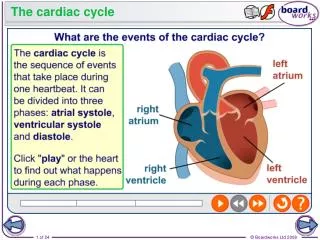
The Cardiac cycle
The Cardiac cycle. Can confidently label internal & external photos of the heart Can describe the cardiac cycle Can explain how the heart valves help with the cardiac cycle. Bell Task. Label the heart diagram and complete the questions. Label the gaps. Answer these questions.

The Cardiac cycle
E N D
Presentation Transcript
The Cardiac cycle • Can confidently label internal & external photos of the heart • Can describe the cardiac cycle • Can explain how the heart valves help with the cardiac cycle
Bell Task • Label the heart diagram and complete the questions
Answer these questions • Which side has the thickest muscular wall and why. • Where does blood go to from the right side of the heart? • Where does blood go to from the left side of the heart? • What is the heart made from? • What is the function of the valves? • What 2 problems would occur with a hole in the wall between the left and right side?
Where are the Valves in the heart? • Atrioventricular valves: these valves separate an atrium from a ventricle. • Semilunar valves: found in arteries leaving the heart (pulmonary arteries and aorta).
Atrioventricular valves • Tricuspid – 3 flaps • Biscuspid – 2 flaps
Valves Inside the heart and at the base of the vessels that leave the heart are valves. These valves only open one way, which ensures that there is no backflow of blood.
The cardiac cycle • Beats around 70 times a minute. • If you listen to the heart with a stethoscope you hear the sounds often described as “lubb-dupp”. • The cardiac cycle is sequence of events that make up one heart beat. • Continuous
Arterial systole • The heart fill up with blood and the muscle in the atrial wall contracts. • Pressure developed is not very big, as muscular atrial walls are only thin. • Forces blood through the atrio-ventricular valve and into the ventricles.
The blood cannot flow back into the vena cava or the pulmonary vein, As these have semilunar valves, to prevent backflow. Instead it is pushed into the ventricles
Ventricular systole • About 0.1 second after atrial systole the ventricles contract. • The thick muscular walls of the ventricles squeeze inwards on the blood. • This increases the pressure and pushes it out of the heart
As soon as the pressure in the ventricles becomes greater than in the atria. The pressure pushes the atrio-ventricular valves shut, preventing backflow. (‘lubb’) Instead it rushes up into the aorta and the pulmonary artery pushing open the semilunar valves.
Ventricular diastole • After about 0.3 seconds, the muscle relaxes and diastole begins. • As pressure drops the semilunar valves snap shut as blood fills their cusps. (‘dubb’) • Whole heart relaxes and blood flows into atria again and the cycle is repeated.
The valves are held open or closed by tendons (heart strings), which are attached at the other end to the papillary muscles in the ventricle walls. The valves open to let blood through and then snap shut. This sound of the valves closing is the ‘lub dub’ sound of the heartbeat.
The muscle of the heart is called cardiac muscle and is made of tightly connecting cells. This close contact allows rapid ion transport from cell to cell. This then allows smooth, efficient waves of depolarisation to produce contractions (and repolarisation to bring about relaxation), which pass through the heart.
The tissue is said to be myogenic i.e. it does not need electrical impulses from a nerve to make it contract. If the cardiac muscle is supplied with oxygen and nutrients (a task carried out by the coronary arteries which you can see running over the surface of the heart) it will continue to contract at a steady pace. Nerves supplying the heart, though they are not needed to start the contractions, can bring about an increase or decrease in the rate of contractions when appropriate.
Task… • Answer question 5 on page 69 • You will need to draw the graph
Heart Action • Can explain how the SAN, AVN & Purkyne tissue coordinate the heart action • Interpret & describe ECG traces in normal & abnormal heart rhythms
Atrio-ventricular valves close because the pressure is higher in the ventricle than in the atria. • Semilunar valve in aorta opens due to pressure from the ventricles. • Semilunar valves close because the pressure in aorta is higher than in ventricle. (Blood tries to flow back and closes the cups in the valve • Atrio-ventricular valves close because the pressure is higher in the atrium than in the left ventricle. Semilunar valve in aorta shuts (aortic valve)
The electrical control of the heart • Cardiac muscle is MYOGENIC which means it can contract & relax without receiving signals from nerves • It can control it’s own activity
The waves spread out over the 2 atrial walls so that they contract. • There is a band of fibres between the atria and ventricles, which have a high electrical resistance so the waves cannot spread from the atria to the ventricles. 2 • The heartbeat is initiated in a specialised area of muscle in the right atrium called the sinoatrial node (SAN) or the pacemaker. • The SAN starts the waves of electrical activity, which results in contraction. • 1 The AVN passes the waves on to the Purkinje (also called Purkyne) fibres in the inter-ventricular septum. The excitation is passed to the apex of the heart and then through the ventricle walls. This causes the ventricles to contract from the base upwards ensuring that the blood is forced up and out in the vessels leaving the heart. 4 • There is an area, however, which conducts in the septum, and the waves can pass from here through the ventricles. • This specialised area is called the atrioventricular node (AVN) and will pass on the waves of electrical activity after about 0.1s. 3 It would be disastrous if the ventricles contracted at the same time as the atria so that is why there is a short period of delay before the ventricles contract.
