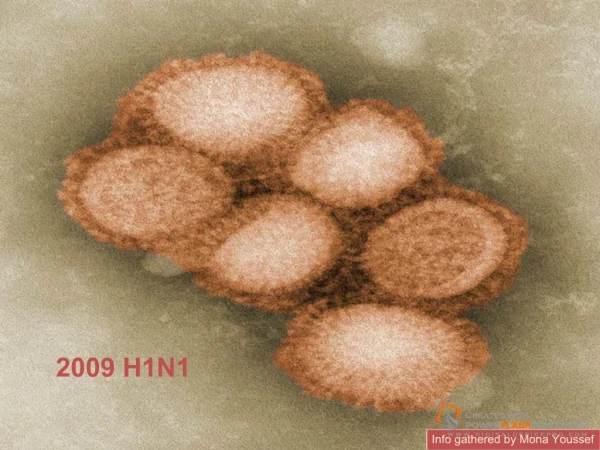
2009 H1N1
2009 H1N1. Creating a Respiratory Protection Program. Introduction. Creating a Respiratory Protection Program. Eileen Franko, DrPH, MS Bureau of Occupational Health, Director New York State Department of Health. Overview Of H1N1 Fall 2009. Module 1. H1N1 Symptoms.

2009 H1N1
E N D
Presentation Transcript
2009 H1N1 Creating a Respiratory Protection Program
Introduction Creating a Respiratory Protection Program Eileen Franko, DrPH, MS Bureau of Occupational Health, Director New York State Department of Health
Overview Of H1N1 Fall 2009 Module 1
H1N1 Symptoms • Cannot distinguish between seasonal influenza, novel influenza and infections with other respiratory viruses based solely on patient’s clinical presentation • Initial patient management decisions need to be based on: • Current levels of seasonal and novel influenza activity in the community • Severity of patient’s illness • Presence of any underlying conditions (including young/old age and pregnancy) that places the patient at higher risk for complications
Human Infection with Novel Influenza A (H1N1) • Symptoms • Influenza-like illness (ILI): • Fever >100°F (37.8°C) and cough or sore throat • Other symptoms • Chills, malaise, headache, fatigue, runny nose, shortness of breath, vomiting, diarrhea • Similar to infection with seasonal influenza virus • Incubation period - 1 –7 days, more likely 1–4 days • Viral shedding can begin 1 day prior to illness onset • Spread by respiratory droplets and indirect transmission
CDC Surveliance Report http://www.cdc.gov/flu/weekly/
Distribution by age group 7/14/09
Flu-like Illness in NYS Hospital Emergency Departments (3 month snapshot)
Pandemic Influenza Control Measures • 1. Delay disease transmission and outbreak peak • 2. Decompress peak burden on healthcare infrastructure • 3. Diminish overall cases and health impacts
New York State Department of Health 2009-2010 Flu MonitoringWeekly Reports http://www.health.state.ny.us/ diseases/communicable/influenza/ surveillance/2009-2010/
Centers for Disease Control Guidance for HealthcareOctober 14, 2009 • Healthcare personnel are persons whose occupational activities involve contact with patients in a healthcare setting. • The guidance includes those working in a clinical setting within a non-healthcare institution such as a school nurse.
