INTEGUMENTARY SYSTEM
A

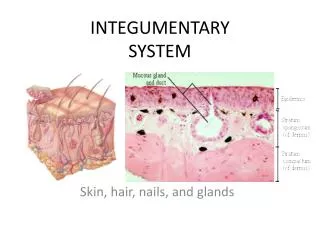
INTEGUMENTARY SYSTEM
E N D
Presentation Transcript
1. INTEGUMENTARY SYSTEM
3. Review cont�. Collagen
Protein that gives strength and resilience to skin
Loss of collagen results in wrinkles
Desquamation
Loss of skin
4. Dermatology-study of skin diseases
Dermatologist-physician who specializes in this field
See Box 74-1
Abrasion
Laceration
Purpura**
Discolored skin d/t blood in the tissue outside the blood
5. Dx Tests: Direct observation
Diagnostic tests can be used to determine the origin of the skin disorder
Wood�s light-use of UV rays to Dx pigment abnormalities, can also detect superficial fungal and bacterial infections
Tzanck�s smear-examination of cells and fluids found in vesicles (ex. Herpes zoster and Varicella), they are applied to a glass slide and examined using a microscope
6. Dx Tests: Biopsy-removal of skin-tissue specimen for microscopic exam to determine malignancy or to Dx a skin disorder
Scabies scraping-shave off the top of a suspected lesion, place on a glass slide covered with immersion oil and examine the slide under a microscope
7. Pruritis (Itching) Sx of skin disease
Can also be caused by systemic disorders, such as liver disease and dry skin
Scratching is inevitable, and causes skin breaks which can result in scarring and infections
Tx: divert attention, hypnosis
Administer medications: antianxiety (Ataraz, Vistaril), antihistamines (Benadryl, Tavist), topical corticosteroids
Prevention: Cotton clothing, apply lotion to dry skin, skin testing, cool or lukewarm baths, soothing baths (colloidal oatmeal, starch)
8. Therapeutic Bath Purposes:
*Cleanse body and soothe skin
*Promotes wound healing
*Relieves itching
Aids in the removal of eschar
Aids in prevention of infection
After the bath, you can apply medication to the body
Give this type of bath in a WP or bathtub, disinfect after each pt. Use
Oatmeal, cereals, starch, tars and baking soda can also be added to the bath
Don�t use soap (dries the skin), use medicated bath oil
**Tepid water (heat makes one itch)-no more than 100 degrees F
Pat the skin dry, rubbing increases pruritis
*Use lotion if the MD allows
9. Skin and Tissue Grafts Skin grafts are used to cover areas of skin lost from burns, infections or wounds
Graft-transplant of skin that is placed on viable tissue
-very painful -may take months to heal, depending on success
Free graft-skin completely removed from its original site and grafted on to the recipient site
Pedicle graft-one end of the graft remains attached to the donor site so that new circulation is established
Nursing Considerations:
Explain procedure
Can expect postop edema, ecchymosis
Protect sites, grafts
Provide emotional support
10. Moist Dressings Moist packs-reduce edema and weeping in acute dermatitis
-soften and remove exudate and crusts
Relieve pruritus and discomfort
-clean or sterile
-closed dressing-covered with plastic or a firm material
-open dressing-not covered, tissues need O2 to prevent necrosis
-requires frequent dressing changes or resoaking q2 hours
-Explain procedure
-Proper disposal
-DOCUMENT
-MD will order the type of dressing or medication to use
11. Wound Debridement Physician or Surgeon will remove loose skin, crusts, eschar or denuded (protective) tissue
Sterile procedure often done when changing moist packs (change moist packs q2hours!!)
