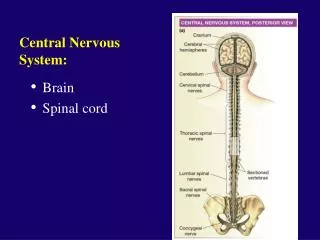
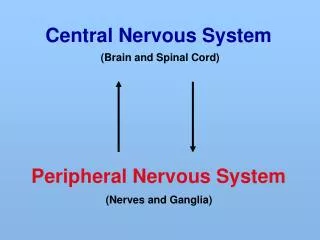
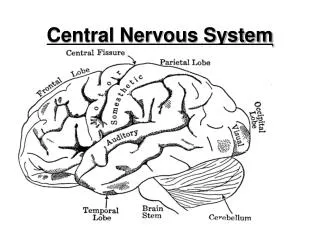
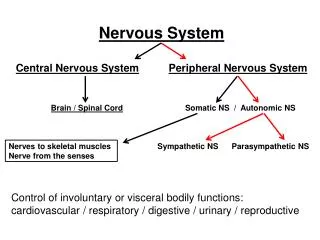
Central Nervous System Depressants
1.33k likes | 2.6k Views
Central Nervous System Depressants. CNS Depressants. Sedatives Drugs that have an inhibitory effect on the CNS to the degree that they reduce: Nervousness Excitability Irritability without causing sleep. CNS Depressants. Hypnotics

Central Nervous System Depressants
E N D
Presentation Transcript
CNS Depressants Sedatives • Drugs that have an inhibitory effect on the CNS to the degree that they reduce: • Nervousness • Excitability • Irritability • without causing sleep
CNS Depressants Hypnotics • Calm or soothe the CNS to the point that they cause sleep
CNS Depressants Sedative-Hypnotics—dose dependent: • At low doses, calm or soothe the CNS without inducing sleep • At high doses, calm or soothe the CNS • to the point of causing sleep
Sedative-Hypnotics: Barbiturates • First introduced in 1903, standard agents for insomnia and sedation • Habit-forming • Only a handful commonly used today due in part to the safety and efficacy of: BENZODIAZEPINES
Sedative-Hypnotics: Barbiturates Four categories: • Ultrashort • mephobexital, thiamylal, thiopental • Short • pentobarbital, secobarbital • Intermediate • aprobarbital, butabarbital • Long • phenobarbital
Sedative-Hypnotics: Barbiturates Barbiturates have a very narrow therapeutic index. Therapeutic Index • Dosage range within which the drug is effective but above which is rapidly toxic.
Sedative-Hypnotics: Barbiturates Mechanism of Action • Site of action: • Brain stem (reticular formation) • Cerebral cortex • By inhibiting GABA, nerve impulses traveling in the cerebral cortex are also inhibited.
Sedative-Hypnotics: Barbiturates Drug Effects • Low doses: Sedative effects • High doses: Hypnotic effects (also lowers respiratory rate) Notorious enzyme inducers
Sedative-Hypnotics: Barbiturates Therapeutic Uses • Hypnotics • Sedatives • Anticonvulsants • Surgical procedures
Sedative-Hypnotics: Barbiturates Side Effects Body System Effects CNS Drowsiness, lethargy, vertigo mental depression, coma Respiratory Respiratory depression, apnea, bronchospasms, cough
Sedative-Hypnotics: Barbiturates Side Effects Body System Effects GI Nausea, vomiting, diarrhea Other Agranulocytosis, vasodilation, hypotension, Stevens-Johnson syndrome
Sedative-Hypnotics: Barbiturates Toxicology • Overdose frequently leads to respiratory depression, and subsequently, respiratory arrest. • Can be therapeutic: • Anesthesia induction • Uncontrollable seizures: “phenobarbital coma”
Sedative-Hypnotics: Barbiturates Drug Interactions • Additive effects: • ETOH, antihistamines, benzodiazepines, narcotics, tranquilizers • Inhibited metabolism: • MAOIs will prolong effects of barbiturates • Increased metabolism: • Reduces anticoagulant response, leading to possible clot formation
CNS Depressants: Benzodiazepines Most frequently prescribed sedative-hypnotics • Most commonly prescribed drug classes • Favorable side effects • Efficacy • Safety
CNS Depressants: Benzodiazepines Classified as either: • Sedative-hypnotic or Anxiolytic (Medication that relieves anxiety)
CNS Depressants: Benzodiazepines Sedative-Hypnotic Type • Long-Acting: • flurazepam (Dalmane), quazepam (Doral) • Short-Acting: • estazolam (Prosom), temazepam (Restoril), • triazolam (Halcion)
CNS Depressants: Benzodiazepines Anxiolytic Type • alprazolam (Xanax) • chloridiazepoxide (Librium) • diazepam (Valium) • lorazepam (Ativan) • midazolam (Versed) zolpidem (Ambien) and zaleplon (Sonata) (nonbenzodiazepine hypnotic agents, share characteristics)
CNS Depressants: Benzodiazepines Mechanism of Action • Depress CNS activity • Affect hypothalamic, thalamic, and limbic systems of the brain • Benzodiazepine receptors
CNS Depressants: Benzodiazepines Drug Effects • Calming effect on the CNS • Useful in controlling agitation and anxiety
CNS Depressants: Benzodiazepines Therapeutic Uses • Sedation • Sleep induction • Skeletal muscle relaxation • Anxiety relief • Treatment of alcohol withdrawal • Agitation • Depression • Epilepsy • Balanced anesthesia
CNS Depressants: Benzodiazepines Side Effects • Mild and infrequent Headache Drowsiness Dizziness Vertigo Lethargy Paradoxical excitement (nervousness) “Hangover effect”
CNS Depressants: Nursing Implications • Before beginning therapy, perform a thorough history regarding allergies, use of other medications,health history, and medical history. • Obtain baseline vital signs and I & O, including supine and erect BPs. • Assess for potential disorders or conditions that may be contraindications, and for potential drug interactions.
