BIOPSY
520 likes | 1.07k Views
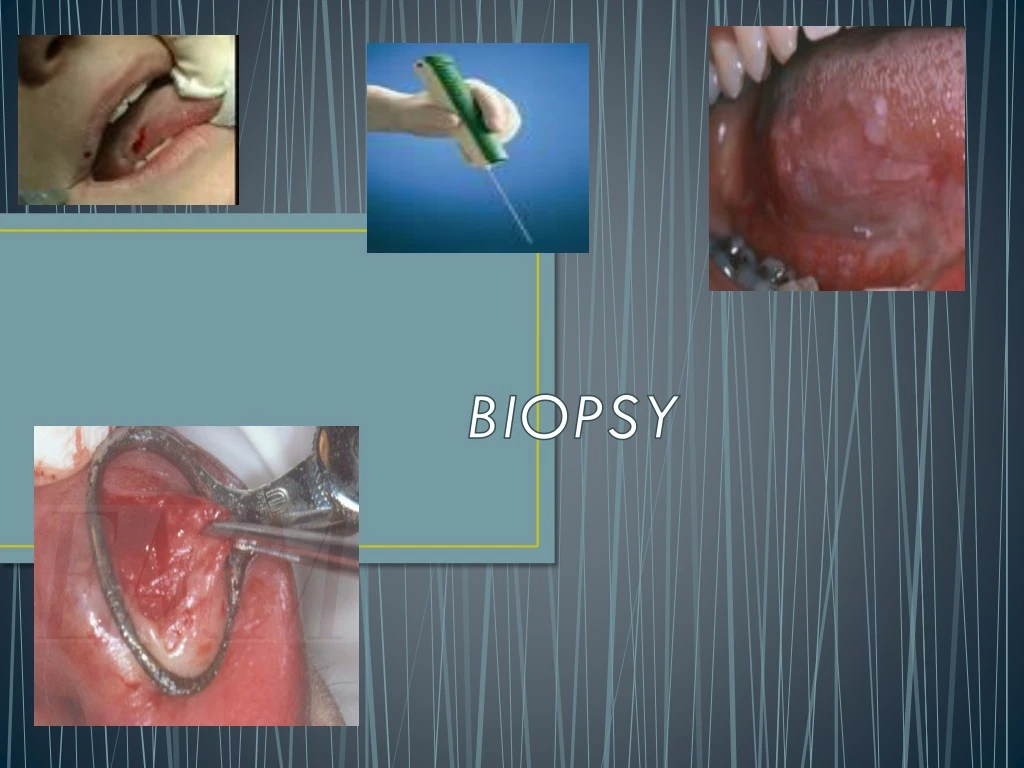
BIOPSY. DEFINITION. “Biopsy is the removal of tissue from living organism for the purpose of microscopic examination and diagnosis” Oral pathology- Shafer 4 th edition. TYPES OF BIOPSY. EXFOLATIVE CYTOLOGY ORAL BRUSH BIOPSY EXCISIONAL BIOPSY INCISIONAL BIOPSY

BIOPSY
E N D
Presentation Transcript
DEFINITION “Biopsy is the removal of tissue from living organism for the purpose of microscopic examination and diagnosis” Oral pathology- Shafer 4th edition
TYPES OF BIOPSY • EXFOLATIVE CYTOLOGY • ORAL BRUSH BIOPSY • EXCISIONAL BIOPSY • INCISIONAL BIOPSY • PUNCH BIOPSY • CORE BIOPSY • BONE BIOPSY
ARMAMENTARIUM FOR BIOPSY INSTRUMENTS FOR SOFT TISSUE BIOPSY: • Local anesthetic equipment • Scalpel (No. 15 blade) • Scissors • Needle holder, suture etc. • Biopsy bottle; 10% formalin • Biopsy data sheet • Fine tissue forceps • Small hemostat • Gauze sponges (suction if necessary)
Additional instruments for hard tissue biopsy or biopsy of soft tissue within bone: • Periosteal elevator • Rongeur • Bur and rotary handpiece • Sterile saline solution • Curettes
INSTRUMENTS FOR ASPIRATION BIOPSY: • 5 or 10 ml syringes • 18-gauge needle for fine needle aspiration biopsy • 23-guage needle for fine needle aspiration cytology
INDICATIONS • Any inflammatory lesion that does not respond to local treatment after 10 to 14 days (i.e., after removing local irritant) • Persistent hyperkeratotic tissues • Lesions that interfere with local function (eg. Fibroma). • Bone lesions not specifically identified by clinical and radiographic findings. • Any lesions that has the characteristic of malignancy (eg. Erythroplakia)
RELATIVE CONTRAINDICATION • This should include inflammatory lesions of allergic, viral, fungal or bacteria etiology. • Normal and racial variations such as those seen physiologic pigmentation, leukedema, linea alba, tori, exostoses etc.
