Plasma Cell
Plasma Cell. Disorders. Monoclonal Gammopathies. Kristi McIntyre M.D. Texas Oncology 2004. Classification of Monoclonal Gammopathies. Monoclonal Gammopathy of Undetermined Significance

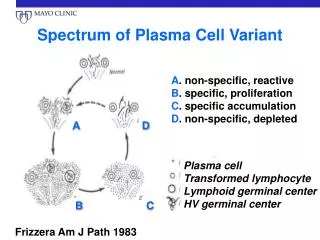
Plasma Cell
E N D
Presentation Transcript
Plasma Cell Disorders Monoclonal Gammopathies Kristi McIntyre M.D. Texas Oncology 2004
Classification of Monoclonal Gammopathies • Monoclonal Gammopathy of Undetermined Significance • Malignant Monoclonal Gammopathies Multiple Myeloma Smolderimg Multiple Myeloma Plasma cell leukemia IgD myeloma POEMS • Plasmacytoma • Malignant Lymphoproliferative disorders • Heavy Chain disease • Amyloidosis
Patient Profile • 61 year old female presented with rash to dermatologists in 2001. SPEP revealed 0.2 IgGlambda M-protein. Asymptomatic otherwise. 2 Breast ca M-protein 1 2001 2002 2003 2004
MGUS Denotes presence of an M-protein in a patient without a plasma cell or lymphoproliferative disorder • M-protein < 3g/dL • < 10% plasma cells in bone marrow • No or small amounts of M-protein in urine • Absence of lytic bone lesions,anemia,hypercalcemia or renal insufficiency • No evidence of B cell lymphoproliferative disorder • Stability of M-protein over time
MGUS Monoclonal Gammopathy of Undetermined Significance • 1% of adults in US • 3% of adults over age 70 years • 11% of adults over age 80 years • 14% of adults over age 90 years
MGUS MGUS can progress to monoclonal disease: IgA or IgG IgM Multiple Myeloma Primary Amyloidosis or related plasma cell disorder NHL CLL Waldentroms macroglobulinemia
MGUS • 1,384 patients MGUS Light chain Heavy chain IgG : 70% IgM :15% IgA :12% Kappa : 61% Lambda : 39% Concentration of uninvolved immunoglobulins reduced in 39% Kyle, R. A. et al. N Engl J Med 2002;346:564-569
MGUS prognosticators( predictors of progression): • Age • sex • Size of initial M-protein • Type of immunoglobulins • Hemoglobin • # of bone marrow plasma cells • Reduction of uninvolved imunoglobulins • Urinary light chains Kyle, R. A. et al. N Engl J Med 2002;346:564-569
Initial Monoclonal Protein Values in 1384 Residents of Southeastern Minnesota in Whom Monoclonal Gammopathy of Undetermined Significance Was Diagnosed from 1960 through 1994 Kyle, R. A. et al. N Engl J Med 2002;346:564-569
Probability of Progression among 1384 Residents of Southeastern Minnesota in Whom Monoclonal Gammopathy of Undetermined Significance (MGUS) Was Diagnosed from 1960 through 1994 Kyle, R. A. et al. N Engl J Med 2002;346:564-569 • Risk of progression to serious disease 1% per year
Patterns of Increase in Monoclonal Protein among 1384 Residents of Southeastern Minnesota in Whom Monoclonal Gammopathy Was Diagnosed in 1960 through 1994 Kyle, R. A. et al. N Engl J Med 2002;346:564-569
MGUS • The size of the M-protein at the time of recognition of MGUS is the most important predictor of progression • IgM & IgA monoclonal proteins have a greater risk of progression than an IgG M-protein • Reduction in uninvolved immunoglobulins & urine protein not significant
MGUS Management: • Periodic monitoring of serum protein electrophoresis • Interval of monitoring based on initial M-protein level • Monitoring should be at least annually LIFELONG • Risk does not go away with time “cumulative” probability of progression • ( 10% at 10 years , 25% at 25 years)
Patient Profile • 64 year old female hospitalized with severe low back pain for 3 weeks. Spine films negative MRI scan showed path fracture at L2 . Fatigue x 2 months ESR: 28mm/hr Creat : 0.6 Calcium 9.4 SPEP : M-protein : IgG kappa 4.8 g/dl
SPEP Multiple Myeloma 3-4 % patients have no serum or urine M-protein “non-secretory myeloma”
Patient Profile • Skeletal survey : diffuse osteoporosis • Bone marrow : 48% atypical plasma cells • L2 biopsy: plasmacytoma
Multiple Myeloma Diagnostic definition: Minimal criteria for diagnosis include a bone marrow containing > 10% plasma cells (or plasmacytoma) plus at least one of the following: • M-protein in serum >3 g/dL • M-protein in urine • Lytic bone lesions
Multiple Myeloma International Myeloma Working Group: • Presence of an M-protein in serum • Presence of bone marrow clonal plasma cells • Presence of related tissue or organ impairment (“CRAB”) C calcium R renal failure A anemia B bone lesions
Multiple Myeloma Bone Disease Conventional radiographs abnormal 80% of patients who present with multiple myeloma Osteopenia or osteoporosis 20% Focal lytic bone 57%% Pathologic fractures 20% Vertebral body compression fractures 20%
Multiple Myeloma MRI scan: • MRI scans of spine are an excellent assessment of bone marrow and myelomatous involvement. • >95% of patients with multiple myeloma have MRI abnormalities: Diffuse involvement of bone marrow Focal bone marrow lesions Heterogeneous bone marrow
