Vascular Access
Vascular Access. A 2-month-old girl arrives at the Emergency Department in cardiac arrest. Other providers promptly begin ventilation and perform chest compression. You need to establish vascular access to administer fluids and medications.

Vascular Access
E N D
Presentation Transcript
A 2-month-old girl arrives at the Emergency Department in cardiac arrest. Other providers promptly begin ventilation and perform chest compression. You need to establish vascular access to administer fluids and medications
What is the optimal site for immediate vascular access for this infant? • If resuscitative efforts are successful, what is the optimal site for vascular access during the post resuscitation period?
Objectives • Prioritize sites of vascular access for different clinical circumstances • Describe the risks and benefits of peripheral venous, central venous, and intraosseous vascular access • Describe the IO access technique
Selection of site and priorities of vascular access 1 For CPR and treatment of decompensated shock the one that is • most readily accessible • not require interruption
Selection of site and priorities of vascular access 2 • Compensated shock… large bore peripheral IV catheter • Post resuscitation phase… central venous catheter • Intracardiac administration of drugs during closed chest compression • Arterial cannulation
Priorities of Vascular Access • During pediatric CPR or treatment of decompensated shock.. IO access • One practical approach: IO or peripheral or central access simultaneously • During attempted resuscitation.. Transtracheal …LEAN
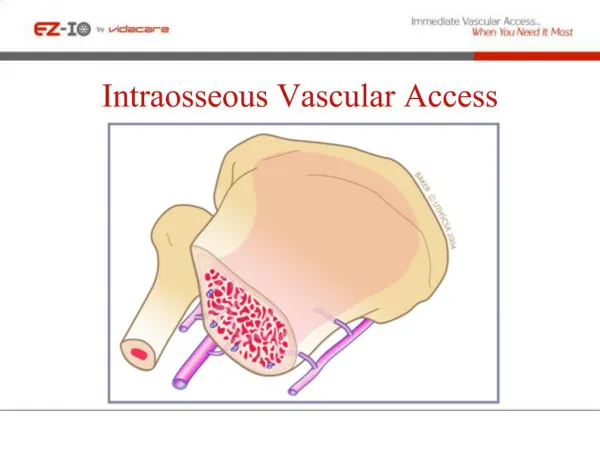
Intraosseous Access • Provides access to a noncollapsible marrow venous plexus which serves as a rapid , safe and reliable route of administration • Often can be achieved in 30-60 seconds by using a rigid needle(specially designed or Jamshidi-type)
A rapid, safe, & effective route for the administration of medications & fluids, & may be used for obtaining an initial blood sample for type & crossmatch & for chemical & blood gas analysis even during resuscitation (Class IIa; LOE 3). Acid-base analysis is inaccurate after sodium bicarbonate administration via the IO cannula. Intraosseous Access
Intraosseous Access • Epinephrine, adenosine, fluids, blood products, & catecholamines can safely be administered. • Onset of action & drug levels achieved are comparable to venous administration. • Use manual pressure or an infusion pump to administer viscous drugs or rapid fluid boluses, & follow each medication with a saline flush to promote entry into the central circulation.
Complications • Complications reported in fewer than 1% • Fracture of Tibia • Lower extremity compartment syndrome • Osteomyelitis • Extravasation of Drugs
Central V/S Peripheral Venous Access • More secure long-term access • Not higher drug levels or a substantially more rapid response • Administration of drugs could injure tissues(vasopressors ,calcium ,sodium bicarbonate)
Complications of central venous cannulation • Local and systemic infection,venous or arterial bleeding, arterial cannulation, Thrombosis,plebitis, pulmonary thromboembolism,hydro pneumo hemo chylo thorax, cardiac tamponade, arrhythmias, air embolism, catheter fragment embolism
Peripheral Venous Access Devices • Over-the-needle catheters • Catheter-over-wire devices • Catheter-through-introducing sheath devices • Butterfly needles
Peripheral Venous Access A tourniquet is placed around the infant's head & the needle inserted 0.5 cm from the intended puncture site in the direction of blood flow.
Mini-cutdown • The vessel is elevated with a hemostat & occluded with gentle traction from a distal tie. • The needle is inserted & the sheath is advanced into the vessel. • The vessel should not be tied off with this technique.
Summary points • Intravascular or intraosseous access is the preferred route for medication and drug delivery in cardiopulmonary emergencies.
2 • Immediate intraosseous access is recommended in cases of decompensated shock and cardiopulmonary arrest, particularly if the provider lacks experience in pediatric central venous access techniques
3 • Central venous catheterization can be used in children in emergencies. But it requires significant expertise. Many complications and delays may occur in expert hands