Oncologic emergency
Oncologic emergency. Kourosh Goudarzipour Jan-2014. list. TLS Chemotherpy guideline in TLS Mediastinal mass and SVC syndrome VOD Seizure Leukostasis Cardiac tamponade thyphlitis. TLS. REFRENCES.

Oncologic emergency
E N D
Presentation Transcript
Oncologic emergency KouroshGoudarzipour Jan-2014
list • TLS • Chemotherpy guideline in TLS • Mediastinal mass and SVC syndrome • VOD • Seizure • Leukostasis • Cardiac tamponade • thyphlitis
REFRENCES • Stephen Lauer, M.D.ToniPetrillo , M.D. Tumor LysisSyndrome,journal of pediatric,2008. • Scott C. Howard, M.D., Deborah P. Jones, M.D., and Ching-Hon Pui, M.D. The Tumor LysisSyndrome,newengland journal,2012 • MARK L. HIGDON, LTC, MC, USA, Martin Army Community Hospital Family Medicine Residency Program, Treatment of Oncologic Emergencies, American Family Physician,2006 • Scot j howard,MD,ST.Jude,tumorlysis syndrome update,2010
Case report • An 8-year-old boy was referred to an otolaryngologist for tonsillectomy after several months of increased snoring, fatigue, sore throat, enlarged tonsils, and gradually increasing painless and nontendercervical lymphadenopathy . • The physician in the emergency department documented nasal congestion, enlarged tonsils that touched in the midline,.
Dexamethasone (4 mg) was administered intramuscularly, and loratadine was prescribed. • During the next 36 hours, the malaise developed and he vomited repeatedly. He returned to the emergency department, where he appeared ill . • Evaluation showed a white-cell count of 84,600 per cubic millimeter, with circulating lymphoblasts; a sodium level of 133 mmol per liter
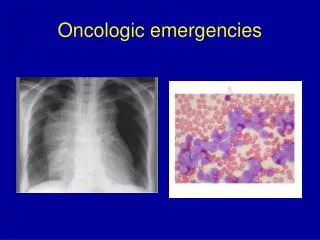
potassium, 5.9 mmol per liter; bicarbonate, 16 mmol per liter; creatinine, 1.0 mg per deciliter phosphorus, 8.5 mg per decilitereruric acid, 12.3 mg per deciliter. • Chest radiography revealed a small mediastinal mass . • DX:Tcell lymphoma • Rx:TLS
Laboratory tumor lysis syndrome requires that two or more of the following metabolic abnormalities occur within 3 days before or up to 7 days after the initiation of therapy.
The corrected calcium level in milligrams per deciliter = measured calcium level in milligrams per deciliter + 0.8 × (4 − albumin in grams per deciliter). • Acute kidney injury is defined as an increase in the creatinine level of at least 0.3 mg per deciliter (26.5 μmol per liter) or a period of oliguria lasting 6 hours or more.
in contrast to Cairo and Bishop’s definition, a 25% change from baseline should not be considered a criterion, since such increases are rarely clinically important unless the value is already outside the normal range. • any symptomatic hypocalcemia should constitute clinical tumor lysissyndrome. New england journal-2012
High-Risk for Tumor Lysis Syndrome (HR-TLS) • Patient with leukemia with a WBC > 100, 000/μL • Patient with a WBC of > 50,000 but < 100,000/μL and elevated uric acid levels less than 2x the upper limits of normal without normalization of uric acid level after 24 hr of hydration and allopurinol .
High-Risk for Tumor Lysis Syndrome (HR-TLS) • Patient with Stage III-IV Burkittlymphoma or B-cell ALL. • Patient with bulky T-cell lymphoblastic lymphoma/leukemia with uric acid level above the upper limits of normal, without normalization of the uric acid level after 24 hours of hydration and allopurinol.
High-Risk for Tumor Lysis Syndrome (HR-TLS) • Patient with bulky leukemia or lymphoma and serum creatin level which is at least 50 % above the upper limits of normal for age regardless of uric acid level or WBC, and which does not normalize after 24 hours of IV hydration.
