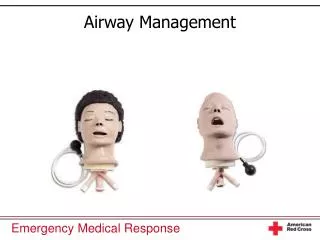
BASIC AIRWAY MANAGEMENT
BASIC AIRWAY MANAGEMENT. Basic Airway Objectives. Upon completion the student will be able to: Describe the anatomy of the airway and the physiology of respiration. Explain the primary objective of airway maintenance Identify commonly neglected prehospital skills related to the airway

BASIC AIRWAY MANAGEMENT
E N D
Presentation Transcript
Basic Airway Objectives Upon completion the student will be able to: • Describe the anatomy of the airway and the physiology of respiration. • Explain the primary objective of airway maintenance • Identify commonly neglected prehospital skills related to the airway • Describe assessment of the airway and the respiratory system • Describe the modified forms of respiration and list the factors that affect respiratory rate and depth • Discuss the methods for measuring oxygen and carbon dioxide in the blood and their prehospital use.
Basic AirwayObjectives • Define and explain the implications of partial airway obstruction with good and poor air exchange and complete airway obstruction • Describe the common causes of upper airway obstruction, including: • The tongue • Foreign body aspiration • Laryngeal spasm • Laryngeal edema • Trauma
Basic AirwayObjectives • Describe complete airway obstruction maneuvers, including: • Heimlich maneuver • Removal with magill forceps • Describe causes of respiratory distress, including: • Upper and lower airway obstruction • Inadequate ventilation • Impairment of respiratory muscles • Explain the risk of infection to EMS providers associated with airway management and ventilation
Basic AirwayObjectives • Describe manual airway maneuvers including: • Head0tilt/chin-lift maneuver • Jaw-thrust maneuver • Modified jay-thrust maneuver • Discuss the indications, contraindications, advantages, disadvantages, complications, special considerations, equipment, and techniques of the following: • Upper airway and tracheobronchial suctioning • Nasogastric and orogastric tube insertion
Basic AirwayObjectives • Oropharyngeal and nasopharyngeal airway • Ventilating a patient by mouth-to-mouth, mouth-to-nose, mouth-to-mask, one/two/three person bag-valve mask, flow-restricted oxygen-powered ventilation device, automatic transport ventilator • Compare the ventilation techniques used for an adult patient to those used for pediatric patients, and describe special considerations in airway management and ventilation for the pediatric patient
Basic AirwayObjectives • Identify types of oxygen cylinders and pressure regulators, and explain safety considerations of oxygen storage and delivery, including steps for delivering oxygen, from a cylinder and regulator • Describe the indications, contraindications, advantages, disadvantages, complication, liter flow range, and concentration of delivered oxygen for the following supplemental oxygen delivery devices: • Nasal cannula • Simple face mask
Basic AirwayObjectives • Partial rebreather mask • Nonrebreather mask • Venturi mask • Describe the use, advantages, and disadvantages of an oxygen humidifier
ADMINISTRATION Oxygen is the most important drug that we can give a patient. Without it, the body’s cells die and thus the patient dies also. • Room air contains approximately 30% oxygen
ADMINISTRATION • Usually stored in seamless, steel cylinders - color GREEN • Sizes and Capacity: * “D” 350 L * “E” 600 L * “M” 3,000 L • Pressure: 2,000-2,200 psi
ADMINISTRATION Pin Index Safety System (PISS) • Prevents interchanging different gases and regulators Delivery 1. Demand Valve * Activated manually or by negative pressure
ADMINISTRATION 2. Flow Meter (Two Types) • Pressure Compensated * Small ball in a calibrated tube; affected by gravity, measures actual delivered flow; found in Units mounted on wall. • Bourdon Gauge * Not affected by gravity; records a higher reading when an obstruction blocks tubing; used on portable O2 tanks
ADMINISTRATION • Nasal Cannula: 2-6 lpm; 25-50% • Basic Mask: 6-10 lpm; 35-60% • Partial Rebreather: 10 & higher lpm; 60% • Non Rebreather: 10 & higher lpm; 60-95% • Demand Valve: 100 lpm; 100% • BVM: 0 lpm 21% 15 w/o reservoir 50% 15 w/reservoir up to 95%
MANUAL TECHNIQUES • Head Tilt/Chin Lift Opens most common cause of obstruction, the tongue
MANUAL TECHNIQUES • Modify for suspected spinal injury: 1. Tongue/jaw lift 2. Modified jaw thrust
BODY POSITION • Left or right lateral positioning of a patient aids airway maintenance by allowing fluids/vomitus to drain out • Only to be used when spinal injury is NOT suspected • If spinal injury is suspected, the patient must be secured solidly to a rigid board so that the body can be turned to the side as a total unit.
