RHEUMATOID ARTHRITIS for the internist...
590 likes | 2.01k Views
RHEUMATOID ARTHRITIS for the internist. Christopher Parker CPT (P), MC, USA Rheumatology Service WRAMC. Introduction. Interactive format Clinical features Laboratory features Extra-articular features Management considerations and paradigms Prognosis.

RHEUMATOID ARTHRITIS for the internist...
E N D
Presentation Transcript
RHEUMATOID ARTHRITISfor the internist... Christopher Parker CPT (P), MC, USA Rheumatology Service WRAMC
Introduction • Interactive format • Clinical features • Laboratory features • Extra-articular features • Management considerations and paradigms • Prognosis
Case Presentation: 55 YOF complains of months of bilateral hand pain. She describes progressive morning stiffness lasting 3 hours with wrist, MCP, and PIP pain and swelling. She has also noted some discomfort and perhaps swelling in her wrists, shoulders, knees, and toes. Review of systems is unremarkable. What historical features speak for RA?
Case Presentation: • Physical exam is notable for swelling, tenderness, and warmth in the elbows, wrists, MCPs, PIPs, knees, and MTPs with non-tender soft tissue nodules over the olecronon. • What is the difference between arthritis and arthralgia? • Are there further tests that can be done to confirm the diagnosis?
WBC = 5.2 H/H = 10/30 with normal RDW PLT= 475k ESR= 75 RF= 450 ANA= positive TSH= normal CK= normal P1-3 + uric acid normal U/A normal Laboratory Exam
Work-up of an inflammatory arthritis • CBC, BUN/Cr, calcium, LFTs, uric acid, UA, HIV, RF, ANA, CPK, CXR • further serologic evaluation and specific tests geared toward the presentation and results from above tests • radiographs have a higher yield with chronic symptoms (> 6 weeks)
Laboratory abnormalities • anemia of chronic disease • thrombocytosis in active disease • low white cell count in Felty’s • ESR • CRP
Rheumatoid factor • series of antibodies that recognize the Fc portion of an IgG molecule • any serotype • most IgM • many conditions associated with RF positivity - chronic inflammation • 70% RA positive at onset, overall 85% in first two years • associated with more severe disease, extra-articular manifestations, mortality
DDX of a positive RF • normal - 1-4%, 10-25% over age 70 • systemic autoimmune diseases • infections • malignancy • chronic liver disease • pulmonary diseases
ANA in RA • 25% RA are positive for ANA • other serologies usually negative • ? more severe disease (RA) with worse prognosis
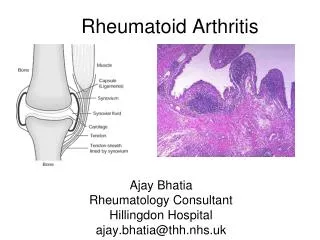
RA - Definition • chronic systemic inflammatory disorder • unknown etiology • diarthroidal joints • synovium affected • bone, cartilage, ligaments • deformity • extra-articular manifestations
RA - Definition • clinical diagnosis • symmetric polyarthritis of small joints • subacute • acute • rheumatoid factor positivity • erosive disease
RA - Epidemiology • worldwide distribution • all races • female > male 3:1 • 1% adults in U.S. • genetic associations • HLA-DR4, DR1
Case Study • 29F presents with 3 weeks of pain and swelling in the wrists, MCPs, and PIPs. She has 2 hours of morning stiffness. She also complains of extreme fatigue and having difficulty keeping up with her four year old boy. Her son is well but had a rash a few weeks ago. Her exam confirms symmetric polyarticular inflammatory arthritis. • Could she have something other than RA?
RA - differential diagnosis • Common diseases • spondyloarthropathies • CTDs • polyarticular gout • CPPD • viral infections • fibromyalgia
RA - differential diagnosis • Uncommon • hypothyroidism • SBE • hemochromatosis • hypertrophic pulmonary osteoarthropathy • hyperlipoproteinemias • hemoglobinopathies • relapsing polychondritis
RA - differential diagnosis • Uncommon • rheumatic fever • sarcoidosis • lyme disease • amyloid • HIV • malignancies/paraneoplastic syndromes
RA - differential diagnosis • Rare • familial mediterranean fever • multicentric reticulohistiocytosis • whipple’s disease • angioimmunoblastic lymphadenopathy
Case Study • 60WM with RA presents with progressive worsening of his joint complaints over the last few months with intermittant fever, swelling of his “glands”, and painful lesions on his finger tips. ROS notable for 5lb wt loss. Exam confirms polyarthritis and small digital infarctions. • Could all of his symptoms be explained by RA?
