Data + Analysis = Decision Support
Data + Analysis = Decision Support. Rema Padman, PhD Professor of Management Science and Health Informatics The Heinz School Carnegie Mellon University MMM Program rpadman@cmu.edu. Outline - Day 1. Introduction Motivation Illustrative Examples DSS Analysis Framework

Data + Analysis = Decision Support
E N D
Presentation Transcript
Data + Analysis = Decision Support Rema Padman, PhD Professor of Management Science and Health Informatics The Heinz School Carnegie Mellon University MMM Program rpadman@cmu.edu
Outline - Day 1 • Introduction • Motivation • Illustrative Examples • DSS Analysis Framework • DSS Reference Architecture • Key Challenges • Decision making • Process • Strategies used by humans • Implications for decision support
Outline - Day 2 • Technology Enablers • Data Management • Databases • Data warehousing • Data marts • OLAP, ROLAP, MOLAP, WOLAP • Analysis Technologies • Decision analysis methods • Rule-based systems • Knowledge discovery and pattern recognition
Outline - Day 3 • DSS Integration, Deployment, Use • Intermountain Health Care • Clinical Reminder System
Information – The Emerging Capital of Healthcare (Diamond Cluster International, Inc.) Volume of Information Provider InformationProcessing Capacity Available PatientInformation HealthcareInformatics Time
The Future- A Decision Support Focus • Real time decision support at the point of care • Customized disease management for the individual and the population • Knowledge nodes that leverage pervasive computing infrastructure • Telemedicine • Public health
Drivers • Demand Pull • Value of information • Reduction of errors • Managing information overload • Technology Push • Computing and communication technologies, decision and information technologies, medical technologies,.. • Regulatory Push • HIPAA, Insurance reform, Patient’s bill of rights…
Motivation: Value of Information • “In attempting to arrive at the truth, I have applied everywherefor information, but in scarcely an instance have I been able to • obtain hospital records fit for any purpose of comparison. If they • could be obtained...they would show subscribers how their money • was being spent, what amount of good was really being done with • it, or whether the money was not doing mischief rather than good...” • Florence Nightingale, 1873 • Notes on a Hospital
Drug dosing systems Diagnostic aids Preventive care systems Other medical care All CDSS studies - 9/15 - 1/5 - 14/19 - 19/26 - 43/65 Evidence for CDSS Adoption?DL Hunt, RB Haynes, SE Hanna, K Smith. Effects of computer-based clinical decision support systems on physician performance and patient outcomes. JAMA 1998 280: 1339-1346.
Motivation: Reducing Medical Errors • 1999 IOM report on medical errors - “To Err is Human: Building A Safer Health System” • "The stunningly high rates of medical errors - resulting in deaths, permanent disability, and unnecessary suffering - are simply unacceptable in a medical system that promises first to 'do no harm,'" says William Richardson, chair of the committee that wrote the report and president and chief executive officer of the W.K. Kellogg Foundation, Battle Creek, Mich. • "Our recommendations are intended to encourage the health care system to take the actions necessary to improve safety. We must have a health care system that makes it easy to do things right and hard to do them wrong.”
Evidence for ADE Reduction?DW Bates et al.. JAMA 1998 280: 1311-1316, DW Bates et al. JAMIA 2003 10:115-128. • BWH interventions • Applications devoted to workflow • Existing, expandable clinical systems • Order entry only way to enter orders • 15,000 orders a day, 400 changed due to intervention (warnings, reminders, ..) • drug-allergy, drug-drug, drug-problem • drug-lab, lab-drug • drug dosing, renal dosing • appropriate dosage • drug substitution • High user satisfaction
Motivation: Managing Information Overload “It is simply unrealistic to think that individuals can synthesize in their heads scores of pieces of evidence, accurately estimate the outcomes of different options, and accurately judge the desirability of those outcomes for patients.” David M. Eddy, MD, PhD JAMA 1990, 263:1265 - 1275
Technology Drivers • Reduced barriers to facilitated and customized information access • Data storage, management, retrieval, and analysis technologies • Input-output technologies • Communication and networking technologies • Internet and web technologies
Technology Drivers Building efficiency, effectiveness, and quality into healthcare delivery and administration • use data in EMRs and CDRs for more than individual patient management
Regulatory Drivers • HIPAA • Administrative provisions • Privacy, security provisions • …. • Leapfrog Group Recommendations • Computer Physician Order Entry (CPOE) • Evidence-based Hospital Referral (EHR) • ICU Physician Staffing (IPS) • ..
