ABO Blood Group System
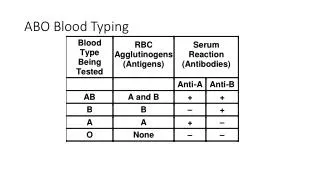
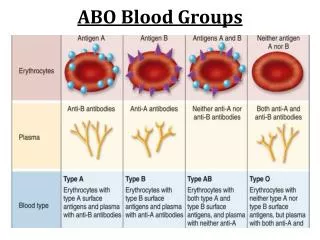
ABO Blood Group System. History: Karl Landsteiner. Discovered the ABO Blood Group System in 1901 He and his five co-workers began mixing each others red cells and serum together and inadvertently performed the first forward and reverse ABO groupings. Why is it important?.

ABO Blood Group System
E N D
Presentation Transcript
History: Karl Landsteiner • Discovered the ABO Blood Group System in 1901 • He and his five co-workers began mixing each others red cells and serum together and inadvertently performed the first forward and reverse ABO groupings
Why is it important? • ABO compatibility between donor cell and patient serum is the essential foundation of pretransfusion testing • It is the only system with expected antibodies • Whether they are IgG or IgM, ABO antibodies can activate complement readily • This means that incompatibilities can cause life threatening situations (transfusion reactions)
ABO antigens: Biochemical & Genetic Considerations
ABO and H Antigen Genetics • Genes at three separate loci control the occurrence and location of ABO antigens • The presence or absence of the A, B, and H antigens is controlled by the H and ABO genes
The presence or absence of the ABH antigens on the red blood cell membrane is controlled by the Hgene • The presence or absence of the ABH antigens in secretions is indirectly controlled by the Se gene
ABO Antigen Genetics • H gene – H and h alleles (h is an amorph) • Se gene – Se and se alleles (se is an amorph) • ABO genes – A, B and O alleles
H Antigen • The H gene codes for an enzyme that adds the sugar fucose to the terminal sugar of a precursor substance (PS) • The precursor substance (proteins and lipids) is formed on an oligosaccharide chain (the basic structure)
Type I and Type II Precursors • There are two potential precursors substances for ABH antigens Type I and Type II • Both are comprised of identical sugars but the linkage of the terminal sugars differs in the two types • Type I precursor has a terminal galactose linked to a subterminal N-acetylgluosamine in a 1-3 linkage • These same sugars combine in a 1-4 linkage in type II precursor • ABH Ags on red cells are derived from Type II chains whereas the ABH Ags in plasma are made from both types I & II precursors
Type II H • After fucose is added to Type II chains, the structure is termed Type II H • Four kinds of Type II H have been identified • H1, H2 are simple straight chain glycolipids • Whereas H3 & H4 have branched chains
RBC Precursor Structure RBC Glucose Galactose Precursor Substance (stays the same) N-acetylglucosamine Galactose
Formation of the H antigen RBC Glucose H antigen Galactose N-acetylglucosamine Galactose Fucose
H antigen • The H antigen is the foundation upon which A and B antigens are built • A and B genes code for enzymes that add a sugar to the H antigen • Immunodominant sugars are present at the terminal ends of the chains and confer the ABO antigen specificity
A and B Antigen • The “A” gene codes for an enzyme (transferase) that adds N-acetylgalactosamine to the terminal sugar of the H antigen • N-acetylgalactosaminyltransferase • The “B” gene codes for an enzyme that adds D-galactose to the terminal sugar of the H antigen • D-galactosyltransferase
Formation of the A antigen RBC Glucose Galactose N-acetylglucosamine Galactose N-acetylgalactosamine Fucose
Formation of the B antigen RBC Glucose Galactose N-acetylglucosamine Galactose Galactose Fucose
Genetics • The H antigen is found on the RBC when you have the Hh or HH genotype, but NOT from the hh genotype • The A antigen is found on the RBC when you have the Hh, HH, and A/A, A/O, or A/B genotypes • The B antigen is found on the RBC when you have the Hh, HH, and B/B, B/O, or A/B genotypes
H antigen • Certain blood types possess more H antigen than others: O>A2>B>A2B>A1>A1B Greatest amount of H Least amount of H
Why do Group O individuals have more H antigen than the other groups? The O gene is a silent allele. It does not alter the structure of the H substance….that means more H antigen sites The O allele
A A A A Group O Group A A Many H antigen sites Fewer H antigen sites Most of the H antigen sites in a Group A individual have been converted to the A antigen
ABO Subgroups • ABO subgroups differ in the amount of antigen present on the red blood cell membrane • Subgroups have less antigen • Subgroups are the result of less effective enzymes. • They are not as efficient in converting H antigens to A or B antigens (fewer antigens are present on the RBC) • Subgroups of A are more common than subgroups of B
Subgroups of A • The 2 principle subgroups of A are: A1 and A2 • Both react strongly with reagent anti-A • To distinguish A1 from A2 red cells, the lectin Dolichos biflorus is used (anti-A1) • 80% of group A or AB individuals are subgroup A1 • 20% are A2 and A2B
A2 Phenotype • Why is the A2 phenotype important? • A2 and A2B individuals may produce an anti-A1 • This may cause discrepancies when a crossmatch is done (incompatibility) • What’s the difference between the A1 and A2 antigen? • It’s quantitative • The A2 gene doesn’t convert the H3 & H4 to A very well • The result is fewer A2 antigen sites compared to the many A1 antigen sites
Other A subgroups • There are other additional subgroups of A • Aint (intermediate), A3, Ax, Am, Aend, Ael, Abantu • A3red cells cause mixed field agglutination when polyclonal anti-A or anti-A,B is used • Mixed field agglutination appears as small agglutinates with a background of unagglutinated RBCs • They may contain anti-A1
B Subgroups • B subgroups occur less than A subgroups • B subgroups are differentiated by the type of reaction with anti-B, anti-A,B, and anti-H • B3, Bx, Bm, and Bel
Other ABO conditions • Bombay Phenotype (Oh) • Inheritance of hh • The h gene is an amorph and results in little or no production of L-fucosyltransferase • Originally found in Bombay (now Mumbai) • Very rare
Bombay • The hh causes NO H antigen to be produced • Results in RBCs with no H, A, or B antigen (patient types as O) • Bombay RBCs are NOT agglutinated with anti-A, anti-B, or anti-H (no antigens present) • Bombay serum has strong anti-A, anti-B and anti-H, agglutinating ALL ABO blood groups • What blood ABO blood group would you use to transfuse this patient??
