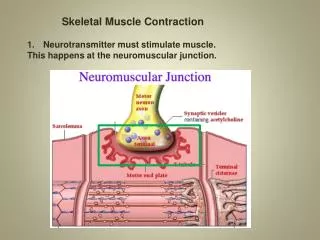
Skeletal Muscle
Skeletal Muscle. KINE 433-504 Physiology of Exercise Fluckey JD TR 9:35-10:50a MBL.TAMU.EDU K_Shimkus@hlkn.tamu.edu. Abbreviations/Definitions. mm – muscle CT – connective tissue myo – muscle sarco - flesh. Functions of Muscle.

Skeletal Muscle
E N D
Presentation Transcript
Skeletal Muscle KINE 433-504 Physiology of Exercise Fluckey JD TR 9:35-10:50a MBL.TAMU.EDU K_Shimkus@hlkn.tamu.edu
Abbreviations/Definitions • mm – muscle • CT – connective tissue • myo – muscle • sarco - flesh
Functions of Muscle • Movement – locomotion; muscle contractions also move body contents for respiration, circulation, digestion, urination, defecation, childbirth • Stability– maintain posture while resisting gravity and unwanted movements • Communication – muscles are used for facial expressions, other body language, speech, and writing • Heat production – As much as 85% of body heat, which is vital for enzymatic reactions
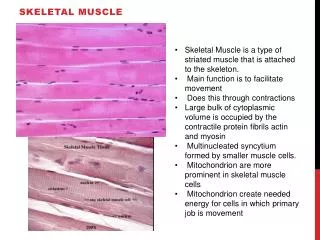
Types of Muscle • Skeletal - striated • w Voluntary muscle; controlled consciously • Over 600 throughout the body Cardiac - striated w Involuntarily controlled (unconscious) by the autonomic nervous system and hormones w Only in the heart • Smooth – non-striated • w Involuntary muscle • In the walls of blood vessels and internal organs
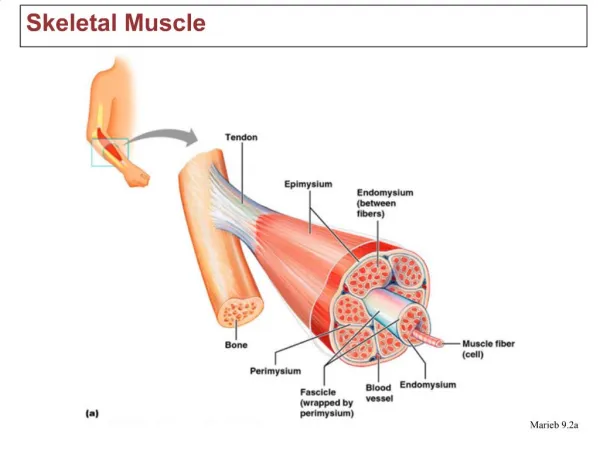
Muscle Structure • Epimysium (CT) encompasses a bundle of muscle cells (fasicle) • Fasiculi are encompassed in perimysium (CT) • Individual muscle fibers (cells) encompassed by endomysium (CT)
Muscle Cell = Muscle Fiber • Fibers are multinucleated • Myonuclei reside under the sarcolemma (plasma membrane) • Satellite cells reside between the sarcolemma and basal lamina • The sarcoplasm contains dissolved proteins, minerals, glycogen, fats, and organelles, such as myoglobin, which store oxygen
The Triad & Sarcoplasmic Reticulum • Made up of the transverse tubule (1) and the terminal cisternae (2) • The t-tubules allow transport of substances and passage of action potentials throughout the muscle fiber and signals for the release of Ca2+ by the SR • The sarcoplasmic reticulum& terminal cisternae stores and releases calcium during contraction
Myofibril wMyofibrils are the contractile “threads” that run the length of the muscle fiber, with several hundred to several thousand within a single fiber. w Myofibrils are made up of sarcomeres in series, the smallest functional units of a muscle. w A sarcomere is composed of filaments of two proteins, myosin and actin, which are responsible for muscle contraction. wThick filament: myosin, which has a globular head at one end wThin filament: composed of actin, tropomyosin, and troponin — is attached to the Z disks at the ends of the sarcomeres.
