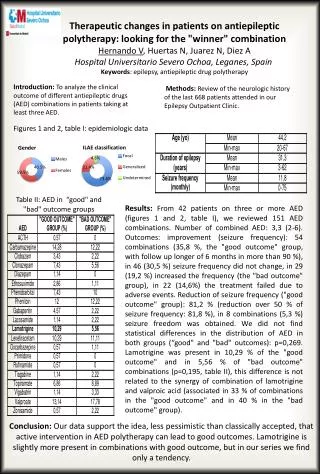
Figures 1 and 2, table I: epidemiologic data
20 likes | 173 Views
Therapeutic changes in patients on antiepileptic polytherapy : looking for the "winner" combination Hernando V , Huertas N, Juarez N, Diez A Hospital Universitario Severo Ochoa, Leganes, Spain Keywords : epilepsy, antiepileptic drug polytherapy.

Figures 1 and 2, table I: epidemiologic data
E N D
Presentation Transcript
Therapeutic changes in patients on antiepileptic polytherapy: looking for the "winner" combinationHernando V, Huertas N, Juarez N, Diez A Hospital UniversitarioSevero Ochoa, Leganes, SpainKeywords: epilepsy, antiepileptic drug polytherapy Methods: Review of the neurologic history of the last 668 patients attended in our Epilepsy Outpatient Clinic. Introduction: To analyze the clinical outcome of different antiepileptic drugs (AED) combinations in patients taking at least three AED. Conclusion: Our data support the idea, less pessimistic than classically accepted, that active intervention in AED polytherapy can lead to good outcomes. Lamotrigine is slightly more present in combinations with good outcome, but in our series we find only a tendency. Figures 1 and 2, tableI: epidemiologic data Table II: AED in “good" and "bad" outcome groups Results:From 42 patients on three or more AED (figures 1 and 2, table I), we reviewed 151 AED combinations. Number of combined AED: 3,3 (2-6). Outcomes: improvement (seizure frequency): 54 combinations (35,8 %, the "good outcome" group, with follow up longer of 6 months in more than 90 %), in 46 (30,5 %) seizure frequency did not change, in 29 (19,2 %) increased the frequency (the "bad outcome" group), in 22 (14,6%) the treatment failed due to adverse events. Reduction of seizure frequency ("good outcome" group): 81,2 % (reduction over 50 % of seizure frequency: 81,8 %), in 8 combinations (5,3 %) seizure freedom was obtained. We did not find statistical differences in the distribution of AED in both groups (“good" and "bad" outcomes): p=0,269. Lamotrigine was present in 10,29 % of the "good outcome" and in 5,56 % of "bad outcome" combinations (p=0,195, table II), this difference is not related to the synergy of combination of lamotrigine and valproic acid (associated in 33 % of combinations in the "good outcome" and in 40 % in the "bad outcome" group).
Instructionsfor poster presentations • Thedimensions of the poster boards are 90 cm wide x 120 cm high. Material formounting posters will be provided in the poster area. • Pleasenote thefollowinginformationregardingyourpresentation: • Thedimensions of the poster board are 90 cm wide x 120 cm high (viewsamplebelow). • Allocatethe top of the poster forthetitle and authors as statedonthesubmittedabstract. • Thetext and illustrationsshould be boldenoughtoreadfrom a distance of twometers (sixfeet). • Tacks and technicalequipmentwill be availableforthehanging of posters. • PleaserefertotheCongress Final Programmeforthe poster numberassignedtoyou, as well as your date of presentation. Please use theboardwiththesamenumber.