Extra-articular manifestations • General • fever, lymphadenopathy, weight loss, fatigue • Dermatologic • palmar erythema, nodules, vasculitis • Ocular • episcleritis/scleritis, scleromalacia perforans, choroid and retinal nodules
Extra-articular manifestations • Cardiac • pericarditis, myocarditis, coronary vasculitis, nodules on valves • Neuromuscular • entrapment neuropathy, peripheral neuropathy, mononeuritis multiplex • Hematologic • Felty’s syndrome, large granular lymphocyte syndrome, lymphomas
Extra-articular manifestations • Pulmonary • pleuritis, nodules, interstitial lung disease, bronchiolitis obliterans, arteritis, effusions • Others • Sjogren’s syndrome, amyloidosis
Felty’s syndrome • classic triad • RA, splenomegaly, leukopenia • generally a neutropenia (<2000/mm3) • thrombocytopenia may occur • complications • infections, non-healing leg ulcers • most require no additional treatment for cytopenias • splenectomy?
Case Study • You are tasked to “back fill” for a small army community hospital as a primary care provider… • GYN exam for perimenopausal 45WF • MSK exam • On NSAIDs • No complaints of pain Are NSAIDs enough? What other medications could you use?
RA - Management • Nonpharmacologic • rest • fatigue, splinting • pain relief • heat, cold, ultrasound, paraffin, massage • physical therapy • occupational therapy • Patient education
RA - Management • Pharmacologic • analgesics • NSAIDs - full dose • corticosteroids • prednisone at low dose - “bridge”, “burst” • intra-articular steroids
Disease modifying agents • every patient should be considered for at least one modifying agent • limitations • may not prevent damage • may not have lasting effect • may not be tolerated due to toxicity
DMARDs • hydroxychloroquine • mild non-erosive disease • combinations • 200 mg bid • eye exams
DMARDs • Sulfasalazine • 1 gm bid - tid • CBC, LFTs • onset 1 - 2 months • Methotrexate • most commonly used drug • fast acting (4-6 weeks) • po, SQ - weekly • CBC, LFTs
DMARDs • IM Gold • slow onset (3-6 months) • weekly then monthly injections • CBC, UA before each injection • Oral Gold • less effective • slow acting (4-6 months) • daily • CBC, UA
DMARDs • Azathioprine • 100-200 mg daily • CBC, LFTs • ?malignancy potential • onset 2 - 3 months • D-Penicillamine • daily • slow onset (3-6 months) • CBC, UA • autoimmune phenomenon
DMARDs • CyclosporinA • daily • BP, UA • Cyclophosphamide • refractory cases • CBC • Chlorambucil • CBC
New Therapies for RA • Enbrel • Soluble tumor necrosis factor fusion protein • Arava • Leflunomide
Chimeric A2 (cA2) Monoclonal Antibody Mouse (binding site for TNF-a) Human (IgG1) • Chimeric (mouse/human) IgG1monoclonal antibody • Binds to TNF-a with highaffinity and specificity Knight, et al. Mol Immunol. 1993.
DMARDs • over the counter remedies • report use of vitamins, health aids, unusual diets • “natural” does not mean “safe”
Case Study: Follow Up • During your training you became comfortable with the use of prednisone + HCQ and begin treatment including prophylatic therapy for OP with calcium, vitamin D, and discuss ERT. You recommend follow up appointment in 4-8 weeks. • What objective parameters will you use to determine if your therapy is effective?
Response to therapy • AM stiffness, total number swollen, tender joints, (S1T2W+) • perception of pain • perception of overall response • health assessment measurement • ESR, CRP levels • physician’s assessment
Criteria for Remission (ACR) • no fatigue • morning stiffness for 15 minutes or less • no joint pain • no joint tenderness or pain on motion • no soft tissue swelling in joints or tendon sheath • ESR <30 mm/hr (women) or 20 mm/hr (men) • 5 of 6 present for 2 months • no vasculitis, pericarditis, pleuritis, myositis, weight loss, fever
RA - long term prognosis • RA shortens survival and produces disability • 1/3 leave work force in five years • aggressive DMARD TX can reduce disability by 30% in 10-20 years