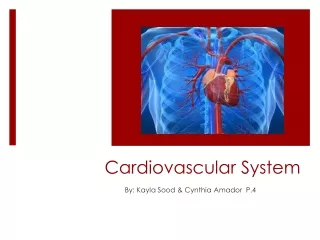
Understanding the Structure and Function of the Human Heart
The human heart is a complex organ located within the mediastinum, surrounded by the pericardium. It consists of three layers and is responsible for pumping blood throughout the body. The heart operates through a series of contractions and relaxations known as the cardiac cycle, producing sounds like "lubb" and "dubb." The heart's conduction system regulates heartbeat, influenced by ions like potassium and calcium. Blood vessels, arteries, and veins facilitate blood flow, with capillaries enabling nutrient exchange. Understanding these components is vital for grasping cardiovascular health.

Understanding the Structure and Function of the Human Heart
E N D
Presentation Transcript
Heart Structure • Hollow • Located within the mediastinum of the thorax. • Base is attached to several large blood vessels. • Distal end extends downward and to the left forming a blunt apex at the fifth intercostal space.
Pericardium or pericardial sac covers the heart.
The inner layer of the pericardium is called the visceral pericardium (epicardium) which covers the heart. The parietal pericardium forms the inner lining of the fibrous pericardium. The fibrous pericardium is tough and composed of mostly connective tissue. Between the layers is the pericardial cavity which has pericardial fluid that lubricates the membranes to reduce friction when the heart moves.
Tricuspid Valve Chordae Tendineae
Pulmonary and Systemic Bloodflow
Circumflex artery – supplies the blood to the walls of the left atrium and left ventricle. Left anterior descending artery – supplies the walls of both ventricles. Posterior interventricular artery – supplies the walls of both ventricles. Marginal artery – supplies the walls of the right atrium and right ventricle.
Heart Actions • Atrial systole is when the atria contract while the ventricles relax which is called ventricular diastole. • Thus systolic and diastolic blood pressure. • This series of contraction and relaxation is called a cardiac cycle.
Heart Sounds • “Lubb” heart sound occurs during the ventricular contraction when the A-V valves are closing. • “Dubb” heart sound occurs during ventricular relaxation when the pulmonary and aortic valves are closing. • A heart murmur is when the heart valves fail to close completely causing leakage.
Sinoatrial Node AtrioVentricular Node Atrioventricular Bundle Purkinje Fibers Heart Conduction System
Sympathetic & Parasympathetic Nervous Systems • Physical exercise, body temperature, and concentration of various ions affect heartbeat. • Branches of sympathetic and parasympathetic nerve fibers innervate the S-A and A-V nodes. • Parasympathetic impulses decrease heart action, sympathetic increases heart action. • Cardiac center in the medulla oblongata regulates autonomic impulses to the heart.
Effects of K+ & Ca2+ • Potassium and calcium are two ions that influence heart action and are the most important. • Potassium affects the electrical potential of the cell membrane. • Calcium ions are needed more for cardiac muscles
Conditions • Hyperkalemia (excessive potassium ions) decreases the rate and force of cardiac contractions. • Very high amounts may block cardiac impulses. • Hypokalemia is low potassium and can cause an abnormal arrhythmia. • Hypercalcemia increases heart action causing a prolonged contraction. • Hypocalcemia depresses heart action.
Arteries are strong, elastic vessels adapted for carrying blood away from the heart under high pressure. Three distinct layers: Endothelium – Inner most layer. Rich in elastic and collagenous fibers. Called the tunica interna. Middle layer – Tunica media. Smooth muscle fibers, thick layer of elastic connective tissue. Outer layer – Tunica externa. Attaches the artery to tissues. Contains vasa vasorum that gives Rise to capillaries
Vasomotor fibers stimulate smooth muscle to contract, thus reducing the diameter of the vessel. • This is called vasoconstriction. • Vasodilation changes the diameter of the vessel that influences the blood flow and pressure. • Arterioles are microscopic continuations of arteries that give off branches called metarterioles that join capillaries. • If arteries are cut they spurt blood due to the high pressure of the heart.
Venules are microscopic vessels That continue from capillaries into To form veins. Veins have valves and are Pushed back if blood begins To back up in a vein. Valves aid in the return of Blood to the heart. Arterial blood loss will cause a sympathetic nerve impulse to stimulate vein walls to return more blood to the heart to maintain blood pressure.
Capillaries exchanges nutrients, gases, and metabolic by-products between the Capillary blood and tissue fluid. Diffusion provides the most important means of transport. The pathways depend on lipid solubilities. Filtration causes a net outward movement of fluid at the arteriolar end of a capillary. Osmosis causes a net inward movement of fluid at the venular end of a capillary. Plasma proteins generally stay in the blood.
Blood Pressure • Arterial blood pressure is produced by heart action; it rises and falls with phases of the cardiac cycle. • Systolic pressure occurs when the ventricle contracts; diastolic pressure occurs when the ventricle relaxes. • Heart action, blood volume, resistance to flow and blood viscosity influence arterial blood pressure. • Blood pressure is controlled by cardiac output. • The more blood that enters the ventricle the greater the stroke volume and the greater the cardiac output.
Venous Blood Flow • Not a direct result of heart action. • Skeletal muscle contraction, breathing movements and vasoconstriction influence the flow. • Venous constriction can increase venous pressure and blood flow.