ABSOLUTE CONTRAINDICATION • Pulsatile lesions or those suggestive of a vascular nature • Intrabony radiolucent lesions • Lesions that are clinically, obviously malignant should be biopsied . • Biopsy irritative/traumatic lesions
OBJECTIVES The aim of the biopsy is to: • Define a lesion on the basis of its Histopathological aspect • To establish a prognosis in malignant or premalignant lesions; • Facilitate Specific treatment • Act as a document with medical-legal value
EXFOLATIVE CYTOLOGY • Exfoliative cytology is the histopathologic examination of cells that have been obtained by their physical removal, followed by their placement on a glass slide. • Term pap smear is used. • The first modern use of cytology for head and neck cancers was in 1949
Technique • The supplies needed for oral cytology are: • 2 glass slides • 1 Cytobrush (if there is more than one lesion, then 1 Cytobrush per lesion) or a wooden or a metal spatula • Any cytology fixative - commonly used is 95% Ethanol; Commercial spray fixatives are also used .
Technique • Tongue blade is placed under tongue • Lesion is stroked gently but firmly with its tip of wooden blade • The exfoliated cells collected is harvested • You should be able to see a white filmy debris on the glass slide • Fixative spray • Repeat the procedure for the second smear on the same lesion.
Cytologicdiagnosis • A cytologic diagnosis is different with a surgical biopsy • Categorize lesions as normal, atypical intermediate ,suggestive or positive • Any lesions with either a suspicious or malignant cytologic diagnosis need to be followed with a biopsy of the site. • In the case of candidiasis, indicate fungal infection
ORAL BRUSH BIOPSY • A simple, rapid, and highly accurate method is currently available for the assessment of oral epithelial abnormalities, • which may include precancerous and cancerous lesions • Unlike cytology instruments, which collect only exfoliated superficial cells the biopsy brush penetrates to the basement membrane, removing tissue from all three epithelial layers . • Does not require topical or local anesthetic and causes minimal or no bleeding or pain.
Indications • Oral and oropharyngeal mucosal abnormalities • leukoplakia erythroplakia • Mixed red and white lesions • Speckled leukoplakia • Cancer or pre cancer • identifying unsuspected oral cancers at early and curable stages.
Procedure • In brush biopsy technique the use of a specially designed circular brush is used. • which is used to sample the epithelial lesion in question. • The brush may be moistened with water or the patient's saliva and applied to the surface of the lesion. • Contact between the brush and the mucosal surface may be along either the flat end or the rounded surface, • Moderate pressure applied
Procedure • The brush is then rotated until pinpoint bleeding is noted and enters into the lamina propria and, thus, obtaining epithelial cells through the full-thickness of the epithelium • Removed cells are transferred to a glass slide. • A fixation step follows immediately by flooding the slide with fixative solution (alcohol/propylene glycol) and allowing it to air dry.
Interpretation • classified as • negative -(ie, no epithelial abnormality) • Atypical -(i.e., abnormal epithelial cells, but of uncertain diagnostic significance), • Positive -(i.e., unequivocal).).
FINE NEEDLE ASPIRATION CYTOLOGY • “An aspiration cytology is the removal of contents of amass for the purpose of analysis” • This technique is usually used to rule out and or differentiate fluid filled lesions.
Removal a very small core of cells from a deep seated-lesions • Used for deep lesions which are not accessible indications • Suspected tumor of parotid gland • Enlarged lymhnodes in sub mandibular ,and submental region.