Multiple Myeloma Osteolytic lesions occur through 2 mechanisms via production of cytokines by myeloma cells adjacent to bone: Stimulation of osteoclastic activity IL-6 Inhibition of osteoblastic activity
The Role of Wnt-Signaling Antagonist DKK1 on the development of Osteolytic Lesions in Multiple Myeloma Gene expression analysis NEJM Tian,E Dec 2003
Multiple Myeloma Bone disease: mechanism for osteolytic lesions BM microenvironment Myeloma cell overexpress DKK1 Osteoclasts osteoblast Tian,EDec 2003 NEJM
Multiple Myeloma Oncologic emergency Spinal cord compression occurs in 5 % of patients with multiple myeloma Managed with urgent: 1. Corticosteroids 2.neurosurgical intervention (laminectomy or anterior decompression) + radiation therapy to preserve neurological function 3. Radiation therapy alone
Multiple Myeloma Normochromic /normocytic anemia occurs in 75% patients at diagnosis
Multiple Myeloma Renal disease • Serum creatinine increased in > 50% at diagnosis • Creatinine >2g/dL in 20% of patients • Renal failure may be presenting manifestation Major causes: • Myeloma cast nephropathy • Hypercalcemia • Amyloidosis • Radiocontrast dye in a patient with myeloma
Multiple Myeloma Prognosticators: • Serum beta2 microglobulin- small protein synthesized by all nucleated cells;light chain moiety of HLA antigen • LDH reflects cell turnover • C-reactive protein reflects IL-6 levels
Multiple Myeloma • Cytogenetics Abnormalities associated with chromosome 13 carry a particularly unfavorable prognosis & respond poorly to therapy
Multiple Myeloma Management MGUS Multiple myeloma SMM SMM –smoldering multiple myeloma : M-protein >3g/dl ,bone marrow plasma cells >10%, but asymptomatic with no organ related problems SMM requires no intervention but close surveillance to assess stability
Multiple Myeloma • Treatment:Bisphosphonates: Pamidronate given monthly IV has been demonstrated to significantly reduce skeletal events in patients with Multiple Myeloma. Pamidronate* Placebo Skeletal events 21% 41% • Also reduces bone pain
Multiple Myeloma Management Multiple Myeloma Age <70 Transplant eligible Age > 70 Transplant ineligible Melphalan 0.15mg/kg x 7 d Prednisone 20mg po tid x 7d MP produces reponse rates of 50-60% & median survival of 2-3 years
Multiple Myeloma Conventional chemotherapy for induction: VAD -Vincristine Adriamycin Dexamethasone ORR CR* 84% 27% Modification of this regimen now with VDD(pegylated lipasomal doxirubicin) *Anderson,H:Br J Cancer 1995
Multiple Myeloma Thalidomide • old drug 1950’s for sedation & pregnancy induced nausea/vomiting • Withdrawn 1961-tetratogenic causing phocomelia • Deformities later found to be due to inhibition of developing fetal limbs vessels (anti-angiogenic) IMiDs (immunomodulatory agent )with antiangiogenic properties
Multiple Myeloma Thalidomide & dexamethasone • Myeloma patients with refractory disease underwent clinical trials producing 50% response rate (CR =PR ) • Median survival from start of therapy 38 months • Relatively minor side effects and taken orally • Major clinical trials now testing thalidomide /Dex as induction regimen
Multiple Myeloma Proteosome inhibitors (Velcade) FDA approval May 2003 Interferes with intracellular pathway that degrades proteins regulating cell cycle, apoptosis,angiogenesis
Multiple Myeloma • Autologous transplantation – recommended for advanced stage myeloma after induction therapy = age <70, good PS, normal renal function Tandem double better than single (41 vs 21 mos OS) • Allogeneic transplantation-insufficient evidence currently nonmyeloblative “mini” transplants as salvage
Poems(osteosclerotic myeloma) • Polyneuropathy dominating feature(100%),motor • Organomegaly-hepatosplenomegaly (50%) • Endocrinopathy hypogonadism, hypothyroidism (66%) • Monoclonal gammopathy • Skin changes hyperpigmentation, hypertrichosis Sclerotic bone lesions –97% Etiology of symptoms related to proinflammatory cytokines (VEGF)
Poems(osteosclerotic myeloma) Treatment : 5000cGy to osteosclerotic bone lesion
Patient Profile • 54 year old high profile male trial attorney went skiing with the “firm” in March 2002. Fell & fractured left humerus. Saw orthopedic surgeon on return to Dallas.”Pathologic fracture”bone survey otherwise negative: MRI spine negative. Lab: BM : <10% plasma cells SPEP 0.52% IgGkappa UPEP -negative DX : Solitary Plasmacytoma left humerus
Solitary plasmacytoma • Presence of single plasmacytoma without evidence of multiple myeloma • Younger median age at presentation (55yrs) • 50-60% will convert multiple myeloma within 10 years • Treatment: tumoricidal radiation to site (5000cGy) • Possible bone marrow collection/storage