Vascular Physiology
Systemic Blood Pressure. Pulmonary Circulation. Overview of Systemic Circulation. Venous System. Physiology of Circulation. Regulation of Blood Pressure. Capillary Dynamics. Arteries of Head and Neck. Arterial System. Tissue Perfusion. Structure of Blood Vessels Walls.

Vascular Physiology
E N D
Presentation Transcript
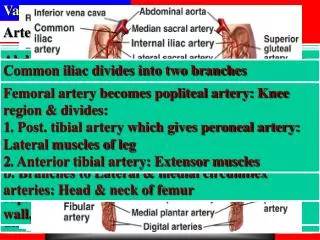
Systemic Blood Pressure Pulmonary Circulation Overview of Systemic Circulation Venous System Physiology of Circulation Regulation of Blood Pressure Capillary Dynamics Arteries of Head and Neck Arterial System Tissue Perfusion Structure of Blood Vessels Walls Arteries of the thorax wall Arteries of the Abdomen Arteries of Pelvis and Leg Arteries of Upper Limb and Thorax Vascular Physiology Three layers:Tunicaintera:Inner most layer, endo-thelium (simple squamous) & some larger vessels have subendothelium (loose CT & BM), Tunica media: Middle layer, circularly arranged smooth muscle, chemical & nervous control of deg. of cont-raction (sym. NS) & change in dia. (VC & VD), Tunica externa: Made of collagen fibers, function (protection, reinforcement & anchor to surround. tissue),accessory tissues(nerve fi., lymphatic v., ela-stic network& tiny Bdv within layer-vasa vasorum) Renal regulation of blood pressure 1. Long-term mechanisms for BP regulation 2. Kidney controls Bd vol. by regulating water loss 3. Blood volume affects CO via: a. Venous pressure b. Venous return, c. EDV & d. Stroke volume 4. BP change parallels change in Bd vol.: a. High vol. increases BP (kidney responds by eliminating water to reduce vol.) & b. Low vol. decreases BP ( kidney reabsorbs water to increase vol.) R. subclavian changes to axillary artery 1.Thoracoacromial: Superior shoulder&pectoral region 2. Lateral thoracic: Lateral chest wall & breast 3. Subscapular: Scapula, latissimus dorsi & thorax wall 4.Ant. & post. circumflex arteries: Deltoid&shoulder joint Enters arm, axillary changes to brachial artery 1.Deep brachial artery: Triceps brachii (post. arm) 2. Brachial artery: Ant. flexor muscles of arm 3. Radial artery: Lateral muscles of forearm 4. Ulnar artery: Medial muscles of forearm 1. Blood flow-volume per unit time (ml/min) 2. Blood pressure-force per unit area (mm Hg) 3. Resistance-opposition to flow; generally encoun-tered in the systemic circuit (peripheral resistance: PR): Sources of resistance (Bd viscosity“thickness related to formed elements”, total bv length‘longer vessel greater resistance’ & bv dia. ‘flow inversely related to dia.; larger dia. less resistance (1/r4)’. In humans, dia. is the greatest source of resistance Blood Flow (F) = ∆P/PR Abd. aorta gives Suprarenal arteries: Adrenal gl.s, Superior mesenteric artery (gives br.s that supply mesenteric organs (Intestinal: Large intestine, Ileocolic: Appendix, colon & R. & middle colic: Transverse colon), Paired renal arteries:Kidneys on each side of body, Gonadal arteries: (Testicular or ovarian), Inferior mesenteric artery: Gives br.s to supply distal part of colon (L. colic, sigmoidal aa , sup. rectal aa), Lumbar arteries: Post. abdominal wall, Median sacral, R. & L. common iliacs Gases & nutrients diffuse from capillary to inter-stitial fluid: Water-soluble solutes pass through clefts & fenestrations while lipid-soluble diffuse through PM of capillary epithelial cells Forces responsible for direction & amount of fluid crossing capillary walls: Hydrostatic & osmotic Pressures (forces oppose) Blood flow is precisely distributed to body tissue: 1. At rest a. Brain: 13% b. Heart 4% c. Kidney: 20% d. Abdominal organs: 24% 2. During exercise: a. Skin, muscles and heart increase b. Other tissues either remain same or decrease Blood flow velocity 1. Inversely proportionate to cross-sectional area of bv to be filled: It is fastest in vessels with smallest cross-sectional area “aorta has a cross-sectional area (2.5 cm2) & an average velocity of 40-50 cm/s, capillaries have a total cross-sectional area of 4500 cm2 and a very slow flow (0.03 cm/s)” Blood flow through individual organs is intrinsical-ly controlled (i.e., autoregulation): Diameter of arterioles feeding a given organ is controlled by it Intrinsic control mechanisms 1. Metabolic controls: Levels of nutrients, particul-arly oxygen, act as autoregulation stimuli 2. Myogenic controls: Excessive or inadequate BP can damage or cause death of an organ, such BP changes stimulate myogenic responses Arterial blood pressure: 1. Factors affecting arterial