Antiemetics
Antiemetics. Vomiting :The act of vomiting and the sensation of nausea that accompanies it are protective reflexes that serve to rid the stomach and intestine of toxic substances and prevent their further ingestion. Pathophysiology of Emesis. Cerebral cortex. Cancer chemotherapy Opioids.

Antiemetics
E N D
Presentation Transcript
Antiemetics Vomiting :The act of vomiting and the sensation of nausea that accompanies it are protective reflexes that serve to rid the stomach and intestine of toxic substances and prevent their further ingestion
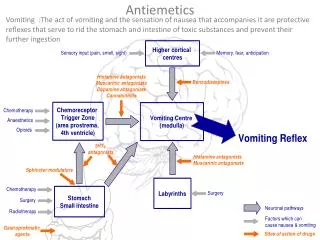
Pathophysiology of Emesis Cerebral cortex Cancer chemotherapy Opioids Smell Sight Thought Anticipatory emesis Chemoreceptor Trigger Zone (CTZ) Vestibular nuclei Vomiting Centre (medulla) Motion sickness Muscarinic Histaminic H1 Muscarinic, 5 HT3 & Histaminic H1 (Outside BBB) Dopamine D2 5 HT3,,Opioid Receptors Chemo & radio therapy Gastroenteritis (vagus) Pharynx & GIT 5 HT3 receptors
Indications of antiemetics 1- Chemotherapy-induced vomiting 2- Post irradiation vomiting 3- Postoperative vomiting 4- Vomiting of pregnancy 5- Motion sickness Group of drugs used as antiemetics Serotonin 5 HT3 Antagonists: Dopamine D2 Antagonist: Anticholinergics: H1 Antihistaminics
Serotonin 5 HT3Antagonist Potent antiemetics Mechanism of action: 1- Peripheral 5-HT3 receptor blockade on intestinal vagal afferents. 2- Central 5-HT3 receptor blockade in the vomiting center and chemoreceptor trigger zone Antiemetic action is mainly against: Emesis mediated by vagal stimulation (e.g. postoperative and chemotherapy) High first pass metabolism Excreted by liver & kidney No dose reduction in renal insufficiency but needed in hepatic insufficiency
Drugs Available Ondansetron Granisetron Dolasetron Palonosteron Adverse Effects The most common adverse effects are: 1- Headache and dizziness 2- Constipation or diarrhoea Indications Chemotherapy induced nausea and vomiting postradiation nausea & vomiting Vomiting of pregnancy Postoperative vomiting
Corticosteroids Corticosteroids have antiemetic properties Mechanism of action: possibly by suppressing peritumoral inflammation and prostaglandin production. Use: to enhance efficacy of 5HT3 receptor antagonists in the treatment of chemotherapy-induced vomiting.
Phenothiazines • Phenothiazines as promethazine are antipsychotic agents • Use: • Chemotherapy-induced vomiting • Radiotherapy-induced vomiting • postoperative nausea and vomiting • Mechanism of the antiemetic action: inhibition of central dopamine, muscarinic and H1 histamine receptors receptors
Butyrophenones • Butyrophenones as droperidole are antipsychotic agents • Mechanism of the antiemetic action: inhibition of central dopamine receptors • Use: • Chemotherapy-induced vomiting • Radiotherapy-induced vomiting • postoperative nausea and vomiting • Adverse effects: droperidol may prolong the QT inter, therefore, it should not be used in patients with QT prolongation (should only be used in patients who have not responded adequately to alternative agents).
Substituted Benzamides • 1- Metoclopramide • 2- Trimethobenzamide Mechanism of antiemetic action: Centraldopamine-receptor blockade Side effects: (mainly extrapyramidal): • Restlessness • Dystonias • Parkinsonian symptoms
H1 receptor antagonists and Anticholinergics Use: prevention or treatment of motion sickness. Adverse effects: sedation, dizziness,confusion, dry mouth, cycloplegia, and urinary retention. .
Benzodiazepines • Uses: • Benzodiazepines such as diazepam are used prior to the initiation of chemotherapy to reduce anticipatory vomiting or vomiting caused by anxiety
Cannabinoids(Dronabinol) • The mechanisms for the antiemetic effects is not known. • Pharmacokinetics. readily absorbed after oral administration It undergoes extensive first-pass metabolism with limited systemic bioavailability after single doses Mmetabolites are excreted primarily via the biliary-fecal route • Adverse effects include: • Euphoria or dysphoria, sedation and hallucinations • Abrupt withdrawal leads o withdrawal syndrome (restless, insomnia and irritability) • Autonomic effects (sympathetic) in the form of tachycardia, palpitation, conjunctival injection, and orthostatic hypotension. • Use: For the prevention of chemotherapy-induced nausea and vomiting
Control of GIT motility Neurogenic control of GIT moyility: the ENS • Enteric nervous system (ENS) is a collection of nerves within the wall of the GI tract responsible for the autonomous gastrointestinal activity. It consists of connected networks of neurons: • myenteric (Auerbach's) plexus, found between the circular and longitudinal muscle layers (responsible for motor control) • submucosal (Meissner's) plexus, found below the epithelium (regulates secretion, fluid transport, and vascular flow). Neurons in both plexuses release acetylcholine at their terminals. • Autonomic nervous system: Parasympathetic : act by releasing acetylcholine at nerve terminals. It causes contraction of muscles in the wall of the intestine and relaxation of the sphincters and increases gland secretion Sympathetic: act by releasing norepinephrine at nerve terminals. It causes relaxation of muscles in the wall of the intestine and contraction of the sphincters Types of cholinergic receptors are M2 and M3 (present in the GIT in a 4:1 ratio). M3 receptor is more important in muscle contraction.