Arrangement of Filaments • The arrangement gives mm its striations • M-line – midline • A-band – dArk region, formed by thick filaments that overlap the thin filaments • H-band – lighter region within A-band, contains thick filaments only • I – band – the lIght region, composed only of thin filaments • Z – disc – protein disc to which thin filaments are anchored to at each end of a sarcomere, a narrow line in the middle of the I band • Sarcomere– the contractile unit of a muscle fiber, z-disc to z-disc
THICK FILAMENT Cross-bridge (actin binding site; ATP binding site; ATPase)
THIN FILAMENT (covers myosinbinding sites at rest) (Ca2+ binding site) (myosin binding site)
Motor Unit • Motor Unit – a single nerve fiber and all of the muscle fibers innervated by it • Motor units of eye contains 3-6 muscle fibers • The gastrocnemius contains ~1000 muscle fibers per motor unit • If a motor unit’s signal reaches threshold, it contracts all of its muscle cells
5. The Ca2+ binds to troponin on the thin filament, and the troponinpulls tropomyosin off the active sites, allowing myosin heads to attach to the actin filament. (continued) Excitation/Contraction Coupling 1. An α-motoneuron, with signals from the brain or spinal cord, releases the neurotransmitter acetylcholine (ACh) at the neuromuscular junction. 2. ACh crosses the junction and binds to receptors on the sarcolemma 3. This initiates an action potential 4. The action potential travels along the sarcolemma and down the t-tubules to the SR, which releases calcium ions (Ca2+)
Excitation/Contraction Coupling 6. ATP is hydrolyzed ( ADP + Pi + Energy), myosin neck cocks back myosin head 7. Myosin attaches to actin’s active spot 8. Pi comes off, resulting in the power stroke and contraction of sarcomere 9. ADP breaks off & new ATP binds to myosin, causing myosin head to release from cross-bridge 10.When calcium is removed from the cytosol, the SR takes up the Ca+2 via ATP-driven ion pumps 11.Lack of Ca+2contributes to removal of the ion from troponin, and myosin’s tight bind is broken, allowing for relaxation ? – What is rigor mortis?
Contraction • The pulling of the actin filament past the myosin results in muscle shortening and generation of muscle force
Architecture of Myofilaments 3D structure 1 myosin = 6 actin 1 actin = 3 myosin
Alterations of sarcomere during contraction • During contraction: • I band shortens • H band disappears • A band has no change • Z discs approach one another, sarcomere is shortened • Contraction velocity/ force dependent on fiber alignment
Physiological Classes of Muscle Fibers • 3 main types in humans • Type I aka Slow-twitch aka slow oxidative aka red • Slower type of myosin ATPase • Smaller diameter • Unit force is low • ATP synthesis is aerobic • Good resistance against fatigue • Myoglobin abundance is high • Mitochondria are abundant and large • Exhibits a relatively slow (100ms) twitch • Smaller motor units (10-180 muscle fibers) • Long-term aerobic (continuted)
Physiological Classes of Muscle Fibers • 3 main types in humans • Type IIa aka fast-twitch aka fast oxidative-glycolytic aka white • Intermediate fiber • Faster type of myosin ATPase • Larger diameter • Unit force is high • ATP synthesis is anaerobic • Modest resistance against fatigue • Myoglobin abundance is lower • Mitochondria are less abundant and smaller • Exhibits a relatively fast (50ms) twitch • Larger motor units (300-800 muscle fibers) • Short, high-intensity endurance (400m run) (continued)
Physiological Classes of Muscle Fibers • 3 main types in humans • Type IIx aka fast-twitch aka fast glycolytic aka white • Fastest type of myosin ATPase • Unit force is highest • ATP synthesis is anaerobic • Poor resistance against fatigue • Myoglobin abundance is lower • Mitochondria are least abundant and smaller • Exhibits a fast (50ms) twitch • Larger motor units (300-800 muscle fibers) • Short, high-intensity anaerobic (50m swim, 100m sprint)
Distribution of Fiber Type • Most muscles some combination of both Type I and Type II (both a and x). • Examples of exceptions include soleus and erector spinae (Type I), and gastroc and biceps brachii (Type II) • Studies have shown successful athletes with more of a particular muscle fiber type that coincides with their sport • Sprinters’ gastroc – 25% Type I • Marathoners’– 93-99% Type I
Determination of Fiber Type • Fast- or slow-twitch fiber characteristics appear early on in age, and studies have shown this to be linked to genetics. • Fiber type is determined by the neuron of the α-motor unit
Alterations of Fiber Type • Both resistance training and aerobic endurance training can contribute to altering the fiber composition of an adult, but the margins are small • Typically see changes around IIa, the intermediate fiber • With aging, muscle fiber type sees a shift from Type II to Type I • With spaceflight, muscle fiber type sees a shift from Type I to Type II
The All-Or-None-Response • Fibers in a motor unit are recruited when an α-motor neuron carries an action potential (impulse) from the central nervous system w All muscle fibers in the motor unit are recruited simultaneously w More force is produced by activating more motor units
Orderly Recruitment of Muscle Fibers • Principle of orderly recruitment states that motor units are activated in a fixed order • Motor units are “ranked” • Size principle states that the order of recruitment is directly related to the motor neuron size. • Slow-twitch fibers, which have smaller motor neurons, are recruited before fast-twitch fibers.
