Brainstem glioma
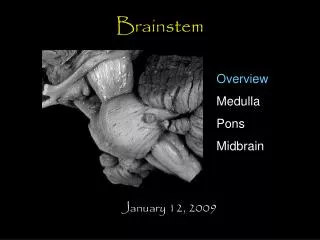
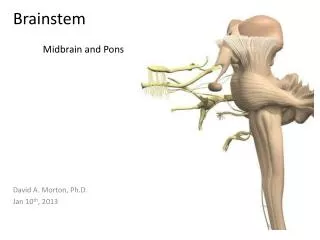
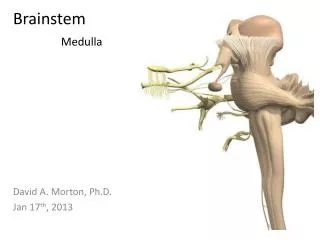
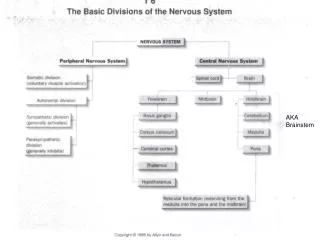
Brainstem glioma. Brainstem gliomas are usually non pilocytic, low grade astrocytomas. On imaging studies they are most commonly solid and infiltrating, with variable contrast enhancement.

Brainstem glioma
E N D
Presentation Transcript
Brainstem gliomas are usually non pilocytic, low grade astrocytomas. On imaging studies they are most commonly solid and infiltrating, with variable contrast enhancement. Tumors intrinsic to the brainstem are biologically more aggressive than pilocytic astrocytomas arising in the optic pathways or cerebellar hemispheres, with most patients dying within two years. Occasionally cystic pilocytic astrocytomas may arise in this region.
History: 3 year-old boy with walking difficulty. Diagnosis: Low grade astrocytoma, WHO I ACR Code: 152.3631
Large T2 hyperintensity mass in clivus with enhancement after contrast administration on T1 weighted image.
History: 34 year-old male with difficulty walking. Diagnosis: Chordoma, clivus. ACR Code: 121.327
-- A chordoma is a primary malignancy arising from remnants of the notochord, most commonly seen in sacrum and the clivus. -- MRI will show heterogenous, bright signal on T2 weighted images. There is usually post-contrast enhancement. -- Differential diagnoses include myeloma, aneurysmal bone cyst, giant-cell tumor, metastatic renal cell cancer, etc.
There are bilateral T2 hyperintensities in the basal ganglia and caudate on the FLAIR and T2 weighted images.
Bright signals are seen in bilateral basal ganglia and caudate on diffusion weighted images which are dark on corresponding ADC map, indicative restricted diffusion from cytotoxic edema.
Post-contrast T1 weighted images show no significant enhancement.
History: 72 year-old male with progressive dementia and myoclonus. Diagnosis: Creutzfeldt-Jacobs Disease. ACR Code: 148.2079
-- Creutzfeldt-Jakob disease (CJD) is a rare and fatal neurodegenerative disease, possibly caused by a peion infection. Patients are usually aged between 50 and 75 and typical clinical features include a rapidly progressive dementia associated, myoclonus and a characteristic electroencephalographic pattern. Neuropathological examination reveals cortical spongiform change, hence the term `spongiform encephalopathy'. -- MRI usually shows characteristic basal ganglia abnormal T2 hyperintensities with restricted diffusion pattern. -- Differential diagnosis is relatively short, including CJD, familial striatal degeneration, Leigh disease, and Wilson's disease .
Non-contrast CT images show a cystic lesion with surrounding edema in the left high parietal region. This represents involutional changes from prior acute hematoma (next image).
Previous (2 weeks earlier) non-contrast head CT images demonstrate high left parietal region acute hematoma after trauma. Blood is also seen within right lateral ventricle occipital horn.
History: 32-old male with trauma to the head. Diagnosis: Cystic hematoma. ACR Code: 132.434
The axial FLAIR image as well as the coronal T1 and T2 weighted MR images demonstrate absence of the septum pellucidum and hypoplasia of the optic chiasm. The coronal T2 weighted image demonstrates small/hypoplastic optic nerves.