Agents that increase GIT motility 1- Cholinergic agents Stimulate cholinergic receptors. Enhance contractions in an uncoordinated manner that produces no net propulsive activity. Not useful for treating motility disorders 2-Prokinetic agents enhance coordinated GIT propulsive motility. Prokinetic agents act at receptor sites on the motor neuron itself increasing the release of acetylcholine at the motor nerve terminal without interfering with the normal physiological pattern and rhythm of motility. Useful for treating motility disorders
Cholinergic Agents • Direct cholinergic agents • Stimulate cholinergic receptors in the wall of the GIT. 1- ACh is not used pharmacologically because: • it affects both nicotinic and muscarinic receptors • It is degraded rapidly by acetylcholinesterase. 2- Bethanechol • Muscarinic receptor agonist • Resists enzymatic hydrolysis. • In addition, it lacks real prokinetic efficacy,
Indirect cholinergic agents: Acetylcholinesterase Inhibitors. These drugs inhibit the degradation of ACh , allowing ACh to accumulate at sites of release. • Neostigmine has been used to treat paralytic ileus.
Decreased motility of GIT Decreased motility of the GIT results from suppression of ACh release from myenteric motor neurons mediated by stimulation of D2 dopaminergic receptors.
Prokinetic agents • Enhance coordinated GI T propulsive motility. • Mechanism of action: 1- Antagonize the inhibitory effect of dopamine on myenteric motor neurons, 2- Relieve nausea and vomiting by antagonism of dopamine receptors in the chemoreceptor trigger zone • Metoclopramide • Domperidone.
Substituted benzamides1-Metoclopramide (1): Pharmacological action: 1- Enhance coordinated GIT propulsive motility of the upper digestive tract where it increases lower esophageal sphincter tone and stimulates antral and small intestinal contractions. Metoclopramide has no clinically significant effects on motility of the colon. • Mechanisms of action (on GIT): • dopamine receptor antagonism • 5-HT4-receptor agonist • vagal and central 5-HT3-antagonist • sensitization of muscarinic receptors on smooth muscle 2- Antiemetic action: • Mechanism of action: • Antagonize dopamine receptors in the CTZ
1-Metoclopramide (2): Therapeutic Use • Nausea and vomiting that often accompany GI dysmotility syndromes. • Gastroesophageal reflux disease (symptomatic relief but not healing of esophagitis). • Gastroparesis where it improves gastric emptying. • Diagnostic procedures such as intestinal intubation or contrast radiography of the GI tract. • Postoperative ileus • Persistent hiccups
1-Metoclopramide (3): Administration: 1- Oral (rapid absorption) 2- I.m. in cases of nausea and vomiting 3- I.v. infusion in chemotherapy-induced vomiting
1-Metoclopramide (4): Adverse Effects: 1- Extrapyramidal effects(more commonly in children and young adults and at higher doses). • Tardive dyskinesia=repetitive, involuntary, purposeless movements (usually involve the face) like tongue protrusion, lip smacking, pursing of the lips and rapid eye blinking. It occurs with chronic treatment (months to years) and may be irreversible • Akathisia = restlessness and inability to sit still or remain motionless • Dystonias = muscular spasms of neck usually occurring acutely after intravenous administration • parkinsonian-like symptoms that may occur several weeks after initiation of therapy generally respond to treatment with anticholinergic or antihistaminic drugs and are reversible upon discontinuation of metoclopramide. 2- Galactorrhea by blocking the inhibitory effect of dopamine on prolactin release (infrequent)
2- Domperidone Pharmacological actions: 1-Enhance coordinated GIT propulsive motility of the upper digestive tract where it increases lower esophageal sphincter tone and stimulates antral and small intestinal contractions. It has no clinically significant effects on motility of the colon. Mechanism of action: dopamine D2 receptor antagonist 2- Antiemetic action Mechanism of action: dopamine D2 receptor antagonist (of D2 receptors in CTZ which is outside BBB)
Adverse effects: • No extrapyramidal side effects (can not cross the blood-brain barrier) • Galactorrhea (by inhibiting dopamine-mediated inhibition of the release of prolactin as the pituitary lacks blood-brain barrier)