Lymphatic & Immune Systems
660 likes | 783 Views
The lymphatic system plays a crucial role in maintaining fluid balance by reabsorbing about 15% of fluid filtered by blood capillaries and returning it to the bloodstream. It is vital for immune defense, protecting against foreign cells and materials while also absorbing dietary lipids from the small intestine. Key components include lymphatic vessels, nodes, and cells, each contributing to the body's defense mechanisms—natural killer cells, T and B lymphocytes, and macrophages actively participate in immunity and the removal of pathogens.

Lymphatic & Immune Systems
E N D
Presentation Transcript
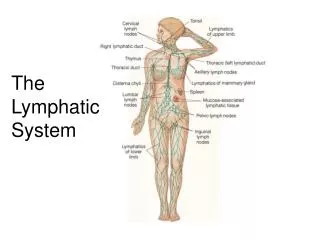
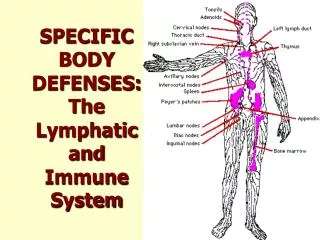
Lymphatic System • Reabsorbs about 15% of fluid filtered by blood capillaries & returns it to blood • Provides immunity & protection from foreign cells & matter in the body • Absorbs dietary lipids in small intestine & transports them to blood p 809
Lymph = fluid in lymphatic vessels • Usually clear, colorless fluid • Originates in lymphatic capillaries p 810
Lymphatic Vessels • Histology similar to veins • Thinner walls • More valves • Flow of Lymph • Like venous; low pressure & speed • Primary driving force is rhythmic contractions of vessels • Assisted by Milking & “Thoracic pump” p 811
Lymph Nodes • In-line filters that cleanse the lymph as it passes through • Reticular fibers act as a filter and delay microbes & debris • Macrophages & reticular cells remove about 99% of impurities from lymph p 817
Lymphatic Cells • Natural killer (NK) = lymphocytes that attack & destroy bacteria, transplanted cells, & host cells that are cancerous or viral-infected • Provide immune surveillance • T lymphocytes= mature in thymus & provide cell-mediated immunity • B lymphocytes = mature in bone marrow & provide antibody-mediated immunity
Lymphatic Cells • Macrophages = develop from monocytes into large highly phagocytic cells that destroy foreign matter and dead tissues & cells • Act as antigen-presenting cells (APCs) by breaking down foreign matter & displaying parts of it on their cell membrane
Lymphatic Cells • Dendritic cells = APCs that engulf foreign matter by endocytosis • Located in epidermis (Langerhans cells), mucous membranes, & lymphatic organs • Reticular cells = act as APCs in thymus • Form blood-thymus barrier that isolates lymphocytes from blood-borne antigens • Produce hormones that promote development & actions of T cells
Lymphatic Tissues • Lymphatic Nodules = dense masses of lymphocytes & macrophages • Some appear temporarily to fight infections • Permanent nodules are found in; • Lymph nodes • Tonsils • Appendix • Ileum of Sm. Intestine (Peyer’s Patches)
Red Bone Marrow • Source of all blood cells which enter the blood through sinusoids • Site where • B lymphocytes mature p 814
Thymus • Site where T lymphocytes mature • Shrinks to small size in adults • Secretes hormones that stimulate development and activities of T lymphocytes p 815
Tonsils. • Patches of lymphatic tissue that guard entrances to the pharynx • Surface has deep pits called crypts that help trap foreign materials p 819
Spleen: • Largest lymphatic organ • Acts as in-line filter for blood, with reticular fibers as filter and macrophages to ingest microbes & foreign material • “Erythrocyte graveyard” where worn out RBCs are phagocytized by macrophages p 819
Nonspecific Defenses • Protection against a wide range of pathogens • Pathogens = anything capable of causing disease • Bacteria • Viruses • Toxic chemicals • Radiation
