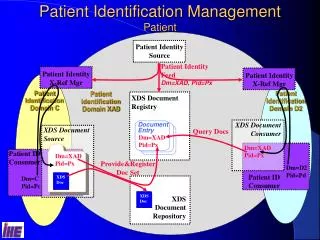
Patient Self-management
Patient Self-management. Connie Davis, MN, ARNP cld@conniedavis.ca. What do I hope to accomplish?. Define self-management, self-management support, and self-efficacy Describe what is known about self-efficacy and its influence on behavior and health

Patient Self-management
E N D
Presentation Transcript
Patient Self-management Connie Davis, MN, ARNP cld@conniedavis.ca
What do I hope to accomplish? • Define self-management, self-management support, and self-efficacy • Describe what is known about self-efficacy and its influence on behavior and health • Describe Brief Action Planning as an approach for improving self-management of MSK conditions • Link to resources for self-management
Think about a time when you accomplished something that challenged you…
Did that success lead to anything else? If so, what? Mt Outram, BC, photo by C Davis
Self-efficacy • People’s beliefs about their capabilities to perform specific behaviors and their ability to exercise influence over events that affect their lives. - Albert Bandura Mt Frosty, BC, photo by C Davis
What is self-management? • Self-management relates to the tasks that an individual must undertake to live well with one or more chronic conditions. These tasks include gaining confidence to deal with medical management, role management and emotional management. - Adams, Greiner and Corrigan (2004)
What is self-management support? • The systematic provision of education and supportive interventions by health care staff to increase patients’ skills and confidence in managing their health problems, including regular assessment of progress and problems, goal setting, and problem-solving support. - Adams et al 2004
Patient education and self-management support • Patient education • Information and skills are taught • Usually disease-specific • May assume that knowledge creates behavior change • Goal is often compliance • Health care professionals are the teachers • Self-management support • Skills to solve pt. Identified problems are taught • Skills are generalizable • Assumes that confidence yields better outcomes • Goal is increased self-efficacy • Teachers can be professionals or peers Bodenheimer et al JAMA 2002;288:2469
Stepped Care for Self-management Support Healthy Communities and Supportive Family, Friends, and Caregivers Expert Methods Advanced Approaches (MI, Case/Care Mgmt,PST, Group, etc.) Behavior Change Support: Goal Setting, Action Planning, Problem solving, Follow-up Health Literacy Culture Activation Patients as Partners, British Columbia
How does self-efficacy impact health? • High self-efficacy is associated with better • recovery level after a heart attack or heart surgery • coping with cancer or end-stage kidney disease • adherence to medication • lung function in chronic lung disease • living with chronic fatigue syndrome • pain management • adherence to prescribed exercise routines • control of alcohol or drug use • - cited in Bandura, 1998
Ways to increase self-efficacy • Skills mastery • Modeling • Reinterpreting symptoms • Social persuasion - Lorig & Holman, Ann Behav Med 2003
Skills mastery • Learning new skills and being successful • What can work: • Action plans to break big goals into smaller, more realistic steps • Education programs that teach skills Joshua Bell
Modeling • Seeing and hearing from others like you who have been successful • What can work • Group visits • Peer supports • Profiles, biographies of successful self-managers
Reinterpreting Symptoms • Symptoms are not just caused by the disease, but can be due to other factors. • What can work: • breathing techniques • relaxation • physical activity • healthy eating • sleep hygiene Poor sleep Physical limitations Fatigue Shortness of breath SYMPTOMS a vicious cycle Pain Stress/ anxiety Depression Difficult emotions Lorig et al, Living a Healthy Life with Chronic Conditions, Bull Publishing, 2012
Social Persuasion Encouragement, expression of hope • What can work • structure for success (ex: small action plans) • group visits • peer support • affirmations (not praise)
Chronic Disease Self-Management Program • Develop and studied by Kate Lorig and colleagues at Stanford • Lay-leaders, 6 sessions, 2 1/2 hours each • Addresses multiple conditions • Includes planning and problem solving, skill acquisition • “Everything you wish people knew” • Outcomes: improved health behaviors and health status, fewer hospitalizations some sustained for 2 years Lorig, Med Care 1999;37:5, 2002;39:1217
For the numbers people… Froud et al, 2009; Tools for Practice, 19 Mar 2012, Zhang et al, OA & cartilage 2010
NNT, cont References: Tools for Practice, 19 Mar 2012; 24 Jan 2011; Kroenke et al JAMA, 2009
What is Brief Action Planning? • A self-management support tool based on the principles and practice of Motivational Interviewing • It is • structured • patient-centered • evidence-informed Reims et al, Brief Action Planning White Paper, 2013 available at www.centreCMI.ca
Spirit of Motivational Interviewing • Compassion • Acceptance • Partnership • Evocation Miller W, Rollnick S. Motivational Interviewing: Preparing People for Change, 3ed, 2013
“Is there anything you would like to do for your health in the next week or two?” Behavioral Menu SMART Behavioral Plan Elicit a Commitment Statement “How confident (on a scale from 0 to 10) do you feel about carrying out your plan?” If Confidence <7, Problem Solve Barriers “Would you like to check in with me to review how you are doing with your plan?” Follow-up
Time to Practice • Work in pairs • Each will help the other make an action plan (or not) for something they really want to do (real play!) • We will go one step at a time, so I will stop you after each step.
