The Diabetic Foot
The Diabetic Foot. Angela Walker Diabetes Specialist Podiatrist. “Why Worry …?”. Approximately 15% of all people with diabetes will be affected by foot ulcer during their lifetime; 85% of diabetes-related amputations are preceded by foot ulcers (International Diabetes Federation) ;

The Diabetic Foot
E N D
Presentation Transcript
The Diabetic Foot Angela Walker Diabetes Specialist Podiatrist
“Why Worry …?” • Approximately 15% of all people with diabetes will be affected by foot ulcer during their lifetime; • 85% of diabetes-related amputations are preceded by foot ulcers (International Diabetes Federation) ; • Up to 70% of amputations are performed on people with Diabetes; • “Someone, somewhere, loses a leg because of diabetes every 30 seconds of everyday…” Lancet. 2005;366:1674
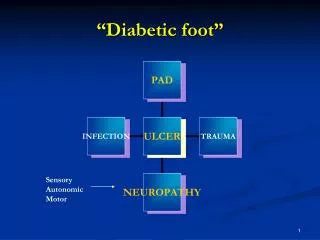
Multifactorial Aetiology • Vascular: macro and microangiopathy results in poor skin quality, poor healing and potential for ulceration and amputation. • Neuropathy causes loss of sensation, potential for injury, infection, leading to ulceration and possible amputation. • Delayed immune response: any injury to the foot is a potential cause for concern.
Diabetic Ischaemia • Micro-vascular and Macro-vascular • Pathology identical to non-diabetics • Earlier onset • Complications of high blood pressure, high cholesterol and smoking are all amplified by diabetes • 1 Cigarette reduces peripheral blood flow by 30% for 1 hour.
Skin Colour & Temperature History of Intermittent Claudication Faint or Absent Pulses Reduced or Absent Hair Anhydrosis & Fissures Changes in Nail & Rate of Growth Loss of Wrinkling of Skin Around Joints
Peripheral Neuropathy • Dysfunction of sensory, motor and autonomic nerves: • Loss of protectivepain sensation – increased susceptibility to foot ulceration • Motor – high medial longitudinal arch, clawed toes, prominent metatarsals • Autonomic – dry, fissured skin, sweat loss, distended dorsal veins
Well nourished tissue “Cramping, Tingling, Aching, Burning, Numbness” Diminished / absent sensation
Good DP and PT pulses Charcot Deformities Callus at pressure points Painless ulcerations
Neuropathic Warm Normal colour Palpable pulses Skin well nourished Callus at pressure points Ulceration plantar Neuroischaemic Cool Pale Pulses diminished/ absent Skin thin shiny no hair No callus fissuring at bony prominences Ulcers peripheral Differential Diagnosis
1. Callus formation 2. Subcutaneous haemorrhage 3. Breakdown of skin 4. Deep foot infection with osteomyelitis Pressure Ulceration
Osteomyelitis • Approximately 25% of foot ulcers will be affected by osteomyelitis (Young, Diabetic Foot Journal, 2008); • Surgery is not always necessary especially in patients without life or limb-threatening infections; • 82% of patients studied by Game and Jeffcoate (Diabetologia, 2008) were able to avoid surgery with one or more courses of antibiotics.
Foot problems can be Deceptive • Is the diabetic ulcer infected? • Compare the temperature of both legs • Check blood glucose levels • Pain is serious in the neuropathic foot • Localised superficial infection is probably the tip of the iceberg • Healed wounds need appropriate protection to prevent recurrence
Debridement • Neuropathic ulcers – need to be debrided as soon as possible to determine the depth of the ulcer and removal of necrotic tissue • Ischaemic ulcers – should not be debrided unless signs of infection present.
Wound Dressing • Aseptic technique; • Change dressings daily, more regularly when strike through noted on dressing; • Diabetic Foot wounds should be kept dry and clean at all times; • Do NOT soak the foot or bath/shower the patient; • Apply saline with gauze to clean wound surface.
Wound Dressings cont’d • Do NOT use hydrocolloid dressing as occlude and macerate the wound; • Simple wound dressing over ulcer site and secured; • Offload with appropriate foot wear/bed rest/turn patient regularly; • Review wound regularly and refer early if wound deteriorates; • Antibiotics?
High blood sugar inhibits body fighting infection Infection raises blood sugar The Cycle of Diabetic Infections Infection gets worse
Does the dressing: Stay intact & in-situ? Prevent leakage? Cause maceration/allergy or sensitivity? Reduce pain? Reduce odour? Is the dressing: Comfortable, conformable, flexible? Suitable for leaving in place for the duration? Easy to remove? Easy to use? Cost effective? Criteria for Wound Dressing Selection
Who to refer to the Diabetes Specialists in WPH • New Ulceration; • New Swelling; • New Discoloration over all or part of the foot; • People with painful leg and foot symptoms whose diabetic control is poor; • Deterioration of a presenting wound: • ↑Odour ↑Discharge ↑Redness ↑Pain ↑Swelling ↑Feeling unwell • Suspected Charcot – Plaster Nurse.
Where to Refer • Diabetes Specialist Team: • Dr Dove/Dr Akinsola • Ward 5 Ext ??? • Tissue Viability Nursing Team Ext ??? • Vascular Team Ext ??? • Plaster Room Ext ??? • Podiatry Department Ext 4221 • (Fax referral: stating Patient Diabetic with active ulcer)
On Discharge….. • Acute problem contact Diabetes Centre Podiatry, King Edward VII Hospital by: Fax on ext 6624. • Patient with diabetic complications. Referral to Community Podiatry Clinics based in Slough, Windsor, Ascot, Bracknell, Langley. • For type 1 or type 2 patient education or advice send for group education via the Diabetes Centre these Education Sessions are held in Community locations.
Summary of Care Planning • Good glycaemic control • Offloading pressure • Safe removal of callus • Safe removal of slough, necrotic tissue • Treat infection • Allow drainage of exudate • Encourage patient compliance/patient education • Best form of treatment is prevention