Contextual Drivers • Increased risk-sharing by providers • IOM reports • To Err is Human: Building a Safer health System (1999) • Crossing the Quality Chasm: A New Health System for the 21st century (2001) • Unequal Treatment: Confronting Racial and Ethnic Disparities in Healthcare (2002) • Patient Safety: Achieving a New Standard for Care (2003) • Bioterrorism and biosurveillance–related objectives
Current Initiatives (EBM Solutions) Payers will focus on these co-dependent variables to reduce costs and improve care • Reduced inappropriate variation and increased adherence to evidence-based guidelines by providers • Increased comprehension of and adherence to evidence-based guidelines by patients.
Variation Reduction + Patient Compliance - Potential Results • Patient Compliance… • $20-50B opportunity (UBS Warburg) • Inappropriate variability… • $200-300B opportunity (Juran) The two are inextricably related…essential to manage how care is delivered to manage costs and improve care
TABLE 1 Simple Rules for the 21st-Century Health Care System. Current Approach New Rule Care is based primarily on visits. Care is based on continuous healing relationships. Professional autonomy drives variability. Care is customized according to patient needs and values. Professionals control care. The patient is the source of control. Information is a record. Knowledge is shared and information flows freely. Decision making is based on training and experience. Decision making is evidence-based. Do no harm is an individual responsibility. Safety is a system property. Secrecy is necessary. Transparency is necessary. The system reacts to needs. Needs are anticipated. Cost reduction is sought. Waste is continuously decreased. Preference is given to professional roles over the system. Cooperation among clinicians is a priority. Transforming Health Care with IT SOURCE: Table 3-1 in Crossing the Quality Chasm, IOM, 2001
Pay-Off: Health Cost Reduction Potential of 10% with New Care Management Model (Gartner) • Necessary for system to move from adverse event model to utilization management model with 10% savings achievable by 2007. • Drivers are… • Increased costs • Patient protection legislation • Increased demand for services • New technology Using Patient Care Management to Preserve and Enhance Profitability Gartner Inc., September, 2002
Pay-Off: Anticipated Impact of Internet Clinical Applications • 20% of Office Visits Eliminated • 30% of Physicians Time Reduced PriceWaterhouse Survey of 400 Healthcare Thought Leaders Healthcast 2010
Unstructured Strategic Long-term impact Tactical Operational Structured Short-term impact Organizational Context • Most organizational decision-making can be classified as occurring at 3 levels: strategic, tactical, and operational (Anthony, 1965)
Illustrative Examples • Biosurveillance – RODS • Clinical DSS – Theradoc, Dxplain • Administrative DSS – ThinkMed Expert, Internetivity • Personalized DSS – Medicalogic, DecisionCoaches
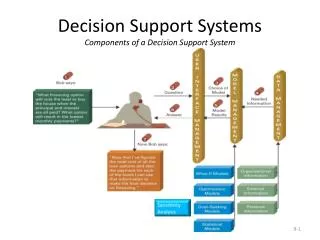
A Conceptual Model of a DSS(Alter) Information Supporting semi-structured or unstructured decisions Data about past and present projections, assumptions People Decision makers, support staff Information Technology Work Practices Goals Interactive systems, software for data analysis, model building, and graphical display
Clinical Decision Framework Patient data Patient Responses Clinical Decisions Interventions Domain info Admin info Alerts Reminders Clinical Guidelines and Pathways Guidelines and Decision Support Pathways
DSS Reference Architecture Language System Problem Processing System Knowledge System Presentation System
DXPlain: Diagnostic DSS from Massachusetts General Hospital • Uses a set of clinical findings to produce a ranked list of diagnoses that might explain the findings • provides justification • suggests additional clinical information to collect • lists unusual manifestations for each disease
Dxplain • Information repository • > 2000 diseases • > 5000 clinical manifestations • Uses a bayesian probabilistic method to draw inferences about diseases based on presented clinical findings • Educational tool for clinical education and clinical problem solving • Electronic medical textbook and a medical reference system
Dxplain info • http://www.lcs.mgh.harvard.edu/privlic.htm • to become a registered user • limited to clinicians
Analyzing a DSS • Is the goal problem finding or problem solving? • What type of activity is involved: planning, execution or control? • What approach is used to improve the decision? • What kinds of answers does the system provide?
Analyzing a DSS • What is the users role and degree of interaction with the system? • What kind of impact does the system have on desired objectives? • What kind of information technology is used?
Feature of system • Extent to which system imposes structure • access to information/tools • enforcement of rules/procedures • substitution of technology for people
Feature of Task • Level of coordination • individual/discretionary • individual/mandatory • workgroup • organizational • inter-organizational
Approach used • Provide background data • individual discretionary, access to info • Support analytic work • individual discretionary, access to tools • structure repetitive decisions • individual mandatory, enforcement of rules • automate decisions • individual mandatory, substitution of technology for people • structure planning processes • organizational, enforcement of rules • structure control processes • organizational, enforcement of rules
DSS Reference Architecture Language System Problem Processing System Knowledge System Presentation System