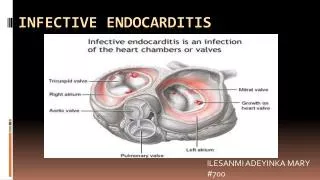
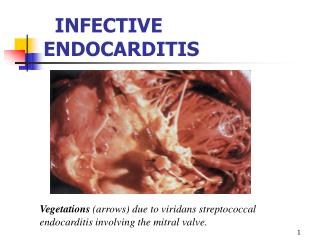
Infective Endocarditis
Infective Endocarditis. Dr. Hussein Amrat Cardiologist PHH-MOH. Microbiology: Organisms Responsible. Bacteria are the predominant cause Fungi Rickettsia Chlamydia Microorganisms vary dependent on risk factors predisposing patient to IE Staph Aureus= single most common cause.

Infective Endocarditis
E N D
Presentation Transcript
Infective Endocarditis Dr. Hussein Amrat Cardiologist PHH-MOH
Microbiology: Organisms Responsible • Bacteria are the predominant cause • Fungi • Rickettsia • Chlamydia • Microorganisms vary dependent on risk factors predisposing patient to IE • Staph Aureus= single most common cause
Native Valve Endocarditis • Streptococcus responsible for more than 50% of cases • Staphylococci • Enterococci • Infection occurs most frequently in those with preexisting valvular abnormality
Staphylococci • Causes endocarditis in those with normal and abnormal valves • Most are coagulase positive S.Aureus • Causes destruction of valves, multiple distal abscesses, myocardial abscesses, conduction defects, and pericarditis
Enterococci • Patients generally have underlying valvular disease • May occur following manipulation of genitourinary or lower gastrointestinal tract • Remainder of cases caused by Haemphilus Actinobacillus, Cardiobacterium, Eikenella, Kingella, Bartonella, or Coxiella Burnetti
Diagnosis • Negative culture can occur in 5% of patients. • 1/3 to ½ are negative due to prior antibiotic use • In patients with culture negative IE, advise lab to allow specialized testing to recover the causative organism which is needed to adequately treat
IDU associated IE • Skin flora and contaminated injection devices are the most frequent sources involved in IDU-associated IE • S. Aureus – Most common (50% of cases) • Streptococcal species • Gram negative Bacilli • Pseudomonas • Serratia species • Fungi • Candida
Prosthetic Valve Endocarditis • Most commonly occur during the perioperative period • S. epidermidis • Most frequently isolated organism • Early PVE (w/i 60 days of surgery) • Assoc. with valve dysfunction and fulminant clinical course • Late PVE (beyond 60 days postop) • Disease course is less fulminant • Mycotic PVE (Aspergillus and Candida) • Larger vegetations
Clinical Features • Acute IE – Rapid onset of high fevers and rigors with hemodynamic deterioration and death within days to weeks if not treated • Assoc. with highly virulent organisms such as Staph Aureus • Subacute IE – Indolent course with progressive constitutional signs and symptoms and gradual deterioration • Assoc. with avirulent organisms such as viridans streptococci
Clinical Features • Bacteremia can produce signs and symptoms that are often nonspecific usually within 2 weeks of infection • Most common course of disease (fevers, chills, nausea, vomiting, fatigue and malaise) • Fever is the most common symptom • Fever can be absent in pts with antibiotic use, antipyretic use, severe CHF, or renal failure • Prosthetic valve patient with a fever requires IE work up
Cardiac Clinical Features • Heart murmurs are present in up to 85% of cases of IE. • Most commonly regurgitant lesions secondary to valvular destruction • Acute or progressive CHF is the leading cause of death in patients with IE (70% of patients) • Distortion or perforation of valvular leaflets • Rupture of the chordae tendinae or papillary muscles • Perforation of the cardiac chambers (rare) • Valvular abscesses and Pericarditis • Heart blocks and Arrhythmias
Embolic Clinical Features • Extracardiac manifestations are the result of arterial embolization of fragments of the friable vegetation • CNS complications occur in 20-40% of cases (embolic stroke with MCA affected most frequently) • Retinal artery emboli may cause monocular blindness • Mycotic aneurysm may cause a SAH • IVDU can cause right sided lesions (tricuspid valve) – Pulmonary complications • Pulmonary complications ( pulmonary infarction, pneumonia, empyema, or pleural effusion) • Coronary artery emboli (Acute MI or myocarditis with arrhythmias) • Splenic infarction (LUQ abdominal pain) • Renal emboli (flank pain or hematuria)
Clinical Features • Persistent bacteremia can stimulate the humoral and cellular immune systems resulting in circulating immune complexes • Petechiae – Red, nonblanching lesions that become brown after several days (20-40%) • Conjunctivae, buccal mucosa, and extremities • Splinter hemorrhages – Linear dark streaks under the fingernails (15%) • Osler’s nodes – Small tender subcutaneous nodules that develop on the pads of the fingers or toes (25%) • Janeway lesions – Small hemorrhagic painless plaques located on the palms or soles • Roth spots – Oval retinal hemorrhages with pale centers located near the optic disc
Diagnosis • Diagnosis of IE requires hospitalization • Cultures • Echocardiogram • Clinical observation • Duke Criteria – 90% sensitive • Major Criteria • Minor Criteria
