Rising Community-Onset Clostridium difficile Infections: Patterns and Impacts
This study examines the alarming rise in community-onset Clostridium difficile infection (CDI) rates, highlighting its escalation from mid-1990s to recent years. While traditionally viewed as a nosocomial infection, CDI's prevalence in the community has been increasingly recognized, with a significant portion of cases showing no prior hospitalization or antibiotic use. Using data from the Nationwide Emergency Department Sample, we analyzed incidence, mortality, hospital charges, and length of stay associated with community-onset CDI, emphasizing the need for broader awareness and updated treatment protocols.

Rising Community-Onset Clostridium difficile Infections: Patterns and Impacts
E N D
Presentation Transcript
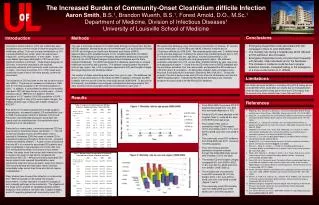
The Increased Burden of Community-Onset Clostridium difficile Infection Aaron Smith, B.S.1, Brandon Wuerth, B.S.1, Forest Arnold, D.O., M.Sc.1Department of Medicine, Division of Infectious Diseases1University of Louisville School of Medicine Conclusions Introduction Methods Clostridium difficile infection (CDI) has traditionally been recognized as a common cause of diarrhea acquired in the healthcare setting. The more severe manifestation of CDI is pseudomembranous colitis, which can lead to toxic megacolon, colonic perforation, or even death. In fact, more deaths have been attributed to CDI than all other intestinal infections combined.1 Three broad categories of CDI exist, nosocomial (acquired in the hospital), community-acquired, and community-onset (unknown site of origin).One study found that 41% of CDI cases were community-onset of which half were actually community-associated.2 The incidence of CDI has been on the rise since the mid to late 1990’s.3 There was an increase in incidence in 1996 from 31/100,000 population to 61/100,000 population in 2003.3 In addition, a concomitant increase in the mortality rate due to CDI has been shown in recent years.1 A study showed a rise in 1999 from 5.7 deaths/1,000,000 population to 23.7 deaths/1,000,000 population in 2004.1 Regarding length of stay (LOS) and hospital charges, the median duration was 10 days with median charges of $32,597.4 Risk factors for hospital-acquired CDI include inpatient hospitalization, increased hospital LOS and antibiotic use.5 In 2008, the European Centre for Disease Control and Prevention recommended physicians avoid high-risk agents such as cephalosporins, fluoroquinolones and clindamycin in at-risk patients.6 Particularly in recent years, community-acquired CDI has been shown to lack these classic risk factors.2,7-9 The US Centers for Disease Control and Prevention (CDC) reported in December 2005 two cases of severe CDI in populations previously thought to be at low risk – pregnant women and healthy children.10 A case-control study found that only 45% of community-associated CDI patients had been hospitalized in the preceding six months with only 52% having antimicrobials in the previous four weeks.8 Further, the study found that contact with infants less than or equal to two years of age had an increased risk association with CDI.8 Among community-associated CDI cases, patients who required hospitalization were significantly older (64 versus 44 years), were more likely to have severe disease and had higher mean Charlson comorbidity index scores than those who did not require hospitalization.11 Many studies have focused their attention on nosocomial CDI. With the spread of CDI outside the hospital environment, it is also important to track the changes of such a deadly pathogen in the community. The objective of this study was to provide an updated population based analysis of the incidence, mortality rate, hospital charges, and LOS regarding patients with community-onset CDI. This was a secondary analysis of the Nationwide Emergency Department Sample (NEDS) database, developed as part of the Healthcare Cost and Utilization Project (HCUP) by the Agency for Healthcare Research and Quality (AHRQ). Approximating a 20% stratified sample of U.S. hospital-based EDs, the NEDS database is the largest all-payer emergency department database constructed from both the HCUP State Emergency Department Database and the State Inpatient Databases. The AHRQ developed this database specifically to analyze healthcare economics and outcomes. The dataset contains patient information such as age, region, sex, LOS, emergency department (ED) and hospital charges, discharge diagnosis and discharge status.12 The number of states submitting data varies from year to year. The database has grown, incorporating data from 24 states and 950 hospitals to 29 states and 964 hospitals over the course of the four year study period; 2006-2009. To account for this disparity, the database has assigned, individualized discharge weights that were used to produce population level event estimates for each year.12 We queried the database using International Classification