Foot Drop
Foot Drop. Chairpersons : Dr. Rupakumar .C.S. Dr . Ravikiran Presented by : Dr. Syed Imran. Definition : Inability to actively dorsiflex and evert the foot.

Foot Drop
E N D
Presentation Transcript
Foot Drop Chairpersons : Dr. Rupakumar .C.S. Dr. Ravikiran Presented by : Dr. SyedImran
Definition : Inability to actively dorsiflex and evert the foot. • Introduction : Foot drop is a condition where the propulsion is partially impaired due to changes in gait.
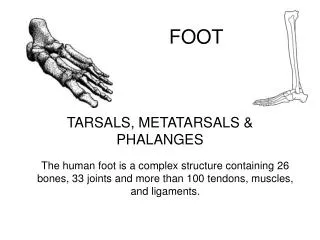
Anatomy of leg : • Two muscular septa divide leg into three compartments • Anterior ( Extensor) compartment • Lateral ( Peroneal ) compartment • Posterior ( Flexor ) compartment
Common Peroneal Nerve • Half size of tibial nerve • L4,5,S1,2 • Enters leg antero- laterally • Branches
Sup Peroneal Nerve • Superficial fibular N • Deep to peroneus Longus then passes Anteroinf b/w peroneuslongus and EDL
Deep peroneal Nerve • Oblique forward deep to EDL to front of interosseus membrane and reaches Ant.Tibial artery in proximal 1/3 • Branches
Etiology : • Neuromuscular disease • Peroneal Nerve • Sciatic Nerve • Lumbosacral plexus • L5 Nerve root • Spinal cord ( poliomyelitis, tumour ) • Brain ( Stroke, TIA ) • Genetic ( CMT ) • Non-organic
Traumatic : Extensor and peroneal tendon injuries • Neurogenic 1. At level of common peroneal N • Direct injuries • Fractures and dislocations • # / dislocation head / neck of fibula • Dislocation of Sup. Tibiofibularjt • Dislocation of knee • Compound # upper 1/3 tibia
Pathogenic • High skeletal tibial traction • Tight plaster around knee joint • High tibialosteotomy • Total knee replacement Others Lat meniscalcysts,Exostosis,Tumour of head of fibula
Above level of Common Peroneal N • At the thigh : # shaft femur, penetrating injuries • At the hip : Post dislocation of hip,# hip • At the gluteal region : Deep iminj • At the spine : IVDP,Spina bifida, tumours
Infective : Leprosy,poliomyelitis, GBS, Syphillis • Metabolic : DM,Beriberi, Alcoholic neuritis • Exogenous toxin : Lead, arsenic, mercury.
Classification : • Seddon : • Neurapraxia • Axontemesis • Neurotemesis
Signs and Symptoms : • Weakness of dorsiflexion and eversion of foot • High stepping gait : Foot slap followed by heel strike, toe drag during swing phase,increased hip and knee flexion • Sensory loss
Autonomous Zone of Common peroneal N
Clinical Examination • Signs of motor denervation : Paralysis, loss of tone, areflexia, Insensibility to compression, atrophy • Signs of Autonomic denervation • Loss of sweating • Vasomotor • Loss of hair • Trophic ulceration
Diagnostic tests : • Nerve conduction velocity
Autonomic tests • Sweat test : Presence of sweat within autonomous zone indicates that complete denervation has not occurred. • Wrinkle test • Skin resistance test : Increased resistance to passage of electric current
Assessment of recovery : • Tinels sign • Motor recovery M0- No contraction M1- Return of contraction in proximal gp M2 – Proximal gp + Distal gp M3- Muscles can act against resistance M4 – All synergistic independent movts possible M5- Complete recovery
Sensory recovery S0- Absence of sensibility in autonomous area S1- Recovery of deep cutaneous pain S2- Superficial cutaneous pain + Tactile sensibility ( some degree ) S3- Throughout autonomous area S3+ - Recovery of 2-point discrimination S4- Complete recovery
Management • Conservative • Aim : Prevention of deformity and improvement of gait. • Proper positioning of foot splints • Passive movements of joints • Electrical stimulation of muscles • Ankle foot orthosis
AFO • Functions : • Provide toe dorsiflexion during swing phase • Medial and lateral stability at ankle during stance • Push off stimulation during late stance • Dynamic or static
Surgical management • Neurorrhaphy • Tendon transfers • Bony operations • Choice of surgical correction depends on • Mobility of joints • Soft tissue and muscle contractures • Availability of muscles and tendons for transfer • Bony changes • Age
