Endocrine System
Endocrine System. Section 1, Chapter 13. Introduction. The endocrine system assists the nervous system with communication and control of the body Characteristics of endocrine glands They are ductless Endocrine glands secrete hormones

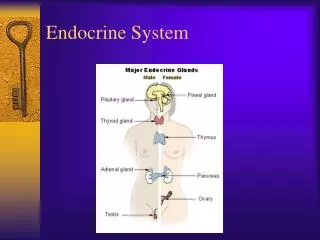
Endocrine System
E N D
Presentation Transcript
Endocrine System Section 1, Chapter 13
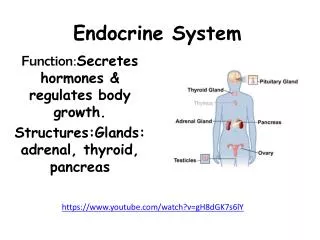
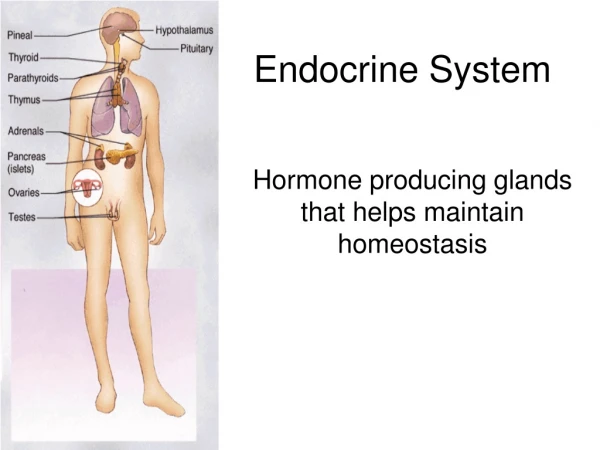
Introduction • The endocrine system assists the nervous system with communication and control of the body • Characteristics of endocrine glands • They are ductless • Endocrine glands secrete hormones • Hormones are carried to distant target cells through the bloodstream • Hormones only act on cells (target cells) that possess receptors sensitive to the hormone – highly specific action.
Other signals • Exocrine glands • Have ducts • Secrete chemicals directly onto a surface • Examples: sweat glands, mucous cells • Paracrine signals • Chemicals that affect only nearby cells • Example: prostaglandins secreted with semen stimulate muscular contractions within female reproductive organs • Autocrine signals • Chemicals that affects only the cells that produced it. • Example: T-cells secrete interleukins (IL), which stimulate the proliferation of the T-cells (monoclonal population) • Neuroendocrine • Nervous tissue that secretes hormones • Example: hormone secretion from the hypothalamus.
Endocrine vs. Nervous Tissue • The endocrine and nervous systems communicate using chemical signals • Neurons release neurotransmitters into a synapse affecting postsynaptic cells • Endocrine glands release hormones into the bloodstream to specific target cell receptors Figure 13.2 Chemical communication. (a) neurons release neurotransmitters onto synapses, affecting postsynaptic cells. (b) Glands release hormones into the bloodstream. Blood carries hormone molecules throughout the body, but only target cells respond.
Endocrine vs. Nervous Tissue Endocrine System Nervous System Cell…………………………………. Neuron Glandular Epithelium Signal………………………………. neurotransmitter hormone Specificity of action…………. receptors on postsynaptic cell receptors on target tissues Speed of onset……………...... <second seconds to hours Duration of action……………. usually very brief may be brief or last for days
Chemistry of Hormones • Chemically, hormones are either: • Steroid or steroid-like hormones • Biogenic Amines • Peptide hormones
Steroid Hormones • Properties • Steroid hormones are derived from cholesterol • They are composed of hydrophobic lipids (insoluble in water) • Include • Estrogen • Testosterone • Androgens (weak sex hormones) • Aldosterone • Corticoids (hormones secreted from the adrenal cortex)
Biogenic Amines • Properties • Amines are synthesized from amino acids • Include • Norepinephrine • Epinephrine • Melatonin • Thyroid hormones (these are also hydrophobic, or water insoluble)
Peptide Hormones • Properties • Composed of long chains of amino acids (polypeptides) • Include • Hypothalamic hormones • Pituitary hormones • Pancreatic hormones • Gastrointestinal hormones
Water Solubility & Membrane Permeability • Steroid + Thyroid Hormones • Are hydrophobic – transported in the plasma attached to proteins • Cell membrane permeable – due to their hydrophobic properties, these hormones readily cross the phospholipid bilayer of the cell membrane. • All other Hormones • Are hydrophilic– freely dissolved in plasma • Cell membrane impermeable – these hormones do not cross the cell membrane, and must rely on 2nd messengers to relay a signal into target cells. • 2nd messenger – molecule that relays and amplifies a hormone signal into the cell.
