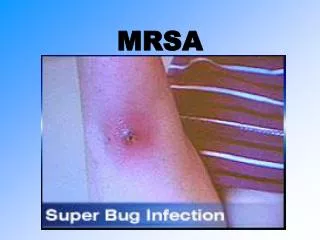
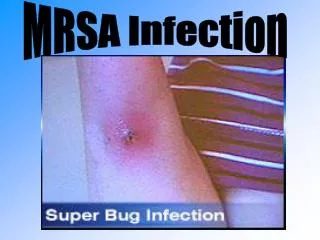
CA-MRSA Skin Infection
400 likes | 737 Views
CA-MRSA Skin Infection. Ann McBride, M.D. June 9, 2004. No financial disclosures HUGE thanks to Patty Boyle. 17 yo high school student, daughter of UW surgeon, with MRSA furunculosis 36 yo F 6 wks after hysterectomy developed extensive furunculosis and skin abscess

CA-MRSA Skin Infection
E N D
Presentation Transcript
CA-MRSA Skin Infection Ann McBride, M.D. June 9, 2004
17 yo high school student, daughter of UW surgeon, with MRSA furunculosis • 36 yo F 6 wks after hysterectomy developed extensive furunculosis and skin abscess • 51 yo Type 1 DM with chronic neurodermatitis, 2 mos after hospitalization for CAP has + MRSA skin lesions.
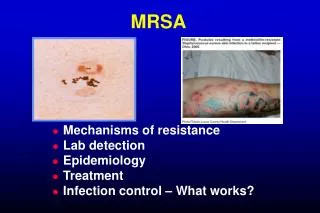
OBJECTIVES • Clinical Characteristics CA-MRSA • Biological Characteristics CA-MRSA • Treatment of MRSA Skin Infection • Prevention of Recurrences
Major Staph clinical syndromes : skin-related infections, cellulitis, osteomyelitis, septic arthritis, TSS, pneumonia Transmission: person-to-person contact from individual with Staph infection or colonization. Can be transmitted from contact with contaminated environment. Can remain days (more than a week) Airborne transmission is prob not frequent route
S aureus frequently part of transient flora. Among healthy individuals, carrier rates est 10 – 30% Common carrier sites of S.aureus : anterior nasal vestibule skin - axilla, perineum- hair, nails
Duration of carrier state – several months Mean duration 8-9 months; can last years Hospital personnel and individuals with chronic skin condition often have higher rates and longer duration of colonization
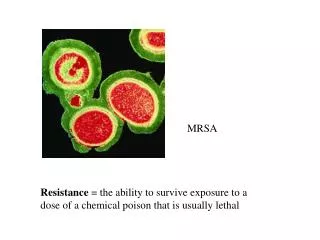
MRSA first described nosocomial pathogen 1960’s MRSA = ORSA resistance to all B-lactams, & cephalosporins 1990’s CA-MRSA vs HCA-MRSA
CA-MRSA(excludes dx of HCA-MRSA) • Dx in outpt setting or culture + MRSA within 48 hrs after hospital admission • No history previous MRSA • No hospitalization or exposure to health care facility within previous year • No permanent indwelling catheter
In 2000 CDC surveillance to characterize clinical, micro- biological, and molecular features of CA-MRSA and HCA- MRSA
JAMA Dec 2003 Comparison of CA-MRSA vs HCA-MRSA 12 labs in MN ½ metropolitan ½ non-metro All labs served inpt and outpt 10/12 Adults and Peds 1/12 Peds only
MN Surveillance: ¼ all S. aureus cultures = MRSA 1100/4612 Range 10-49% Among MRSA: 85% HCA 12% CA 3% unclear
MN Surveillance: Of CA-MRSA 53% metropolitan 47% non-metro Younger median age of CA-MRSA vs HCA-MRSA 30 yo vs70 yo
mecA gene required for MRSAmecA gene codes PBP 2aPcn Binding Protein low affinity for B-lactams Thus, more resistant to B-lactams.
