Acute Joint Dislocation
Acute Joint Dislocation. Dr. Abdulrahman Algarni , MD, SSC (Ortho), ABOS Assist. Professor, King Saud University Consultant Orthopedic and Arthroplasty Surgeon. objectives. To know mechanisms of the most common joint dislocations Be able to make the diagnosis

Acute Joint Dislocation
E N D
Presentation Transcript
Acute Joint Dislocation Dr. AbdulrahmanAlgarni, MD, SSC (Ortho), ABOS Assist. Professor, King Saud University Consultant Orthopedic and Arthroplasty Surgeon
objectives • To know mechanisms of the most common joint dislocations • Be able to make the diagnosis • To know and interpret the appropriate x-rays • To know the common complications and how to avoid them
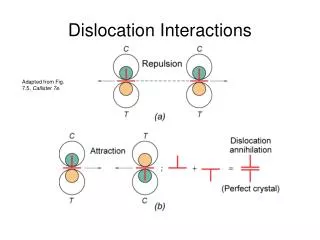
Acute Joint Dislocation • Complete separation of the articularsurface: Joint surfaces are no longer in contact • Position of distal to proximal fragment: Anterior, Posterior, Inferior, Superior
Acute Joint Dislocation • Usually results from high-energy trauma • They occur most frequently in young patients
Clinical Features • Painful; inability to move the limb • Abnormal shape of the joint • The limb is often held in a characteristic position • Careful NV exam before reduction is attempted.
Imaging X-rays • adequate views • Confirm the diagnosis • Rule out fractures i.e. a fracture-dislocation • Reduce before X-rays: knee, ankle • CT scan
Treatment • Urgent reduction: Closed; surgical if failed • Adequate pain relief; muscle relaxant; GA • Imaging after reduction: Post-reduction films • Immobilization • physiotherapy
Complications • Neurovascular injury: Knee, ankle • Avascular necrosis of bone • Recurrent dislocation: shoulder • Heterotopic ossification • Joint stiffness • Secondary osteoarthritis
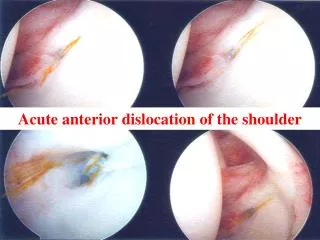
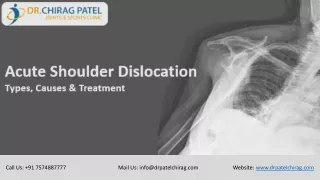
ACUTE SHOULDER DISLOCATION • The most commonly dislocating joint • shallowness of the glenoid socket and wide extraordinary range of motion
ACUTE SHOULDER DISLOCATION • Anterior dislocation is the most common • Posterior dislocation is rare; less than 2%
ANTERIOR SHOULDER DISLOCATION • Fall on the outstretched hand (abduction & external rotation)
ANTERIOR SHOULDER DISLOCATION • The lateral outline of the shoulder may be flattened • Bulge may be felt just below the clavicle
ANTERIOR SHOULDER DISLOCATION • X-rays: antero-posterior and lateral (axillary) views: • Overlapping shadows of the humeral head and glenoidfossa
ANTERIOR SHOULDER DISLOCATION • The head usually lying below and medial to the socket • Rule out greater tubrosity fracture
ANTERIOR SHOULDER DISLOCATION • Avulsion of the antero-inferior glenoid labrum (Bankart lesion). • Indentation of the postero-lateral part of the humeral head (Hill–Sachs lesion)
ANTERIOR SHOULDER DISLOCATION Reduction • Different techniques: Kocher’s, Stimson’s, Milch’s, Hippocratic
ANTERIOR SHOULDER DISLOCATION Reduction • Kocher’s method
ANTERIOR SHOULDER DISLOCATION Complications • Recurrent dislocation: age at first dislocation • Rotator cuff tear: elderly • Axillary nerve injury; neuropraxia • Axillary artery injury • Shoulder stiffness: prolonged immobilization • Unreduced (undiagnosed) dislocation
POSTERIOR SHOULDER DISLOCATION • Indirect force producing marked internal rotation and adduction • Convulsion, or with an electric shock
POSTERIOR SHOULDER DISLOCATION • The diagnosis is frequently missed; more than 50% • The arm is held in internal rotation and is locked in that position • The front of the shoulder looks flat with a prominent coracoid
POSTERIOR SHOULDER DISLOCATION Imaging • The humeral head is medially rotated (electric light bulb) • (The empty glenoid sign) • Axillaryor Scapular view is essential • Rule out fractures; neck, glenoid or lesser tuberosity • CT
HIP DISLOCATION • High energy trauma • posterior (the commonest) • anterior
POSTERIOR HIP DISLOCATION • Road Traffic accident; knee striking against the dashboard • Limb is short, adducted, internally rotated and slightly flexed.
POSTERIOR HIP DISLOCATION • Rule out associated fractures; femur or acetabulum • Rule out sciatic nerve injury
POSTERIOR HIP DISLOCATION • Reduction
POSTERIOR HIP DISLOCATION • Reduction
POSTERIOR HIP DISLOCATION • Reduction; stable • CT scan: the best to demonstrate an acetabular fracture (or any bony fragment)
POSTERIOR HIP DISLOCATION • Sciatic nerve injury; 10% • Avascular necrosis of the femoral head ;10% • If reduction is delayed by more than 12 hours, it rises to over 40% • Hetrotopic ossification
ANTERIOR HIP DISLOCATION • Rare compared with posterior • The leg lies externally rotated, abducted and slightly flexed • Palpable head in the groin
KNEE DISLOCATION • High energy mechanism; RTA • The cruciate ligaments and one or both lateral ligaments are torn
KNEE DISLOCATION • If dislocated joint has reduced spontaneously; swelling and gross instability
KNEE DISLOCATION • If still dislocated; gross deformity
KNEE DISLOCATION • Repeated vascular examination is necessary; popliteal artery injury; risk compartment syndrome • Common peroneal nerve injury: 20 % of cases
KNEE DISLOCATION • X-ray: dislocation, fracture of the tibial spine (cruciate ligament avulsion), avulsion of the fibular styloid (collateral ligament avulsion)
KNEE DISLOCATION • Angiograpy
KNEE DISLOCATION • Urgent reduction • Immediate vascular intervention if needed • Acute or delayed reconstruction of the ligaments
KNEE DISLOCATION Complications • Instability • Stiffness
Summary • Dislocation is an orthopedic emergency and need urgent reduction • Anterior shoulder dislocation is the commonest • Obtain adequate imaging to rule out posterior shoulder dislocation • Acute unstable knee is a knee dislocation until proven otherwise • Always suspect vascular injuries with dislocated knee