Functional Human Physiology for Exercise and Sport Sciences The Urinary System: Renal Function
950 likes | 1.56k Views
Functional Human Physiology for Exercise and Sport Sciences The Urinary System: Renal Function. Jennifer L. Doherty, MS, ATC Department of Health, Physical Education, and Recreation Florida International University. Functions of the Urinary System.

Functional Human Physiology for Exercise and Sport Sciences The Urinary System: Renal Function
E N D
Presentation Transcript
Functional Human Physiologyfor Exercise and Sport Sciences The Urinary System: Renal Function Jennifer L. Doherty, MS, ATC Department of Health, Physical Education, and Recreation Florida International University
Functions of the Urinary System • The kidneys remove metabolic wastes from the blood and excrete them to the outside of the body in the form of urine • The careful regulation of renal activity keeps blood composition and body fluids within normal limits
The kidneys also… • Maintain electrolyte and acid-base balance in body fluids • Regulate plasma pH by regulating the concentration of bicarbonate ions and hydrogen ions • Regulate the volume, composition, and pH of blood • Regulate plasma osmolarity and chemical composition • Assist in the regulation of BP • Regulate plasma volume and produces renin to regulate BP • Assist in the regulation of RBC production • Regulate RBC production by producing erythropoietin to stimulate RBC formation in bone marrow • Assist in the regulation of Ca++ absorption • Metabolize vitamin D to its active form, which affects the rate of Ca++ absorption from the small intestines
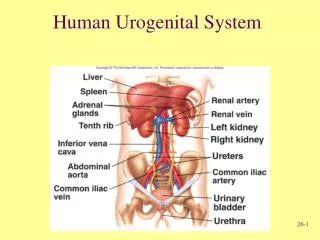
Anatomy of the Urinary System Structures of the urinary system • Kidneys (2) • Form urine • Renal arteries and veins • Ureters (2) • Tubes for transport of urine from the kidneys to the bladder • Urinary bladder (1) • Storage reservoir for urine • Urethra (1) • Transport tube for urine to the outside of the body
Microscopic Anatomy of the Kidneys • The nephron is the structural and functional unit of the kidney. • Each kidney contains about one million nephrons • Nephrons consist of: • The renal corpuscle • Proximal convoluted tubule • Loop of Henle • Distal convoluted tubule • Collecting duct • Empties urine into the minor calyx
The Nephron: Renal Corpuscle • The renal corpuscle consists of… • Glomerulus • Glomerular Capsule
The Nephron: Renal Corpuscle • The Glomerulus is the filtering unit of the nephron • Tangled cluster of capillary beds lying between the afferent and efferent arterioles • Contained within the glomerular capsule
The Nephron: Renal Corpuscle • The Glomerular Capsule (Bowman’s capsule) is a thin walled, cup-shaped structure surrounding the glomerulus • It leads to the renal tubule • It receives fluid that filters through the glomerulus
Basic Renal Exchange Processes • Nephrons function to… • Remove wastes from the blood • Regulate water and electrolyte concentrations • Urine is the end product of these functions • The following 3 exchange processes occur within the nephrons • Glomerular Filtration • Reabsorption • Secretion
Glomerular Filtration • This is the beginning of urine formation • Glomerular capillaries are extremely permeable compared to systemic capillaries • Hydrostatic and Osmotic Pressure Gradients • Greater inside glomerular capillaries • Forces water and dissolved solutes to leave the blood plasma in the glomerular capillaries and cross the glomerular membrane into the glomerular (Bowman’s) capsule • Filtrate • Water and dissolved solutes in the glomerulus
Glomerular Filtration The glomerular membrane • Separates glomerular capillary blood from the glomerular capsule space • Contains many small pores that allow almost all materials to pass through the membrane • Exceptions: formed elements
Glomerular Filtration Glomerular filtrate • Contains water and dissolved solutesthat have been filtered from the blood plasma in the glomerular capillaries and collected by the glomerular capsule • Similar to tissue fluid containing water, glucose, amino acids, urea, uric acid, creatine, creatinine, sodium, chloride, potassium, calcium, bicarbonate, phosphate, and sulfate ions • Will be processed by the renal tubules to form urine
Glomerular Filtration • A nonselective, passive process • Water and dissolved solutes from the blood plasma in glomerular capillaries are forced through the glomerular membrane by hydrostatic and osmotic pressure gradients • Water and dissolved solutes travel down their pressure gradients