Task… • With the help of diagrams you must produce a flow chart showing the stages that are involved in the heart beat • Pages 70, 71 & 72 will help you • Use all of the relevant keywords: Myogenic, SAN, AVN, Purkyne tissue…
Un-Control of Heart Beat!Put in the correct order • SAN contracts and starts off signal • Passes to the base of the septum and up through the ventricle wall • Wave passes to Purkyne fibres in the septum • Fibres between atria and ventricles do not contract • Wave spreads to AVN in septum • Ventricles contract • Atria contract
Un-Control of Heart Beat!Put in the correct order • SAN contracts and starts off signal • Atria contract • Fibres between atria and ventricles do not contract • Wave passes to Purkyne fibres in the septum • Wave spreads to AVN in septum • Passes to the base of the septum and up through the ventricle wall • Ventricles contract
ECG - Electrocardiograph • Doctors can check heart activity by using a machine that records the electrical activity of the heart • The heart depolarises (looses electrical charge) when it contracts • It repolarises (regains charge) when it relaxes • An electrocardiogram allows doctors to assess heart health
ECG QRS complex = contraction of ventricles T wave = relaxation (repolarisation) of ventricles P wave = contraction (depolarisation) of atria 0.4 0.8 0 0.2 Time/s Atrial systole Ventricular systole Diastole
Tasks • What is fibrillation? • Describe an electrocardiogram showing fibrillation • How do heart monitors save a patient’s life? • What is a defibrillator & when might it be used? • Answer SAQ 6 • Past questions
Blood vessels • Can identify veins, arteries & capillaries from diagrams/photos • Can describe how the structure of these vessels relates to their function
Which is the ‘normal?’ Regular rhythm of approx 60 bpm Irregular rhythm, heart rate too slow
Which is the ‘normal?’ Regular rhythm of approx 60 bpm Irregular rhythm, heart rate too fast
Which is the ‘normal?’ Regular rhythm of approx 60 bpm Irregular rhythm, no clear P wave, SA node not initiating beat
Which is the ‘normal?’ Regular rhythm of approx 60 bpm Irregular rhythm, Atrial fibrulation, no clear SAN, most of atrium generating own impulses, no clear P wave due to random impulses
Which is the ‘normal?’ Regular rhythm of approx 60 bpm AV block, impulse not reacing AVN from SAN, long PR interval
Tunica externa
Arteries… • Transport blood at high pressure to the tissues • Inner endothelium made of squamous epithelium (smooth cells to reduce friction) • Tunica media containing smooth muscle, collagen & elastic fibres • Tunica externa containing elastic fibres & collagen
Externa & elastic fibres & collagen
Arterioles… • Smaller branches of the arteries • Walls are similar to arteries but have a greater proportion of smooth muscle • This allows them to contract & narrow the lumen so blood flow can be controlled • For example during exercise they will be dilated to allow maximum blood flow to muscles
Capillaries • Smaller branches of the arterioles & will serve every cell in the body • Found in every tissue except the cornea & cartilage • Group together to form capillary beds • The lumen is same size as a RBC to allow efficient diffusion • They are 1 cell thick… made up of endothelial tissue
Venules Veins • Capillaries regroup to form venules which them turn into veins • Transports blood back to heart at very low pressure • Contains semi-lunar valves to prevent backflow of blood • The Tunica externa is mostly collagen • The Tunica media is very thin & contains some smooth muscle & elastic fibres • The Tunica intima is the same as the artery with endothelium tissue
Questions • How do muscles help veins perform their function? • Arteries carry oxygenated blood away from the heart, but what is the 1 exception? • Why do you think there are no capillaries in the cornea of the eye? • What does blood pressure oscillate (go up & down) in the arteries? • Why does the blood pressure drop in the arterioles & capillaries?