would not be required for a child over 5 years of age.
Kindergarten • Second MMR: Measles, Mumps, Rubella • Hepatitis B • Hepatitis A in high risk areas • D Tap: tetanus, diphtheria, pertussis
Communicable Diseases • Chicken pox (varicella) • Measles (Rubeola) • Pertussis (Whooping Cough) • Rubella (German Measles) • Scarlet Fever • Mumps
Varicella • Agent: varicella zoster virus • Incubation: 10 – 14 days • Transmission: respiratory • Period of communicability: 2 days before eruption of vesicles until lesions crusted. • Prodromal phase: slight fever, malaise, pruritic rash; macular to papular to vesicular.
Varicella • Communicability: children who have “chicken-pox” are infectious for two days before the vesicles erupt until all vesicles are crusted over (about 5 days).
Management of Varicella • Isolation • Skin care: tepid bath, calamine lotion, clip finger nails. • Keep from scratching • Antihistamines for itching - Benadryl • No ASA (salicylate containing products) – acetaminophen only. • Varicella vaccine now available.
Reyes Syndrome • Almost always preceded by a viral illness, URI, Flu, chickenpox • Linked to the use of aspirin or aspirin containing medications (salicylates) • Assessment • Persistent vomiting • Lethargy or sleepiness • Confusion, irrational or combative behavior • Seizures to coma
Measles or Rubeola • Agent: Virus • Transmission: respiratory, blood and urine • Incubation period: 10 to 20 days • Period of Communicability: 4 days before and 5 days after rash appears. • Prodromal stage: fever, cough, conjunctivitis, Koplik spots.
Rubella or German Measles • Agent: Rubella virus • Source: nasopharyngeal secretions; secretions in blood, stool, and urine. • Transmission: direct contact. • Incubation period: 14 to 21 days • Period of communicability: 7 days before to 5 days after appearance of rash.