12. Surgical Treatments Plastic or Reconstructive Surgery-improves disfigurement, may be performed for cosmetic effects, to repair congenital defects or repair trauma tissue
13. Skin and Tissue Grafts Assess the skin:
-report any changes
-color
-turgor
Document: size, color, texture, location or distinct characteristics of the skin
Fluid and Electrolyte Balance
Encourage the client to drink and eat
Provide high Kcal, high protein meals
Observe and document I & O
14. Acute and Chronic Skin Conditions Urticaria (hives)
S/S: edematous, raised pink areas called wheals
Wheals itch and burn
May disappear quickly or stay for days
Most commonly caused by an allergic reaction to meds, foods, spores or pollens
Chronic urticaria lasts longer than 6 weeks, cause is unknown in 80-90% of adults
**Angioedema-involves deeper dermal and Subq. Tissues. Affects the lips, eyelids, skin, GI tract, hands, feet, genitalia, tongue, and larynx
TX: removal of cause, tepid baths, antipruritic lotions, antihistamines, epinephrine for severe cases
15. Vitiligo Occurs when areas of skin lack in pigmentation
Results in patches of pale or white looking skin
Cause unknown
Tx: methoxsalen after exposure to sunlight can temporarily darken the affected area
Surgical tx: grafting and melanocyte transplantation
Melanin-gives skin color
Albinos cannot make melanin
Can also use cosmetics to cover birthmarks
17. Eczema (atopic dermatitis) Sx: small vesicles appear along with red and pruritic skin, when the vesicles burst and ooze, crusts form
Viral, bacterial or fungal skin infection may develop
Cause unknown but heredity, allergy, and emotional stress can contribute
Most commonly found in the folds of the elbow, back of the knees, on the face, neck, wrists, hands and feet
18. Eczema (atopic dermatitis) Tx: prevent dry skin, cracking and itching
Apply moisturizing creams, corticosteroid ointments, or wet dressings
Use lanolin free lotions
Meds: Topical corticosteriods-exert localized anti-inflammatory activity, reduce swelling, redness, itching, antihistamines-may relieve itching!
Potency depends on drug concentration and the vehicle (lotion, cream, etc.)
Adverse Reactions:
Burning, itching, irritation, redness, dryness of the skin, secondary infections
21. Psoriasis Chronic, noncontagious disorder that affects young adults and middle aged adults
Cause is unknown but hereditary, environmental, metabolic or immune factors contribute to breakouts
Stress and anxiety precede exacerbations of the disorder
22. Psoriasis S/S: red papules covered with silvery, yellow-white scales that the client sheds
Patches appear on the elbows, knees, scalp and lower back, the nails may loosen at the fingertips (onycholysis)
Tx: reduce scaling and itching
Therapeutic baths, wet dressings, or lubricating ointments
23. Psoriasis Meds:
Topical antipsoriatics-help remove the plaques associated with this disorder
Ex: calcipotriene (Dovonex)
Anthralin (Anthra-Derm)
Antihistamines
Methotrexate & oral retinoids are useful in treating severe, extensive psoriasis
Adverse Reactions:
Burning, itching and skin irritation
Anthralin may cause temporary discoloration of the hair and fingernails
25. Infections Warts (verrucae)
Small, flesh-colored, brown or yellow papules caused by HPV
Common warts-found on the hands (esp. children), or on other sites subjected to trauma
Filiform warts-slender, soft, thin, finger-like growths seen on the face and neck
Plantar/palmar warts-firm, elevated or flat lesions occurring on the soles or palms
Tx: electrodessication-short duration of high frequency electrical current or curettage-scraping or suctioning is the treatment for filiform warts
26. Warts
27. Warts Cryosurgery-application of liquid nitrogen
Keratolytic agents-removes excess growth of the epidermis. Used to remove warts, callusues, and corns
Ex. Salicylic acid, masoprocol (Actinex)
Adv. Rxns: burning sensation, rash, dry skin, scaling or flu-like syndrome
Contraindicated: for use on moles, birthmarks or warts with hair growing from them, genital or facial warts, warts on mucous membranes
Salicylate acid may cause salicylate toxicity
28. Wart Cryosurgery
29. Warts Condylomata acuminate-venereal warts
Grow in warm, moist body areas, skinfolds
Usually develop in clusters
