lyme disease Borrelia
340 likes | 517 Views
lyme disease Borrelia. Dr.T.V.Rao MD. In the early 1900s, manifestation first reported in Europe associated it with tick bites In 1975, outbreak in Lyme, Connecticut Believed to be juvenile rheumatoid arthritis

lyme disease Borrelia
E N D
Presentation Transcript
lyme diseaseBorrelia Dr.T.V.Rao MD Dr.T.V.Rao MD
In the early 1900s, manifestation first reported in Europe associated it with tick bites In 1975, outbreak in Lyme, Connecticut Believed to be juvenile rheumatoid arthritis In 1982, spirochetes were identified in the midgut of the black-legged tick (Ixodes scapularis) and named Borrelia burgdorferi. In 1984, Borrelia burgdorferi was isolated from the blood of patients with EM and from the rash lesion itself. Determined etiologic agent Today, it is the most common tick-borne infection in the U.S. more than 16,000 infections each year. Disease History
Borrelia is a Spirochete • Group or bacteria with a highly characteristic appearance • Helical, slender, relatively long cells • One of the species of “borrelia” cause lyme disease in human Dr.T.V.Rao MD
Borrelia and Amédée Borrel. • Borrelia is a genus of bacteria of the spirochete phylum. It causes borreliosis, a zoonotic, vector-borne disease transmitted primarily by ticks and some by lice, depending on the species. There are 36 known species of Borrelia. The genus was named after the French biologist Amédée Borrel. Dr.T.V.Rao MD
taxonomy Super kingdom: Bacteria Phylum: spirochaetes Order: spirochaetales Family: spirochaelaceae Genus: Borrelia Species: borrelia burgdorferi Dr.T.V.Rao MD
Borrelia burgdorferi sensu stricto Spirochete: slender helical shaped bacteria Gram negative Motile Extracellular pathogen Aerobic or microaerophilic Causative Agent
Population at risk • Most Burgdorferi infections result from residential exposure to infected ticks during property maintenance, recreation, and leisure activity • The person who engage in outdoor occupations • Forestry • landscaping Dr.T.V.Rao MD
Lyme Disease • Lyme disease is caused by bacteria called Borrelia burgdorferi (B. burgdorferi). Blacklegged ticks carry these bacteria. The ticks pick up the bacteria when they bite mice or deer that are infected with Lyme disease. You can get the disease if you are bitten by an infected tick. • Lyme disease was first reported in the United States in the town of Old Lyme, Connecticut, in 1975 Dr.T.V.Rao MD
What is lyme disease • Lyme disease (named after the town of Lyme, Connecticut, where a number of cases were identified in 1975) is a seriously complex multi-system inflammatory disease that is triggered by the bacterial lipoproteins (BLPs) produced by spiral-shaped bacteria called Borrelia burgdorferi, also called Bb. Bb are difficult to isolate, grow, and study in the laboratory. Dr.T.V.Rao MD
Caused by spirochete Borrelia burgdorferi Transmitted by Ixodes ticks Nymph-stage ticks feed on humans May through July - transmit spirochete Endemic areas Northeastern coastal states Wisconsin & Minnesota Coast of Oregon & northern California EPIDEMIOLOGY
Distribution • Mostly localized to states in the northeastern, mid-Atlantic, and north-central regions, and to several counties in northwestern California http://www.cdc.gov/ncidod/dvbid/lyme/ Dr.T.V.Rao MD
Vector-borne disease Vector is deer or black-legged tick (Ixodes scapularis) or by the western black-legged tick (Ixodes pacificus) on the Pacific Coast. Transmits B. burgdorferi while feeding on an uninfected host the spirochetes are present in the midgut and migrate during blood feeding to the salivary glands, from which they are transmitted to the host via saliva. B. burgdorferi cannot penetrate intact skin Methods of Transmission Dr.T.V.Rao MD
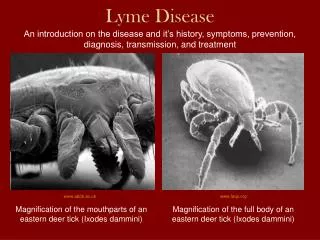
Larva, nymph, and adult female and male Ixodes dammini ticksThey are smaller than we think Dr.T.V.Rao MD
Ticks life cycle Dr.T.V.Rao MD
What is Lyme Disease? • Lyme disease is caused by the bacterium Borrelia burgdorferi and is transmitted to humans by the bite of infected ticks. • *Normally lives in mice, squirrels and other small animals • Blacklegged (deer) ticks • Lone star ticks • American dog ticks
How the infection is initiated • When an infected louse feeds on an uninfected human, the organism gains access when the victim crushes the louse or scratches the area where the louse is feeding. B. recurrentis infects the person via mucous membranes and then invades the bloodstream. Dr.T.V.Rao MD
Symptoms • The early symptoms are mild and easily overlook. • The first symptom is usually an expanding rash. • Called erythema migrans. • Appear as a solid red expanding rash or blotch, OR a central spot surrounded by clear skin that in ringed by an expanding red rash looks like bull’s eye. Dr.T.V.Rao MD