Now What Do We Do? • Evaluate using a hierarchy of controls to limit exposure • If N-95 Respirators are needed you will need: • Written Respiratory Protection Program • Employee Medical Assessments • Fit Testing • Training • Recordkeeping • Hierarchy of controls and each component of a program will be described in one of the following modules
End of Module 1 - Introduction Click here for Module 2
Hierarchy of Controls • Prevention methods in order of • most effective to least effective: • Elimination of exposure • Engineering controls • Administrative controls • Personal protective equipment (PPE) • N95 respirators
Elimination of Exposure • Having students and staff stay home when sick • Denying visitors to school who are sick • Social distancing • Have persons with ILI wear surgical mask until they can be sent home • Stay a minimum of 6 feet from a person with ILI
Engineering Controls • Designate separate room or area for sick students waiting for a ride home • Use barriers or partitions when a separate room is not available or feasible • Install hand washing stations with soap and water. If not possible use sanitizing stations in common areas to encourage good hygiene
Administrative Controls • Vaccination • Enforcing exclusion of sick students and staff • Implementing respiratory hygiene/cough etiquette strategies • Minimize the number of staff interacting with students identified to have flu-like symptoms
Vaccination • Although vaccination is an administrative control, it is one of the most effective interventions for preventing transmissions of influenza • Prevents transmission in work, community, and home settings
Personal Protective Equipment (PPE) • Respirators (N95) • Facemasks • Gloves
Respirators • Least effective control in the hierarchy • Relies on the individual to use and maintain properly • Implementation of policies for eliminating exposures, engineering controls and administrative controls reduces the need to rely on N95 respirators
End of Module 2 - Hierarchy of Controls Click here for Module 3
Components of a Respiratory Protection Program • Written program specific to the workplace • Specify employees from each department/ unit that are included in respiratory protection program • Assign a qualified administrator to implement program • A person is qualified when they have had the appropriate training or experience to administer or oversee the program and conduct the required program evaluation
Selecting a Respirator • Must be NIOSH - Certified Respirator used in compliance with the conditions of its certification • Based on respiratory hazards and activities encountered in the workplace • Provide sufficient number of models and sizes to fit a variety of staff facial morphology (2009 H1N1 demand may limit ability to provide a variety of sizes and models)
Employee Medical Evaluation • The employer must select a Physician or Other Licensed Health Care Professional (PLHCP) to perform medical evaluations • The PLHCP may be a physician, registered nurse, nurse practitioner, physician assistant or other licensed health care professional acting within the scope of their state license, registration, or certification (OSHA Directive CPL 2-0.120) • The PLHCP uses a medical questionnaire from the OSHA Respiratory Standard, Appendix C, that is considered an initial medical examination (NOTE: the ASTM Z88 standard provides some guidance for medical qualifications for respirator use.)
Respirator Fit Testing Procedures • Qualitative fit test method using Saccharin or Bitrex • Utilize same make, model and size employee will use • Fit test will be performed annually
Employee Respirator Training • Provide effective training to employees required to use respirators • Conduct annually: comprehensive and understandable • Include proper use, inspection and reasons for use
Record Keeping • Program Evaluation For Proper Implementation • Medical Evaluations • Respirator Fit Testing • Employee Training
End of Module 3 - Components of a Respiratory Protection Program Click here for Module 4
Initial Medical Evaluation (Questionnaire or Medical Exam) • A respirator may place a respiratory burden on employees that varies with the job and workplace conditions, and the medical status of the employee • The employer shall provide a medical evaluation to the employee before the employee is fit tested or required to use the respirator • The employer shall identify a physician or other licensed health care professional (PLHCP) to perform medical evaluations (as defined on the Employee Medical Assessment slide) • The PLHCP shall obtain information specified by the OSHA Respirator Medical Evaluation Questionnaire (see Appendix C of 29CFR1910.134)
Follow-up Medical Examination • The employer shall ensure that an employee receives a follow-up medical examination (physical exam) when the initial medical evaluation warrants one • The follow up medical examination must be performed by a licensed physician, nurse practitioner, or physician’s assistant. • The follow-up medical examination shall include any medical tests, consultations, or diagnostic procedures that the PLHCP deems necessary to make a final determination that the user can safely wear a respirator.