Found on the foreskin and the penis or on vaginal and labial mocosa and the urethral meatus or perianal area
Spread by sexual contact
30. Veneral Warts
31. Bacterial skin infections Impetigo-contagious among infants and young children
Caused by strept or staph
Vesicles ooze a clear exudates that develops into golden-yellow crust that causes discomfort and pruritis
Tx: systemic antibiotics
Good handwashing
Bacteria transfers from infected client to another person through touch**
Meds: mupirocin (Bactroban)
Adv. Rxns: burning, stinging, pain, itching, rash, nausea, dry skin
33. Impetigo
34. Bacterial skin infections Folliculitis-white pustules or follicular nodules
A staph infection starting around the hair follicle
Moisture, trauma and poor hygiene can contribute
Deep folliculitis-on face
Superficial folliculitis-responds to antibacterial soap cleansing or topical antibiotics
Furuncle (boil) �firm, red, tender nodule
May drain pus and finally extrude the core
Core is dead tissue that can drain by itself or be reabsorbed into the skin
Can also be I & D
35. Folliculitis
36. Bacterial skin infections Found in areas of hair-bearing skin, esp. the face, scalp, buttocks and axillae
Furunculosis-recurrent boils on people who have the staph organism
Carbuncle-interconnecting boils in a cluster
Drains at multiple sites
Mostly located on the back of the neck, the back and the thighs
Tx: warm, wt dressings or soaks to localize the boil and carbuncle infections to one spot
I & D large boils
Oral antibiotics after a sensitivity test
37. Furuncle
38. Parasitic Infections Scabies (mites that burrow under the outer layer of the host�s skin)-intense itching, red spots appear with rows of blackish dots with tiny vesicles and depressions
Mostly found between the fingers
Mites can live for months or years in people if left untreated
Infection can be transmitted through clothing, linens, or towels
Meds:
5% permethrin cream (Elimite)
lindane (Kwell)
Leave medication on for 8-24 hours and then bathe thoroughly, repeat tx. In one week
39. Scabies
40. Scabies
41. Lice-Pediculosis Pediculosis humanus capitis head lice
Pediculosis humanus corporis-body lice
Phthirus pubis, pediculosis pubis-pubic lice
Survival depends on sucking blood
Difficult to get rid of
Nits (eggs) can live for a long time on clothes, bedding, furniture
S/S: presence of nits, extreme pruritis
Tx: permethrin (Elimite, Nix) and pyrethrings (RID), apply to hair for 5-10 minutes, rinse with water. Remove the nits by combing the hair with a fine-toothed comb, apply petroleum to the eyelashes and eyebrows to remove nits
ALL LIVE LICE AND NITS MUST BE DESTROYED TO PREVENT RE-INFESTATION!!
42. Lice-Pediculosis Bedbugs-Cimex lectularius
4-5 millimeters and can survive up to 1 year without food
Live in clothing or bedding and are difficult to get rid of
Bites appear as red macules that develop into nodules
Bites often appear in groups of three, and bite the legs and feet resulting in itching and burning
Tx: lotions containing menthol, phenol, or 0.5% hydrocortisione cream
Spray all crevices in furniture with an insecticide
43. Sebaceous Gland Disorders Sebaceous Cysts-secrete oil and when plugged with oil, small nodules form called cysts
Usually not treated unless they become large and then they are I & D
Seborrhea, Seborrheic Dermatitis and Dandruff
Seborrhea-sebaceous discharge that forms large scales or cheeselike plugs on the body
*Seborrheic dermatitis causes scaling, primarily of the scalp that itches, erupts where there is a large concentration of sebacous glands-scalp, eyebrows, eyelashes
Dandruff-dry form of seborrheic dermatitis
Scales range from small and dry to thick and powdery
Oily form of seborrheic dermatitis is characterized by greasy or oily scales and crusts on a red base
Tx: Shampoo frequently with selenium sulfide suspension (Selsun Blue) and leave on for 5-10 minutes, coal tar**
If lotions or solutions contain steroids, use sparingly
44. Burns Result in tissue loss or damage and are traumatic
45. Classification: Thermal-most common, caused by steam, hot water, flames and direct contact with heat sources.
Electrical � Caused by electric shocks due to exposure to lightning or electricity
Chemical � caused by exposure to acids, alkalis or other organic substances.