Major Criteria • Positive blood culture for: • Strep bovis, Strep viridans, or HACEK group • Staph aureus or Enterococci • Microorganisms c/w IE from persistent positive blood cultures • 2 positive blood cultures drawn >12 hrs apart • All of 3 or a majority of 4 or more positive blood cultures
Major Criteria • Echocardiographic involvement: • Mass on valve • Abscess • Dehiscence of prosthetic valve • New valvular regurgitation
Minor Criteria • Predisposition: Heart condition or injection drug use • Fever > 38 degrees C • Vascular: Emboli, conjunctival hemorrhages, janeway lesions • Immunological: Glomerulonephritis, osler’s nodes, roth spots, and rheumatoid fever • Positive blood cultures • Echocardiographic findings c/w IE
Duke Criteria • Definite infective endocarditis • Microorganisms demonstrated by culture or histologic examination of vegetation or emboli • Abscess with active endocarditis • Two major criteria • One major and three minor criteria • Five minor criteria • Possible endocarditis • Findings c/w IE that fall short of definite, but not rejected • Rejected • Firm alternate diagnosis • Resolution of manifestations of IE with abx for < 4 days • No pathologic evidence of IE at surgery or autopsy after 4 days of abx
DDx and Consideration of IE • IE should be considered in: • All febrile IDUs • Pts with a cardiac prosthesis and fever (or malaise, vasculitis or new murmur) • Pts with new murmur or change in murmur with evidence of vasculitis or embolization • Any cardiac risk factor with unexplained fever • Any patient with a prolonged fever (>2 weeks)
Evaluation of Bacteremia • All patients with suspected bacteremia should have blood cultures drawn in the ED prior to abx • Blood cultures should be drawn in 3 different sites • Minimum of 10 ml blood in each bottle • Minimum of one hour between first and last bottle
Diagnostic Tests • ECG should be done in all pts with suspected IE • Nonspecific usually • Conduction abnormalities ( new LBBB, Prolonged PR interval, new RBBB, complete heart block) • Junctional tachycardia • Chest Xray • Pulmonic emboli or CHF • Nonspecific lab tests • Anemia (70-90% of cases) • Elevated ESR (>90% of cases) • Hematuria
Echocardiography • Mandatory in all pts with possible IE • Transthoracic Echo(TTE) should be done first. • Specificity for vegetations is 98% • Sensitivity varies but it is the highest with IDUs because they more often have larger vegetations, right sided valvular lesions and favorable precordial windows. • Transesophageal Echo(TEE) has a higher sensitivity and specificity than TTE • Recommended for the following: • Prosthetic valves • Pts with obesity, chest wall deformities, COPD • Intermediate or high probability of IE
Treatment • Initial Stabilization • Rapid airway stabilization secondary to possible respiratory or hemodynamic compromise( acidosis, altered mental status, sepsis) • Cardiac decompensation may occur secondary to left sided valvular rupture • Intraaortic balloon counterpulsation may be indicated • Neurologic complications such as stroke • Standard stroke protocol
Empiric Treatment • Therapy of suspected Bacterial Endocarditis • Uncomplicated history • Ceftriaxone or nafcillin plus gentamycin • IVDU, Congenital heart disease, MRSA, current abx use • Nafcillin plus gentamycin plus vancomycin • Prosthetic heart valve • Vancomycin plus gentamycin plus rifampin • Most patients will require 4 to 6 weeks of antibiotic therapy
Surgical Treatment • Indications for surgical management: • Severe valvular dysfunction: Acute CHF or impaired hemodynamic status • Relapsing prosthetic valve endocarditis • Major embolic complications • Fungal endocarditis • New conduction defects or arrhythmias • Persistent bacteremia
Anticoagulation • Anticoagulation for native valve endocarditis has not been shown to be beneficial • Increase the risk of intracranial hemorrhage • Pts with prosthetic valves who are treated with anticoagulation can be maintained on their regimen with proper caution for CNS complications
IE Prophylaxis • Prophylaxis is indicated for: • Prosthetic heart valves • Congenital cardiac manifestations • Acquired valvular dysfunction • Hypertrophic cardiomyopathy • Mitral valve prolapse with documented regurgitation • History of endocarditis • Not indicated for the following: • MVP without regurgitation • Pacemakers • Physiologic murmurs • Prior CABG, angioplasty, ASD repair, VSD, or PDA
IE Prophylaxis • Dental, oral, respiratory or esophageal procedures • Amoxicillin or Ampicillin or Clindamycin • Genitourinary, gastrointestinal procedures • Ampicillin plus Gentamycin plus Ampicillin (post) or Amoxicillin • Alternate regimen: Vancomycin plus Gentamycin
Question 1: • T/F Streptococcus is responsible for more than 50% of Native Valve Endocarditis.
Question 2: • Embolic clinical features of infective endocarditis include: A) CNS complications B) Pulmonary complications C) Coronary Artery Emboli D) All of the above
Question 3: • Small hemorrhagic painless plaques located on palms or soles are called? A) Janeway lesions B) Osler’s nodes C) Roth Spots D) Splinter hemorrhages
Answers • 1) T • 2) D • 3) A