Nonspecific Defenses • External Barriers • Leukocytes & Macrophages • Immunological Surveillance • Interferons • Complement System • Inflammatory Response • Fever
External Barriers • Skin • Mucous Membranes • Secretions; • Tears, saliva, urine, vaginal secretions, perspiration • Lysozymes = antibacterial enzymes that breakdown cell walls • Stomach acid
Leukocytes & Macrophages • Neutrophils • Phagocytosis, plus • Lysozymes release enzymes that trigger the respiratory burst, which produces; • Superoxide (O2-) • Hydrogen peroxide (H2O2) • Hypochlorite (HClO) • All highly toxic, so form a killing zone, that kills many bacteria & neutrophils
Eosinophils • Phagocytosis • Release toxic chemicals • Particularly effective against allergens & parasites • Basophils • Secrete histamine (vasodilator) • Secrete heparin (anticoagulant) • Stimulated by Eosinophils
Monocytes • Leave blood and become macrophages • Wandering (Free) macrophages • Fixed macrophages • Includes; • Dendritic cells • Microglia • Alveolar macrophages • Hepatic macrophages (Kuppfer’s cells)
Interferons • Small proteins • Released from viral-infected cells & bind to receptors on surface of nearby cells causing them to make antiviral proteins that prevent viral replication, thereby protecting those cells • Act as cell to cell signals to stimulate activities of macrophages and NK cells
Complement System • Group of 30 or more proteins • Important role in both Specific and Nonspecific defenses p 823
Membrane Attack Complex p 824
Immune SurveillanceNatural Killer (NK) Cellspatrol body looking to find & destroy bacteria, transplanted cells, viral-infected cells, & cancer cells. p 824
Inflammation • Inflammation is a local defensive response to injury, like trauma or infection • Purposes; • Limit spread of pathogens & eventually destroy them • Remove debris of damaged tissue • Start tissue repair • Words ending in itis denote inflammation of that tissue (arthritis, dermatitis, etc) • Signs = heat, redness, swelling, pain
Inflammation • Vasodilation triggered by histamine & other chemicals released from basophils, mast cells & damaged cells (flow=heat, redness) • These chemicals also cause Increased Blood Vessel Permeability as intercellular clefts widen & allow increased filtration of; • Fluids (swelling) • Leukocytes • Proteins (complement, antibodies, clotting factors)
Neutrophil Behavior • Margination = loose adhesion to vessel wall • Diapedesis = crawl thru gaps between cells • Chemotaxis = move toward chemical signals from damaged cells • Phagocytosis = engulf and digest foreign cells & molecules p 826
Neutrophils release signaling molecules to attract more phagocytes (neutrophils & macrophages) through chemotaxis • Macrophages engulf & destroy pathogens, and casualties, like tissue cells & neutrophils • Macrophages secrete colony-stimulating factors, that trigger increased production of more leukocytes (reinforcements)
What remains is Pus which is the dead cells, tissue debris & fluid that are eventually absorbed • Pain receptors are stimulated by; • Direct injury • Pressure from edema • Chemicals released by damaged cells (like prostaglandins & bradykinin) and bacterial toxins
Fever • Fever is an abnormal increase in body temp due to hypothalamus raising the set point for body temp. • Pyrogen (fever-causing agent) = interleukin-1, that triggers hypothalamus release of prostaglandin E (PGE) which raises set point for temp p 827
Specific Immunity • Specific immunity is directed at • one and only one specific pathogen • An initial exposure to a pathogen will create a memory • When exposed again to the same pathogen the body reacts so quickly that there is no noticeable illness.
