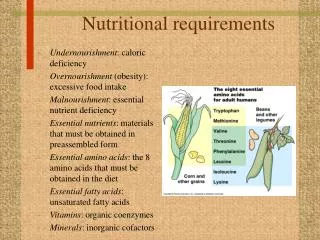
Nutritional Progress Notes
Nutritional Progress Notes. Objectives. After this presentation, you will be able to: State the descriptive words for the acronym SOAP Give a brief description of the meaning for each word in the acronym SOAP Write a progress SOAP progress note from a case study. What is a SOAP Note?.

Nutritional Progress Notes
E N D
Presentation Transcript
Objectives After this presentation, you will be able to: • State the descriptive words for the acronym SOAP • Give a brief description of the meaning for each word in the acronym SOAP • Write a progress SOAP progress note from a case study
What is a SOAP Note? • Summary report of client’s/patent’s condition • Written in client’s/patient's chart • Acronym for • S = subjective • O = objective • A = assessment • P = plan
Pros and Cons of SOAP Charting PROS • Common use by nutrition care professionals and other medical disciplines • Taught in most dietetics education programs • Easy to learn and utilize CONS • Can encourage lengthy chart notes • Some physicians are less likely to respond to this format than others • Can downplay continued reevaluation of client’s progress • Emphasizes legitimacy of objective over subjective data
S: Subjective Information provided/spoken by patient, family, or other person. • Pertinent socioeconomic, cultural info • Level of physical activity • Significant nutritional history: usual eating pattern, cooking, dining out • Work schedule
O: Objective Factual and reproducible observations. • Diagnosis • Height, age, weight—and weight gain/loss patterns • Lab data • Clinical data (nausea, diarrhea) • Diet order • Medications • Estimation of nutritional needs
A: Assessment Summary of dietitian's professional nutrition diagnosis or clinical thoughts. • Interpretation of patient’s status based on subjective and objective info • Evaluation of nutritional history • Assessment of laboratory data and medications • Assessment of diet order • Assessment of patient’s comprehension and motivation
P: Plan Describes the scope of Treatment and contains the action plan and prognosis. • Diagnostic studies needed • Further lab work or lab data needed • Medical nutrition therapy goals • Education nutrition plans • Recommendations for nutritional care • Date for any follow-up
Sample SOAP Note Subjective S: works second shift, eats two meals a day, before/after shift; usually eats in fast food restaurants (fried foods, burgers, ice cream) for lunch and dinner. Does not add salt to foods. Takes blood pressure 2x/day. Activity: Plays volley ball on weekends
Sample SOAP Note Objective O: 34 y.o. female; last menstrual period = 01/05/2006; iron level= 12.3; history of hypertension x 2 years; blood pressure = 130/85 for last four readings; height = 5ft. 3in; weight: 205 lb; BMI=36.
Sample SOAP Note Assessment A: obese; hemoglobin level normal; excessive sodium intake (NI-5.10.2) related to frequent use of fast food meals as evidenced by diet history. Blood pressure high/normal. Low physical activity.
Sample SOAP Note Plan P: Reviewed DASH diet. Identified foods to pack from home to eat during lunch/dinner. Discussed non-food rewards to purchase with money saved from not eating out when weight and B/P goals are reached. Encouraged more activity to facilitate weight loss. Next appointment = 30 days from today.
Conclusion • Not all the parts are used at every visit • Complete sentences are not necessary • Signature goes at end of last line • Never leave a blank line between entries • Never leave a half filled line. Draw a line to fill the line.
Lecture Quiz • What does the acronym SOAP stand for and give a brief description of the meaning for each word. • What medical professionals usually use SOAP notes? • Name one advantage and one disadvantage to using SOAP progress notes.
Lecture Quiz • Write a progress SOAP progress note using the following case study: Your second appointment for the day is with a 25 year old Chinese male. He states he was told by his doctor that his cholesterol is high and he should to “eat better” but he is confused as to how to do that. He hands you a paper with the following labs on it: height = 67”; weight = 200#; blood pressure = 120/80; total cholesterol = 150 and LDL levels= 160.