ral H ealth I s V ital
330 likes | 513 Views
ral H ealth I s V ital . What is hiv ?. HIV stands for Human I mmunodeficiency V irus HIV weakens a person ’ s immune system, resulting in complications and higher susceptibility to various diseases. TARGET AUDIENCE. 12-18 year olds with xerostomia (dry mouth).

ral H ealth I s V ital
E N D
Presentation Transcript
What is hiv? • HIV stands for Human Immunodeficiency Virus • HIV weakens aperson’s immune system, resulting in complications and higher susceptibility to various diseases
TARGET AUDIENCE 12-18 year olds with xerostomia (dry mouth) Source: New York States Department of Health AIDS Institute; NIDRC. Youth with HIV/AIDS
YOUTH WITH HIV: GENERAL FACTS Source: New York States Department of Health AIDS Institute; NIDRC. • Majority of HIV positive adolescents acquire their infection during the adolescent period • In the U.S., approximately half of new HIV infection cases are within the range of 13-24 years old • With the introduction and improvement in antiretroviral (ARV) therapy, children and adolescents with HIV are now living longer • Health care providers are now more likely to encounter adolescents living longer with HIV
YOUTH WITH HIV & ORAL HEALTH • Caries is a cumulative diseasethat begins in early childhood • Periodontal disease begins in early adolescence • Teens have the highest disease rate of all child age groups
YOUTH WITH HIV & ORAL HEALTH • Intrinsic factors: • Effects of HIV medications on salivary flow Xerostomia • Delayed dental eruption • Progressive immunodeficiency • Extrinsic factors: • Limited resources/access to dental care • Lack of caregiver knowledge Youth infected with HIV are at higher risk for developing dental caries than those without Source: New York State Department of Health AIDS Institute
YOUTH WITH HIV & ORAL HEALTH Source: Stenger 2006. • Some symptoms suggestive of HIV in youth: • Abnormal oral conditions: infections & lesions • Developmental delays such as: • Age-appropriate weight & height • Age-appropriate neurological development • Dental eruptions; retention of primary teeth
CHARACTERISTICS OF YOUTH WITH HIV Oral candidiasis • 30-80% of HIV-infected individuals display oral abnormalities • Common oral conditions include: • Xerostomia (dry mouth) • Oral candidiasis • Herpes • Kaposi’s sarcoma • Hairy leukoplakia Kaposi’s sarcoma Source: Stenger2006
Xerostomia • Xerostomia is a condition associated with a decrease or lack of saliva production, resulting in a dry mouth
Why Xerostomia? • 40% of patients HIV positive patients suffer from this condition • Lack of saliva production can result in diminished antimicrobial properties • Lead to a rapid increase in dental caries and many other serious periodontal diseases • Since this condition seems to prevail among HIV-infected individuals and it affects oral health, it will be our main focus to manage and prevent dental caries (Stenger, 2006)
XEROSTOMIA AMONG Hiv positive patients • Large array of xerostomic medication • Antihistamines, Antidepressants, Antipsychotic, Antihypertensive an Anticholinergic agents • Salivary gland hypofunction study on a cohort of HIV positive and HIV negative women: • HIV + Resting unstimulated saliva production: 0.29mL/min • HIV – Resting unstimulated saliva production: 0.35mL/min (M.Navazesh, 2000)
Functions of saliva • Surface Coating of Mucosa and Teeth • Acid Buffering • Humidifies and lubricates the mouth • Cohesive Food Bolus Formation to Facilitate Swallowing • Digestive Enzymes for Starch Hydrolysis • Antimicrobial properties • Modulation of Demineralization and Remineralization of Tooth Structure (John Hicks, 2003)
Complications of Xerostomia • Plaque build-up around dentition • Acid release from metabolism of Carbohydrates • Leading to dental caries and subsequent cavities if left untreated. • Plaque build-up: a multifactorial issue • Management of Plaque • Treatment of source of xerostomia
Management of plaque • Most effective manual method of plaque removal • TOOTH BRUSHING!!!! • Studies have shown that a combination of use of toothbrush, dental floss and tooth pick yields best results, compared to using any single device (Max O. Schimd, 1976)
Plaque Removing Effect (Max O. Schimd, 1976)