OROPHARYNGEAL AIRWAY (OP AIRWAY) • Semicircular, disposable and made of hard plastic. Guedel and Berman are the frequent types. • Guedel is tubular and has a hollow center. • Berman is solid and has channeled sides. • Displaces the tongue away from the posterior pharyngeal wall.
OP AIRWAY Even when in place, it is necessary to maintain manual positioning of the airway by a head-tilt, chin-lift or jaw-thrust maneuver. INDICATIONS • Adjunct for airway control, determines presence of gag reflex. • Unconscious/unresponsive
OP AIRWAY INDICATIONS • Remove the airway if patient regains a gag reflex • May be inserted as a bite block after successful intubation
OP AIRWAY SIZING • Hold the airway next to the side of the patient's face and measuring the length of the airway from the corner of the mouth to the tip of the earlobe, • Center of the mouth to the angle of the mandible.
INSERTION • Choose the appropriate size • Open the airway • Insert the airway: 1. Using a tongue blade. Preferred method in children. 2. Insert upside down and rotate into place. Not to be used in children.
COMPLICATIONS • With intact gag reflex could cause vomiting. • Laryngospasm • Inappropriate size: 1. To Long: may push the epiglottis closed over the glottic opening, causing complete airway obstruction 2. To Short: May be easily displaced, distal opening may become obstructed by tongue
COMPLICATIONS • May occur from insertion. Improperly placed may push the tongue back into the pharynx and cause obstruction. • Aggressive insertion may cause trauma to the upper airway and bleeding. • The lumen of the tube is not large enough to allow for suctioning. Suctioning must be performed around the tube.
NASOPHARYNGEAL AIRWAYNP AIRWAY A curved hollow tube constructed of soft plastic or rubber with a bevel at the distal end and a flange or flare at the proximal end. This airway is less likely to stimulate gagging and vomiting because the the pliable tube moves and flexes as the patient swallows.
NP AIRWAY It may be used in a patient who is breathing but needs assistance in maintaining a patent airway. 15cm in length. The distal tip sits at the posterior pharynx while the proximal flare is seated on the external nare.
NP AIRWAY • Still requires manual airway maneuvers be maintained during its use.
NP AIRWAY • Indications: 1. When OP is not able to be inserted 2. Airway of choice in spontaneously breathing, but less responsive patient needing airway control. • Sizing 1. Proximal end of the tube at the tip of the nose and the distal end at the earlobe
NP AIRWAY • Technique of Insertion * Needs to be lubricated. * Proper size * Advance with bevel toward the septum * If patient is breathing you should feel airflow when placed properly. * If you meet resistance, remove and use other nare.
NP AIRWAY • Complications * Improper size and too long could end up in the esophagus * Too short could be occluded by the tongue * Laryngospasm * Trauma
ESOPHAGEAL OBTURATOR AIRWAY (EOA) • Was widely used, but due to complications and ET training its use has dropped. • Recommended in situations when airway control was necessary and not able to intubate. • Comprised of a mask and a cuffed esophageal tube with a sealed distal end. • 16 air holes allow for ventilation.
EOA • Inflation port to inflate the cuff with a syringe and a pilot balloon to indicate the cuff volume. • Placed in the esophagus, to seal and not allow air entry into the esophagus • During ventilation, the air is forced through the mask and out of the openings in the proximal end. Air is facilitated in to the glottic opening and hence the trachea.