The Urinary System
The Urinary System. Chapter 17. Chapter 17 Objectives. To understand: Renal hormones that control blood volume Renal control of acid-base balance Mechanism of action of diuretics Kidney disease Role of the kidneys in heart failure. Kidney Function.

The Urinary System
E N D
Presentation Transcript
The Urinary System Chapter 17
Chapter 17 Objectives To understand: • Renal hormones that control blood volume • Renal control of acid-base balance • Mechanism of action of diuretics • Kidney disease • Role of the kidneys in heart failure
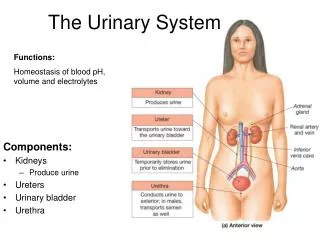
Kidney Function • Regulates plasma and interstitial fluid by formation of urine • In process of urine formation, kidneys regulate: • Volume of blood plasma, which contributes to BP • Waste products in plasma • Concentration of electrolytes • Including Na+, K+, HCO3-, and others • Plasma pH
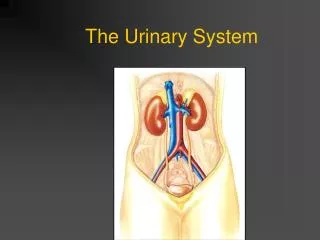
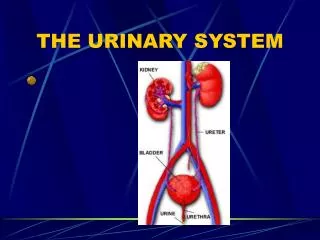
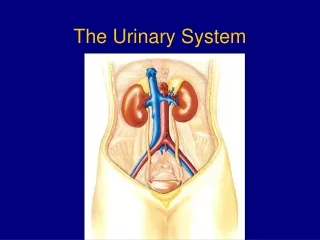
Structure of Urinary System • Kidneys – by vertebral column below diaphragm • About size of fist • Filtration and urine production • Urine flows into ureters • empty into bladder • Bladder – temporary storage for urine • Urethra – drains urine to the external environment
Structure of Kidney • Cortex – outer region • contains many capillaries • Medulla – consists of renal pyramids • separated by renal columns • Pyramids contain minor calyces, unite to form a major calyx
Structure of Kidney • Major calyces join to form the renal pelvis • Collects urine • Conducts urine to ureters which empty into bladder
Micturition Reflex (Urination) • Bladder – temporary storage for urine • Detrussor musclesmooth muscular wall • Stretching can cause spontaneous action potentials and contraction • Also innervated and controlled by parasympathetic ANS • Drugs for overactive bladders target muscarinic ACh receptors
Micturition Reflex (Urination) • Internal and external urethral sphincters – regulated by reflex center in sacral part of spinal cord • Filling of bladder – activates stretch receptors that send impulses to the micturition reflex center • Activates parasympathetic neurons with contraction of the detrusor muscle • Relaxes internal urethral sphincter creating sense of urgency • There is voluntary control over external urethral sphincter • Urination consciously initiated – descending motor tracts stimulus to micturition center • Inhibit somatic motor fibers of external urethral sphincter and urine is expelled
Nephron • Functional unit of kidney • responsible for forming urine • >1 million nephrons/kidney • Consists of small tubes or tubules • and associated capillaries • Filtrate – fluid formed by capillary filtration • Enters tubules, is modified, and leaves as urine
Renal Blood Vessels • Blood enters kidney through renal artery • divides into interlobar arteries into arcuate arteries into interlobular arteries
Renal Blood Vessels • Interlobular arteries give rise to afferent arterioles which supply glomeruli • Glomeruli – mass of capillaries inside glomerular capsule • Gives rise to filtrate that enters nephron tubule • Efferent arteriole drains glomerulus • Delivers that blood to peritubular capillariesand vasa recta • Blood from peritubular capillaries enters interlobular veins
The Tubules • Fluid formed by capillary filtration enters the tubules to be modified by transport processes • Resulting in fluid that leaves as urine • Reabsorption – transport of molecules out of the tubular filtrate (from the tubules) back to the blood • Secretion – transport of secreted molecules and ions • Move out of the peritubular capillaries into interstitial fluid, then • Transported across basolateral membrane of tubular epithelial cells, and into the • Lumen of the nephron tubule • Excretion – transport of urine out of the body
Nephron Tubules • Begins with glomerular capsule: • Transitions into proximal convoluted tubule (PCT) then to • Descending and ascendinglimbsof Loop of Henle (LH) and finally to • Distal convoluted tubule (DCT) • Tubule ends where it empties into collecting duct (CD)
Renal Corpuscle • Glomerular (Bowman’s) capsule and glomerulus • Where glomerular filtration occurs • Filtrate passes into proximal convoluted tubule
Proximal Convoluted Tubule • Walls – single layer of epithelial cuboidal cells with millions of microvilli • Increase surface area for reabsorption • Reabsorption – salt, water, and other molecules needed by the body • transported from the lumen through the tubular cells and into surrounding peritubular capillaries