pr.: Stretching of arteries near Ht (compliance & distensibility) & vol. Bd forced into arteries near Ht 2. Changes associated with sys.: Aorta is stretched by Bd leaving lt ven. (kinetic energy) & Bd moves toward periphery because peripheral Pr. is lower than aortic Pr. (SP: 120 mm Hg) 4. Baroreceptors: a. Detect changes in art. BP: Pr. sensitive mechano-receptors when BP rises, receptors are stretched b. Located in carotid sinuses, aortic arch & walls of all large vessels c. Stretching increase signal to vasomotor center: Inhibits vasomotor center causes VD d. Arteriole dilation reduces peripheral resistance Venous return: Venous pressure is too low for adequate return, need functional modifications: a. Respiratory pump (abdominal pr. squeeze local veins, backflow is prevented by valves, Bd is forced toward the Ht, chest cavity pr. Decreases, thoracic veins expand & Bd enters rt atrium b. Muscular pump ‘more important’ (contraction of skeletal muscle surrounding veins compress vein, backflow is prevented by valves so Bd moves in direction of Ht Osmotic pressure: Net movement of water from an area of low to high solute conc. which is relatively high in capillary Bd (high concentration of plasma proteins). Capillary colloid osmotic pr. (OPc) = 26 mm Hg. Interstitial osmotic pressure (OPif) = 0.1 - 5 mm Hg. Net osmotic pressure ≈ 25 mm Hg Aorta and Major Arteries of Systemic Circulation Aortic arch 1. Coronary arteries 2. Brachiocephalic: a. R. common carotid (i. R. internal carotid & ii. R. external carotid) & b. R. subclavian (i. R. vertebral & ii. R. axillary) 3. L. common carotid: a. L. internal carotid & b. L. external carotid 4. L. subclavian: a. L. vertebral & b. L. axillary Common iliac divides into two branches 1. Internal iliac: Pelvis & visceral organs (bladder, rectum, uterus&vagina(prostate& ductus deferens) & br.s to gluteal muscles & external genitalia 2. External iliac: Enters thigh becomes femoral art. a. Deep femoral artery: Posterior thigh b. Branches to Lateral & medial circumflex arteries: Head & neck of femur Thoracic aorta (above the diaphragm) 1. Parietal branches 2. Visceral branches Abdominal aorta (below diaphragm) 1. Parietal branches 2. Visceral branches 3. R. common iliac 4. L. common iliac a. Adrenal medulla hormones i. NE and EPI (nicotine is a monoamine agonist) ii. NE is a vasoconstrictor iii. EPI increase CO by increasing contractility b. Atrial natriuretic peptide (ANP) i. Atrial peptide hormone ii. Reduces BP by antagonizing aldosterone iii. Increases water excretion from kidney 2. Muscular arteries-distributing arteries: Distal to elastic arteries, deliver Bd to specific organs, thick media layer (more smooth muscle) & 0.3 - 1.0 cm 3. Arterioles: Determine flow into capillary beds, mostly smooth muscle & 10 µm - 0.3 cm 4. Capillaries: Smallest blood vessels (8 - 10 µm), tunica interna only & exchange of materials Classification based on size and function 1. Elastic (conducting) arteries: Thick-walled, near heart, largest diameter, more elastic, large lumen (dampen BP changes associated with Ht contraction , passive accommodation results in smooth flow of blood ‘1.0 - 2.5 cm’ d. Angiotensin II: Mediated by release of renin by JGA of kidney tubule. When Bd amount entering kidney tubule is too low; renin releases & catalyzes the conversion of angiotensinogen to angiotensin II which II causes VC of systemic arterioles & increases BP. Angiotensin II also causes release of aldosterone from adrenal cortex which increases absorption of water by kidney tubules 1. Internal thoracic artery off subclavian artery a. Anterior intercostal art.s: 2. Costocervical trunk gives rise to the first two posterior intercostals arteries 3. The thoracic aorta gives rise to the next nine pairs: Posterior intercostal spaces & deep muscles of back, vertebral columns & spinal cord R. common carotid artery: (off R brachiocephalic) R. external & internal carotid arteries From external carotid artery: 1. Superior thyroid:Supplies thyroid & larynx 2. Lingual: Supplies tongue 3. Facial: Supplies skin & muscles of anterior face 4. Occipital: Supplies posterior scalp 5. Maxillary: Supplies upper & lower jaw 6. Superficial temporal: Supplies most of scalp e. Endothelium-derived factors: Endothelin (VC), prostaglandin-derived growth factor“PDGF” (VC) , nitrous oxide “NO” (fast acting local VD) f. Inflammatory chemicals (VD): Histamine, etc. (increase capillary permeability) g. Alcohol: Reduces BP, inhibits ADH release (increases loss of water in urine) & increases VD (skin) by depressing vasomotor center Net filtration pressure (NFP): Reflects interaction between hydrostatic & osmotic pressures At arterial end: NFP = (HPc - Hpif) - (OPc - OPif) = 35 - 25 = 10 mm Hg At Venous end: NFP = (HPc - Hpif) - (OPc - OPif) = 17 - 25 = -8 mm Hg e. Venodilation shifts Bd to venous reservoirs: Venous return decreases & CO declines f. Baroreceptors also send efferent signals to card. centers in medulla: Inhibit sym. NS, stimulate parasym. NS to decrease HR & contractile force g. Respond to acute changes in BP: Carotid sinus reflex protects Bd supply to brain & aortic reflex maintains supply to systemic circuit Hydrostatic pressure (HP): Force exerted by fluid against vessel wall. In capillary bed HP is the same as capillary BP that forces fluid through capillary wall: Greater at arterial end (35 mm Hg) & lower at venous end (17 mmHg). HPc is opposed by inter-stitial fluid HP (Hpif) which is assumed to be zero (interstitial fluid is withdrawn by lymphatic tissue). Net effective HP is equal to HPc (=HPc - Hpif) Abdominal artery lies below level of the diaphragm 1. Inferior phrenic arteries: Diaphragm 2. Celiac trunk: Three branches a. Common hepatic b. Splenic c. L. gastric artery 5. Chemoreceptors a. Respond to changes in O2 and CO2 concentrations and pH b. Located in carotid and aortic arch and carotid sinus c. Primarily involved in control of respiratory rate and depth Pulmonary trunk, rt. and lt. pulmonary arteries, lobar arteries (3 in rt lung & 2 in lt), arterioles, capillaries, venules, pulmonary veins (2 per lung), which drain into left atrium 5. Direct action of the kidney a. Alters rate of fluid filtration from Bd stream to kidney tubules (High BP increases filtrate entering tubules greater than can be processed, fluid leaves body as urine, Bd vol. decreases & therefore BP b. Indirect renal mechanisms (renin-angiotensin mechanism, aldosterone also cause release of ADH which promotes water reabsorption by kidney b. Splenic: a. Sends branches to stomach and pancreas b. Splenic terminates in the spleen c. Lt gastroepiploic branches: Supplies stomach c. L. gastric artery: Stomach & inferior esophagus R. Internal carotid: 1. Enters the skull and services the brain 2. Opthalmic: eyes, orbits, forehead & nose 3. R. internal carotid divides to form a. R. ant. cerebral artery: Medial surface of brain b. R. middle cerebral artery: Lateral parts of temporal and parietal lobes Types of capillary 1. Continuous: Uninterrupted endothelial cells, incomplete tight junctions (intercellular clefts) 2. Fenestrated: Endothelial cells have oval pores (fenestrations) to permit greater permeability 3. Sinusoidal: Modified, leaky capillaries (large molecules can pass through) Sequence of Bd movement through capillary bed 1. Terminal arteriole 2. Metateriole: True capillaries branch off (Pre-capillary sphincter controls Bd flow into capillary 3. Thoroughfare channel: Capillaries rejoin 4. Post-capillary venule Capillary beds 1. Capillaries act as networks-capillary beds 2. Microcirculation: Arteriole to venule 3. Parts of a capillary bed: a. Vascular shunt: Connects arteriole with venule b. True capillaries a. Common hepatic: Gives branches to stomach, small intestine & pancreas (after giving off gastro-duodenal artery, common hepatic becomes hepatic artery which branches off to R gastroepiploic: Supplies stomach), then hepatic splits into right & left branches:Supplies liver Capillary blood pressure 1. 40 mm Hg entering 2. 20 mm Hg exiting Venous blood pressure 1. Relatively steady throughout cardiac cycle 2. Gradient from venules to vena cava (20 mm HG ‘60 from aorta to arterioles’) Types of vessels 1. Venules: 8 - 100 µm, properties vary with size (little muscle & thin externa) 2. Veins: Formed from venules, thinner walls and less muscle than arteries, little muscle in media (mostly elastin) & externa is thickest wall layer Capacitance vessels 1. Veins act as reservoirs: Large lumens & low BP allows walls to thin 2. Venous valves: Prevent backflow (folds of interna) Circle of Willis 1. R. and L. posterior communicating arteries connect posterior cerebral arteries with R. and L. anterior cerebral arteries 2. Anterior communicating artery connects R. and L. anterior cerebral arteriors R. Brachiocephalic artery branches off aortic arch 1. R. subclavian artery 2. R. vertebral artery 3. Basilar artery (R+L vertebrals) 4. R. and L. posterior cerebral arteries: Supply occipital and inferior temporal lobes of brain a. Regulation of blood vessel diameter b. Vasomotor fibers (sym. Efferents, innervate sm of blood v.