ANSWER: • Another Bombay • Group O RBCs cannot be given because they still have the H antigen • You have to transfuse the patient with blood that contains NO H antigen
ABO Blood Group ABO Antibodies
Landsteiner’s Rule: • Normal, Healthy individuals possess ABO antibodies to the ABO antigen absent from their RBCs
ABO Blood Group System • The ABO Blood Group System was the first to be identified and is the most significant for transfusion practice • It is the ONLY system that the reciprocal antibodies are consistently and predictably present in the sera of people who have had no exposure to human red cells
Blood Group Systems • Most blood group systems (ABO and others) are made up of: • An antigen on a red cell and the absence of it’s corresponding antibody in the serum (if you’re A, you don’t have anti-A) • If you do NOT have a particular antigen on your red cells then it is possible (when exposed to foreign RBCs) to illicit an immune response that results in the production of the antibody specific for the missing antigen
ABO • Remember: • The ABO Blood Group System does NOT require the presence of a foreign red blood cell for the production of ABO antibodies • ABO antibodies are “non-red blood cell stimulated” probably from environmental exposure and are referred to as “expected antibodies” • Titer of ABO Abs is often reduced in elderly and in patients with hypogammaglobulinemia • Infants do not produce Abs until 3-6 months of age
Anti-A1 • Group O and B individuals contain anti-A in their serum • However, the anti-A can be separated into different components: anti-A and anti-A1 • Anti-A1 only agglutinates the A1 antigen, not the A2 antigen • There is no anti-A2.
Anti-A,B • Found in the serum of group O individuals • Reacts with A, B, and AB cells • Predominately IgG, with small portions being IgM • Anti-A,B is one antibody, it is not a mixture of anti-A and anti-B antibodies
ABO antibodies • IgM is the predominant antibody in Group A and Group B individuals • Anti-A • Anti-B • IgG (with some IgM) is the predominant antibody in Group O individuals • Anti-A,B (with some anti-A and anti-B)
ABO antibody facts • Complement can be activated with ABO antibodies (mostly IgM, some IgG) • High titer: react strongly (4+)
ABO Antibodies • Usually present within the first 3-6 months of life • Stable by ages 5-6 years • Decline in older age & in hypogammaglobulinemia • Newborns may passively acquire maternal antibodies (IgG crosses placenta)
Nature of antibodies • Non-red blood cell stimulated • ABO antibodies • Red blood cell stimulated • Antibodies formed as a result of transfusion, etc • Usually IgG • Active at 37°C • Can occur in group O (may occur in group A or B) • These antibodies also occur in the other Blood Group Systems
ABO Antigens in Secretions • Secretions include body fluids like plasma, saliva, synovial fluid, etc • Blood Group Substances are soluble antigens (A, B, and H) that can be found in the secretions. • This is controlled by the H and Se genes
Secretor Status • The secretor gene consists of 2 alleles (Se and se) • The Se gene is responsible for the expression of the H antigen on glycoprotein structures located in body secretions • If the Se allele is inherited as SeSe or Sese, the person is called a “secretor” • 80% of the population are secretors
Secretors • Secretors express soluble forms of the H antigen in secretions that can then be converted to A or B antigens (by the transferases) • Individuals who inherit the sese gene are called “nonsecretors” • The se allele is an amorph (nothing expressed) • sese individuals do not convert antigen precursors to H antigen and has neither soluble H antigen nor soluble A or B antigens in body fluids
Secretor Status Summary • The Se gene codes for the presence of the H antigen in secretions, therefore the presence of A and/or B antigens in the secretions is contingent on the inheritance of the Se gene and the H gene A antigen Se gene (SeSe or Sese) H antigen in secretions and/or B antigen No antigens secreted in saliva or other body fluids se gene (sese)