Radiation � exposure to the radiation, sun
46. Burns Severity of injury is related to the burn�s depth, extent, location and length of exposure
Inhalation injuries occur in closed areas with fire and smoke
s/s: singed nasal hairs, facial burns, and soot � stained sputum
47. Burn depth and size Partial-thickness-superficial, moderate and deep-dermal burns
1st degree and 2nd degree
Full thickness (3rd degree)-includes all the characteristics of 1st and 2nd degree burns along with subq. Fat, connective tissue, muscle and even bone.
See table 74-2 in book
48. �Rule of Nine� Used in determining% of body burned
Adults:
Head=9%
Each arm = 9%, front 4.5%; back 4.5%
Each leg = 18%
Front or back = 18%
Genitals = 1%
See page 1104 for child �Rule of Nines� classification
Phases of Burn Injury Management
Immediately � apply cold packs or cold water
49. Resuscitative phase: Initial hours after burn, stabilize immediate health concerns!!
Burn care unit
Always wash hands, use sterile gloves
V/S
NEVER apply ointments to an extensive burn!!!!
Monitor respiratory status-rate and depth of repirations
Suspect inhalation injury if client was in a closed in area with fire and smoke
Report cough immediately!! Note amount and character of sputum-black/gray indicates smoke inhalation
May need O2, keep an ET tube or trach tube at bedside
Prevent pneumonia
50. Fluid and Electrolyte Balance: Lose body fluids from capillary leaks and open wounds, require large amounts of IV fluids particularly containing sodium
Record I&O
Assess electrolytes: potassium, sodium
51. Renal Function: Monitor urine output hourly, decrease could show shock
If u/o is less than 30mls/hr. dialysis may be needed.
52. Infection: Leading cause of death for burn clients
May be placed in protective isolation to prevent exposure to pathogens
53. Pain Management Assess pain level, location
Superficial burns have more pain that full-thickness burns because the nerve endings have been destroyed
PCA may be used
Morphine � Monitor RR!!
Imagery, distraction may also be used
Some cultures may not use drugs to relieve pain
54. Acute Phase: Client remains ill and requires continuous assessment, focus on the burn wound Dressings such as OpSite, DuoDerm (synthetic) promote healing and cover the wound
Impregnated antibiotic gauze may also be used
Wounds heal better when moist
55. Acute Phase: Tight occlusive dressings may be used as they prevent keloid (scar) tissue
Tropical agents:
Mafenide Acetate (Sulfamylon)
Silver sulfadiazine (Sivadene)
Bacitracin ointment
Used for superficial and facial burns applied as a thin layer 2-3 times/day
Silver Nitrate
56. Acute Phase: Topical proteolytics (enzymes) may be used to remove dead tissue
Debridement-removing eschar, exposing living tissue
WP is used, more comfortable
MD�s can use laser scalpels or scalpels to excise eschar
57. Acute Phase: Enzymatic Debridement using a proteolytics substance digests necrotic tissue
58. Burns Skin grafting-replaces tissue that does not heal or can be used for cosmetic reasons
Autograft-uses the client�s own skin, MD cuts slices of skin from an unaffected part of the client�s body and places these graft on the affected areas
Homograft/Allograft � cadaver skin
Take immunosuppressive meds to prevent rejection
59. Burns Heterograft/Xenograft � using pigskin
**The client�s body will reject in 1 week but the pigskin will aid the body in fluid retention, promote healing and prevent infection
CEA � cultured epithelial autografts
Biopsy is performed on unburned skin and grows new skin, used to cover extensive burns.