‘primarily arterioles’& release NE: VC) c. Vasomotor tone (tonic vasoconstriction) Factors that enhance CO 1. Reduce parasym. control (HR increases) 2. Increase sym. Activity: Increases contractility of Ht (reduces ESV & increases SV) & releases Epi into Bd stream from adrenal med. (increases HR) 3. Increase activity of resp. & muscular pumps: Increases venous return (increases EDV & SV) Neural control of blood pressure 1. Short-term mechanisms 2. Nervous control of peripheral resistance a. Alter blood distribution b. Alter blood vessel diameter 3. Vasomotor center BP = CO X PR 1. Cardiac output is directly related to Bd vol. 2. BP is directly related to CO, BV and PR CO = Stroke volume X HR Background 1. Heart pumping generates blood flow 2. Pr. results when flow opposed by resistance 3. Bd flows along a pr. gradient from higher to lower pr. (highest in aorta & lowest in rt atrium) Femoral artery becomes popliteal artery: Knee region & divides: 1. Post. tibial artery which gives peroneal artery: Lateral muscles of leg 2. Anterior tibial artery: Extensor muscles Chemical control of blood pressure 1. Short-term 2. Levels of O2 and CO2 3. Blood-borne chemicals c. Antidiuretic hormone (ADH) i. Posterior pituitary hormone ii. Increases BP by increasing water reabsorption iii. At high conc., causes vasoconstriction 3. Changes associated with dias.: Semilunar valve closes, aorta recoils & Pr. is maintained by reducing volume (DP: 70 - 80 mm Hg) 4. Pulse pressure (PP): SP minus DP 5. Mean arterial pressure (MAP)=DP+ 1/3 PP Factors influences blood pressure 1. Cardiac output 2. Peripheral resistance 3. Blood volume Home Exit BASIM ZWAIN LECTURE NOTES
Vascular Physiology Arteries of Pelvis and Leg Veins of Abdomen Major Veins of the Systemic Circulation Veins of Upper Limbs and Thorax Veins of Head and Neck Veins of Pelvis and Lower Limbs Hepatic portal system 1. Multiple hepatic vv from liver to inf. vena cava 2. Cystic veins drain gall bladder & join hepatic vv Hepatic portal v drains digestive viscera: 1. Superior mesenteric 2. Inferior mesenteric: Large intestine & rectum & joins splenic 3. Splenic: Spleen, parts of stomach & pancreas & joins superior mesenteric Other veins draining into inferior vena cava 1. Lumbar veins: R. & L. ascending lumbar veins 2. Gonadal veins: R: ovariaries or testes on right side of body (directly into vena cava), L: ovariaries or testes on left side of body (into L. renal vein) 3. Suprarenal: R: right adrenal gland (directly into vena cava), L: left adrenal gland (into left renal v) 4. Renal veins: Drain kidneys Common iliacs join to form inferior vena cava Azygous system drains thoracic tissues: Post. inter-costals, hemiazygous & accessory hemiazygous vv drain into azygous v. that drains to sup. vena cava Deep drainage of upper limb 1. Distal vv of arm drain into ulnar & radial vv 2. Ulnar & radial vv unite to form brachial vein 3. Brachial v. enters shoulder becomes axillary v. 4. At level of first rib, it becomes subclavian v. Ant. & post. tibial vv joins to form popliteal which becomes femoral vein to become external iliac joins internal iliac to form common iliac Saphenous veins a. Great: Medial aspects of leg, longest v empties into femoral v b.Small:Deep fascia of calf, empties into popliteal v Inferior vena cava runs from junction of common iliac veins to R. atrium. It receives: 1. Hepatic veins (R. and L.) 2. R. suprarenal vein 3. Renal veins (R. and L.) 4. R. gonadal vein 5. Lumbar veins Sup. vena cava pours into R atrium. It is a union of L & R brachiocephalic veins. R. brachiocephalic vein receives: 1. R. internal jugular vein 2. R. vertebral vein 3. R. subclavian vein receives R. external jugular *Left side corresponds to right side Superficial drainage of upper limb 1. Median v. of forearm lies between ulna & radius (connects either to basilic or cephalic vv) 2. Cephalic vein joins with axillary vein 3. Basilic vein joins with brachial vein 4. Median cubital v. connects basilic & cephalic vv (commonly used to obtain blood samples) Drainage of blood from brain 1. Most veins drain into dural (meningial) sinuses a. Superior sagittal b. Straight c. Cavernous d. Transverse 2. Most Bd from brain drains into internal jugulars Deep veins of face drain into inferior jugulars 1. Facial 2. Superficial temporal Home Exit BASIM ZWAIN LECTURE NOTES