Case 30 Clinical information supplied
120 likes | 309 Views
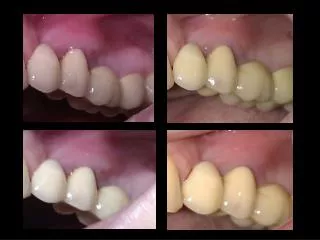
Case 30 Clinical information supplied. 25 year old male patient with Crohn’s disease for 4 years. Six week history of oral ulceration with cobblestoning of oral mucosa and pustules (confluent ) on the lips.

Case 30 Clinical information supplied
E N D
Presentation Transcript
Case 30Clinical information supplied • 25 year old male patient with Crohn’s disease for 4 years. • Six week history of oral ulceration with cobblestoning of oral mucosa and pustules (confluent ) on the lips. • Associated with confluent pustular vegetative plaque which is mildly exudative in the groin bilaterally and perineum. • Nil axillary • History of eye inflammation. • Increased eosinophils on FBC. Recently on Infliximab until 8/52
Ancillary investigations • PAS – neg • IMF - neg
Pyostomatitis vegetans • Admitted to dermatology ward • Oral steroids and steroid mouth wash • Improved • Had a similar flare 2012. • Crohn’s symptoms deteriorating until started steroids • ? Need to review Crohn’s treatment • Currently on mesalazine • Adalumimab and AZA failed
Pyostomatits vegetans • Pyodermatitis-pyostomatitisvegetans is a rare but characteristic pustular eruption of the mouth and skin folds consistently associated with inflammatory bowel diseases such as ulcerative colitis and Crohn’s • The skin disease is pyodermatitisvegetans and the mucosal disease is pyostomatitisvegetans.
Pyostomatitis vegetans • The inflammatory bowel disease usually precedes the development of the skin and/or mouth problem by months or years. Sometimes however the bowel problem is only diagnosed when it is looked for after the skin/mouth diagnosis. • Age group 20-50 years. • It is more common in males than females (3:1).
Pyostomatitis vegetans • The typical features of pyodermatitisvegetans include: • redness • pustules • crusting • large raised (vegetating) plaques • Brown post-inflammatory pigmentation is prominent. • In the mouth, pyostomatitisvegetans consists of redness with multiple yellow or white pustules. The pustules (microabscesses) easily rupture, to form superficial ulcers (erosions) which have been likened to snail trails. • Signs in the lining of the mouth in pyostomatitisvegetans include: • swelling and thickening • cobblestoned appearance • raised growths (vegetations)
Pyostomatitis vegetans • On routine pathology, pustules (microabscesses) either within or just below the epidermis will be seen, typically with many eosinophils (early lesions) and/or neutrophils (late lesions). Granulomas do not occur. Direct immunofluoresence is negative or only weakly positive. • On blood tests, indirect immunofluorescence is negative, i.e., there are no skin antibodies circulating. The blood count almost always reveals an increased number of eosinophils. Liver abnormalities have been reported so these should also be tested for routinely. • The diagnosis of pyodermatitis-pyostomatitisvegetans is therefore made on the combination of: • clinical presentation • histological features • negative direct and indirect immunofluorescence • eosinophilia on blood test • exclusion of infection.