Common presenting symptoms in lyme disease • Symptoms of early localized Lyme disease (Stage 1) begin days or weeks after infection. They are similar to the flu and may include: • Body-wide itching • Chills • Fever • General ill-feeling • Headache • Light-headedness or fainting • Muscle pain • Stiff neck • There may be a "bull's eye" rash, a flat or slightly raised red spot at the site of the tick bite. Often there is a clear area in the center. It can be quite large and expanding in size. Dr.T.V.Rao MD
Classic Bull’s Eye Rash Dr.T.V.Rao MD
Less Classic lesions Dr.T.V.Rao MD
symptoms of early disseminated Lyme disease (Stage 2 and Stage 3 ) • Paralysis or weakness in the muscles of the face • Muscle pain and pain or swelling in the knees and other large joints • Heart problems, such as skipped heartbeats (palpitations) • Symptoms of late disseminated Lyme disease (Stage 3) can occur months or years after the initial infection. The most common symptoms are muscle and joint pain. Other symptoms may include: • Abnormal muscle movement • Muscle weakness • Numbness and tingling • Speech problems Dr.T.V.Rao MD
General Profound fatigue, headache, fever severe muscle aches/pain Brain (tingling sensations of the extremities- peripheral neuropathy, facial palsy Eyes :vision changes, retinal damage, optic atropy Skin: rash not at bite site (erythema migrans) Disseminated lyme disease Dr.T.V.Rao MD
Relapsing fever • Relapsing fever borreliosis often occurs with severe bacteraemia. Borrelia recurrentis is transmitted by the human body louse; no other animal reservoir of B. recurrentis is known. Lice that feed on infected humans acquire the Borrelia organisms that then multiply in the gut of the louse. Dr.T.V.Rao MD
There are number of blood test available Antibody test :ELISA and western blot tests. Although there is false positive and negative results Antigen detection tests Polymerase chain reaction: this test multiplies the of Bb DNA to detectable measurable level Diagnosis Dr.T.V.Rao MD
Serologic data by IFA, ELISA and imunoblottingtechniques. Detect presence of IgM or IgG antibodies in patient’s serum against Borrelia burgdorferi Tests are insensitive the first several weeks of infection Western blot is more accurate and is used 6-12 weeks after infection to confirm results Direct Isolation Biopsies of the skin lesions may yield the organism in 50% or more of cases Diagnosis Dr.T.V.Rao MD
Antibiotic therapy Doxycycline and amoxicillin are used for two to four weeks in early cases Doxycycline is also effective against human granulocytic ehrlichiosis Cefuroxime axetil or erythromycin can be used for patients who are allergic to penicillin or who cannot take tetracycline's. More developed cases, may require treatment with intravenous ceftriaxone or penicillin for 4 weeks or more Treatment Dr.T.V.Rao MD
Precautionary routine Wear enclosed shoes and light-clolred clothing with a tight weave to spot ticks easily Scan clothes and any exposed skin Stay on cleared, well- traveled trails Insect repellent containing DEET (Diethyl-meta-tolumide) in skin or cloths Inspect yourself and your children carefully after been heavily bushed area prevention Dr.T.V.Rao MD
Avoid tick habitats Wear appropriate barrier clothing that follow personal protection procedures Apply insect repellent containing DEET to skin Apply permethrin to clothes Perform regular body checks for ticks Remove ticks promptly with tweezers and clean area with antiseptic Education of the general public Prevention Dr.T.V.Rao MD
How to remove ticks Dr.T.V.Rao MD
Prevention of lyme disease • Take precautions to avoid direct contact with ticks. Be extra careful during warmer months. Whenever possible: • Avoid wooded or bushy areas, or areas with high grasses and leaf litter.. • Ticks that carry Lyme disease are so small that they are very hard to see. After returning home, remove your clothes and thoroughly inspect all skin surface areas, including your scalp. Shower soon after coming indoors to wash off any unseen ticks. Dr.T.V.Rao MD
Habitat modification for ticks -Clear trees and brush Chemical control of tick populations -Apply pesticides to residential properties Habitat modification for deer and rodents -Keep rodents and deer away from houses and gardens Host management -Deer feeding stations equipped with pesticide applicators -Baited devices to kill ticks on rodents Control Dr.T.V.Rao MD
Programme Created by Dr.T.V.Rao MD for Medical and Health Care Professionals • Email • doctortvrao@gmail.com Dr.T.V.Rao MD