Peripheral Vascular System
Peripheral Vascular System. Consists of a system of intertwining veins and arteries which carry blood to and from the heart and lungs Also involves the capillaries and lymph system . Peripheral Vascular Disease. Disorders which alter the normal flow of blood through the arteries and veins

Peripheral Vascular System
E N D
Presentation Transcript
Peripheral Vascular System • Consists of a system of intertwining veins and arteries which carry blood to and from the heart and lungs • Also involves the capillaries and lymph system
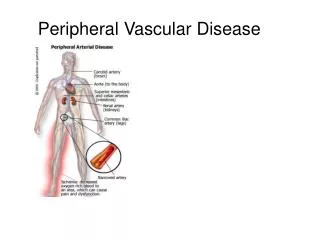
Peripheral Vascular Disease • Disorders which alter the normal flow of blood through the arteries and veins • Effects the lower extremities more frequently the the upper • A client with a diagnosis of PVD implies arterial disease rather than venous • Some client have both arterial and venous disease
Patho • PVD is the manifestation of systemic atherosclerosis • Chronic condition in which partial or total occlusion deprives the lower extremities of oxygen and nutrients • Fatty substances accumulate at the site of vessel wall injury and alter or occlude the blood flow • Risk factors: • Hypertension, smoking, high lipids and cholesterol, diabetes, obesity and family predisposition
Data Collection for PVD • Subjective symptoms • Aching calves • Numbness in legs • Leg cramps • Loss of sensation in legs • Pain in legs during exercise (intermittent claudicating) • History of diabetes, thrombophlebitis, hypertension or alcoholism
Objective Symptoms Cold or blue feet Redness (rubor) of leg in dependent position (arterial) Spares hair distribution Dry, scaly, dusky, pale, or mottled skin Edema Stasis ulcers (venous-occur around ankle and foot is warm, arterial- painful,on toes and can become gangrene) Muscle atrophy Varicose veins Diminished or absent pulses – use grading scale Delay in capillary refill Bruits heard in major arteries Differences in the circumference of legs Check for Homans’ sign Data Collection for PVD, cont.
Diagnosis • Arteriography – (not widely used), inject dye onto arterial system • Segmental systolic B/P measurements – noninvasive, inexpensive method which uses measurements of B/P at intermittent segments of the lower extremities • Doppler ultrasound – sound waves to identify changes in the walls of the blood vessels • Plethsmography – used to determine venous thrombus and blood flow through the veins
Interventions • Non-surgical • Elastic stockings/intermittent pneumatic compression • Teach client to avoid tissue trauma – wear shoes, inspect feet, trim nail straight across • Exercise • Positioning • Promoting vasodilation • Drug therapy • PCTA • Laser assisted angioplasty • Anthrectomy
Interventions, cont. • Surgical • Arterial revascularization – surgically bypassing the occlusion with a saphenous vein or synthetic material • Pre-op care • NPO, vitals, pulses, IV, Foley, A-line, etc • Post-op care • Watch circulation and B/P • May need anticoagulation • No crossing legs, no ROM of limb, may be on bed rest • No dependent position for extended period • May elevate extremity • Pain RX, may need vasodilators, nitroglycerine, NSAIDS
Arterial Embolism • More common in the lower extremity • Life threatening • May break loose and travel, causing other occlusions • 6 P’s or S/S • Pain • Pallor • Pulselessness • Paresthesia • Paralysis • Poikilothermia (coolness)
Arterial Embolism, cont. • Immediate treatment to prevent permanent damage or loss of extremity • 1st intervention is Heparin • May need embolectomy • Can be done with arthroscopy • May need to open and remove embolus • Post-op care involves watching for color changes and signs of occlusion • May have spasms and swelling • Also may develop compartment syndrome
Raynaud’s Disease • Caused by vasospasms of the arterioles and arteries of the upper and lower extremities • Affects hands but can be on toes and tip of nose • S/S – chronic, intermittent, numbness, coldness, pain and pallor • Women 16-40 years of age • Cause is unknown • After spasm the skin becomes reddened and hyperemic
Raynaud’s Disease, cont. • Diagnosis is based on symptoms • Treatment involves relieving the vasospasms and prevent pain • Vasodilators • Topical nitroglycerine • Calcium channel blockers • ACE inhibitors
Raynaud’s Disease, cont. • Nursing care • Pain control • Teach client to avoid stimuli which may trigger episode (stress, cold air temp, smoking) • Keep extremity warm • Use hair dryer, warm H2O, etc • Protect area from trauma