Actions of steroid hormones A steroid hormone crosses the cell membrane Hormone combines with a protein receptor in the nucleus The hormone-receptor complex activates transcription of a specific DNA region The mRNA leave the nucleus into the cytoplasm The mRNA is translated into a protein.
Actions of Non-steroid hormones A non-steroid hormone reaches the target cell, The hormone binds to a membrane receptor Binding to the receptor activates an enzyme in the cell membrane (adenlyatecyclase) Adenlyatecyclase converts ATP into cyclic adinosine monophosphate (cAMP) cAMP is a second messenger that promotes a series of reactions leading to the cellular changes associated with the hormone’s action.
Control of Hormonal Secretions • Hormone secretion is generally controlled in three ways: • Negative Feedback • Hormone Deactivation • Up/Down Regulation
Negative Feedback The endocrine gland, or system controlling it senses the concentration of the hormone that gland secretes. When the level of a specific hormone drops below needed levels, the endocrine gland is stimulated to secrete more hormone. As the hormone concentration reaches the needed level, stimulation of that endocrine gland is reduced, and production of that hormone is reduced. Figure 13.10 Hormone secretion is under negative feedback.
Negative Feedback Indicates negative feedback inhibition. Figure 13.8 Examples of endocrine system control. (a) one way the hypothalamus controls the anterior pituitary, which in turn controls other glands (b) the nervous system controls some glands directly, and (c) some glands respond directly to changes in the internal environment. Figure 13.11 As a result of negative feedback, hormone concentration s remain relatively stable, although they may fluctuate slightly above and below average concentrations.
Hormone Deactivation Half-life: measures the time for half of the hormone molecules to be removed from plasma Time Hormone Concentration 0 minutes 100% 10 minutes 50% 20 minutes 25% 30 minutes 12.5% Example of half-life: a hormone with a half-life of 10 minutes, decreases in concentration by half every 10 minutes. Hormones are continually secreted in the urine, and broken down by enzymes, primarily in the liver.
Up/Down Regulation • Up-regulation increases the number of receptors on the target cell • Up regulation increases a cell’s sensitivity to a hormone • Down-regulation decreases the number of receptors on target cells. • Down regulation decreases a cell’s sensitivity to a hormone
EndocrineSystem Section 2, Chapter 13
Pituitary Gland (Hypophysis) Location: Lies at the base of the brain in the sellaturcica, connected to hypothalamus by a pituitary stalk (infundibulum) 2 Lobes: Anterior pituitary (adenohypophysis) Posterior pituitary(neurohypophysis)
Control of Pituitary Gland Anterior Pituitary Gland Posterior Pituitary Gland Releasing hormones secreted from hypothalamus regulates the anterior lobe. Nerve impulses from hypothalamus regulate the posterior lobe.
