FONTAN CIRCULATION
FONTAN CIRCULATION. Dr Bijilesh u Senior Resident, Dept. of Cardiology, Medical College, Calicut. Normal mammal cardiovascular system double circuit connected in series —systemic —pulmonary powered by a double pump —the right and left heart.

FONTAN CIRCULATION
E N D
Presentation Transcript
FONTANCIRCULATION Dr Bijilesh u Senior Resident, Dept. of Cardiology, Medical College, Calicut
Normal mammal cardiovascular system double circuit connected in series —systemic —pulmonary • powered by a double pump —the right and left heart
Many complex cardiac malformations - one functional ventricle • Maintain systemic and pulmonary circulation - not connected in series but in parallel • Major disadvantages • arterial desaturation • chronic volume overload to single ventricle - in time impair ventricular function
1971, Fontan and Baudet • Goal was to create a circulatory system in which the systemic venous blood enters the pulmonary circulation, bypasses the right ventricle, and thus places the systemic and pulmonary circulations in series driven by a single ventricle • All shunts on the venous, atrial, ventricular and arterial level are interrupted
Advantages of a Fontan circuit include • (near) normalisation of the arterial saturation • abolishment of the chronic volume overload • Cost for such a circulation includes • Chronic hypertension and congestion of the systemic veins • decreased cardiac output • Cardiac output is no longer determined by the heart,but rather by transpulmonary flow
INDICATIONS FOR A FONTAN CIRCUIT • Cardiac malformation and a single functional chamber • dysfunctional heart valve • absent or inadequate pumping chamber • Tricuspid atresia • Pulmonary atresia with intact ventricular septum • Hypoplastic left heart syndrome • Double-inlet ventricle
SELECTION OF PATIENTS 1978, Choussat et al • 10 criteria for optimal results following the Fontan • age at operation between 4 and 15 years • presence of normal sinus rhythm • normal systemic venous connections • normal right atrial size • normal pulmonary arterial pressure (mean≤ 15 mmHg) • low pulmonary vascular resistance (4 Woods units/m2) • adequate-sized PA with diameter ≥75% of the aorta • normal left ventricular ejection fraction ≥ 60% • absence of mitral valve insufficiency • absence of complicating factors from previous surgeries
Refined by many centres • After repair • LA pressure must be low (determined by good LV fn) • transpulmonary gradient must be low (determined by the pulmonary vasculature) • Cardiac requirements nowadays are • unobstructed ventricular inflow (no atrioventricular valve stenosis, no regurgitation) • reasonable ventricular function • unobstructed outflow (no subaorticstenosis, and no coarctation
Pulmonary requirements • non-restrictive connection from systemic veins to the PA • good sized PA without distortion • a well developed distal vascular bed • (near) normal PVR - 2.5 U/m2 • unobstructed pulmonary venous return • Marc Gewillig , Heart 2005;91:839–846. doi: 10.1136/hrt.2004.051789
Fontan Procedure • Since its original description, the Fontan circuit has known numerous modifications • Early modifications of the Fontan procedure connected pulmonary arteries to the right atrium
Original procedure included • SVC to RPA anastomosis (Glenn shunt) • Anastomosis of RA appendage to LPA directing IVC flow through a valved homograft • Placement of a valved homograft at the IVS-RA junction • Closure of the atrialseptal defect
RA was included to - improve pulmonary blood flow, being a pulsatile chamber • Instead RA dilated and lost contractile function • Turbulence and energy loss • Decreased pulmonary blood flow de Leval et al
Right atrial–pulmonary circuits - obsolete • Replaced with newer techniques - direct connection between each vena cava and PA • Bypass the right atrium and right ventricle • More efficient cavopulmonary blood flow to the lungs – reduce risk for arrhythmia and thrombosis
Modern Fontan procedure involves connecting SVC and IVC to the RPA • Originally performed at the same time • Resulted in a marked increase in blood flow to the lungs - pulmonary lymphatic congestion, and pleural effusions • No longer performed together
Currently total cavopulmonaryFontan circulation done in two stages • To allow body to adapt to different hemodynamic states • Reduce overall surgical morbidity and mortality • Allows a better patient selection and intermediate preparatory interventions