Type of Nephrons • Corticalnephrons originate in outer 2/3 of cortex • Juxtamedullarynephrons originate in inner 1/3 cortex • Long LHs • Important in producing concentrated urine
Glomerular Filtration • Glomerular capillaries and Bowman's capsule form a filter for blood • Fenestrated capillaries contain large pores between its endothelial cells • Big enough to allow any plasma molecule to pass • 100-400 times more permeable than other capillaries
Glomerular Filtration • To enter the tubule filtrate must pass through narrow slit diaphragms • formed between pedicels of podocytes • Filtered molecules pass out of the fenestrae and through filtration slits • Enter the capsular cavity • Plasma proteins are excluded from the filtrate by the glomerular basement membrane and slit diaphragm
SEM of Glomerular Capillaries and Capsule • Pedicels interdigitate around the glomerular capillaries • Spaces between adjacent pedicels form ‘filtration slits’
Glomerular Filtration • Plasma proteins – mostly excluded from the filtrate because of large size and negative charge • Slit diaphragms lined with negative charges repel negatively-charged proteins • Some protein (especially albumin) normally enters the filtrate but most is reabsorbed, or transported across the PCT • Filtered albumin reabsorptionis performed by receptor-mediated endocytosis • Previously basement membrane was considered as the primary filter but recent research found • Genetic defects in proteins that compose the slit diaphragm results in massive leakage of protein in the filtrate (proteinuria)
Filtration Barrier • Separates the capillary lumen • from cavity of the glomerular capsule EM of filtration barrier between the capillary lumen and glomerular capsule
Formation of Glomerular Ultrafiltrate • Only a fraction of plasma proteins (green) are filtered • Smaller plasma solutes (purple) easily enter glomerularultrafiltrate • But most are reabsorbed
Glomerular Filtration Rate (GFR) • Volume of filtrate produced by both kidneys/minute • ~115 ml/minute in women • ~125 ml/minute in men • Totals about 180L/day (45 gallons) • Total blood volume average ~5.5 L • Most filtered water must be reabsorbed or death would ensue from water lost through urination
Regulation of GFR • Diameter of afferent arterioles – vasoconstriction or dilation affects rate of blood flow to glomeruli and thus GFR • Controlled by extrinsic and intrinsic mechanisms • Extrinsic regulatory mechanisms – produced by sympathetic innervation • Intrinsic mechanisms – renal autoregulation within the kidney
Sympathetic Effects • Sympathetic activity constricts afferent arteriole • Helps maintain BP • Shunts blood to heart and muscles
Renal Autoregulation • Defined as ability of kidneys to maintain relatively constant GFR in the face of fluctuating blood pressure • 2 mechanisms responsible: • Myogenic constrictionof afferent arteriole • due to smooth muscle responding to an increase in arterial pressure • Tubuloglomerular feedback • via effects of locally produced chemicals on afferent arterioles
Renal Autoregulation • Tubuloglomerular feedback – negative feedback between afferent arteriole and volume of filtrate • Increased flow of filtrate sensed by macula densa(juxtaglomerular apparatus) in thick ascending LH signals afferent arteriole to constrict
Reabsorption of Salt and H2O • PCT – returns most molecules and H2O from filtrate back to peritubular capillaries • About 180 L/day of ultrafiltrate produced but only 1–2 L of urine excreted/24 hours • Urine volume varies according to needs of body • Obligatory water loss– minimum of 400 ml/day urine needed to excrete metabolic waste produced by the body
Reabsorption of Salt and H2O • Reabsorption – transport of molecules out of the tubular filtrated back into the blood • Water is never transported – other molecules transported and water follows by osmosis
Reabsorption in PCT • Coupled transport of glucose and Na+ into the cytoplasm • Primary active transport of Na+ across basolateral membrane by Na+/K+ pump • Glucose is then transported out of the cell by facilitated diffusion • And reabsorbed into the blood
PCT – Salt and Water Reabsorption • Na+ actively transported out of filtrate and Cl- follows passively by electrical attraction :
Significance of PCT Reabsorption • PCT – about 65% Na+, Cl-, and H2O reabsorbed and returned into bloodstream • Additional 20% reabsorbed in descending loop of Henle • Thus 85% of filtered H2O and salt are reabsorbed early in tubule • Constant and independent of hydration levels • Energy cost 6% of calories consumed at rest • Remaining 15% reabsorbed variably depending on level of hydration
