Understanding the Urinary System: Functions, Organs, and Processes
220 likes | 317 Views
Learn about the functions of the urinary system, major organs like kidneys and bladder, nephrons, urine formation, and filtration processes to maintain homeostasis and eliminate wastes effectively.

Understanding the Urinary System: Functions, Organs, and Processes
E N D
Presentation Transcript
The Urinary System DeShawn Lowery Nate Falk Period 3
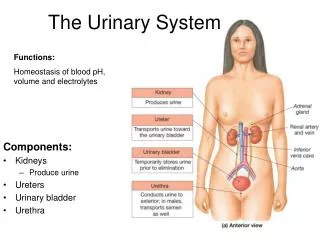
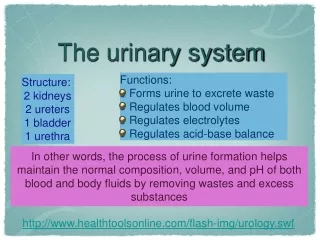
Functions • The Urinary system removes certain salts and nitrogenous wastes. • Helps maintain the normal concentrations of water and electrolytes within body fluids. • Regulates the pH and volume of body fluids. • Helps control red blood cell production and blood pressure.
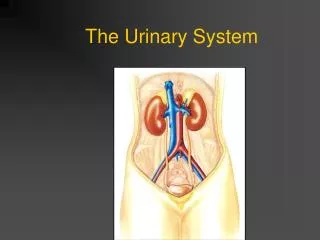
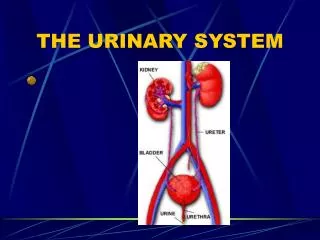
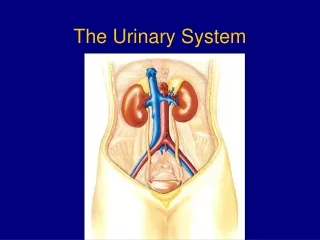
Major Organs • Kidneys: on the posterior wall of the abdominal cavity. • Ureters: extends downward behind the parietal peritoneum and runs parallel to the vertebral column. • Urinary Bladder: within the pelvic cavity, behind the symphysis pubis and beneath the parietal peritoneum. • Urethra: its wall is lined with mucous membrane and contains a thick layer of smooth muscle tissue.
Functions • Kidneys: Removes substance from blood, form urine, and help regulate certain metabolic processes • Ureters: transport urine from the kidneys • Urinary Bladder: Stores urine • Urethra: conveys urine to the outside of the body.
Kidneys • The kidneys are high on the posterior wall of the abdominal cavity. • An adult kidney is about 12 cm long, 6 cm wide, and 3 cm thick. • The left kidney is usually 1.5 – 2.0 cm higher than the right one.
Kidney Structure • A kidney contains a hollow renal pelvis. • The ureter expands into the renal pelvis. • Renal papillae project into the renal sinus • Each kidney divides into a medulla and a cortex
Kidney Functions • Maintain homeostasis by removing metabolic wastes from blood and excreting them. • Regulates….. • Red blood production • Blood volume • Blood pressure • The volume, composition, and pH of body fluids.
Pathway of blood in the kidney Renal Artery hilum interlobar arteries arcuate arteries interlobar arteries afferent arterioles renal vein
Nephrons • A nephron is the functional unit of the kidney • A kidney contains about 1 million nephrons. • It is make up of a renal corpuscle and a renal tubule.
Nephrons • A renal corpuscle is composed of a tangled cluster of blood capillaries called a glomerulus. • Glomerular capillaries filter fluid (first step of urine formation). • Segments of the renal tubule include the proximal convoluted tubule, nephron loop, and distal convoluted tubule, which empties into a collecting duct. • The collecting duct empties into the minor calyx of the renal pelvis.
Urine Formation • Glomerular Filtration: filtration of plasma by the glomerular capillaries. • Tubular reabsorption: moves substances from the tubular fluid back into the blood within the peritubular capillary into the renal tubular. • Tubular Secretion: moves substances from the blood within the peritubular capillary into the renal tubule.
Glomerular Filtration • The first step in urine formation is filtration of substances out of glomerular capillaries and into the glomerular capsule. • Glomerular filtrate passes through the fenestrate of the capillary endothelium.
Filtration Rate • As colloid osmotic pressure in the glomerulus increases, filtration rate decreases. • As hydrostatic pressure in the glomerular capsule increases, filtration rate decreases. • The kidneys produce about 125 milliliters of glomerular fluid per minute, most of which is reabsorbed.
Filtration Pressure • Filtration is due mainly to hydrostatic pressure inside glomerular capillaries. • The osmotic pressure of plasma and the hydrostatic pressure in the glomerular capsule also affect filtration.
Regulation of filtration rate • When the macula densa senses decreased amounts of chloride, potassium, and sodium ions in the distal tubule, it causes juxtaglomerulaar cells to release renin. • This triggers a series of changes leading to vasoconstriction of afferent and efferent arterioles, which may affect glomerular filtration rate, and aldosterone secretion, which stimulates tubular sodium reabsorption.
Tubular Reabsorption • Substances are selectively reabsorbed from glomerular filtrate. • The peritubular capillaries permeability adapts it for reabsorption. • Most reabsorption occurs in the proximal tubule, where epithelial cells have microvilli.
Tubular Secretion • Secretion transports substances from plasma to the tubular fluid. • Potassium and hydrogen ions are secreted both actively and passively.
Urine Composition • Urine is about 95% water, and it also usually contains urea and uric acid. • Urine volume varies with fluid intake and with certain environmental factors
Urine Composition • Urea is a by-product of amino acid catabolism. • Urea enters the renal tubule by filtration, about 50% of it is reabsorbed, and the rest is excreted by urine. • Uric acid is a product of the metabolism of certain organic bases in the nucleic acids. • Active transport reabsorbs uric acid. Some uric acid is secreted into the renal tubule.
Urine Elimination • Peristaltic waves in the ureter force urine to the urinary bladder. • The urinary bladder stores urine and forces it through the urethra during micturition. • Micturition expels urine from the urinary bladder. • In micturition, the detrusor muscle contracts, along with the abdominal wall and pelvic floor.
Diseases • Kidney Stones: kidney stones are formed in uric acid, calcium oxalate, calcium phosphate, or magnesium phosphate, and can form in the collecting ducts and renal pelvis. • Causes include excess vitamin D, blockage of the urinary tract, or a complication of a urinary tract infection. • Can be avoided by drinking a lot of water.