High-Risk for Tumor Lysis Syndrome (HR-TLS) • Patient with leukemia, WBC > 50,000/uL, and nephromegalyregardless of uric acid and serum creatinine levels. • Patient has 2 or all 3 laboratory features of TLS prior to treatment without normalization of laboratory values after 24 hours of IV hydration and PO allopurinol.
Laboratory/Imaging Guidelines/Consults • Renal function panel and uric acid Q 3-6 hr • LDH • For patients with bulky leukemias or lymphomas and those with renal insufficiency prior to starting therapy, ultrasound of abdomen and kidneys should be done to assess kidney size and rule out renal masses hydronephrosis, hydroureter or bladder compression or distention.
Consult with Nephrology • Consult with Urology service if imaging studies show obstructive uropathy. • G-6-PD screening
Prevention Guidelines • Patients with HR-TLS are candidates for treatment with Rasburicase. • IV hydration: 3000 cc/m2/24 hr D5W ¼ NS ( if < 1 yr old) or D5W½ NS (if > 1 yr old). • Goal: Achieve and maintain urine output of 2500 cc/m2/24 hr and urine specific gravity of < 1010.(urin output more than100cc/m2/hr).
Do not add potassium to IV solution • Do not use sodium bicarbonate routinely –unless it is needed to control significant metabolic acidosis.because significant hyperuricemia is unlikely to occur when Rasburicase is used, thus urine alkalinization is not necessary. Rasburicase does not prevent hyperphosphatemia - and phosphorus is less soluble in alkaline urine.
Clinical Monitoring • Strict I & O • Check weight BID • Check urine output Q 4-6 hr. • Consult with Nephrology
If urine output < 60 % of intake within the first 4 hours of IV hydration and there are no signs of volume overload (e.g. hypertension, tachypnea hypoxemia, S3 gallop), give normal saline boluses (10 cc/kg x 2). • If there is no response may give furosemide (lasix) 1-2 mg/kg Q 6-8 hr. (Do not write any of these as standing orders).
Treatment Guidelines • Rasburicase 0.15 mg/kg/dose (round down to multiple of 1.5 mg vial size) • Repeat dose q. 12-24 hr as necessary to keep uric acid < normal limits. • For overweight patients use ideal body weight. • After first dose of rasburicase, start allopurinol 300 mg/m2/day (or 10 mg/kg/day) PO divided TID.
Give first dose of Rasburicase as soon as HR-TLS criteria for elevated uric acid are met, even if therapy is not to start immediately. • If uric acid is not elevated at diagnosis, give first dose about 4 hours prior to starting chemotherapy.
When patient is on treatment with Rasburicase, blood samples for uric acid measurements should be kept in ice until analyzed, to prevent continuing ex-vivo degradation of uric acid by rasburicase and thus, falsely low uric acid levels.
Start chemotherapy when good urine ouput is established and uric acid is < normal limits, regardless of urine pH. • If patient has moderate to severe renal dysfunction at diagnosis ( i.e. e stimatedGFR < 50 %), consider renal dialysis prophylactically.
Patients with Low-Risk for Tumor Lysis Syndrome (LR-TLS) • Definition: Patients who do not meet criteria for HRTLS. • Most of these patients can be safely managed with IV fluids and PO allopurinol
Laboratory and Imaging Guidelines • Monitor renal panel and uric acid Q 8 - 12 hr • Imaging studies as noted above
Prevention Guidelines • Hydration: IV fluids: 3000 cc/m2/24 hr as D5 W ¼ NS ( < 1 yr old) or D5 ½ NS ( > 1 yr old). • Start chemotherapy when good urine output is established. • Allopurinol: 300 mg/m2/ day (or 10 mg/kg/day) PO divided TID. • If patient is unable to take PO, consider use of IV allopurinol 200 mg/m2/day (max 600 mg/day) divided Q 8 hr.