History: 4 year-old female suspected for developmental delay. Diagnosis: Septo-optic dysplasia ACR Code: 1613.1354
-- The septum pellucidum may be completely (64%) or partially (36%) absent which results in a squared-off appearance of the frontal horns of the lateral ventricles. -- Up to 50% of patients may have schizencephaly. Others include dysgenesis of the corpus callosum, olfactory, aplasia, gray matter, heterotopia, and cerebellar dysplasia. -- Septo-optic dysplasia is often considered in the spectrum of holoprosencephaly as representing the most minor form of holoprosencephaly.
Abnormal T1 hypointensities are noted in the left temporal tip region which demonstrate no significant enhancement on the post-contrast image.
Abnormal T2 yhperintensity lesion in the left temporal lobe with mild enhancement on the coronal image.
History: 3 year-old girl with seizures. Diagnosis: Dysembryoplastic neuroepithelial tumor (DNET) with nodullar oligodendroglial hypercellularity and focal cortical dysplasia. ACR Code: 1348.3638
-- An uncommon, slow-growing superficial hemispheric lesion found mainly in young adults. -- Due to the slow growth, the cortical location (usually in the temporal lobe) and the frequent presence of cysts, skull remodelling with erosion of the inner and middle table is frequently found. -- The most common clinical presentation is partial complex seizure disorder.
Pre- and post-contrast enhanced head CT images demonstrate hypodensity lesion in the right middle cranial fossa. No apparent enhancement is seen.
FLAIR and T1 weighted ( pre- and post-contrast) images of the brain demonstrate ill-defined large T2 hyperintensity and T1 hypointensity lesion in the right temporal lobe without significant enhancement on post contrast image (coronal image).
History: 4 year-old boy with partial complex seizures. Diagnosis: DNET. ACR Code: 1348.3638
Young patients with intractable seizures – almost always partial complex • 2. Well-circumscribed supratentorial cortical lesions • a. Temporal or frontal lobes most common sites • b. Multinodular architecture (mucinous or gelatinous cysts) with glioneuronal elements and foci of cortical dysplasia is also a common finding • 3. Benign, nonaggressive
DNET Imaging Findings: 1. Isointense on T1WI, hyperintense on T2WI (often "bubbly" appearance). Usually don't enhance (20% do). 2. Remodelling of overlying calvarium common (45%). 3. Calcification in 20-25%, gyral thickening/dysplasia. 4. Differential diagnosis: a. Ganglioglioma b.Oligodendroglioma
Large, mixed signal intensity extra-axial mass in the lateral left posterior fossa.
T1 weighted pre- and post contrast images show no enhancement
Diffusion weighted image with corresponding ADC map image Demonstrate restricted diffusion of this lesion.
History: 38 year-old male with headache. Diagnosis: Epidermoid inclusion cyst. ACR Code: 134.3622
History: 46 year-old male with gait disturbance. Diagnosis: Non-Langerhans cell histiocytosis (Erdheim-Chester disease). ACR Code: 158.389
It is a rare histiocytic disorder of adults characterized by an infiltrate of lipid-laden macrophages, multinucleated giant cells, inflammatory infiltrate of lymphocytes and histiocytes, that can involve many organs. The central nervous system involvement of the hypothalamic / pituitary axis can lead to diabetes insipidus, intra-&-extra axial cerebral infiltration, retro-orbital fat infiltration. They demonstrate as T2 hyperintensity signals which enhance after Gd contrast administration. There is no significant mass effect. The most common neurologic manifestation is central diabetes insipidus and gait disturbance.
Ring enhancing right frontal lobe mass with adjacent parenchymal edema and associated mass effect.
History: 38 year-old male with seizures. Diagnosis: Pathology findings indicate that the lesion fulfills criteria for glioblastoma multiforme. It is astrocytic, mitotically active, and has exuberant vascular proliferation. Also present are focal eosinophilic granular bodies as are common in pleomorphic xanthroastrocytoma (PXA). While the lesion is thus unequivocally malignant, it is possible that is arose in a PXA. ACR Code: 1318.3634