Understanding Self-Funded Health Plans: Structure, Benefits, and Responsibilities
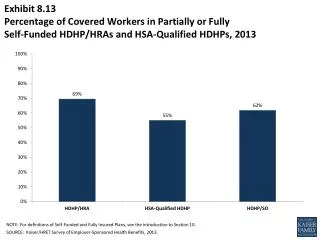
Self-funded health plans operate under federal laws, governed by ERISA, rather than state regulations. Managed by a Third Party Administrator (TPA), these plans consist of an Employer, a Health Insurance Company, and unique financial buckets: Claims Fund, Administrative Fund, and Stop-Loss Insurance. Employers make premium payments, which can be refunded based on claims usage. Self-funded plans often cost less than traditional options and may not adhere to all essential health benefits under the PPACA. Discover their advantages and how they can tailor employee healthcare solutions effectively.

Understanding Self-Funded Health Plans: Structure, Benefits, and Responsibilities
E N D
Presentation Transcript
Self-Funded Plans Presented by Insurance4Dallas
What Laws are Subject to Self-Funded Plans? Self-Funded plans, unlike traditional health Plans, are not subject to state laws. These plans are governed by federal law through the jurisdiction of the US Department of Labor under the “Employee Retirement Income and Security Act of 1974” (ERISA).
Who Issues a Self-Funded Plan? In most cases, Self-Funded Health plans are issued through a Third Party Administrator (TPA), which manages a three prong arrangement consisting of fulfillment of benefits, monthly premium payments and claim transactions which are transparent to the Employer.
Self-Funded Plan Defined In summary, a Self-Funded Health Insurance plan is an arrangement between: • A Health Insurance Company • AThird Party Administrator • The Employer
What is the Employer’s Responsibility? The Employer will make regular monthly premium payments to the TPA as they would normally for an insurance policy. However, premium payments will be allocated to three unique financial buckets overseen by the Third Party Administrator.
The “Three Unique Financial Buckets”? • Stop Loss Insurance Fund • The Administrative Fund • The Claims Fund Total Premium Claims Fund = Administrative Fund + Stop Loss Insurance +
The Employer’s Responsibility The Employer provides Health Benefits to their employees with the Employer’s own funds, designated or accumulated via monthly premiums to their Claims Fund, one of the unique financial buckets managed by the Third Party Administrator. Employer’s Claim Fund
Do I Have Refundable Premiums? In addition, money contributed to the Claim Fund’s Bucket during the preceding year is refundable, depending on how much of it was used to pay claims after individual deductibles are used. Business Owner
What is the Employer’s Risk? The Employer’s risk is limited by the amount of money accumulated or targeted by their annual contributions to the Claims Fund ONLY! Risk Management
How Does Stop Loss Insurance Work? Medical Bills that accumulate beyond the amount of savings in the Claims Fund, are covered by “Stop Loss Insurance” (SLI) premiums. SLI premium is one of the three unique financial buckets and absorbs all additional costs not covered by the Claims Fund. Stop Loss Premiums
How are Medical Claims Paid? Medical Claims are paid through and managed via a Third Party Administrator, of which the insurance company has issued a contract to manage all of their Self-Funded policies. This too is one of the three unique financial buckets paid with premiums. Third Party Administrator
Why Do Self-Funded Plans Cost Less? All of the preceding arrangements combined reduces the overall costs of health insurance to an employer. In addition, unlike other plans issued via the Patient Protection Affordable Care Act (PPACA), these Plans may not include all the “Ten Essential Health Benefits” and are medically underwritten, which reduce costs.
Unique Features of a Self-Funded Plan • 1099 Employees are eligible • Full Time work is 20 to 40 hours per week • Can cover employees at multiple locations • Four Tier Rates • Number of Children Impacts Rates
What is the Maximum Cost on Claims ? In Addition, ERISA managed policies mandate Self-Funded plans not exceed the maximum costs for claims to consumers per calendar year, which is $6350 for an individual and $12,700 for a family (in-network only). This is the same mandate in the PPACA.
What are the Advantages of a Self-Funded Plan? • May reduce Monthly Premium Costs • May get Premium Dollars Back at the End of the Year • Agents are free to be creative and offer other ways to reduce cost, such as eliminating your deductible.
How Else May We Reduce Costs? Ask Your Agent About - Insurance4Dallas John (Rick) Thornton (972) 219-6004 Mail@Insurance4Dallas.com • High Deductibles • GAP Insurance