Treatment of Xerostomia • Direct link between reduction of saliva flow and dental caries. (James Guggenheimer, 2003) • Inability to clear foods containing sugars and acids from oral cavity • Symptomatic management of xerostomia involve the use of saliva stimulants and saliva substitutes. • Drugs may also be used
Saliva Substitutes • Water: • Common saliva substitute • 15mL of water resulted in 12 minute subjective improvement, and an objective improvement of 5.5 minutes. • Over the Counter substitutes: • In the form of lozenges and mouth sprays • Mucin, a common constituent of saliva is commonly prescribed and is known to have twice the improvementof water. (Davies, 1997)
Saliva Stimulants Acids: • Ascorbic acid (Vitamin C) • Citric acid (lemon juice) Sugarless chewing Gum • Stimulates taste receptors, which stimulate salivary flow (Davies,1997)
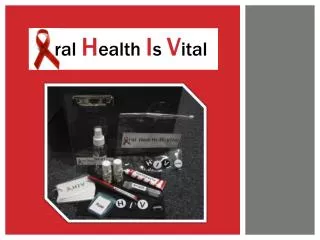
Our product • Our product features a care pack” with all the essential tools for healthy oral hygiene • The main product is a USB-wristband
WHY TECHNOLOGY • Technological world • 84% own a laptop, desktop computer, cell phone or personal digital device • Stigmatization against HIV youth • Access to information • Powerpoint • Helpful resources
The care Pack • Also included in this care pack, you will find: • Reusable Bag • Toothbrush • Toothpaste • Floss • Small Spray Bottle • Sugar-free Chewing Gum • Notepad, Clipboard and Pen • Brushing/Flossing Technique Guide • USB-wristband
USB KEY • Main product: USB-wristband • Educate the patient • Raise awareness/Spread the word • Personal Use Spread the word. Raise awareness. Wear it. Store it. Pass it along. How To Use Me: • Use to store data • Wear it proudly and pass it along to friends
Reusable Bag Spread the word. Raise awareness. Save the environment. How To Use Me: • Lunch bag • Make-up bag • Storage bag
Toothbrush Spread the word. Raise awareness. Have a clean mouth. How To Use Me: • Use with toothpaste & brushing guide
ToothPaste Spread the word. Raise awareness. Have a sparkling mouth. How To Use Me: - Use with toothbrush & brushing guide
Floss Spread the word. Raise awareness. Have a fresh mouth. How To Use Me: - Floss using the floss guide
Spray Bottle Spread the word. Raise awareness. Refresh your mouth. How To Use Me: • Spray into mouth as needed
SUGAR-FREE Gum Spread the word. Raise awareness. Say goodbye to a dry mouth. How To Use Me: - Chew throughout the day
clipboard Spread the word. Raise awareness. Keep things organized. How To Use Me: - As a clipboard for class
Notebook & Pen Spread the word. Raise awareness. Write it down. How To Use Me: - Write down and monitor your appointments with the dentist
what to do • Dentist should wear the wristband for convenience and to raise awareness • Plug USB-wristband into USB port of a computer • Go through the presentation with the patient and explain the importance of oral hygiene to prevent dental caries • Give patient “care pack” to take home • Patient can review the information at home as many times as desired • Pass it onto friends
links YEAH – Youth Empowerment Against HIV/AIDS http://www.yeah.org.au/About-Us.aspx Australian Dental Association http://www.ada.org.au/
REFERENCE LIST • Davies, A. N. (1997). The management of Xerostomia: A review. European Journal of Cancer Care , 6, 209-214. • James Guggenheimer, P. A. (2003). Xerostomia Etiology, Recognition and Treatment. The Journal of American Dental Association . • John Hicks, F. G.-G. (2003). Biological factors in dental caries: role of saliva and dental plaque in the dynamic process of demineralization and remineralization (part 1). The Journal of Clinical Pediatric Dentistry , 47-52. • Max O. Schmid, O. P. (1976). Plaque-removing effect of a toothbrush, dental floss, and a toothpick. Journal of Clinical Periodontology , 157-165. • New York State Department of Health AIDS Institute. (2001, December). HIV Clinical Resource. Retrieved March 9, 2011, from Oral Health Management in Children and Adolescents With HIV Infection: http://www.hivguidelines.org/clinical-guidelines/hiv-and-oral-health/oral-health-management-in-children-and-adolescents-with-hiv-infection/ • Stenger, M. (2006). Oral Manifestations of HIV Disease. Perspective