Glomerular Filtration Glomerular Filtration Pressure (Net Filtration Pressure) • The net force acting to move materials out of the glomerulus (glomerular capillaries) and into the glomerular capsule • Filtration pressure is much higher in the glomerular capillaries compared to systemic capillaries because of: • The high permeability of the glomerular membrane • It is more permeable than systemic capillary membranes • High glomerular blood pressure (60 mmHg) • It is higher compared to systemic capillary blood pressure (41 mmHg)
Glomerular Filtration Starling Forces • Represent the overall effect of all the forces operating at the glomerular membrane
Glomerular Filtration: Starling Forces • Forces favoring filtration are the forces driving fluid and solutes out of the glomerular capillaries • Glomerular capillary hydrostatic pressure • PGC = 60 mmHg • The primary force pushing water and solutes out of the glomerular capillaries • Osmotic pressure in the glomerular (Bowman’s) capsule • πBC = 0 mmHg • Negligible since few plasma proteins are normally present in the glomerular capsule
Glomerular Filtration: Starling Forces • Forces opposing filtration are the forces driving fluid and solutes back into the glomerular capillaries • Glomerular (Bowman’s) capsule hydrostatic pressure • PBC = 15 mmHg • Exerted by the fluids within the glomerular capsule • Osmotic pressure in the glomerular capillaries • πGC = 29 mmHg • Due to the plasma proteins in glomerular blood
Glomerular Filtration Pressure • Glomerular Filtration Pressure Equation • Filtration pressure = (forces favoring filtration) - (forces opposing filtration) • Forces favoring filtration • (glomerular capillary hydrostatic pressure + capsular osmotic pressure) • Forces opposing filtratrion • (capsular hydrostatic pressure + glomerular capillary osmotic pressure) • Values • (60 mmHg + 0 mmHg) - (15 mmHg + 29 mmHg) = 16 mmHg
Glomerular Filtration Rate (GFR) • GFR = the amount of filtrate produced in the kidneys per minute • Normal values: • 125 ml/min (180 L/day) • GFR varies with the filtration pressure • All the factors that affect glomerular filtration pressure will affect the GFR • Glomerular capillary osmotic pressure • Glomerular capillary hydrostatic pressure • Glomerular capsule osmotic pressure • Glomerular capsule hydrostatic pressure
Glomerular Filtration Rate (GFR) • Glomerular capillary hydrostatic pressure • ↑ glomerular capillary hydrostatic pressure = ↑ GFR • Glomerular capsule osmotic pressure • ↑ glomerular capsule osmotic pressure = ↑ GFR • Glomerular capillary osmotic pressure • ↑ glomerular capillary osmotic pressure = ↓ GFR • Glomerular capsule hydrostatic pressure • ↑ glomerular capsule hydrostatic pressure = ↓ GFR
Glomerular Filtration Rate (GFR) • GFR varies with the rate of blood flow through the glomerular capillaries • To maintain a high GFR, blood must flow quickly through glomerular capillaries • Vasocontriction or vasodilation in the glomerular arterioles elicit changes in the glomerular filtration pressure • Changes in the glomerular filtration pressure effect GFR
Glomerular Filtration Rate (GFR) • Vasoconstriction of the afferent arterioles or vasodilation of the efferent arterioles • ↓ glomerular capillary hydrostatic pressure • ↓ GFR • Vasodilation of the afferent arterioles or vasoconstriction of the efferent arterioles • ↑ glomerular capillary hydrostatic pressure • ↑ GFR
Regulation of GFR • GFR remains relatively constant • May be ↑ or ↓ according to the body’s need • Mechanisms of regulation: • Intrinsic control (Autoregulation) • Myogenic regulation • Tubuloglomerular feedback • Extrinsic control • Renal blood flow • Exercise
Regulation of GFR: Intrinsic Control • The ability of the kidney to maintain a constant blood flow when arterial BP is changing • The ability of the kidneys to maintain a relatively constant GFR when mean arterial pressure is changing • This mechanism is effective over the "normal" range of arterial BP • 80 - 120 mmHg
Regulation of GFR: Intrinsic Control Myogenic Regulation • Related to the inherent property of smooth muscle to contract when stretched • ↑ mean arterial pressure = ↑ stretch of smooth muscle in the afferent arteriole walls stimulating vasoconstriction • Vasoconstriction of the arterioles causes a decrease in glomerular capillary hydrostatic pressure • This protects the delicate glomerular capillaries from high mean arterial pressures • Myogenic regulation is especially effective in the afferent arteriole
Regulation of GFR: Intrinsic Control Tubuloglomerular Feedback • Negative feedback system • GFR is regulated by changes in flow of tubular fluid past the macula densa • Specialized cluster of epithelial cells in the distal convoluted tubule near the afferent and efferent arterioles • Changes in Na+ andCl- concentration in the filtrate are detected by osmoreceptors in the macula densa