Difference in exotoxin genes between CA- and HCA MRSA PVL (Panton Valentine Leukocidin) gene: * common in CA MRSA (20/26 vs. 1/26) esp. skin infections, necrotizing pneumonia * codes for Cytotoxin disrupts cell membrane; cause severe tissue necrosis, destruction WBCs * facilitates MRSA penetration of intact skin
Frequency of MRSA colonization not addressed • ** 500 otherwise healthy children seen UCCH 1996; 132 colonized with S. aureus • 11/132 (8.3%) were MRSA
Pt #1 17 yo recurrent furunculosis Fall 2003 Dau of UW surgeon abscess L arm +MRSA dau’s skin wound & nares culture +MRSA - DM, Skin dz, needle use hs swim team; no skin infctn among teammates 2 households – only father and my pt +MRSA grandmother in nursing home
Impr: colonized w/ MRSA and recurrent furunculosis Management: Decolonization End of swim team participation Treatment of recurrent furuncles --minocycline + rifampin x 2 wks
Decolonization for CA-MRSA • Generally NOT recommended for single case MRSA infection • Consider for recurrent MRSA infection (3 or more infections in 6 months)
Decolonization Mupirocin ointment anterior nares “match head size” ½ anterior vestibule one nostril ½ anterior vestibule other nostril Press sides of nose together Gently massage bid x 5 days (to 14??); one week later f/u nasal culture if nasal culture +MRSA repeat once no more than 3 mupirocin treatments
Purell hand cleansing Bath/shower daily with antiseptic Wet skin thoroughly Body wash – chlorhexidine (Rx Hibiclens) Apply disinfectant soap with moistened face cloth Caution: Skin irritation ? Substitute tree oil cleanser
Pat skin dry gently; avoid abrading skin • Use moisturizer while skin is moist after bathing • Consider D/C shaving temporarily • Avoid tightly fitting clothes/bands could rub skin
Environment Launder • Hot water • Bed sheets, towels, wash cloths Dryer (med to high heat) for clothes -- not air drying Wipe down bathroom and kitchen counters, and handles –refrigerator, doors, cabinets (bleach)
Outbreaks CA-MRSA described in various populations including participants in sports. Risk factors for Staph infections in athletes: Contact with lesions of other players Skin trauma Sharing of sports equipment
CDC’s Recommendations for Preventing Staph Infections • Cover all wounds. If a wound cannot be covered adequately, consider excluding player until lesions healed • Encourage good hygiene—showering w/ soap after all practices and competitions • Ensure availability of soap and hot water • Discourage sharing of towels, clothing, and equipment • Establish routine cleaning schedule for shared equipment • Educate athletes and coaches re: potentially infectious skin lesion • Encourage early reporting/assessment for skin lesions
With recurrence minocycline + rifampin clindamycin + rifampin TMP-SMX + rifampin Minocycline has excellent skin penetration Rifampin + atbtc to reduce emergence of resistance
Lecture by Dr. Maki If furuncle appears to develop, apply liberal amount of OTC Bacitracin ointment Apply Tegaderm (Transparent polyurethene dressing) This maintains high concentration of drug in lesion x 3-4 days
Pt #2 36 yo woman undergone hysterectomylate summer 2003. Developed “bug bites”buttocks and thighs fall 2003Gyn treated ceph Next day, came to IM “no better” ; R leg furuncle had small amt of purulent drainageDiclox initiated, skin lesion +MRSA
RTC 48 hrs; Lesion had drained and improved after draining.Diclox D/C’d; No systemic antibioticDecolonization effort and topical/local treatment of recurrence per Dr. Maki’s recommendationOne additonal lesion, did not require po atbtcF/up surveillance cultures negative x 3
+ MRSA Patient Presenting to Clinic • Pt placed directly into exam room • Need not be negative flow • Door may remain open • Gown, gloves required if touching pt or any item in room • Mask not usually required (unless +MRSA nares w/ URI)
Gown, gloves left in room Stethoscope cleansed with ETOH Purell hand cleansing before exiting Room closed until housekeeping cleanses/disinfects
MRSA precautions in clinic cannot be lifted until three sets of neg surveillance cx • On order card check “MRSA Screen” • Each set obtained at least one week apart • Swabs from L & R nares combined (single swab for both nares) • Swabs from axilla and groin can be combined (single swab for both axillae and both sides of groin)
No role for attempting mupirocin or systemic (oral antibiotics) decolonization in pt with chronic skin condition
Patient #3 50 yo Type 1 DM w/ neurodermatitis chronically excoriated skin hospitalized Nov 2002 with pneumonia In Dec 2002, MD in neuroderm clinic +MRSA arm lesion Early 2003 – appt in IM Clinic; WISCR = +MRSA No attempt to decolonize 2003 – 2 small skin abscesses I & D; Consult w/ ID- rec decolonization attempt to decrease bioburden Decolonization effort has worsened dermatitis
Three patients -- all three “HCA-MRSA” -- yet clinical presentation assoc with CA-; atbtc susc pattern ‘typical’ for CA-MRSA Clinical importance/helpfulness of this distinction???
Clinical setting most predictive of S aureus infection. Clinical syndromes CA-MRSA – typically, skin infections, cellulitis, abscess – closely resemble clinical syndrome of MSSA in community Atbtc selection depends upon susc pattern
Management Future – PCR testing for mecA gene to est MRSA sooner??