CNS Depressants: Nursing Implications • Give 15 to 30 minutes before bedtime for maximum effectiveness in inducing sleep. • Most benzodiazepines (except flurazepam) cause REM rebound and a tired feeling the next day; use with caution in the elderly. • Patients should be instructed to avoid alcohol and other CNS depressants.
CNS Depressants: Nursing Implications • Check with physician before taking any other medications, including OTC medications. • It may take 2 to 3 weeks to notice improved sleep when taking barbiturates. • Abruptly stopping these medications, especially barbiturates, may cause rebound insomnia.
CNS Depressants: Nursing Implications • Safety is important • Keep side rails up • Do not permit smoking • Assist patient with ambulation (especially the elderly) • Keep call light within reach • Monitor for side effects
CNS Depressants: Nursing Implications • Monitor for therapeutic effects • Increased ability to sleep at night • Fewer awakenings • Shorter sleep induction time • Few side effects, such as hangover effects • Improved sense of well-being because of improved sleep
Chapter 8 Topics • Epilepsy • Parkinson’s Disease • Myasthenia Gravis • Attention-Deficit Disorders • Amyotrophic Lateral Sclerosis (ALS) • Multiple Sclerosis (MS) • Alzheimer’s Disease
Learning Objectives • Develop an understanding of the physiologic processes that occur in epilepsy. • Classify seizures and the goals of their therapy. • Understand that specific drugs are used in different classes of seizures.
Learning Objectives • Be familiar with Parkinson’s disease and the drugs used in its treatment. • Know the symptoms and treatments of • myasthenia gravis • attention-deficit disorders • amyotrophic lateral sclerosis • multiple sclerosis • Alzheimer’s disease
Epilepsy • Common neurologic disorder with sudden and recurring seizures • Caused by abnormal electrical impulses in the brain
Epilepsy • In the U.S., 2.5 million people are affected. • Not all seizure disorders are epilepsy.
Epilepsy Seizure Abnormal electrical discharges in the cerebral cortex caused by sudden, excessive firing of neurons • Result in a change in behavior of which the patient is not aware • While conscious, the patient may or may not lose movement control • Loss of body control may affect one area or the entire body
Epilepsy Causes of Seizures • Imbalance of excitatory and inhibitory neurotransmitters: • Glutamate – inhibitory • GABA – excitatory • Other neurotransmitters can be involved • Neurotransmitter levels are controlled by enzymes • Disruption in enzymes = disruption of neurotransmitters
Causes of Seizures ETOH withdrawal Cardiovascular disease High fever Hypocalcemia High or low blood sugar Hypoxia Infection (meningitis) Metabolic abnormalities Brain tumor Toxic substances Trauma or injury to the head Epilepsy
Epilepsy Classes of Seizures • Partial • Generalized
Epilepsy Classes of Seizures • Partial • Simple-partial • Complex-partial • Generalized
Epilepsy Classes of Seizures • Partial • Simple-partial • Complex-partial • Generalized • Tonic-clonic or grand mal • Absence or petit mal • Myoclonic • Atonic
Epilepsy Partial Seizures • Localized in a specific area of the brain • Occurs with 65% of epileptic patients • Can progress to generalized seizures
Epilepsy Partial Seizures • Simple-Partial • Complex-Partial
Epilepsy Partial Seizures • Simple-Partial • No loss of consciousness • May have muscle twitching or sensory hallucinations • Complex-Partial
Epilepsy Partial Seizures • Simple-Partial • No loss of consciousness • May have muscle twitching or sensory hallucinations • Complex-Partial • Impaired consciousness • With confusion, blank stare, and postseizure amnesia
Epilepsy Generalized Seizures • Involves both hemispheres of the brain, not one specific location • Types • Tonic-Clonic • Absense • Myoclonic • Atonic
Generalized Seizures Tonic-Clonic Seizures • Tonic – body becomes rigid, lasts a minute or less • Clonic – initiated with muscle jerks, and may be accompanied by shallow breathing, loss of bladder control, and excess salivation
Generalized Seizures Absence • Interruption of activities by blank stare, rotating eyes, uncontrolled facial movements, rapid eye blinking, and/or jerking of an arm or leg • No generalized convulsions • Usually lasts 30 seconds or less • Many times it progresses to tonic-clonic as the patient gets older
Generalized Seizures Myoclonic • Occurs with sudden, massive, brief muscle jerks or non-massive, quick jerks • Consciousness is not lost • Can occur during sleep
Generalized Seizures Atonic • Begins with sudden loss of muscle tone and consciousness • Muscles relax, limbs go limp • Lasts a few seconds to a minute, then patient can resume standing and walking
Generalized Seizures Status Epilepticus • Continuous tonic-clonic seizures with or without return to consciousness • High fever and lack of oxygen severe enough to cause brain damage or death