JOINT COMMISSION’S
JOINT COMMISSION’S. National Patient Safety Goals for 2008. PURPOSE. Promotes specific improvements in patient safety Highlights problematic areas in health care Describes evidence and expert-based consensus to solutions to these problems. LIST OF 2008 NPSGs.

JOINT COMMISSION’S
E N D
Presentation Transcript
JOINT COMMISSION’S National Patient Safety Goals for 2008
PURPOSE • Promotes specific improvements in patient safety • Highlights problematic areas in health care • Describes evidence and expert-based consensus to solutions to these problems
LIST OF 2008 NPSGs • Goal 1_Improve the accuracy of [patient] identification • Goal 2_Improve the effectiveness of communication among caregivers • Goal 3_Improve the safety of using medications • Goals 4&5&6_NA • Goal 7_Reduce the risk of healthcare-associated infections • Goal 8_Accurately & completely reconcile medications across the continuum of care • Goal 9_Reduce the risk of [patient] harm resulting from falls • Goals 10&11&12_NA • Goals 13_Define & communicate the means for [patients] and their families to report concerns about safety and encourage them to do so • Goal 14_NA • Goal 15_The organization identifies safety risks inherent in its [patient] population • Goal 16_Improve recognition & response to changes in a patient’s condition • Universal Protocol_ The organization fulfills the expectation set forth in the Universal Protocol
GOAL 1: Improve the accuracy of patient identification Requirement: Use at least two patient identifiers when providing care, treatment or services Rationale for requirement for Goal 1: Wrong patient errors occur in virtually all aspects of diagnosis & treatment
GOAL 1: Improve the accuracy of patient identification Implementation Expectations • Two patient identifies are used when administering medications or blood products; • Two identifiers are used when collecting blood samples and other specimens for clinical testing; • Two identifiers are used when providing other treatments or procedures; • The patient’s room number or physical location is not used as an identifier; • Containers used for blood and other specimens are labeled in the presence of the patient.
GOAL 2: Improve the effectiveness of communication among caregivers Requirement 2A: For verbal or telephone orders or the telephonic reporting of critical test results, verify the complete order or test result by having a person receiving the information record and “read-back” the complete order or test result.
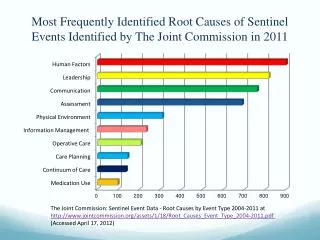
GOAL 2: Improve the effectiveness of communication among caregivers Rationale for Requirement 2A: Ineffective communication is the most frequently cited category of root causes of sentinel events. Effective communication, which is timely, accurate, complete, unambiguous, and understood by the recipient, reduces error and results in improved patient safety.
GOAL 2: Improve the effectiveness of communication among caregivers Implementation Expectation Requirement 2A: The receiver of the information writes down the complete order or test result or enters it into a computer. The receiver of the information reads back the order or test result. The receiver of the information receives confirmation from the individual who gave the order or test result.
GOAL 2: Improve the effectiveness of communication among caregivers Requirement 2B: Standardize a list of abbreviations, acronyms, symbols, and designations that are not to be used throughout the organization. Implementation Expectation The organization implements the list and applies this list to all orders and medication-related documentation when handwritten or entered as free text into a computer.
GOAL 2: Improve the effectiveness of communication among caregivers Implementation Requirement 2B: The abbreviations not to be used includes: Preprinted forms do not include any abbreviations identified as not to be used.
GOAL 2: Improve the effectiveness of communication among caregivers Implementation Requirement 2C: Measure, assess, and if appropriate, take action to improve the timeliness of reporting, and receipt by the responsible licensed caregiver, of critical tests and results and values.
GOAL 2: Improve the effectiveness of communication among caregivers Implementation Expectation Requirement 2C: The organization defines • Critical tests and critical results and values • Acceptable length of time between the ordering and reporting of critical tests, results & values • Length of time between availability and receipt of results The organization • Collects data on the timeliness of reporting of critical tests, results & values • Assesses data & determines whether there is a need for improvement • Takes appropriate action to improve & measure the effectiveness of those actions
GOAL 2: Improve the effectiveness of communication among caregivers Requirement 2E: Implement a standardized approach to “hand-off” communications, including an opportunity to ask and respond to questions.
