Progressive Supranuclear Palsy
Progressive Supranuclear Palsy. Shirley H. Wray, M.D., Ph.D. Professor of Neurology, Harvard Medical School Director, Unit for Neurovisual Disorders Massachusetts General Hospital. Criteria for Dx PSP. Gradually progressive disorder Onset at age 40 years old or later

Progressive Supranuclear Palsy
E N D
Presentation Transcript
Progressive Supranuclear Palsy Shirley H. Wray, M.D., Ph.D. Professor of Neurology, Harvard Medical School Director, Unit for Neurovisual Disorders Massachusetts General Hospital
Criteria for Dx PSP Gradually progressive disorder Onset at age 40 years old or later Vertical supranuclear palsy Slowing of vertical saccades Postural instability with falls in the first year of disease onset
Supportive Criteria for Dx PSP Symmetric akinesia or rigidity Abnormal neck posture, especially retrocollis Poor or absent response of parkinsonism to levodopa therapy Early dysphagia and dysarthria Early onset of cognitive impairment, including at least 2 of these: apathy, decreased verbal fluency, impaired abstract reasoning, and utilization behavior
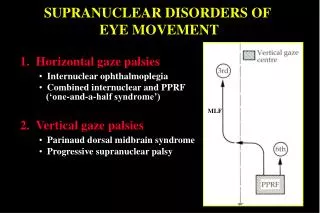
Clinical Features of PSP Slow vertical saccades, especially down, with a preserved range of movement, may be the first sign of the disorder; later, loss of vertical saccades and quick phases Horizontal saccades become slow and hypometric Disruption of steady gaze by horizontal saccadic intrusions (square-wave jerks) Impaired smooth pursuit, vertically (reduced range) and horizontally (with catch-up saccades)
Clinical Features of PSP Smooth eye-head tracking may be relatively preserved, especially vertically Preservation of vestibulo-ocular reflex Horizontal disconjugacy suggesting INO Loss of convergence Ultimately, all eye movements may be lost, but vestibular movements are the last to go
Clinical Features of PSP Eyelid disorders: delay in lid opening, lid lag, repetitive blinking in response to flashlight stimulus (failure to habituate), blepharospasm Tonic head deviation opposite to direction of body rotation (vestibulocollic reflex) Inability to clap just three times (applause sign) Leigh RJ, Zee DS. Diagnosis of Central Disorders of Ocular Motility. Chpt 12: 598-718. The Neurology of Eye Movements, Fourth Edition. Oxford University Press, NY, 2006.
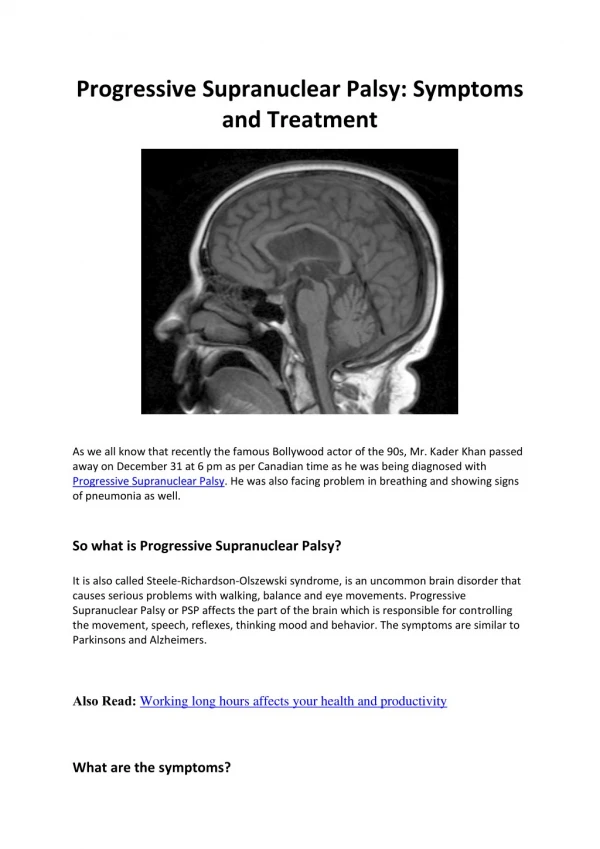
Neuroimaging Figure 1: Sagittal T2-weighted MR in another patient with PSP shows the tectal plate is markedly thinned and atrophic. Courtesy Anne Osborn, MD.
Figure 2. Single photon emission tomography (PET) scan of a patient with PSP demonstrating frontal lobe hypoperfusion.
Figure 3. PET in a patient with PSP. Showing area of hypoperfusion (blue).
Pathology Figure 4: PSP_pale locus ceruleus Figure 5: PSP_pale substantia nigra
Pathology Figure 6: PSP-the-globose Tangle
Pathology Figure 7: PSP-tau-globose-tangle Figure 8: PSP-tau-tufted
Tauopathies: Clinical Diseases Alzheimer’s disease PSP Dementia pugilistica MSA Guam ALS/PD Corticobasogangli- Pick disease onic degeneration Argyrophilic grain FTDP-17 disease Postencephalatic PD Nieman-Pick, type C Autosomal recess- SSPE ive PD
References Freidman DI, Jankovic, J, McCrary III JA. Neuro-ophthalmic findings in progressive supranuclear palsy. J Clin Neuro-ophthalmol. 1992 Jun; 12(2):104-109. Growden JH, Rossor MN. The Dementias. Blue Books of Practical Neurology. Butterworth-Heinemann 1998; vol 19.
Richardson JC, Steele J, Oszewski J. Supranuclear ophthalmoplegia, pseudobulbar palsy, nuchal dystonia and dementia. A clinical report on eight cases of heterogenous system degeneration. Trans Am Neurol Assoc. 1963; 88:25-29. Stanford PM, Halliday GM, Brooks WS, Kwok JBJ, Storey CE, Creasey H, Morris JGL, Fulham MJ, Schofield PR. Progressive supranuclear palsy pathology caused by a novel silent mutation in exon 10 of the tau gene: explanation of the disease phenotype caused by tau gene mutations. Brain 2000; 123(Pt 5): 880-893.