Buerger’s Disease(Thromboangiitis Obliterans) • Uncommon occlusive disease of the medium and small arteries and veins • The distal upper and lower limbs are most frequently affected • In young adult men who smoke • May result in fibrosis and scarring of the perivascular system
Buerger’s Disease(Thromboangiitis Obliterans) • Pain in the arch of the foot is the first clinical indicator • Pain may be ischemic in nature • Clients have increased sensation to cold • Pulses may be diminished in the distal extremities and are cool and red or cyanotic • Ulcerations and gangrene may occur • Treatment is same as with Raynaud’s
Aneurysms • Permanent localized dilation of an artery • Area stretches and weakens, and balloons out • As it enlarges the risk of rupture increases • Can be acquired or congenital • Acquired are caused by trauma, arteriosclerosis, or infection • Abdominal aorta is most prevalent site –(AAA are about 75%)
Aneurysms, cont. • S/S • Most are asymptomatic • May be discovered on routine exam • Pain may be caused by the pressure on organs surrounding the aneurysm • May notice a pulsation in the upper abdomine or by hearing a bruit
Aneurysms, cont. • Clients with a rupturing AAA are critically ill • Will go into hemorrhagic shock (hypovolemic) • Hypotension • Diaphoresis, mental confusion, oliguria, dysrhythemias • Retroperitioneal hemorrhage produces flank bruising • Abdominal distention may occur • Shortness of breath, hoarseness, and difficulty swallowing may be signs of a thoracic aneurysm
Aneurysms, cont. • Diagnosis • Abdominal or lateral of the spine • CT scan • Ultrasound
Aneurysms, cont. • Interventions • Nonsurgical • Monitor growth • Maintain B/P • Frequent CT scans
Aneurysms, cont • Surgical • Elective mortality = 2-5% • Emergency = 50% • AAA resection with graph • Preop – as described for vascular surgery • Postop –client in ICU • Monitor vitals, A-line, EKG, etc. • Watch for • MI, graph occlusion, hypovolemia, renal failure, respiratory distress, paralytic ilius
Aortic Dissection, cont. • Symptom • Pain which is a tearing, ripping, stabbing that tends to move from the point of origin • Pain may be in the anterior chest, back, neck, throat, jaw or teeth • Emergency care • Elimination of pain • Control B/P – 100 to 120 systolic or lower • If uncomplicated may be conservative treatment • If dissection is in the proximal aorta, require CPB
Aortic Dissection • Not a rupturing aneurysm • Dissecting hematoma or aortic dissection • Caused by a sudden tear in the aortic intima • Hypertension is a contributing factor • Relatively common - 2000/year in the US • Ascending aorta and the descending thoracic aorta are the most common sites
Varicose Veins • Dilated, tortuous leg veins with back flow of blood caused by incompetent valve closure, which results in venous congestion and vein enlargement • Usually affects the saphenous vein and its branches • Causes • Unknown but may be R/T congenital weakness of valve • Thrombophlebitis • Venous stasis – pregnancy, prolonged standing • Familial tendency
Varicose Veins, cont. • Data Collection • Subjective • Aching • Cramping and pain • Feeling of heaviness • Objective • Palpable nodules • Ankle edema • Dilated veins • Pigmentation of calves and ankles
Varicose Veins, cont. • Diagnosis • History and physical • Venogram • Trendelburg’s test –demonstrates the backward flow of the blood in the venous system
Varicose Veins, cont. • Treatment • Conservative • Avoid standing or sitting for long periods of time • Weight reduction • Support hose • No restrictive clothing
Varicose Veins, cont. • Surgical treatment • Vein stripping, ligation or sclerosing • Postop care • Pain RX • Elevate leg • Watch for bleeding • May need to rewrap leg q shift from toes to thigh • Watch for CMS
Venous Thrombosis(plebitis, thrombophlebitis, deep vein thrombosis) • Phlebitis is inflammation • Thrombophlebitis is a clot in the vein • DVT is presence of a clot in a deep vein rather than a superficial vein
Venous Thrombosis, cont. • Risk factors • Bedrest • Surgery • Leg trauma with cast • Venous insufficiency • Obesity • Oral contraceptives • Malginancy
Venous Thrombosis, cont. • Treatment • Anticoagulant, bedrest, elevate extremity, warm soaks, TED hose • Nursing care • Control pain • Watch skin • Help anxiety • Assess tissue perfusion • Watch respiratory status for embolus
Venous Thrombosis, cont. • S/S • May not have any signs • With obstruction: • Edema • Warmth • Pain, tenderness • Positive Homans’ sogn • Diagnosis • Venogram • Doppler