Neurorrhaphy • Indications • Clean and sharply incised nerve injury • Contaminated and nerve transection with ragged ends • Nerve injury following blunt trauma or closed fractures • Following closed reduction or manipulation of fracture
Techniques • Epineuralneurorrhaphy • Perineuralneurorrhaphy • Epiperineuralneurorrhaphy • Interfascicularnervegrafting
EpineuralNeurorrhaphy • Gap can be closed end to end Without excessive tension
Tendon transfers • When joints are mobile and muscles and tendons are available for transfer • Objectives • To provide active motor power to replace function of paralysed muscle • To eliminate deforming force when antagonist is paralysed • To improve stability by improving muscle balance
Principles of tendon transfer • The muscle to be transferred should be healthy • Muscle strength should be grade 4-5 • Free range of movement in joint • Any bony deformity should be corrected • It is desirable to use synergistic muscle as it is easier to rehabilitate
Joints proximal to parts to be moved should be stabilised by tendon action • Tendon must be attached under moderate tension • If tendon is split, tension must be equal at all points • Nerve and blood supply must not be impaired
Barr technique • Make a skin incision on medial side of ankle from insertion of tibialis posterior and post to malleolus proximally along medial border of tibia. • Split the sheath in a proximal direction until distal 5cm of muscle is mobilised.
Make second incision anteriorly beginning distally at level of ankle joint extending laterally to tibialis ant tendon . • The dissection should be between tendons of tibialis anterior and EHL preserving dorsalispedis artery.
Make a generous window in interosseus membrane pass tibialis posterior tendon through window between bones. • Expose third cuneiform or base of third metatarsal,inciseperiosteum drill a hole large enough to receive tendon and anchor in bone with a wire
Two-tailed trasfer • Two tailed transfer of tibialis posterior • The tendon of tibialis posterior is identified through a small incision over the tuberosity of the navicular bone. • The tendon is then detached from its insertion and its synovial attachments are divided. .
five-centimetre longitudinal incision is made in the lower part of the leg close to the medial border of the tibia, about ten centimetres above the medial malleolus. The tendon of tibialis posterior is identified and pulled out.
The tendon is then split longitudinally into two “ tails “ up to the point where it will cross the tibia proximally. • Two transverse incisions are made on the dorsum of the foot, one over the extensor hallucislongus tendon and the other more laterally, over the tendons ofthe extensor digitorumlongus.
A tendon tunneller (Andersen’s tunneller) is passed from the wounds in the dorsum to the wound in the leg. The tunnels are made subcutaneously. • Two separate tunnels are made for the two “ tails “ of the motor tendon.
The motor slips are pulled through. One is implanted in the tendon ofextensorhallucislongus and the other in the tendons of extensor digitorumlongus. • During this stage the knee is held in flexion of about 30 degrees and the ankle in dorsiflexion of at least 10 degrees.
After operation a below-knee plaster is applied, with the foot further dorsiflexed to release any tension on the tendon sutures during healing. • Six weeks after operation the patient is started on walking training. On the average the patient needs another two weeks to learn to walk normally.
Lengthening of tendoachilles • White technique • Use a posteromedial incision to expose the Achilles tendon from its insertion to approximately 10 cm proximally, preserving the sheath • Divide the posteromedial two thirds of the tendon near its insertion. • Apply a moderate dorsiflexion force to the foot, and divide the medial two thirds of the tendon approximately 5 to 8 cm proximal to the site of the distal division.
Dorsiflex the foot so that the tendon lengthens to the desired length • Carefully close the tendon sheath and subcutaneous tissues to prevent adherence of the tendon to the overlying skin. • Apply a short leg cast with the ankle in maximal dorsiflexion.