Advantages • Case performance • Cost • Effectiveness • Convenience • Accuracy
Indications • Cysts ,Abscess, Vascular lesions, Hematomas, Sialoceles, or Empty cavities (Traumatic bone cyst). • The aspiration cytology is applicable to both intraosseous as well as soft tissue masses. • All radiolucencies in the jaws
Procedure • Under local anesthesia, • 23-guage needle attached to a 10-cc disposable syringe • Negative pressure • The aspirate is expressed onto the glass slide. • A second slide is placed on the first and used to spread the aspirant. • One in 95% ethanol fixative other is air dried • Alcohol fixed- Papanicolaou’s stain • Air dried-wrights stain ( quick evaluation)
EXCISIONAL BIOPSY • “Excisional biopsy is removal of a lesion in total, plus a layer of surrounding normal tissue” • It is the combination of a diagnostic and definitive therapy
Indications • For lesions less than 2-2.5cms in diameter • clinically benign • That are small, well defined bony lesions Contraindication • Vascular & pigmented
ADVANTAGES • Entire lesion is available • Biopsy may be treatment for many cases
INCISIONAL BIOPSY • “Incisional Biopsy is the removal of a small portion of the lesion for microscopic examination”
Indications 1)Large Intrabony or soft tissue lesions 2)Diffuse lesions 3)Suspected malignancies • Hyperkeratotic lesions
Contraindications • Pigmented and vascular lesions • Ulcerations
PUNCH BIOPSY • This is a form of biopsy that in is best suited for the diagnosis of mucosal abnormalities that may require multiple biopsies • Biopsy punches • Size from 1.0 to 12.0 mm, increasing in increments of 0.5mm.
Procedure • The biopsy is done by placing the punch at the intended biopsy site • Rotating the punch back and forth • Until the level of the head of the punch is no longer visible • The punch is removed • Curved iris scissors. • Multiple plugs of tissues can be taken.
CORE BIOPSY • Core needle biopsy was introduced to over come the limitations of FNA • The core needles are larger caliber than fine needles • Mounted onto a spring-loaded device that allows small cylinders of tissue to be cut and collected within the notch of the needle ,14-gauge needles
BONE BIOPSY • A bone biopsy or bone marrow biopsy is a test in which a piece of bone or marrow taken for biopsy • A special drill needle is usually used. • A local anesthetic is given • A small (about 1/8 inch) incision is made in the skin • Biopsy needle is pushed and twisted into the bone. Bone marrow is removed for examination
Indications • Anemia • Hemochromatosis • Thrombocytopenia • Polycythemia Vera • Infectious diseases • Osteoid osteoma • Osteoblastoma • Bone cyst
HEALING • Healing of Biopsy wound is identical to healing of similar wound • By primary or secondary healing • Primary healing -healing which occurs after excision of a piece of tissue with close apposition of the edges. • This wound heals rapidly.
HEALING • Secondary healing- Healing by granulation or healing of an open wound occurs • When there is loss of tissue and edges of wound cannot be approximated • It is similar to healing by primary intention • Except that the fibroblasts and capillaries have a greater distance to migrate • More granulation tissue must form and healing is slower.
TOLUIDINE BLUE • Toluidine blue is a cationic metachromatic dye that binds sulphates, phosphates and carboxylates • This dye is used as an adjunct diagnostic test for the early detection of epithelial dysplasia and SCC of the oral cavity
Early detection of malignant changes in premalignant lesions. • As a method of follow-up.
Composition 100 c.c of the 1% TB solution:- 1gm of TB powder, • 10 ml of 1% acetic acid • 4.19 ml of absolute alcohol • 86ml of distilled water to make up 100 ml of a 1% solution of TB.
Procedure • Rinse his mouth twice with water for 20 seconds • 1% acetic acid is given for 20 seconds to remove any ropey saliva. • 1% TB solution is then applied for 20 seconds either with cotton swab or given as a rinse • A second rinse with 1% acetic acid will be given to reduce the extent of mechanically retained stain • Finally the mouth is rinsed with water
FIXATIVES • They undergo a process of self-destruction or autolysis • Which is initiated soon after cell death by the action of intracellular enzymes • Causing the breakdown of protein and eventually liquefaction of the cell. • Autolysis is independent of any bacterial action • Retarded by cold • Greatly accelerated at temperatures of about 30°C .
Autolysis is more severe in tissues which are rich in enzymes ,less in elastic fiber and collagen • `washed-out' appearance with swelling of cytoplasm • Objectives is to preserve cells and tissue constituents- life-like state, without change • Fixation arrests autolysis and bacterial decomposition
Formaldehyde solutions10% neutral buffer formalin (4% formaldehyde)REAGENTS REQUIRED1] 40% formaldehyde 100 ml2] Distilled water 900 ml3] Sodium dihydrogen orthophosphate 4 g4] Disodium hydrogen orthophosphate (anhydrous) 6.5 g
Interpretation • A dark blue (royal or navy)- positive • Light blue staining is considered doubtful. • If there is no colour absorbed-negative Positive