Concentration Gradient in Kidney • In order for H2O to be reabsorbed, interstitial fluid must be hypertonic • Osmolality of medulla interstitial fluid (1200-1400 mOsm) is 4X that of cortex and plasma (300 mOsm) • Concentration gradient results largely from loop of Henle • Allows interaction between descending and ascending limbs
The Countercurrent Multiplier System • Extrusion of NaCl from ascending limb makes surrounding interstitial fluid more concentrated • Concentration multiplied due to descending limb • Passively permeable to H2O • Fluid concentration increases • As surrounding interstitial fluid becomes more concentration • Deepest region of medulla • 1,400mOsm
Ascending Limb Loop of Henle • Thin segment in depths of medulla and thick segment toward cortex • Impermeable to H2O; permeable to salt • Thick segment Actively Transports NaCl out of filtrate • Active Transport of salt • filtrate becomes dilute (100 mOsm) by end of Loop of Henle
Transport of Ions in Ascending Limb • In thick segment – Na+ and K+ together with 2 Cl- enter tubule cells • Na+ then actively transported out into interstitial space, Cl- follows passively • K+ diffuses back into filtrate; some also enters interstitial space
Active Transport in Ascending Limb • Na+ – actively transported across basolateral membrane by Na+/ K+ pump • Cl- passively follows Na+ down electrical gradient • K+ passively diffuses back into filtrate
Countercurrent Multiplier System • Countercurrent flow and proximity allow descending and ascending limbs of to interact • This causes osmolality to build in medulla • Salt pumping in thick ascending part raises osmolality around descending limb, causes more H2O to diffuse out of filtrate • This raises osmolality of filtrate in descending limb causes more concentrated filtrate to be delivered into ascending limb • As concentrated filtrate is subjected to Active Transport of salts, it causes even higher osmolality around descending limb (positive feedback) • Process repeats until equilibrium is reached when osmolality of medulla is 1400
Vasa Recta • For countercurrent multiplier system to be effective: • Most of the salt extruded from ascending limbs must remain in the interstitial fluid of the medulla • Most of the water that leaves descending limbs must be removed by the blood • This is accomplished by the vasa recta • Thin-walled capillaries parallel LH of juxtamedullary nephrons • Walls permeable to water because of aquaporins channels, NaCl, and urea but not plasma proteins • Therefore colloid osmotic (oncotic) pressure in vasta recta is higher than in surrounding tissue fluid • results in movement of H2O from interstitial fluid into ascending vasa recta that can be removed from the renal medulla
Countercurrent Exchange in Vasa Recta • Important component of countercurrent multiplier • Permeable to salt, H2O (via aquaporins), and urea • Recirculates salt, trapping some in medulla interstitial fluid (maintains hypertonicity) • Reabsorbs H2O coming out of descending limb • Descending section has urea transporters • Ascending section has fenestrated capillaries
The Role of Urea in Urine Concentration 1. Urea diffuses out of inner collecting duct (in renal medulla) into interstitial fluid 2. Urea then passes into ascending limb • Recirculates in interstitial fluid of renal medulla • Urea and NaCl in interstitial fluid make it very hypertonic, so 3. Water leaves the CD by osmosis
Collecting Duct (CD) • Plays important role in water conservation • Is impermeable to salt in medulla • Permeability to H2O depends on levels of ADH
Homeostasis of Plasma Concentration Maintained by ADH • Secreted by post pituitary in response to dehydration • Stimulates insertion of aquaporins PM of collecting duct (CD) • ADH high – H2O is drawn out of CD by high osmolality of interstitial fluid • And reabsorbed by vasa recta
ADH Stimulation of Aquaporins • ADH absent – aquaporins located in membrane of IC vesicles within CD epithelial cells • ADH stimulates fusion of vesicles and • Insertion of aquaporins into PM • When ADH is withdrawn, PM pinches inward forms IC vesicle and removes aquaporin channels
Osmolality of Different Regions of the Kidney • Countercurrent multiplier system in LH and countercurrent exchange in vasa recta • Creates hypertonic renal medulla • Under influence of ADH CD becomes more permeable to H2O • Thus more H2O is drawn out by osmosis into hypertonic renal medulla and peritubular capillaries