Specific Immunity • Cellular (cell-mediated) immunity = lymphocytes directly attack & destroy foreign cells or diseased host cells where • Pathogen is inside human cells • Intracellular Viruses, Bacteria, • Protozoans, & Yeast • Cells of Transplanted Tissue & Cancer Cells
Specific Immunity • Humoral (antibody-mediated) immunity = antibodies tag or mark the pathogen for destruction by other mechanisms • Indirect attack by antibodies, • instead of immune cells directly • Extracellular Viruses, Bacteria, • Protozoans, & Yeast • Molecular (noncellular) pathogens • like, toxins, venoms and allergens
Antigens • Antigen = any molecule that triggers an immune response, normally proteins, polysaccharides, glycoproteins, & glycolipids • Antigenic Determinant Sites (epitopes) • = portions of the exposed surface of the antigen that actually make it an antigen, (trigger an immune response) • = sites where antibodies bind • Immune system must distinguish between; • Self vs. Nonself molecules
Haptens • Too small to be an antigen • Bind host macromolecule = then antigenic • Second exposure may not require binding • Include many allergens; • Cosmetics • Detergents • Industrial chemicals • Poison ivy • Animal dander
T Lymphocytes (T Cells) • “Born” in bone marrow, then to thymus where they become immunocompetent, meaning they get receptors on their surface for one antigen • Must pass a test to be sure they can recognize foreign antigens, but not attack self-antigens (only 2% pass) • Graduation = multiple & form clones of identical T cells that recognize that one specific antigen, then leave thymus as naive T lymphocytes
B Lymphocytes (B Cells) • Born and become immunocompetent in bone marrow (develop receptors on surface for specific antigen) • Must pass same test to be sure they will tolerate “self” cells and recognize foreign or “nonself” cells • Then multiple & form clones of identical B cells that recognize that one specific antigen and leave marrow as naive B lymphcytes
Major Histocompatiblity Complex (MHC) Proteins • Complex = genes are on chromosome #6 • Glycoproteins on surface of cells (except RBC), about 200,000 per cell • Unique to each person • Shaped like hotdog bun, they pick up antigens from inside the cell, migrate to the surface & hold them in their central groove • Class I on all cells (except RBC)
. Acting like an information relay, the MHC Class I (MHC-I) molecules retrieve bits and pieces of the proteins from inside the cell and display them on the cell surface. • MHC complexes essentially give • a read out of what's inside the cell
Antigen-Presenting Cells (APCs) • Phagocytosis of antigen • Break down into molecular fragments • Display (present) the epitopes on its MHC proteins • Class II MHC proteins on APCs only • macrophages, B cells, reticular & dendritic cells p 831
Cellular Immunity • Cytotoxic T (TC) cells = carry out direct attack on enemy cells • Also known as T8, CD8, or CD8+ cells because they have a surface glycoprotein for binding to other cells called CD8 • Helper T (TH) cells = promote actions of TC cells and play a key role in humoral immunity & nonspecific defenses • Also known as T4, CD4, or CD4+ cells due to CD4 glycoprotein
Cellular Immunity • Memory T (TM) cells = descended from cytotoxic T cells and provide memory of initial exposure to an antigen, providing for a very rapid response if exposed again
Immunity as a Three Act Play • Act One = Recognition • Act Two = Attack • Act Three = Memory • OR • “the three Rs of immunity” • Recognize • React • Remember
Recognition • Naive T cells inspect cells MHC proteins & antigens • Self antigens = okay • Viral proteins, abnormal antigens made by cancer cells = Respond • Like a sign that says, • “I’m infected” or • “I’m a cancer cell” • TC cells only MHC-I • TH cells only MHC-II p 833
T Cell Activation • Receptor on T cell surface must match foreign antigen on MHC • = binds MHC • Second binding called costimulation required for activation • Triggers clonal selection, repeated mitosis which produces a clone of T cells with receptors for same epitope p 833
T Cell Attack • Helper T cells secrete interleukins that; • Attract neutrophils & natural killer cells • Atrract macrophages & stimulate phagocytosis • Stimulate T and B cell mitosis & maturation p 833
T Cell Attack • Cytotoxic T cells attack & destroy cell with a release of chemicals • For example, Perforin creates pores in cell membrane that kill it • Recall the Membrane Attack Complex p 833