of Disease, 9th revision, clinical modification (ICD-9-CM) code 008.45 (intestinal infection due to Clostridium difficile) for 2006-2009. We obtained patient data with C. difficile listed as the principle diagnosis, indicating the patient was admitted primarily due to CDI. The data was stratified by sex, age group, hospital characteristics, LOS, hospitalization costs, mortality rate, and geographical region. We obtained population estimates from U.S. census data, stratified similarly by year, age group and geographical region.13 Using the total ED visits from the NEDS database and the population estimates from the census data, we tabulated the ED incidence of CDI within the U.S. population. All descriptive statistics were completed using Microsoft Excel (Microsoft Corporation, Redmond, WA, USA 2011). During the analysis, the unit of analysis was each ED visit while the stratification unit was the NEDS hospital stratum. Institutional Review Board exemption was obtained because this study used a de-identified public database. • Emergency Department visits associated with CDI increased in the U.S. from 2006-2009. • The mortality rate during a hospital stay which followed an ED admission also increased. • Emergency Department visits occurred more frequently with females, older individuals and in the Northeast. • The increase in incidence could be due to greater detection methods, increased testing or the emergence of a more virulent strain of C. difficile. Limitations Our study had some limitations, including using ICD-9 coding as our case identifier which could alter our results due to misclassification. If we had false positive cases due to incorrect ICD-9 coding, then the severity may have actually been lower than we found. Results References • From 2006-2009, there were 372,237 patients discharged from U.S. EDs with a principle diagnosis of CDI. • A total of 92.4% were admitted to the hospital (Table 1), while 46.9% were in the 65-84 year age group. • The number of ED visits of community-onset CDI increased 19.5% from 2006 to 2007, 5.1% from 2007 to 2008, and 2.8% from 2008 to 2009. • The community-onset CDI incidence from 2006-2009 was 30.71 cases per 100,000 population. • The LOS following hospital admission remained constant through the 2006-2009 study period with a median LOS of five days. • The median ED and hospital charges increased 8.6% from 2006 to 2007, 11.9% from 2007 to 2008, and 2.4% from 2008 to 2009 (Table 2). • The mortality rate of community-onset CDI increased 34.1% from 2006 to 2007, 1.9% from 2007 to 2008, and 3.6% from 2008 to 2009 (Figure 1 and 2). • The community-onset CDI mortality rate from 2006-2009 was 10.96 deaths per 1,000,000 population. • Redelings, M.D., Sorvillo, F. & Mascola, L. Increase in Clostridium difficile-related mortality rates, United States, 1999-2004. Emerg Infect Dis13, 1417-1419 (2007). • Kutty, P.K., et al. Risk factors for and estimated incidence of community-associated Clostridium difficile infection, North Carolina, USA. Emerg Infect Dis16, 197-204 (2010). • McDonald, L.C., Owings, M. & Jernigan, D.B. Clostridium difficile infection in patients discharged from US short-stay hospitals, 1996-2003. Emerg Infect Dis12, 409-415 (2006). • Dubberke, E.R., Reske, K.A., Olsen, M.A., McDonald, L.C. & Fraser, V.J. Short- and long-term attributable costs of Clostridium difficile-associated disease in nonsurgical inpatients. Clin Infect Dis46, 497-504 (2008). • Freeman, J., et al. The changing epidemiology of Clostridium difficile infections. ClinMicrobiol Rev23, 529-549 (2010). • Vonberg, R.P., et al. Infection control measures to limit the spread of Clostridium difficile. ClinMicrobiol Infect14 Suppl 5, 2-20 (2008). • Benson, L., Song, X., Campos, J. & Singh, N. Changing epidemiology of Clostridium difficile-associated disease in children. Infect Control HospEpidemiol28, 1233-1235 (2007). • Wilcox, M.H., Mooney, L., Bendall, R., Settle, C.D. & Fawley, W.N. A case-control study of community-associated Clostridium difficile infection. J AntimicrobChemother62, 388-396 (2008). • Bauer, M.P., et al. Community-onset Clostridium difficile-associated diarrhoea not associated with antibiotic usage--two case reports with review of the changing epidemiology of Clostridium difficile-associated diarrhoea. The Netherlands journal of medicine66, 207-211 (2008). • Severe Clostridium difficile-associated disease in populations previously at low risk--four states, 2005. MMWR. Morbidity and mortality weekly report54, 1201-1205 (2005). • Khanna, S., Pardi, D.S., Aronson, S.L., Kammer, P.P. & Baddour, L.M. Outcomes in community-acquired Clostridium difficile infection. Alimentary pharmacology & therapeutics35, 613-618 (2012). • National Emergency Department Sample (NEDS) from the Agency for Healthcare Research and Quality. Healthcare Cost and Utilization Project Nationwide Emergency Department Sample. • U.S. Census Bureau. US Census 2000-2009. Available at: http://www.census.govAccessed November 18, 2010.