Thought Question From a biological perspective, why do you find within a synergistic group of anti-gravity muscles (like the calf muscles) one muscle that is primarily made up of slow fibers (i.e., soleus muscle), and other muscles primarily made up of fast fibers (i.e., gastrocnemius and plantaris muscles)?
Functional Classification of Muscles Agonists—prime movers; responsible for the movement Antagonists—oppose the agonists to prevent overstretching of them Synergists—assist the agonists and sometimes fine-tune the direction of movement
Frequency of action potentials (rate coding) Tension (force) produced by one motor unit Brooks et al., Exercise Physiology, 3rd ed., Mayfield, 2000.
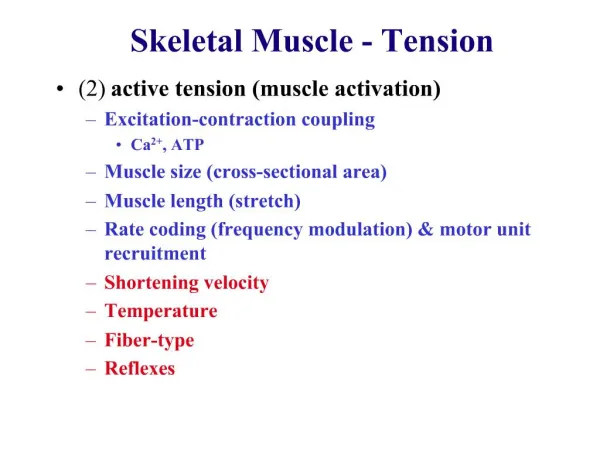
Factors Influencing Force Generation • Number of motor units activated • Rate of stimulation of the motor unit (rate coding) • Type of motor units activated (FT or ST) • Muscle size • Initial muscle length • Joint angle • Speed of muscle action (shortening or lengthening) • Muscle fiber arrangement (series or paralell)
TYPES OF MUSCLE ACTION Force > load Force = load Force < load
For Next Time • Review Intro Chapter PPT/notes • Review Muscle Chapter PPT/notes • Catch up on reading (1-55) • Read Neural Chapter (59-81) • Quiz Tuesday will cover information from today’s lecture
Muscle Biopsy • An important advancement in the field of exercise physiology was the implementation of the skeletal muscle biopsy. • It enabled scientists to have a ‘snapshot’ look at the cellular structure, morphology, metabolism and physiology of skeletal muscle. • There are a variety of tools available to the exercise physiologist if tissue biopsies are obtained: • Assessments of muscle fiber morphology • Assessments of metabolism • Assessments of turnover • DNA expression • Contractile/functional properties • Hormone function
Muscle Biopsy w Area near biopsy is shaved and cleansed with povidone.
Muscle Biopsy w Lydocaine is injected just below the skin, followed by an injection of from fascia to epidermis.
Muscle Biopsy • A small incision is made at the biopsy site using a sterile scalpel. • After the incision is made, a 5mm biopsy needle is inserted into the wound. • The needle is inserted into the ‘belly’ of the muscle, and with suction applied, the biopsy is removed via a sharp-edged trocar located within the biopsy needle. The biopsy needle is in the muscle for ~1-2 seconds until the procedure is completed.
Muscle Biopsy w After the biopsy is obtained, the sample is removed from the needle, and placed in the appropriate environment for experiments or analyses.
Muscle Biopsy w Pressure is applied to the biopsy site to ensure a minimum of bleeding, and dressed with a closure and pressure bandage.
Muscle Biopsy w Sample is mounted, frozen, thinly sliced, and examined under a microscope. w Samples may also be used for a variety of in vitro analyses, such as muscle protein synthesis. w Allows study of muscle fibers and the effects of acute exercise and exercise training on fiber composition/metabolism.