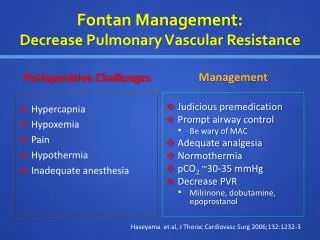
As no ventricular contraction to pump blood through the lungs, elevated PAH is an absolute contraindication for Fontan procedure • At birth, it is impossible to create a Fontan circulation • PVR is still raised for several weeks • Caval veins and pulmonary arteries - too small
Initially in the neonatal period, management must aim to achieve • Unrestricted flow from the heart to the aorta • coarctectomy • Damus- Kaye-Stansel • Norwood repair • Well balanced limited flow to the lungs • pulmonary artery band • modified Blalock-Taussig • Unrestricted return of blood to the ventricle • Rashkind balloon septostomy
Bidirectional Glenn Shunt / Hemi-fontan • At 4–12 months of age • First half of creating a total cavopulmonary circulation circuit • End-to-side anastomosis between SVC & RPA • RPA is not divided, resulting in blood flow from the SVC into the right and left PA • Children may remain cyanotic because blood from the IVC is not directed to the lungs
Bidirectional Glenn Shunt / Hemi-fontan • Cardiac end of the divided SVC is attached to MPA or the under surface of RPA • Lower stump of SVC is connected to IVC with a conduit • Open end of the SVC is either oversewn or occluded with a polytetrafluoroethylene patch • Allows Fontan circulation to be completed later
When patients reach 1–5 years of age total cavopulmonaryFontan circuit is completed • IVC connected to pulmonary artery with a conduit
Modified Fontan directing IVC flow through the lateral portion of the RA into PA via an anastomosis to the underside of the RPA • SVC flow is already directed into the RPA by a previous bidirectional Glenn shunt
Internal conduit - pass through the right atrial chamber • External conduit - run completely outside the heart to the right side of the right atrium
Intraatrial tunnel method • Conduit is constructed with both the lateral wall of the right atrium and prosthetic material • Inferior aspect of the tunnel is anastomosed to the IVC and the superior aspect is anastomosed to the pulmonary arteries • Conduit enlarges as the child grows - may be used in children as young as 1 year old • Internal conduit may lead to atrial arrhythmia
Extracardiac conduit method • Usually performed only in older than 3 years • PTFE tube graft is placed between the transected IVC and the pulmonary artery, bypassing RA • Entire atrium is left with low pressure - less atrialdistention, arrhythmia, and thrombosis
Cannot enlarge as the patient grows • Performed only in patients who are large enough to accept a graft of adequate size to allow adult IVC blood flow
Fenestrated fontan • small opening or fenestration may be created between the conduit and the right atrium • Functions as a pop-off valve (a right-to-left shunt) • prevent rapid volume overload to the lungs • Limit caval pressure • Increase preload to the systemic ventricle • Increase cardiac output • cyanosis may result from the right-to-left shunt
Fenestrations decrease postop pleural effusions • May be closed after patients adapt to new hemodynamics • Now, fenestrations are seldom created during the completion of the Fontan • improved patient selection and preparation • improved staging
Early increase in preload • Fontan circulation provides definitive palliation for complex cardiac lesions not suitable for biventricular repair • Some form of palliation is done in early infancy • Results in a parallel pulmonary and systemic circulation and a net increase in preload
Reduction of preload • Most patients undergo a staged transition to their complete Fontan via Bidirectional Glenn • BDG procedure leads to marked decrease in preload • Degree of reduction depends on prior pulmonary to systemic flow ratio, which often exceeds 2:1 • Reduction of preload results in reduced ventricular dilation and work
Abnormal systolic ventricular performance is rarely a problem in early years of palliation prior to Fontan • Is sustained or improved in most, after completion of Fontan circuit • It was shown that restoration of normal systolic wall stress was achieved in most individuals undergoing a Fontan procedure prior to the age of 10 years • Sluysmans T et al. Natural history and patterns of recovery of contractile function in single left ventricle after Fontanoperation. Circulation Dec 1992;86(6):1753–61.