Administration of the Medical Questionnaire and Examinations • Both the questionnaire and the examinations shall be administered confidentially during the employee's normal working hours or at a time and place convenient to the employee • The questionnaire shall be administered in such a manner that is understood by the employee • The employer shall provide the employee with an opportunity to discuss the questionnaire and examination results with the PLHCP
Employer Provides the PLHCP with the Following Information: • Type and weight of the respirator to be used by the employee • Duration and frequency of respiratory use • Expected physical work effort • Additional protective clothing and equipment to be worn • Temperature and humidity extremes • Copy of the company's written respiratory protection program • Copy of the medical evaluation section of the OSHA respiratory protection standard
Medical Determination • Employer shall obtain a written recommendation from PLHCP to determine the employees ability to use a respirator. • The written recommendation shall specify: • limitations on respiratory use related to medical condition of the employee • limitations on respirator use related to the workplace conditions • whether or not the employee is medically able to use the respirator • a statement that the PLHCP has provided the employee with a copy of the written recommendation
Sample PLHCP Approval Physician or other Licensed Health Care ProfessionalMedical Evaluation (PLHCP) for N95 Respirator Use Employer Name: _________________________________________________________ Employee Name: ____________________________ Last 4 #’s of SS#: _________ Medical Evaluation: The employee had the following medical evaluation for respirator use: (check all that apply) □---Respirator Medical Evaluation Questionnaire (1910.134 Appendix C) □---Initial Respirator Medical Exam □---Follow-up Respirator Medical Exam Medical Determination: (check all that apply) □---Medically cleared for use of a disposable N95 respirator without restrictions. □---Not medically cleared for use of a disposable N95 respirator. □---Medically cleared for use of a disposable N95 respirator with the following restrictions: □---Limitations on respirator use related to medical condition of employee. □---Limitations on respirator use related to workplace conditions. □---Details of limitations are noted below: (ex.─ limiting duration or frequency of use, discontinuing if symptoms occur, etc.)
Sample PLHCP Approval (cont) □---Re-evaluation of medical clearance recommended in ____ years. □---The employee and employer were sent a copy of this written recommendation and were apprised of the medical evaluation results. □---Additional Comments/Information: _______________________________________ _______________________________________________________________________ ________________________________________________________________________ PLHCP: Printed Name of Physician or LHCP: __________________________________________ Title: (Physician or LHCP) __________________________________________________ Physician or LHCP Signature: ________________________________________________ Date: ____________________________________________________________________
Negative Medical Determination • If the PLHCP finds a medical condition that may place the employee's health at increased risk if a negative pressure respirator such as a N-95 is used, the employer should reevaluate if another person can fill the role with the ILI student. • Alternatives should be considered from the administrative, engineering and workpractice controls.
Additional Medical Evaluations Shall be Provided When: • An employee reports medical signs or symptoms that are related to ability to use a respirator • A PLHCP, supervisor, or the respiratory program administrator determines the need for a re-evaluation • Workplace conditions and employee work activities change
Click here for Module 5 End of Module 4 - Medical Evaluation
Employee Training about Hazards and Proper Use of N-95 Respirators • Employers are required to provide training to employees who are required to wear N-95 respirators • This training program is intended for health care personnel identified in the CDC October 14, 2009 guidance on infection control
When Should the Training be Provided? • Prior to requiring the employee to use a respirator (initial use) • Annually • When there are changes in the workplace • When there are changes in the type of respirators selected or used • When there are inadequacies in the employee's knowledge or skill of respirator usage
What Subjects Should Employee Training Cover? • Why the respirator is necessary • When it should be used • What are the limitations and capabilities of the respirator • How improper fit, usage, or maintenance can compromise the protective effect of the respirator • How to inspect, put on and remove, use and check the seals of the respirator
Employee Training Subjects (cont.) • The procedures for maintenance and storage of the respirator • How to recognize medical signs and symptoms that may indicate a respiratory problem • The procedure for reporting a problem associated with the respirator
Storing N-95 particulate respirators • Supplies should be placed in clean, secure, temperature-controlled environments to prevent damage or contamination • Avoid storage areas that are damp or have temperature extremes • Use oldest supplies first
Click here for Module 6 End of Module 5 - Employee Training