Excessive Bleeding in the Surgical Patient
260 likes | 548 Views
Excessive Bleeding in the Surgical Patient. Jeffrey H. Lawson, MD, PhD Director, Vascular Surgery Research Lab Director of Clinical Trials in Vascular Surgery Duke University Medical Center Durham, North Carolina. Learning Objectives.

Excessive Bleeding in the Surgical Patient
E N D
Presentation Transcript
Excessive Bleeding in the Surgical Patient Jeffrey H. Lawson, MD, PhD Director, Vascular Surgery Research Lab Director of Clinical Trials in Vascular Surgery Duke University Medical Center Durham, North Carolina
Learning Objectives • Develop strategies for patient risk stratification during the preoperative examination • Assess emergency surgical maneuvers to achieve operative hemostasis • Review challenges in balancing hemorrhage and thrombosis
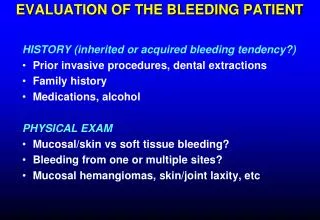
The Preoperative Patient Evaluation We’ve discussed previously in this initiative about certain risk factors to determine who might bleed perioperatively. Can you walk us through a proper “preoperative” patient evaluation?
The Preoperative Patient Evaluation • Conduct biochemical tests PT PTT Bleeding time Drawback: Not sophisticated enough to identify patients with subtle, undetectable polymorphisms • Conduct good clinical patient history Question patient on: • Multiple miscarriages • Bleeding from minor procedures • Easy bruising • Problems with previous surgeries • Family members having had difficult surgeries • Goal: Develop more appropriate screening measures that address coagulation polymorphisms not otherwise detected by abnormalities in PT, PTT PT = prothrombin time; PTT = partial thromboplastin time.
Stratifying Patients for Bleeding Risk Would you suggest using a formal risk stratification system in real practice?
Stratifying Patients for Bleeding Risk • Use general stratification system • Formal stratification with delineated levels of risk works in theory • In practice, consider a continuum of risk Patient placement on continuum based on medical history, family medical history, surgery type • Don’t pigeon-hole patients according to risk level • Inform patient and family of possible surgical risks for postoperative bleeding and thrombosis • For high-risk patients, modify surgical plan accordingly: Anesthesia requirements Cardiology clearance Availability of blood, other clotting factors
Continuum of Patient Types Although there may not be an awful lot of data to this end, is it rare to see patients on the more risky side of the continuum?
Continuum of Patient Types • General surgery Primarily low-risk patient cohorts • Vascular surgery; complex, targeted surgery High-risk patient cohorts • Elderly patients • Patients with prior surgeries • Patients with kidney failure • Patients with heart failure • All surgeries associated with bleeding and clotting issues
Surgical Hemostasis Outside of vascular surgery, for example in oncology, urology, orthopedic surgery … is this issue of hemostasis as critical as it is in vascular surgery?
Surgical Hemostasis • Bleeding and clotting are the most underappreciated problems in surgery As common as breathing air Like gravity that existed before Newton described it • At Duke University Medical Center, >50%-70% of surgical complications seen weekly are associated with bleeding and clotting • Bleeding and clotting are the leading cause of morbidity and mortality in surgery today
Prevention and Management of Perioperative Bleeding and Clotting What are some of the things that can be done perioperatively to manage bleeding and clotting issues when they occur?
Prevention and Management of Perioperative Bleeding and Clotting • Prevention of perioperative bleeding and clotting = good physiology and good surgery Good anesthesia support Patients kept warm Patients well resuscitated Management of calcium and acidemia • Management of perioperative bleeding and clotting: “Don’t get caught . . . behind the 8-ball” Ensure anesthesia is available Role for topical hemostatic agents Role for systemic therapies • Fresh frozen plasma • Cryoprecipitate • Platelets • Recombinant factor VIIa (rVIIa) • Antifibrinolytic molecules
Transfusion Issues It seems the threshold for initiating transfusion when bleeding occurs has been creeping lower. Can you discuss the use of blood and blood products?
Transfusion Issues • Still a role for blood and transfusion therapies • Blood management community more comfortable using lower transfusion threshold for patients • All blood is not created equal Fresher blood has healthier red cells than older blood Older, nearly expired red cells can be deleterious to patients • Transfusion trigger lower than it was 10-15 years ago • Quality of red blood cells and of transfused products is critical and still an area of important research
Practicing Bloodless Medicine What is the concept of “bloodless medicine”?
Practicing Bloodless Medicine • Possible for medical institutions to become completely bloodless • Respect religious beliefs and ethical systems of patients who do not advocate transfusion • Acknowledge risks associated with practice of bloodless medicine and possible adverse effects of hemorrhage • Balance inherent in transfusion; possible to practice bloodless medicine Accept some risk Derive some benefit • Requires a highly committed surgical team Anesthesia support OR staff Nursing staff • Intellectual shift required in postoperative management of patients
Newer Strategies for Achieving Optimal Hemostasis You had mentioned some “newer strategies” for achieving optimal hemostasis. Can you describe some of these and how you’re implementing them now?
Newer Strategies for Achieving Optimal Hemostasis • rVIIa Off-label use has gained wide acceptance in surgical community • Trauma • Intracranial bleeding • General surgery Novel, effective therapy • Antifibrinolytics Despite FDA concerns regarding aprotinin*, role for halting fibrinolysis is an exciting one Area of unique biologic therapy • Protamine Useful in stopping systemic heparinization • Future strategies in hemostasis Molecules with shorter half-lives Novel antidote therapies to reverse anticoagulation *Currently suspended for use in the United States.
Clopidogrel: Hemostatic Considerations What are some of the special considerations for patients taking clopidogrel (PLAVIX)?
Clopidogrel: Hemostatic Considerations • Standard of care for patients with drug-eluting coronary stents • Options for perioperative management of clopidogrel-treated patients: Operate through the clopidogrel Treat patient with systemic anticoagulation prior to surgery while clopidogrel wears off • No randomized trials demonstrating efficacy • In many cases, accept clopidogrel as a surgical reality and manage hemorrhagic complications that may result
The Hemorrhage and Thrombosis Continuum Let’s discuss the general balance between hemorrhage and thrombosis. How do they relate?
The Hemorrhage and Thrombosis Continuum • Hemorrhage and thrombosis are both extreme ends of the same biologic process • Lethal in their own right • Determine patient’s position on the continuum Hemorrhagic phenotype? Thrombotic phenotype? • Goal is to manage patients through a critical period—clinically, maintaining them in the center of both extremes
Healthcare Provider Call to Action Based on our conversation today, what would be your call to action to the audience?
Healthcare Provider Call to Action • Consider the way bleeding is approached clinically • Recognize that patients comprise a broad spectrum • No one type of normal phenotype in hemostasis • Each patient has different hemostatic needs Perioperative use of blood thinners Perioperative use of hemostatic tools Identifying postoperative risk for thrombosis • Despite lack of good biomarkers, use clinical intuition to identify who may be at risk for bleeding or thrombosis
Thank you for participating in today’s program www.bloodcmecenter.org Your source for CE/CME educational programs on operative hemostasis and transfusion medicine, including uniquely progressive learning designed for each clinical discipline