60. Grafts DO NOT DISTURB SKIN GRAFTS!
They need to attach to the live tissue underneath and grow
61. Other Considerations Diet high in calories, nitrogen, and protein
Monitor wound drainage
Administer LR (per MD order)
STRICT I & O
62. Rehabilitative Phase Lasts months to years
May need PT Service for WP tx�s
Financial assistance
Complications:
anemia
Infections, GI disturbances, pneumonia, kidney failure, anemia, skin ulcers, contractures (ROM)
Escharotomy may need to be performed to relieve tension on skin.
63. Rehabilitative Phase Curling�s ulcers-may develop 1 week after the injury causing a GI bleed
Occurs when gastric mucosa becomes ischemic, excess hydrogen ions, inadequate mucosal cell proliferation
Monitor GI pH, internal feedings, medications that reduce stomach acid
Provide emotional support
Teach: wound care, meds, s/s infection
Neoplasms: New growths, tumors
Malignant
Benign
64. NEOPLASMS Nonmalignant tumors are warts, angiomas, keloids, cysts and nevi (moles)
Moles may become malignant
Angiomas can be difficult to remove, or they may often go unnoticed.
Birthmarks or vascular skin tumors involving underlying tissues and blood vessels
Port-wine angioma-difficult to remove
Most angiomas are not noticeable or dangerous
Keloids � benign overgrowths that develop at scar sites
65. Skin Cancer Most common
Most curable
Caused by sun exposure
Light skinned, light-eyed people or those that burn vs. tan are at the highest risk
A deeply pigmented mole should be checked
American Cancer Society rules for mole evaluation:
Asymmetry
Border
Color
Diameter
66. Skin Cancer Tx: curettage, electrodessication, cryosurgery, or wide excision
Pathologist examines the tissue
Basal cell carcinoma-small, fleshy bump or nodule
Found in UV exposed tissues, head and neck
Most common type
67. Skin Cancer Basal cell carcinoma
Found in areas exposed to sunlight or UV light
Most common form of skin cancer
68. Skin Cancer Squamous cell carcinoma � appears as a nodule or red, scaly patch
Found on rim of ear, face, lips, or mouth
May metastasize, increases in size and develops into large mass
95% cure rate with surgery!
Malignant melanoma � darkly pigmented mole or skin tumor
Most virulent of all skin cancers
May metastasize to the skin, bone, brain, and lung
69. Topical Drugs Antiviral
Acyclovir
Antiseptic and Germicides (kill bacteria)
Chlorhexidine
Povidone-iodine
Corticosteroids (apply sparingly) exert localized anti-inflammatory activity
Amcinonide
Betamethasone
dexamethasone
70. Topical Drugs Anti-psoriatic
calcipotriene
Selenium sulfide
Collagenase
Keratolytic (removes excess growth of the epidermis)
Diclofenac
Salicyclic acid
Local anesthetics
Benzocaine
lidocaine
71. Nursing Process: Implementation
Topical Anti-infectives-clean area with soap and warm water prior to applying medicine
Topical corticosteroids-applied sparingly, clean area prior to applying
Topical enzymes
Topical antipsoriatics - apply only to the psoriatic lesions
Topical anesthetics � when using lidocaine viscous for oral anesthesia for pain control, instruct client not to eat food for 1 hour after use, anesthetic may impair swallowing
72. Nursing Process: Education patient and family
Keep topical meds away from the eyes (unless ordered by PCP)
If product is accidentally spilled or sprayed in the eyes, wash the eyes with copious amounts of water.
73. Shingles Herpes Zoster
Incubation period is 14-21 days
Rash appears on the face and trunk and then develops into blisters surrounded by a red ring