Early diastolic dysfunction • Increase in wall thickness coincident with the acute reduction in end-diastolic volume • Result s in abnormalities of early relaxation & characteristically reduced early rapid filling • Consequently, much of diastolic filling is dependent on atrial systole • Early diastolic dysfunction negatively impact recovery after subsequent Fontan operation
Persistently abnormal early relaxation with worsening ventricular compliance markedly reduces ability of the ventricles to fill • Reduces pulmonary blood flow • Accounts for some of late failure seen in these patients • Worsen naturally with age as in the normal heart
Avoidance of factors known to lead to worsening compliance (persistent LV outflow tract obstruction, hypertension) is of fundamental importance
While diastolic abnormalities predominate early-on , systolic failure also becomes apparent in some patients late after the procedure
Systemic vascular bed • Many studies have reported uniformly elevated systemic vascular resistance after Fontan • Senzaki H, Masutani S, Kobayashi J, et al
Use of ACE inhibition in Fontan patients • Enalapril or placebo was given for 10 weeks in 18 patients approximately 14 years after the Fontan operation • Tendency to worsen exercise performance. • Reduced incremental cardiac index during exercise in the patients receiving enalapril • Kouatli et al ,Enalapril does not enhance exercise capacity in patients after Fontan procedure. Circulation Sep 2 1997;96(5):1507–12.
Many patients continue to receive ACE inhibition, in the hope of a beneficial effect when given chronically • It is possible that there are subgroups that may benefit e.g. severe systolic dysfunction • Presently no evidence for this therapy being beneficial
The veno-pulmonary circuit • Major evolution in the hemodynamic design of the Fontan operation since its inception • Initial right atrial to pulmonary connection has been abandoned in favor of more streamlined versions
Cardiac output - using respiratory mass spectrometry and an acetylene re-breathing method • There was no difference between the patient group at rest • Cardiac output & respiratory rate higher in the lateral tunnel group than the atriopulmonary group at low and moderate workloads • Rosenthal M et al Comparison of cardiopulmonary adaptation during exercise in children after the atriopulmonary and total cavopulmonary connection Fontan procedures. Circulation Jan 15 1995;91(2):372–8.
Work of breathing is a significant additional energy source to circulation in Fontan • Normal negative pressure inspiration has been shown to increase PBF after the atrial pulmonary connection and TCPC • Redington AN, Penny D, Shinebourne EA. Pulmonary blood flow after total cavopulmonary shunt. Br Heart J Apr 1991;65(4):213–7
Philadelphia group, using magnetic resonance flow measurements,have estimated that approximately 30% of the cardiac output can be directly attributed to the work of breathing in patients after the TCPC • FogelMA,Weinberg PM, Rychik J, et al. Caval contribution to flow in the branch pulmonary arteries of Fontan patients Circulation Mar 9 1999;99 (9):1215–21.
Positive pressure ventilation • Increasing levels of PEEP during positive pressure ventilation is adverse to Fontan circulation • Higher the mean airway pressure, lower cardiac index • Maintain with minimum mean airway pressure compatible with normal oxygenation and ventilation • Williams DB, Hemodynamic response to positive end-expiratory pressure following right atrium-pulmonary artery bypass (Fontan procedure). J ThoracCardiovasc Surg Jun 1984;87(6):856–61y
The pulmonary vascular bed • Low PVR is a prerequisite for early success after Fontan operation • Lower the total pulmonary resistance (PVR , pulmonary venous resistance and LA resistance) the better • LA resistance is influenced by the abnormal ventricular response
Structural pulmonary venous abnormalities • Naturally occurring • May evolve as a result of abnormal hemodynamics • Atriopulmonaryanastomosis- gross enlargement of RA may compress adjacent pulmonary veins
Abnormalities of arteriolar resistance adversely influence early outcome, in terms of morbidity and mortality • Few data available regarding the long-term effects of the Fontan circulation on the pulmonary vascular bed. • Pulmonary thromboembolism is not infrequent - lead to adverse changes in vascular resistance
Pulmonary artery flow in Fontan is relatively low velocity, laminar • Different to the normal pulsatile flow of pulmonary vascular bed in normal circulation • Release of nitric oxide from the endothelium is dependent on pulsatile flow in the normal circulation • Experimentally, reducing pulsatility leads to reduced NO production and an increase in vascular resistance • Nakano T et al, Pulsatile flow enhances endothelium-derived nitric oxide release in the peripheral vasculature. Am J Physiol Heart Circ Physiol Apr 2000;278(4):
Creation of Fontan circulation is palliative by nature • Proved good results with ideal hemodynamics • Substantial morbidity and mortality • in those with unfavorablehemodynamics • those who underwent older surgical techniques
Risk factors for complications include • elevated pulmonary artery pressure • anatomic abnormalities of the right and left pulmonary arteries • atrial-ventricular valve regurgitation • poor ventricular function