GOAL 2: Improve the effectiveness of communication among caregivers Rationale for Requirement 2E: The primary objective is to provide accurate information about care, treatment, and services, current condition and any recent or anticipated changes. The information communicated during a “hand off” must be accurate in order to meet patient safety goals.
GOAL 2: Improve the effectiveness of communication among caregivers Implementation Expectations for Requirement 2E: The organization’s process for effective “hand-off’ communication includes: • Interactive communications allowing the opportunity for questioning between the giver and receiver of information. • Up-to-Date information regarding the care, treatment and services, condition and any recent or anticipated changes • A process for verification of the received information, including repeating back or read-back • An opportunity for the receiver to review relevant historical data, which may include previous care, treatment and services • Interruptions during hand-offs are limited to minimize the possibility that information would fail to be conveyed or would be forgotten
GOAL 3: Improve the Safety of Using Medications Requirement 3C: Identify and, at a minimum, annually review a list of look-alike/sound-alike drugs used by the organization,, and take action to prevent errors involving the interchange of these drugs.
GOAL 3: Improve the Safety of Using Medications Implementation Expectations for Requirements: 3C_Identify & at a minimum, annually review a list of look-alike/sound-alike (LASA) drugs; 3D_Label all medications, medication containers syringes, medicine cups, basins or other solutions on & off the sterile field; 3E_Reduce the likelihood of patient harm associated with the use of anticoagulation therapy.
GOAL 7: Reduce the Risk of Healthcare Associated Infections Requirement 7: 7A_Comply with current World Health Organization or CDC Hand Hygiene guidelines; 7B_Manage as sentinel events all identified cases of unanticipated death or major permanent loss of function associated with a health care-associated infection.
GOAL 8: Accurately and completely reconcile medications across the continuum of care Requirements : 8A_There is a process for comparing the patient’s current medications with those ordered for the patient while under the care of the organization; 8B_A complete list of the patient’s medications is communicated to the next provider of service when a patient is referred or transferred to the next provider of service, when a patient is referred or transferred to another setting, service, practitioner, or level of care within or outside the organization. The complete list of medications is also provided to the patient on discharge from the facility.
GOAL 9: Reduce the risk of patient harm resulting from falls 9B_Implement a Fall Reduction Program including an evaluation of the effectiveness of the program
GOAL 13: Encourage patients’ active involvement in their own care as a patient safety strategy 13A_Define and communicate the means for patients and their families to report concerns about safety and encourage them to do so.
GOAL 15: The Organization identifies safety risks inherent in its [patient] population 15A_The organization identifies patients at risk for suicide. [Applicable to psychiatric hospitals and patients being treated for emotional or behavioral disorders in general hospitals-(NOT APPLICABLE TO CRITICAL ACCESS HOSPITALS)]
GOAL 16: Improve recognition and response to changes in a patient’s condition 16A_The organization selects a suitable method that enables health care staff members to directly request additional assistance from a specially trained individual(s) when the patient’s condition appears to be worsening.[Critical Access Hospital, Hospital]
UNIVERSAL PROTOCOL Requirements for UP 1A_Conduct a pre-operative verification process as described in the Universal Protocol; 1B_Make the mark at or near the incision site as described in the Universal Protocol ; 1C_Conduct a “time out” immediately before starting the procedure as described in the Universal Protocol. *Universal Protocol Guidelines for Preventing Wrong Site, Wrong Procedure and Wrong Person Surgery are found on page (17 to 19) of the JC National Patient Safety Goals, requirements & implementation expectations. How to access the JC NPSG: JC Web Address: http://www.jointcommission.org/PatientSafety/NationalPatientSafetyGoals At the Joint Commission Web page; click on 2008 National Patient Goals for HOSPITALS. Click on 2008 National Patient Safety Goal, Manual Chapter (Includes Rationale & Implementation Expectations)
Test Your Knowledge of the NPSG Please Email or fax the completed test to SNI. The results of your test will be emailed back to you.