Tubuloglomerular Feedback Macula Densa Cells • Respond to changes in the Na+Cl- concentration in the filtrate in the distal convoluted tubule • ↓ Na+Cl- concentration = afferent arteriole vasodilation • Vasodilation of the afferent arteriole results in: • ↑ blood flow to the glomerular capillaries • ↑ glomerular filtration pressure • ↑ GFR • The opposite is also true
Tubuloglomerular Feedback Juxtaglomerular Cells • Contain mechanoreceptors that stimulate the juxtaglomerular cells to release renin in response to changes in mean arterial pressure • Renin is an enzyme that catalyzes a cascade of reactions in the bloodstream • Renin converts angiotensinogen → angiotensin I • Angiotensin converting enzyme (ACE) converts angiotensin I → angiotensin II • Angiotensin II is the most powerful vasoconstrictor in the body • Increases mean arterial blood pressure
Tubuloglomerular Feedback • Activation of the juxtaglomerular cells to release renin occurs when there is a decrease in mean arterial pressure • Usually when mean arterial pressure is less than 80 mmHg • Direct activation of juxtaglomerular cells • Achieved via the mechanoreceptors sending impulse through the sympathetic nervous system • Indirect activation of juxtaglomerular cells • Achieved via the macula densa cells which detect changes in Na+Cl- concentrations in the filtrate • Macula densa cells cause vasoconstriction or vasodilation, which alters mean arterial pressure as detected by the juxtaglomerular cells
Regulation of GFR: Extrinsic Control Renal Blood Flow • The sympathetic nervous system is able to override autoregulation of the kidneys • ↑ sympathetic input = ↓ GFR • Sympathetic input causes vasoconstriction of both afferent and efferent arterioles, thereby decreasing GFR
Regulation of GFR: Extrinsic Control Exercise • Exercise results in increased sympathetic nerve impulses • Sympathetic nerve impulses stimulate the adrenal medulla to release epinephrine, which stimulates… • Release of renin = ↑ mean arterial pressure • Vasoconstriction of the afferent arteriole = ↓ GFR
Reabsorption • The process of reclaiming fluid and solutes from the filtrate in the renal tubules • Reabsorption occurs in the peritubular capillaries • Solutes and water move from the lumen of the renal tubules back into the plasma • If reabsorption did not occur, a person would lose 1L of fluid in the urine in 8 min
Solute Reabsorption • Substances are selectively reabsorbed from the filtrate • Peritubular capillaries are specially adapted for the process of reabsorption • Under very low BP • Walls are very permeable • Reabsorption occurs throughout the renal tubule; however, most reabsorption occurs in the proximal convoluted tubule
Solute Reabsorption: Proximal Convoluted Tubule • Most reabsorption occurs in the proximal convoluted tubule • Proximal convoluted tubule contains epithelial cells with microvilli • Microvilli increase the surface area within the renal tubules
Solute Reabsorption: Proximal Convoluted Tubule • Solutes are moved from the tubule lumen, across the apical membrane, into the epithelial cells lining the tubule walls
Solute Reabsorption: Proximal Convoluted Tubule • Solutes then move out of the epithelial cells lining the tubule walls, across the basolateral membrane, into the peritubular space
Solute Reabsorption: Proximal Convoluted Tubule • From the peritubular space, solutes easily diffuse into the peritubular capillaries
Regional Specialization of the Renal Tubules: Proximal Tubule • Na+ ions are actively reabsorbed by active transport • Requires ATP • Reabsorption of Na+ establishes an electrical gradient for reabsorption of negatively charged ions • As positively charged Na+ ions are transported out of the filtrate, negatively charged ions accompany them via passive diffusion • Cl- • Bicarbonate (HCO3-) • Reabsorption of Na+ also establishes an osmotic gradient for the reabsorption of water • Water is passively reabsorbed by osmosis and returned to the systemic circulation by the peritubular capillaries
Regional Specialization of the Renal Tubules : Proximal Tubule • The mechanisms of reabsorption in the proximal tubule are so efficient that 70% of water and Na+ filtered is reabsorbed before the tubular fluid reaches the loop of Henle • Water and Na+ reabsorption are regulated by several hormones • At the end of the proximal convoluted tubule, the filtrate and the blood in the peritubular capillaries are isotonic (electrically neutral)