Question 1 “Is there anything you would like to do for your health in the next week or two?”
Skill #1 Behavioral Menu • Offer a behavioral menu when needed or requested.
Behavioral Menu • “Is it okay if I share some ideas from other people who are working to improve their health? “ • If yes, share two or three ideas briefly in a group. • “Maybe one of these would be of interest to you or maybe you have thought of something else while we have been talking?” Exercise Resuming Daily Activities Weight management Taking meds Adapted from Stott et al, Family Practice 1995; Rollnick et al, 1999, 2010
Skill #2 SMART Behavioral Plan Action Planning is “SMART”: Specific, Measurable, Achievable, Relevant and Timed • What? • How much? • When? • Where? • How often? Based on the work of Locke (1968) and Locke & Latham (1990, 2002); Bodenheimer, 2009 .
Skill #3 Elicit a Commitment Statement • After the plan has been formulated, the clinician/coach elicits a final “commitment statement.” • Strength of the commitment statement predicts success on action plan. Aharonovich, 2008; Amrhein, 2003
Question 2 “How confident (on a scale from 0 to 10) do you feel about carrying out your plan?”
Skill #4 Problem Solving • Problem-solving is used for confidence levels less than 7. Bandura, 1983; Lorig et al, Med Care 2001; Bodenheimer review, CHCF 2005; Bodenheimer, Pt Ed Couns 2009.
Problem Solving “A ___ (the number they chose) is higher than a zero. That’s good.” “Is there something you could do to raise your confidence?” Yes No Behavioral Menu Revise plan, restate plan and repeat confidence measure
Question 3 “Would you like to check in with me to review how you are doing with your plan?”
Skill #5 Follow-up Follow-up builds confidence • Follow-up often with early action plans and decrease frequency as behavior is more secure. • Regular contact over time is better than 1x intervention. • Follow-up builds a trusting relationship Resnicow, 2002; Artinian et al, Circulation,2010
Follow-up “How did it go with your plan?” Success Partial success Did not try or no success Recognize success Recognize partial success Reassure that this is common occurrence “What would you like to do next?”
“Is there anything you would like to do for your health in the next week or two?” Have an idea? Not sure? Behavioral Menu Not at this time Permission to check next time SMART Behavioral Plan Specific Measureable Achievable Relevant Timely 1) Ask permission to share ideas. 2) Share 2-3 ideas. 3) Ask if any of these ideas or something else might work. Elicit a Commitment Statement “How confident (on a scale from 0 to 10) do you feel about carrying out your plan?” Confidence ≥7 Confidence <7, Problem Solving “Would you like to set a specific time to check back in with me so we can review how things have been going with the plan?” Follow-up “Would you like to set a specific time to check back in with me so we can review how things have been going with the plan?” “Would you like to set a specific time to check back in with me so we can review how things have been going with the plan?” “Would you like to set a specific time to check back in with me so we can review how things have been going with the plan?” “Would you like to set a specific time to check back in with me so we can review how things have been going with the plan?”
Tips for Giving Information and Advice • When? • They ask for information or advice • You ask permission to give it • You have a professional obligation to inform your client of something they don’t know
Tips for Giving Information and Advice How? ASK-TELL-ASK and respect their autonomy • ASK • Ask what they already know • TELL • Fill in any gaps or gently correct misunderstandings • Concentrate on key messages • ASK • Use Teach-Back • Ask what they think about your information or advice
What do we know about Brief Action Planning in practice? • Family practice • team sport • Question 1 asked in about half the visits • half of those make an action plan • 2/3 will do at least part of their plan • Specialty practice • in rheumatology, Question 1 asked routinely will result in ¾ of patients making action plans - unpublished data, CCMI and Handley, 2006
What resources are there to support people with MSK conditions?
Tools in MSK Toolkit • Arthritis education programs resource list • Resources for acute and chronic low back pain • CHARD • Local arthritis resources
Purpose of the Personal Health Record • Compile health information – share with new providers or foster communication between providers • Track symptom changes • Prepare for medical visit • Set action plan and monitor outcomes of those actions
Current Personal Health Record • 10 Sections • Personal and health care team information • My health care appointments • Allergies • Medical conditions/surgeries • Medications/supplements • Test results • Pain diary / General health diary • Notes for next health care visit • Reminder for future medical tests • My action plan
Arthritis Society Programs • Arthritis answers line • www.Arthritis.Ca • Arthritis self-management program • Chronic pain management workshop • Lifestyle makeover challenge • Take charge! Early intervention for OA • Joint works and water works
Talk to Your Doctor and other Health Care Professionals • Trained peer leaders • Started in Prince George, Victoria and the Lower Mainland • Workshop focused on • Informed shared decision-making • Communication skills for patients (prepare, ask, clarify, express concerns) • Partnering with many organizations as workshop providers