Anterior Pituitary Gland • Hypophyseal Portal System – • Releasing hormones secreted by the hypothalamus are conveyed to the anterior gland through Hypophyseal portal veins. • Releasing hormones act on specific target cells within the anterior pituitary gland • In response, the pituitary gland secretes tropic hormones that travel throughout the body acting on distant target cells. Tropic hormone = hormones that have other endocrine glands as their target
Example of hypophyseal pathway Releasing Hormone: Thyroid releasing Hormone (TRH) secreted from hypothalamus Tropic Hormone: Thyroid Stimulating Hormone (TSH) is secreted from the anterior pituitary Target Cells: Thyroid Hormone (Thyroxine) is secreted from thyroid glands
Anterior Pituitary Hormones Growth Hormone (somatotropin) Hypothalamic Control of GH: • Growth Hormone Releasing Hormone (GHRH): promotes GH secretions • Somatostatin: inhibits GH secretion • Target Cells: • Epithelial and Connective Tissue • Adipose Tissue • Liver Actions of GH: • Promotes cell growth and division, especially in skeletal muscles and chondrocytes • Promotes breakdown and use of fat for energy • Liver: promotes breakdown of glycogen for energy
Growth HormoneDisorders • Gigantism • Results from oversecretion of GH in childhood • Usually caused by a tumor of the pituitary gland • Hypopituitary Dwarfism • Insufficient GH during development • GH therapy may treat condition if administered before the epiphyseal plates ossify
Anterior Pituitary Hormones 2. Thyroid Stimulating Hormone (thyrotropin) Hypothalamic Control of TSH: Thyroid Releasing Hormone Target Cells: Thyroid Gland Actions: TSH promotes secretions of thyroid hormones (T3 & T4)
Thyroid Hormones and Negative Feedback Under normal conditions, T3 and T4 inhibit further secretions of TRH and TSH Iodine obtained from the diet is essential for thyroid hormone (T3 & T4) synthesis
An Iodine deficiency prevents the formation of Thyroid Hormones. TRH & TSH continually stimulate the thyroid gland without inhibition. Goiter = enlarged thyroid gland
Anterior Pituitary Hormones 3. Prolactin (mammotropin) • Hypothalamic Control of PRL: • Prolactin Releasing Factor: promotes secretion of prolactin • ProlactingRelease Inhibiting Hormone: inhibits PRL secretion Target Cells: Mammary Glands Actions: Prolactin promotes milk production
Anterior Pituitary Hormones 3. Adrenocorticotropic Hormone (ACTH) Hypothalamic Control of ACTH: Corticotropin Releasing Hormone Target Cells: Adrenal Cortex Actions: ACTH promotes secretions of hormones from the adrenal cortex (e.g. cortisol)
Anterior Pituitary Hormones Follicle Stimulating Hormone (FSH) 5. Luteinizing Hormone (LH) 4 & 5 = gonadotropes Hypothalamic Control: Gonadotropin Releasing Hormone (GRH) Target Cells: Gonads Male: testes Female: Ovaries Actions of gonadotropes: Follicle Stimulating Hormone: Female = promotes development of ovarian follicles Male = promotes development of sperm Luteinizing Hormone: Female = promotes the secretion of estrogens and progesterone Male = promotes the production of testosterone
Figure 13.15 Hormones released from the hypothalamus, the corresponding hormones released from the anterior lobe of the pituitary gland, and their target organs.
Posterior Pituitary Gland Structurally consists of neurosecretory cells Hormones are produced by the hypothalamus, then released from the posterior pituitary gland.
Posterior Pituitary Hormones Antidiuretic Hormone (ADH) (also called vasopressin) Target Cells: Kidneys & Blood Vessels Actions of ADH depend the receptors to which it binds • V1 receptors • Located within blood vessels • ADH, in high concentrations promotes vasoconstriction • May prevent a drop in blood pressure with profuse bleeding • V2 receptors • Located within tubules of kidneys • ADH promotes water reabsorption at the kidneys, and thus decreases water loss. • Alcohol inhibits ADH secretion, which explains its role as a diuretic.
Posterior Pituitary Hormones 2. Oxytocin Actions of Oxytocin • Females: • stimulates smooth muscle contractions in the uterus during delivery • Promotes ejection of milk from mammary glands Males: Function is unknown
EndocrineSystem Section 3, Chapter 13 The Peripheral Endocrine Glands
Thyroid Gland Location: The thyroid gland is located just inferior to the larynx. • Structure: • It consists of two lateral lobes connected by an isthmus • Contains several follicles.
