Surveillance data collection in IDSP
330 likes | 719 Views
Surveillance data collection in IDSP. Integrated Disease Surveillance Programme (IDSP) district surveillance officers (DSO) course. Outline of this session. Principles of surveillance data collection Diseases under surveillance Practical organization of data collection.

Surveillance data collection in IDSP
E N D
Presentation Transcript
Surveillance data collection in IDSP Integrated Disease Surveillance Programme (IDSP) district surveillance officers (DSO) course
Outline of this session • Principles of surveillance data collection • Diseases under surveillance • Practical organization of data collection 2
Surveys versus surveillance • Survey • Data collection at one point in time • Prevalence data • Surveillance • Ongoing, routine data collection • Incidence data Concepts 3
Reporting methods • Individual cases • Each and every case is reported • “Line listing” similar to an OPD register • Aggregated cases • Number of cases with selected characteristics • Usual methods in place in the contact of the Integrated Disease Surveillance Programme (IDSP) • Requires aggregation of the individual cases Concepts 4
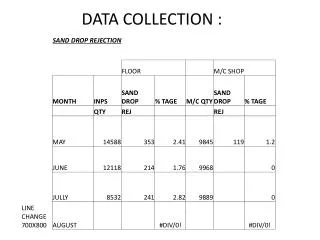
Example of a line listing for reporting individual cases of measles Concepts 5
Reporting of aggregated cases of diseases in (place) during (time) Concepts 6
Conditions under regular surveillance in integrated disease surveillance programme (IDSP) List 7
Rationale for the use of case definitions • Uniformity in case reporting at district, state and national level • Use of the same criteria by reporting units to report cases • Compatibility with the case definitions used in WHO recommended surveillance standards • Allow international information exchanges Collection 8
Types of case definitions in use More specificity Collection 9
What is an epidemiologically linked case? • One or few probable cases are confirmed by the laboratory • Other probable cases that most likely belong to the same cluster are considered “epidemiologically linked” if they had: • Exposure to the same source • Contact with a confirmed case • These “epidemiologically linked” cases are reported on a separate section of the “P” form Collection 10
Example of “epidemiologically linked” cases • Outbreak of 123 severe diarrhea cases with dehydration among adults • 7/12 rectal swabs confirmed the diagnosis of cholera • The non confirmed, probably cases become “epidemiologically linked” cases and should be reported as such in the separate section of the “P” form Collection 11
Summary of the data collection forms used for the various levels of case definition • Form “S” (Suspect cases) • Health workers (Sub centres) • Form “P” (Probable cases) • Doctors (Primary health centres, Community health centres, Hospitals) • Form “L” (Laboratory confirmed cases) • Laboratories Collection 12
Persons collecting information on syndromic reports (“S” forms) • Health worker, Male • Health worker, Female • Auxiliary nurse, midwife/ Public health nurse/ Lady health visitors • Accredited Social health Activities (ASHA) • Anganwadi Worker • Link worker • Village Health Guide/Community Health Volunteer • Panchayat/ Community member Collection 13
Core sources of information for “S” forms • Health workers visit diary (40 houses / day) • Require regular maintenance and entries • May include information from other co-workers/functionaries • Sub centre out patient department register • Usually records identifiers and drugs dispensed • Not syndromes • Age often inadequate, unclear or absent • No summary • Does not usually include diary entries • Similar other diary and register with other workers • Malaria slide register in some states Collection 14
Revised malaria form (MF) 11(Revised to fit IDSP format, to be ultimately merged) The new malaria form takes into account IDSP classification of fever cases for better coordination Collection 15
Completion and transmission of form “S” • Completion • Health worker (Female) usually completes the form on the basis of registers • Ideally the new IDSP “S” register • Or other registers (OPD, house visits) • Transmission • Health worker (Male) usually takes the form to health supervisor/ inspector at the PHC on MONDAY • In some places: • The form reaches the block PHC directly • The form is communicated to the district by phone Collection 16
Problems associated with completion and transmission of form “S” • While compiling records for “S” forms the core registers may not be consulted (although it should) • The report may cover a period modified to suit convenience of meeting date • Incomplete information usually gets dropped Collection 17
Check list for “S” form completion • Filled in time (Friday-Saturday) • Filled using figures from registers only • Tally mark by health worker • Entries in the “S” form can traced back to individual cases in the registers • Each cell filled in individually • Detection of rising trends of disease Collection 18
Applying the checklist: Making sure all numbers in the “S” form come from individual cases in the “S” register S register S form 19
Poor data entry on form “S”:Some cells are not filled ------- NIL ------- 20
First level of consolidation: The sector primary health centre (PHC) • Sector PHC • Approximate population: 20-30,000 • Sometimes more • Target date for receipt of forms is MONDAY • 5-6 “S” forms expected • Transmission to the block PHC or community health centre (CHC) on Tuesday • “S” forms forwarded • PHC “P” form added • Responsibility: Pharmacist (Usually) • Often a weak link Collection 22
Summary: The flow of the “S” form Form “S”transmission Form “S”completion 23
Sources of data for “P” form • Primary health centre outpatient register • Records name of the patient • Social status (e.g., Below poverty line) • Primary health centre pharmacist • Register with name, outpatient number etc. • At some places there is a medical officers individualized register as well • New IDSP “P” register Collection 24
Completion of the “P” form in primary health centres (PHCs) • Focal person: • Pharmacist • Public health nurse • Various combinations in practice to fill “P” form • Pharmacist register does not have diagnosis • OPD registers do not have any disease/treatment info • Doctors register generally incomplete and do not cover all patients • Checklists similar to the one used for the “S” Form can be used to assure data quality at this level Collection 25
Applying the checklist: Making sure all numbers in the “P” form come from individual cases in the “P” register “P” register “P” form Collection 26
Block primary health centre (BPHC) Community health centre (CHC) “S”, “P” and “L1” forms converge at the block level Collection 27
Information from other reporting sources Big labs“L2” form Small labs“L1” form HospitalsConsolidated “P” forms Clinics and practitioners “P” forms Quacks and traditional practitioners “S” forms Collection 28
Reporting units • All government entities should be part of the reporting network • All local health institutions should be made part of the network in phases • Gradually the data should be disaggregated by reporting unit to pinpoint the source and demarcate local trend line for particular diseases • Ultimately we need to report incidences in relation with the denominator • CDC: Count, divide compare • Compare rates rather than numbers Collection 29
Take home messages • IDSP is mostly based upon aggregated reporting • Know the diseases under surveillance • Understand the data flow of each of the case definition levels • “S” forms • “P” forms • “L1/2” forms 30
Additional reading • Section 2 and 3 of IDSP operations manual • Module 5 of training manual • Format and guidelines for reporting of information on disease surveillance (electronic manual) • IDSP manual 31