Thyroid Gland Follicles Follicles consists of simple cuboidal epithelium & a colloid center Follicular Cells: produce T3 & T4 Coloid: contains Thyroglobulin, which is a storage form of thyroid hormones. Extrafollicular Cells: produce Calcitonin Follicular Cells take up thyroglobulin by endocytosis, then release the thyroid hormones into the bloodstream.
Thyroid Hormones Target Cells: T3 & T4 affect many cells throughout the body. • Actions of T3 & T4: Raise Metabolic Rate • Increase rate of carbohydrate catabolism • Enhance protein synthesis • Promotes the breakdown and use of lipids T3 & T4 are major factors in determining the basal metabolic rate (BMR) BMR = calories required to sustain life
Thyroid Hormones Follicular cells require iodine salts (iodide) to produce T3 and T4. T3 & T4 are hydrophobic molecules (insoluble in water) • Nearly 75% of thyroid hormones are attached to thyroid binding globulins. • Only the small amounts of the unbound hormones act on target cells.
Transport of Thyroid Hormones T4 accounts for 95% of circulating Thyroid Hormone, But… • T3 is physiologically more active. • T3 is 5 times as potent as T4 • T3 also has a 50-fold higher “free” concentration in the plasma (see figure below).
Thyroid Disorders Hypothyroidism – insufficient T3 & T4 • During infancy – results in intellectual disability, stunted growth, abnormal bone formation (cretinism) • During adulthood – low metabolic weight, sluggishness, poor appetite, and sensitivity to cold Infantile hypothyroidism Hyperthyroidism – excess T3 & T4 • Results in high metabolic rate, hyperactivity, weight loss, sensitivity to heat, and exophthamia (protruding eyes) • Grave’s Disease • Autoimmune Disorder: Antibodies target the thyroid gland and mimic TSH. Thyroid antibodies overstimulate thyroid gland, resulting in hyperthyroidism. Grave’s disease may cause exophthalmia
Calcitonin Extrafollicular cells (C-cells) secrete Calcitonin Calcitonin lowers blood calcium concentrations. Actions of Calcitonin • Stimulates Osteoblast activity – increases bone deposition • Inhibits osteoclast activity – reduces bone resorption • Promotes the excreting of calcium from the kidneys Major Source of Control: elevated blood calcium ion concentration
Parathyroid Glands • Location: • 4 small parathyroid glands are located on the posterior aspect of the thyroid gland • Hormone: PTH (parathyroid hormone) One parathyroid gland surrounded by thyroid follicles.
Parathyroid Hormone (PTH) Parathyroid Hormone elevates blood calcium levels. Actions of PTH: • Stimulates Osteoclast activity – increases bone resorption • Inhibits osteoblast activity – reduces bone deposition • Promotes calcium reabsorption from the kidneys. • PTH also promotes the activation of Vitamin D, which enhances calcium absorption from the small intestine. Major Source of Control: Inadequate blood calcium ion concentration
Figure 13.27 Parathyroid Hormone (PTH) stimulates bone to release Calcium (Ca2+) and the kidneys to conserve calcium. It indirectly stimulates the intestine to absorb calcium. The resulting increase in blood calcium concentration inhibits secretion of PTH by negative feedback.
Calcitonin and PTH have opposing effects on the levels of calcium ions in circulation. Both work together to maintain calcium homeostasis.
Adrenal Glands Location: The adrenal glands are located on the superior aspect of the kidneys. • Structure: • Adrenal glands are pyramid shaped organs that consist of two parts • Adrenal Medulla = secretions controlled by sympathetic nerve fibersAdrenal Cortex = Under hormonal control
Hormones of the Adrenal Medulla Nerve fibers control secretions: Hormones of the adrenal medulla are under control by the sympathetic division (fight or flight) of the ANS. • Hormones: Norepinephrine (noradrenalin) & Epinephrine (adrenalin) • Both are classified as catecholamines. • Actions: Effects are similar to sympathetic nerve fibers, but longer lasting. • Increases heart rate and force of contraction • Increases blood pressure • Increases metabolic rate • Increases blood glucose levels (primarily epinephrine) • Decreases digestion